 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Sexually Transmitted Diseases Treatment Guidelines --- 2002Prepared by The material in this report was prepared for publication by the National Center for HIV, STD, and TB Prevention, Harold W. Jaffe, M.D., Acting Director; and the Division of Sexually Transmitted Diseases Prevention, Harold W. Jaffe, M.D., Acting Director. SummaryThese guidelines for the treatment of patients who have sexually transmitted diseases (STDs) were developed by the Centers for Disease Control and Prevention (CDC) after consultation with a group of professionals knowledgeable in the field of STDs who met in Atlanta on September 26--28, 2000. The information in this report updates the 1998 Guidelines for Treatment of Sexually Transmitted Diseases (MMWR 1998;47[No. RR-1]). Included in these updated guidelines are new alternative regimens for scabies, bacterial vaginosis, early syphilis, and granuloma inguinale; an expanded section on the diagnosis of genital herpes (including type-specific serologic tests); new recommendations for treatment of recurrent genital herpes among persons infected with human immunodeficiency virus (HIV); a revised approach to the management of victims of sexual assault; expanded regimens for the treatment of urethral meatal warts; and inclusion of hepatitis C as a sexually transmitted infection. In addition, these guidelines emphasize education and counseling for persons infected with human papillomavirus, clarify the diagnostic evaluation of congenital syphilis, and present information regarding the emergence of quinolone-resistant Neisseria gonorrhoeae and implications for treatment. Recommendations also are provided for vaccine-preventable STDs, including hepatitis A and hepatitis B. IntroductionPhysicians and other health-care providers play a critical role in preventing and treating sexually transmitted diseases (STDs). These recommendations for the treatment of STDs are intended to assist with that effort. Although these guidelines emphasize treatment, prevention strategies and diagnostic recommendations also are discussed. This report was produced through a multi-stage process. Beginning in 2000, CDC personnel and professionals knowledgeable in the field of STDs systematically reviewed literature (i.e., published abstracts and peer-reviewed journal articles) concerning each of the major STDs, focusing on information that had become available since publication of the 1998 Guidelines for Treatment of Sexually Transmitted Diseases (1). Background papers were written and tables of evidence constructed summarizing the type of study (e.g., randomized controlled trial or case series), study population and setting, treatments or other interventions, outcome measures assessed, reported findings, and weaknesses and biases in study design and analysis. A draft document was developed on the basis of the reviews. In September 2000, CDC staff members and invited consultants assembled in Atlanta for a 3-day meeting to present the key questions regarding STD treatment that emerged from the literature reviews and the information available to answer those questions. When relevant, the questions focused on four principal outcomes of STD therapy for each individual disease: a) microbiologic cure, b) alleviation of signs and symptoms, c) prevention of sequelae, and d) prevention of transmission. Cost-effectiveness and other advantages (e.g., single-dose formulations and directly observed therapy [DOT]) of specific regimens also were discussed. The consultants then assessed whether the questions identified were relevant, ranked them in order of priority, and attempted to arrive at answers using the available evidence. In addition, the consultants evaluated the quality of evidence supporting the answers on the basis of the number, type, and quality of the studies. In several areas, the process diverged from that previously described. The sections concerning adolescents and hepatitis A, B, and C infections were developed by other CDC staff members knowledgeable in this field. The recommendations for STD screening during pregnancy were developed after CDC staff reviewed the published recommendations from other knowledgeable groups. The sections concerning early human immunodeficiency virus (HIV) infection are a compilation of recommendations developed by CDC staff members knowledgeable in the field of HIV infection. The sections on hepatitis B virus (HBV) (2) and hepatitis A virus (HAV) (3) infections are based on previously published recommendations of the Advisory Committee on Immunization Practices (ACIP). Throughout this report, the evidence used as the basis for specific recommendations is discussed briefly. More comprehensive, annotated discussions of such evidence will appear in background papers that will be published in a supplement issue of the journal Clinical Infectious Diseases. When more than one therapeutic regimen is recommended, the sequence is alphabetized unless the choices for therapy are prioritized based on efficacy, convenience, or cost. For STDs with more than one recommended regimen, almost all regimens have similar efficacy and similar rates of intolerance or toxicity unless otherwise specified. These recommendations were developed in consultation with public- and private-sector professionals knowledgeable in the treatment of patients with STDs. They are applicable to various patient-care settings, including family planning clinics, private physicians' offices, managed care organizations, and other primary-care facilities. When using these guidelines, the disease prevalence and other characteristics of the medical practice setting should