 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Escherichia coli O157:H7 Outbreak at a Summer Camp -- Virginia, 1994On August 8, 1994, the Virginia Department of Health was notified that several campers and counselors at a summer camp had developed bloody diarrhea. The outbreak began during the July 17-30 session at a rural camp where activities included frequent overnight trips at which meals were cooked over a campfire. This report summarizes the findings from the investigation, which confirmed E. coli O157:H7 as the causative agent. To determine the source and extent of the outbreak, a standardized questionnaire was administered in person, by telephone, or sent by mail to all campers (aged 7-17 years) and counselors (aged 16-25 years) who attended the session; when necessary, parents assisted younger campers in responding to the questionnaire. A case-patient was defined as a camper or counselor either with a history of bloody diarrhea or with nonbloody diarrhea (three or more loose stools in a 24-hour period) and abdominal cramps with onset during July 17-August 7. A total of 156 (76%) of the 205 campers and counselors from this session were contacted. Attack rates for illness were 13% (18 of 135) among campers and 10% (two of 21) among counselors. The median age of case-patients was 12 years (range: 9- 22 years). Onset of illness occurred from July 22 through August 3 Figure_1. The median duration of illness was 6 days (range: 3-10 days). Seven patients had grossly bloody diarrhea, and three were hospitalized, including one with hemolytic uremic syndrome. Of nine patients for whom clinical specimens were submitted to laboratories, evidence of E. coli O157:H7 infection was detected in seven (specimens for two were positive by stool culture, and elevated IgM antibody titers to E. coli O157 lipopolysaccharide antigen were present in serum samples of five). Consumption of rare (red or pink) ground beef during the camp session was associated with a substantially increased risk for illness (attack rates: 53% {eight of 15} versus 9% {12 of 141}; relative risk 6.3; 95% confidence interval 3.1-12.9). Increased risk for illness was not associated with consumption of other foods and beverages at camp (including well-cooked ground beef), handling uncooked ground beef, contact with ill campers, sharing water bottles, or swimming frequency. Of the 15 persons who reported eating rare ground beef while at camp, 13 ate the rare ground beef at meals cooked over a campfire on an overnight trip. Rare ground beef was reported to have been eaten at seven different meals cooked over a campfire. No other risk factors for illness were identified in case-patients who did not report eating rare ground beef. Cultures of specimens of ground beef from one of six lots used during the camp session and of drinking water and swimming water at the camp were negative for E. coli O157:H7. A traceback conducted by the Virginia Department of Agriculture and Consumer Services identified one package of ground beef from a lot distributed to another site; cultures of specimens from this package also were negative for E. coli O157:H7. Reported by: B Frost, MD, Dept of Preventive Medicine, Medical College of Virginia, Richmond; C Chaos, MPH, L Ladaga, W Day, M Tenney, MD, Augusta-Staunton Health Dept, Staunton; D McWilliams, MPH, E Barrett, DMD, L Branch, S Jenkins, VMD, M Linn, E Turf, PhD, D Woolard, MPH, GB Miller, Jr, MD, State Epidemiologist, Virginia Dept of Health; S Henderson, B Campbell, M Mismas, J Dvorak, D Patel, D Peery, Div of Consolidated Laboratory Svcs, Virginia Dept of General Svcs; J Morano, K Campbell, Bur of Food Inspection, Virginia Dept of Agriculture and Consumer Svcs. Div of Field Epidemiology, Epidemiology Program Office; Foodborne and Diarrheal Diseases Br, Div of Bacterial and Mycotic Diseases, National Center for Infectious Diseases, CDC. Editorial NoteEditorial Note: E. coli O157:H7 is increasingly reported as a cause of both sporadic and outbreak-associated gastroenteritis in the United States. The increase in reported cases is believed to reflect both a true increase in incidence and improved laboratory testing and reporting (1). The spectrum of E. coli O157:H7 infection includes asymptomatic infection, nonbloody or bloody diarrhea, and hemolytic uremic syndrome, which occurs in approximately 6% of cases and is a leading cause of acute renal failure among U.S. children. Clinicians considering a diagnosis of E. coli O157:H7 gastroenteritis should determine whether a specific request for culture of E. coli O157:H7 is required by their laboratory because the range of enteric pathogens included in "routine" stool cultures varies widely by laboratory. For example, of 78 hospital laboratories in Virginia that were surveyed during September 1994, only 14 (18%) reported screening for E. coli O157:H7 as part of their routine procedure (2). Outbreaks of E. coli O157:H7 have been associated with an expanding range of foods (3,4), beverages (5), and activities (6) and with person-to-person transmission (7). Consumption of undercooked ground beef accounts for the greatest number of foodborne-related E. coli O157:H7 infections (1) and was epidemiologically implicated as the cause of the outbreak described in this report. Thorough cooking is the most effective measure to prevent E. coli O157:H7 infection associated with consumption of ground beef. Adequate cooking requires that the core temperature of the meat reach 155 F (68 C) for at least 15 seconds, and can be qualitatively assessed by ensuring that the meat is gray or brown throughout and juices are clear (8). In 1994, CDC received reports of three E. coli O157:H7 outbreaks at U.S. summer camps. Prevention of such outbreaks requires that campers and counselors who cook over campfires be informed about the importance of determining that ground beef has been adequately cooked. Kitchen staff who have been trained also can assist campers and counselors with food preparation; summer camps that serve ground beef should consider purchasing fully precooked ground beef. The importance of proper foodhandling practices at dining halls and campsites should be emphasized during routine summer camp inspections conducted by health departments, and instructions regarding the handling and cooking of ground beef should be included in scouting and camping manuals. References
Figure_1 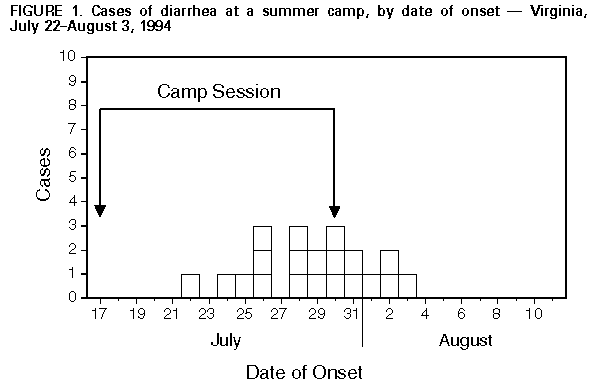 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|