 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Epidemiologic Notes and Reports Dengue Fever Among U.S. Military Personnel -- Haiti, September- November, 1994Since September 19, 1994, approximately 20,000 U.S. military personnel have been deployed to Haiti as part of Operation Uphold Democracy. To monitor the occurrence of mosquitoborne illnesses (including dengue fever {DF} and malaria) among deployed military personnel, on September 19 the U.S. Army established a surveillance system for febrile illness. Before deployment, all military personnel were instructed to take antimalarial chemoprophylaxis, either chloroquine phosphate (500 mg weekly) or doxycycline (100 mg daily). This report summarizes surveillance findings for September 19-November 4. U.S. military personnel who developed a febrile illness with no apparent underlying cause and reported to a military outpatient clinic were referred to the U.S. Army's 28th Combat Support Hospital in Port-au-Prince for admission and evaluation, including serial blood smears for malaria, blood specimens for virus isolation, and serologic studies. Because dengue virus is the principal flavivirus known to be endemic in Haiti, a probable case of DF was defined as detection of antiflavivirus immunoglobulin M (IgM) antibodies. A confirmed case was defined as isolation of dengue virus. During September 19-November 4, a total of 106 military personnel who had febrile illnesses were evaluated. Onset of illness began as early as 7 days after deployment, and the weekly number of cases peaked during the week ending October 22 Figure_1. Of the 106 patients, 24 had an illness compatible with DF (i.e., fever, headache, myalgia and/or arthralgia, with or without rash). Dengue-like illnesses occurred in personnel stationed in both urban and rural areas of Haiti. One patient with probable DF had hemorrhage from a duodenal ulcer. Another had onset of fever, myalgias, and thrombocytopenia after returning to the United States. As of November 10, preliminary laboratory results were available for 48 febrile patients. Of these, antiflavivirus IgM was detected in 11 (23%), and dengue virus was isolated from three additional patients (dengue type 1 {one patient} and dengue type 2 {two patients}). Confirmatory testing of specimens from these patients and other febrile personnel is ongoing. Repeated malaria smears were negative for all patients. The detection of DF cases among U.S. troops in Haiti prompted the following interventions: 1) use of personal protective measures against biting insects (e.g., DEET-containing repellant and bed nets) was reemphasized among unit commanders; 2) routine ultralow volume spraying of troop areas with insecticide (i.e., malathion) was implemented; and 3) common larval habitats of Aedes aegypti mosquitoes (e.g., discarded automobile tires) were identified and eliminated where possible. Reported by: LTC R DeFraites, LTC B Smoak, MAJ A Trofa, COL C Hoke, MAJ N Kanesa-thasan, MAJ A King, P MacArthy, J Putnak, PhD, J Burrous, Walter Reed Army Institute of Research; COL C Oster, COL R Redfield, LTC N Aronson, MAJ M Brown, MAJ J Fishbain, Walter Reed Army Medical Center, Washington, DC. COL VT Deal, MAJ J Quan, MAJ A Jollie, MAJ J Long-acre, MAJ J Shuette, MAJ T Logan, 28th Combat Support Hospital, Port-au-Prince, Haiti. P Jahrling, PhD, C Rossi, US Army Medical Research Institute of Infectious Diseases, Fort Detrick, Frederick, Maryland. Div of Vector-Borne Infectious Diseases, National Center for Infectious Diseases, CDC. Editorial NoteEditorial Note: Dengue virus infection is increasing throughout the Caribbean (1). Although recent surveillance data from Haiti are not available, the documentation of illness and infections among U.S. military personnel confirms the continuing occurrence of DF in Haiti and the circulation of at least two