 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Update -- Trends in AIDS Among Men Who Have Sex with Men -- United States, 1989-1994During 1994, local, state, and territorial health departments reported to CDC 34,974 cases of acquired immunodeficiency syndrome (AIDS) among men whose only reported HIV exposure was sexual contact with other men. Although previous reports indicated progressively smaller annual increases in cases of AIDS among men who have sex with men (MSM) (1), male-to-male sexual contact continues to represent the most frequently reported mode of HIV transmission among persons with AIDS. This report summarizes trends during January 1989-June 1994 in the occurrence of AIDS among MSM aged greater than or equal to 13 years. * For this analysis, AIDS surveillance data were reported from the 50 states, the District of Columbia, and Puerto Rico for 6-month reporting periods (i.e., January-June and July-December). Because the AIDS surveillance case definition was expanded in 1993, trends in AIDS incidence are evaluated using the estimated incidence of AIDS-defining opportunistic illnesses (AIDS-OIs) (2). Estimated AIDS-OI incidence is the sum of the observed AIDS-OI incidence and the incidence based on estimated dates of AIDS-OI diagnosis for persons reported with AIDS based only on severe immunosuppression **; both incidences are adjusted for reporting delays and anticipated redistribution of cases initially reported with no identified risk. Because the estimated dates of AIDS-OI diagnosis are based on data from a longitudinal record review project of persons in care, these rates account for changes in AIDS-OI incidence reflecting the effects of antiretroviral therapy or prophylactic therapy for Pneumocystis carinii pneumonia (2). To calculate rates for 1989-1990, the denominators were derived from 1990 U.S. census population estimates; rates for 1991, from 1991 intercensal estimates; and rates for 1992-1994, from 1992 intercensal estimates. For analysis of data by metropolitan statistical area (MSA), denominators were derived from 1990 census data for the United States and Puerto Rico. From January-June 1989 through January-June 1994, rates of AIDS-OI for MSM increased 31%, from 12.1 to 15.9 cases per 100,000 males aged greater than or equal to 13 years Figure_1. Rates varied subtantially by geographic region ***: in the Midwest and South, rates increased 51% (from 5.7 to 8.6) and 49% (from 11.6 to 17.3), respectively. Increases were smaller in the West (21%; mid-1994 rate: 21.7) and the Northeast (13%; mid-1994 rate: 15.0). Increases also varied by race/ethnicity Figure_1, and during January-June 1989 and January-June 1994, rates were highest among black men (20.8 and 37.3, respectively); the largest proportionate increase in rate (79%) during January 1989-June 1994 also occurred among black men. Rates also increased among Hispanic men (61%, from 14.0 in mid-1989 to 22.6 in mid-1994), American Indian/Alaskan Native men (77%, from 3.9 to 6.9), Asian/Pacific Islander men (55%, from 4.0 to 6.2), and white men (14%, from 10.7 to 12.2). Among males in the youngest age group (13-24 years), rates increased for blacks (31%, from 5.2 to 6.8) and Hispanics (39%, from 2.3 to 3.2) but decreased (31%, from 1.6 to 1.1) for whites. By region, the largest race/ethnicity-specific increase in rate occurred among black men in the South (109%, from 16.0 to 33.4). The only decrease occurred among white men in the Northeast (7%, from 10.0 to 9.3). Differences in rates between white men and black and Hispanic men increased in all regions during the 5-year period. The increase in rates also varied substantially by size of MSA. Although rates during mid-1989 were lowest (2.6) in rural areas (i.e., population less than 50,000), the percentage increase in rate was highest in these areas (69%; mid-1994 rate: 4.4) and in MSAs with populations of 50,000-1 million (55%; mid-1994 rate: 10.2). In comparison, although rates during mid-1989 were highest (20.8) in the largest MSAs (i.e., population greater than 2.5 million), these MSAs were characterized by the smallest 5-year percentage increase (19%; mid-1994 rate: 24.8). Since June 1981, three MSAs (New York, Los Angeles, and San Francisco) have reported 27% of all AIDS cases among MSM. During the 5-year surveillance period, rates of AIDS-OI in these three MSAs