be considered. These recommendations should be regarded as a source of clinical guidance and not as standards or inflexible rules. These guidelines focus on the treatment and counseling of individual patients and do not address other community services and interventions that are important in STD/HIV prevention. Clinical Prevention GuidelinesThe prevention and control of STDs is based on the following five major concepts: a) education and counseling of persons at risk on ways to adopt safer sexual behavior; b) identification of asymptomatically infected persons and of symptomatic persons unlikely to seek diagnostic and treatment services; c) effective diagnosis and treatment of infected persons; d) evaluation, treatment, and counseling of sex partners of persons who are infected with an STD; and e) preexposure vaccination of persons at risk for vaccine-preventable STDs. Although this report focuses mainly on the clinical aspects of STD control, primary prevention of STDs begins with changing the sexual behaviors that place persons at risk for infection. Moreover, because STD control activities reduce the likelihood of transmission to sex partners, treatment of infected persons constitutes primary prevention of spread within the community. Clinicians have a unique opportunity to provide education and counseling to their patients. As part of the clinical interview, health-care providers can obtain sexual histories from their patients. Guidance in obtaining a sexual history is available in Contraceptive Technology, 17th edition (4). Prevention MessagesPrevention messages should be tailored to the patient, with consideration given to the patient's specific risk factors for STDs. Messages should include a description of specific actions that the patient can take to avoid acquiring or transmitting STDs (e.g., abstinence from sexual activity if STD-related symptoms develop). If risk factors are identified, providers should encourage patients to adopt safer sexual behaviors. Counseling skills (e.g., respect, compassion, and a nonjudgmental attitude) are essential to the effective delivery of prevention messages. Techniques that can be effective in facilitating rapport with the patient include using open-ended questions, using understandable language, and reassuring the patient that treatment will be provided regardless of circumstances unique to individual patients (including ability to pay, citizenship or immigration status, language spoken, or lifestyle). Many patients seeking treatment or screening for STDs expect evaluation for all common STDs; all patients should be specifically informed if testing for a common STD (e.g., genital herpes and human papillomavirus [HPV]) is not performed. Sexual Transmission The most reliable way to avoid transmission of STDs is to abstain from sexual intercourse (i.e., oral, vaginal, or anal sex) or to be in a long-term, mutually monogamous relationship with an uninfected partner. Counseling that encourages abstinence from sexual intercourse is crucial for persons who are being treated for an STD or whose partners are undergoing treatment and for persons who wish to avoid the possible consequences of sexual intercourse (e.g., STD/HIV and unintended pregnancy). A more comprehensive discussion of abstinence and the range of sexual expression is available in Contraceptive Technology, 17th edition (4).
Preexposure Vaccination Preexposure vaccination is one of the most effective methods for preventing transmission of certain STDs. For example, because hepatitis B virus infection frequently is sexually transmitted, hepatitis B vaccination is recommended for all unvaccinated persons being evaluated for an STD. In addition, hepatitis A vaccine is currently licensed and is recommended for men who have sex with men (MSM) and illegal drug users (both injection and non-injection). Vaccine trials for other STDs are being conducted, and additional vaccines may become available in the next several years. Prevention MethodsMale Condoms When used consistently and correctly, male latex condoms are effective in preventing the sexual transmission of HIV infection and can reduce the risk for other STDs (i.e., gonorrhea, chlamydia, and trichomonas). However, because condoms do not cover all exposed areas, they are likely to be more effective in preventing infections transmitted by fluids from mucosal surfaces (e.g., gonorrhea, chlamydia, trichomoniasis, and HIV) than in preventing those transmitted by skin-to-skin contact (e.g., herpes simplex virus [HSV], HPV, syphilis, and chancroid). Condoms are regulated as medical devices and are subject to random sampling and testing by the Food and Drug Administration (FDA). Each latex condom manufactured in the United States is tested electronically for holes before packaging. Rates of condom breakage during sexual intercourse and withdrawal are low in the United States (i.e., approximately two broken condoms per 100 condoms used). Condom failure usually results from inconsistent or incorrect use rather than condom breakage. Male condoms made of materials other than latex are available in the United States. Although they have had higher breakage and slippage rates when compared with latex condoms, the pregnancy rates among women whose partners use these condoms are similar. Non-latex condoms (i.e., those made of polyurethane or other synthetic material) can be substituted for persons with latex allergy. Patients should be advised that condoms must be used consistently and correctly to be highly effective in preventing STDs. Patients should be instructed in the correct use of condoms. The following recommendations ensure the proper use of male condoms.