dengue virus serotypes. The incubation period for DF generally ranges from 2 to 7 days but may be as long as 14 days; therefore, illness may occur while U.S. military personnel are stationed in Haiti or after they return to the United States. Illness is characterized by abrupt onset of fever, chills, headache, eye pain, and lower back pain. Common associated symptoms include myalgia, arthralgia, nausea, vomiting, anorexia, malaise, and a blanching erythematous rash. The clinical course may be characterized by recrudescence of fever for 1-2 days after initial improvement. Laboratory findings include leukopenia and thrombocytopenia. However, a small proportion of patients may develop dengue hemorrhagic fever (DHF), which is characterized by fever, thrombocytopenia (platelet count less than 100,000/mm3), and abnormal capillary permeability evidenced by hemoconcentration, hypoalbuminemia, or pleural or abdominal effusions; mild or severe hemorrhage can occur. DHF can result in circulatory instability or shock, and the risk for these complications may be increased among persons with secondary dengue virus infections. Most dengue virus infections are self-limited and can be treated with bed rest, acetaminophen, and oral fluids. Some U.S. military personnel deployed to Haiti who also participated in Operation Restore Hope in Somalia during 1992-94 and acquired dengue infections during that operation (3) may be at increased risk for DHF. Laboratory diagnosis of DF includes detection of serum IgM antibodies, which are usually absent in specimens collected while patients are febrile but can be present in specimens collected after fever has abated (2). Definitive proof of DF requires virus isolation from serum or a fourfold or greater rise in dengue-specific antibody titers between acute- and convalescent-phase samples. Virus can be isolated from serum obtained only while patients are febrile. During November-December, approximately 9000 military personnel will be returning to the United States from Haiti. Nonmilitary U.S. residents also may be traveling to and from Haiti during this period. Because DF and malaria are endemic in Haiti, physicians and other health-care providers in the United States should consider these diseases in the differential diagnosis of febrile illnesses in any person who has recently been in Haiti or other tropical countries in the Americas (4). The occurrence of DF among troops deployed to Haiti highlights the increasing impact of this disease in the Americas, the need for an effective vaccine, and the need for increased efforts to control Ae. aegypti, the mosquito vector of dengue virus. Dengue virus is now endemic in all Caribbean countries except Cuba and the Cayman Islands (1). The potential exists for introduction of dengue virus into the United States, and for secondary transmission in areas with vector mosquitoes, because of increased travel to and from regions of the Americas where dengue is endemic. For assistance with diagnosis of dengue in persons returning from Haiti, specimens from military personnel should be sent through the state health department laboratories to the Walter Reed Army Institute of Research, Building 40, Room 2044, Attention: Major N. Kanesa-thasan, Washington, DC 20307; telephone (202) 576-2015. Specimens from civilians should be sent through state health department laboratories to CDC's Dengue Branch, Division of Vector-Borne Infectious Diseases, National Center for Infectious Diseases, 2 Calle Casia, San Juan, PR 00921-3200; telephone (809) 766-5181. Specimens for virus isolation should be sent on dry ice; specimens sent only for serologic testing may be shipped on cold packs. References
Figure_1 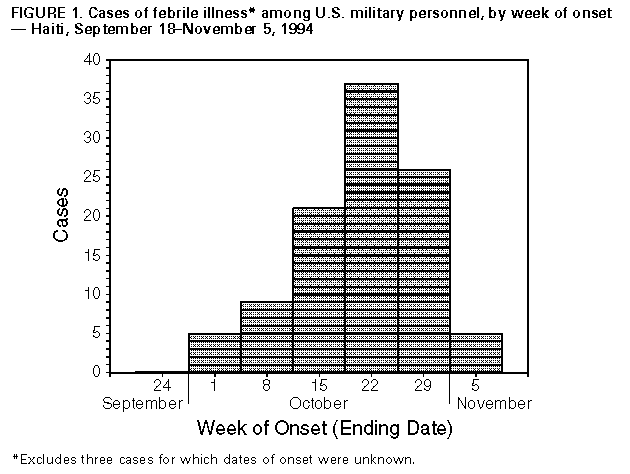 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 09/19/98 |
|||||||||
This page last reviewed 5/2/01
|