increased 8%, 12%, and 7%, respectively, (mid-1994 rates: 44.4, 34.9, and 127.7, respectively). In all three MSAs, the rate for white men decreased (20%, 16%, and 3%, respectively), and the rate for black men increased (49%, 48%, and 53%, respectively). Reported by: Local, state, and territorial health departments. Div of HIV/AIDS Prevention, National Center for Prevention Svcs, CDC. Editorial NoteEditorial Note: The findings in this report indicate a continuing increase in the occurrence of AIDS-OI diagnosed among MSM during January 1989-June 1994, although increases during this period were smaller than earlier in the epidemic. This decline in the level of increase in AIDS cases among MSM began during the late 1980s (1) and may reflect, in part, decreases in high-risk sexual behaviors and HIV incidence among MSM during the mid- to late 1980s (3). However, the occurrence of AIDS among MSM is high (151,994 new AIDS cases were reported among MSM during the 5-year period), and cases of new infections continue to occur, especially among young MSM. For example, during 1992-1993, HIV seroprevalence was 4.8% among MSM aged 18-23 years in San Francisco (4) and, during 1990-1991, 9% among MSM aged 18-24 years in New York City (5). During the same periods, the overall rates of new HIV infections among MSM in San Francisco and New York City were 1.2% and 2%, respectively (4,5). Regardless of mode of transmission, the incidence of AIDS has been higher among black and Hispanic men than among white men (6). Factors potentially associated with the increased risk among racial/ethnic minorities include decreased access to HIV-prevention services, higher rates of sexually transmitted diseases (7), and culturally inappropriate HIV-prevention activities (8). This report documents the disproportionate occurrence of AIDS among black and Hispanic MSM compared with white MSM during January 1989-June 1994. This finding underscores the need for community planning groups to consider culturally appropriate prevention services when addressing the HIV-prevention needs of racial/ethnic minorities. The use of rates to evaluate trends in estimated AIDS-OI incidence allows comparison of the impact of the epidemic among persons in different racial/ethnic groups, geographic regions, and age groups. However, rates calculated with denominators comprised of all men underestimate the impact of the epidemic among MSM because the true denominator of MSM at risk is substantially smaller than census counts of all men aged greater than or equal to 13 years. Geographic differences in rates of AIDS attributed to male-to-male sexual contact may reflect variations in the prevalence of homosexual behavior and in the prevalence of HIV infection in different communities. For example, when compared with men living in rural areas, the prevalence of men who self-identified as homosexual was seven times greater among men in the 12 largest central cities (9). The AIDS epidemic among MSM should be viewed as a composite of multiple epidemics with different times of onset and patterns of spread. AIDS surveillance data collected by health departments should be used to characterize and track local epidemics and to assist community planning groups and providers in designing and implementing HIV-prevention programs at the community level (10). References
* Single copies of this and the following report in this issue will be available free until June 1, 1996, from the CDC National AIDS Clearinghouse, P.O. Box 6003, Rockville, MD 20849-6003; telephone (800) 458-5231 or (301) 217-0023. ** CD4+ count less than 200 T-lymphocytes/uL or a CD4+ T-lymphocyte percentage of total lymphocytes of less than 14. *** Northeast=Connecticut, Maine, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, and Vermont; Midwest=Illinois, Indiana, Iowa, Kansas, Michigan, Minnesota, Missouri, Nebraska, North Dakota, Ohio, South Dakota, and Wisconsin; South=Alabama, Arkansas, Delaware, District of Columbia, Florida, Georgia, Kentucky, Louisiana, Maryland, Mississippi, North Carolina, Oklahoma, South Carolina, Tennessee, Texas, Virginia, and West Virginia; and West=Alaska, Arizona, California, Colorado, Hawaii, Idaho, Montana, Nevada, New Mexico, Oregon, Utah, Washington, and Wyoming. Figure_1 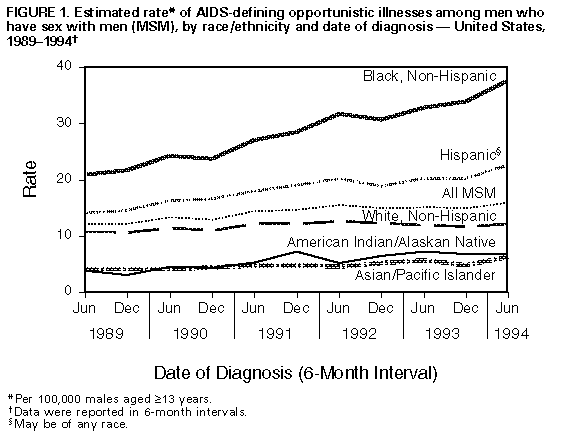 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|