Female Condoms Laboratory studies indicate that the female condom (Reality™), which consists of a lubricated polyurethane sheath with a ring on each end that is inserted into the vagina, is an effective mechanical barrier to viruses, including HIV (5). With the exception of one investigation of recurrent trichomoniasis, no clinical studies have been completed to evaluate the efficacy of female condoms in providing protection from STDs, including HIV. If used consistently and correctly, the female condom may substantially reduce the risk for STDs. When a male condom cannot be used properly, sex partners should consider using a female condom. Vaginal Spermicides, Sponges, and Diaphragms Recent evidence has indicated that vaginal spermicides containing nonoxynol-9 (N-9) are not effective in preventing cervical gonorrhea, chlamydia, or HIV infection (6). Thus, spermicides alone are not recommended for STD/HIV prevention. Frequent use of spermicides containing N-9 has been associated with genital lesions, which may be associated with an increased risk of HIV transmission. The vaginal contraceptive sponge appears to protect against cervical gonorrhea and chlamydia, but its use increases the risk for candidiasis. In case-control and cross-sectional studies, diaphragm use has been demonstrated to protect against cervical gonorrhea, chlamydia, and trichomoniasis; however, no cohort studies have been conducted (7). Neither vaginal sponges nor diaphragms should be relied on to protect women against HIV infection. The role of spermicides, sponges, and diaphragms for preventing transmission of HIV to men has not been evaluated. Diaphragm and spermicide use has been associated with an increased risk of bacterial urinary tract infection in women. Condoms and N-9 Vaginal Spermicides Condoms lubricated with spermicides are no more effective than other lubricated condoms in protecting against the transmission of HIV and other STDs. Distribution of previously purchased condoms lubricated with N-9 spermicide should continue provided the condoms have not passed their expiration date. However, purchase of any additional condoms lubricated with the spermicide N-9 is not recommended because spermicide-coated condoms cost more, have a shorter shelf-life than other lubricated condoms, and have been associated with urinary tract infection in young women. Rectal Use of N-9 Spermicides Recent data indicate that N-9 may increase the risk for HIV transmission during vaginal intercourse (6). Although similar studies have not been conducted among men who use N-9 spermicide during anal intercourse with other men, N-9 can damage the cells lining the rectum, thus providing a portal of entry for HIV and other sexually transmissible agents. Therefore, N-9 should not be used as a microbicide or lubricant during anal intercourse. Nonbarrier Contraception, Surgical Sterilization, and Hysterectomy Women who are not at risk for pregnancy might incorrectly perceive themselves to be at no risk for STDs, including HIV infection. Contraceptive methods that are not mechanical or chemical barriers offer no protection against HIV or other STDs. Women who use hormonal contraception (e.g., oral contraceptives, Norplant™, and Depo-Provera™), have intrauterine devices (IUDs), have been surgically sterilized, or have had hysterectomies should be counseled regarding the use of condoms and the risk for STDs, including HIV infection. STD/HIV Prevention CounselingInteractive counseling approaches directed at a patient's personal risk, the situations in which risk occurs, and use of goal-setting strategies are effective in STD prevention (8). One such approach --- "client-centered" HIV prevention counseling --- involves two sessions, each lasting 15--20 minutes, and has been recommended for STD clinic patients who receive HIV testing. In addition to prevention counseling, certain videos and large group presentations that provide explicit information about how to use condoms correctly have been effective in reducing the occurrence of additional STDs among persons at high risk, including STD clinic patients and adolescents. Results from randomized controlled trials demonstrate that compared with traditional approaches to providing information, certain brief risk reduction counseling approaches can reduce the occurrence of new sexually transmitted infections by 25%--40% among STD clinic patients (9). Interactive counseling strategies can be effectively used by most health-care providers, regardless of educational background or demographic profile. High-quality counseling is best ensured when clinicians are provided basic training in prevention counseling methods and skills building approaches, periodic supervisor observation of counseling with immediate feedback to counselors, periodic counselor and/or patient satisfaction evaluations, and regularly scheduled meetings of counselors and supervisors to discuss difficult situations. Prevention counseling is believed to be more effective if provided in a non-judgmental manner appropriate to the patient's culture, language, sex, sexual orientation, age, and developmental level. Partner NotificationPartner notification, once referred to as "contact tracing" but more recently included in the broader category of partner services, is the process of learning from persons with STDs about their sexual partners and helping to arrange for evaluation and treatment of those partners. Providers can furnish this service directly or with assistance from state and local health departments. The intensity of services and the specific conditions for which such services are offered by health agencies vary from area to area. Such services usually are accompanied by health counseling and may include referral of patients and their partners for other services. Many persons benefit from partner notification; thus, providers should encourage their patients to make partners aware of potential STD risk and urge them to seek diagnosis and treatment, regardless of assistance from local health agencies. However, whether the process of partner notification effectively decreases exposure to STDs from a person's sexual environment or whether it changes the incidence and prevalence of disease is uncertain. The paucity of supporting evidence regarding the consequences of partner notification has spurred the exploration of alternative approaches. One such approach is to place partner notification in the larger context of the sexual and social networks in which people are exposed to STDs. The underlying hypotheses are that networks have an influence on disease transmission that is independent of personal behaviors, that network structure is related directly to prevalence and to underlying disease transmission dynamics, and that network approaches provide a more powerful tool for identifying exposed persons and other persons at risk. A second such approach for which supporting data are being collected is the use of patient delivered therapy for treatment of contacts and others at risk, a technique that can considerably expand the role of practitioners in the control of STDs. The combination of these approaches has the potential to provide both an intervention and its evaluative tool. These approaches have not yet been sufficiently assessed to warrant definitive recommendations. However, practitioners and public health professionals should be aware of the current potential use of these nontraditional modalities in the prevention and control of STDs. Reporting and ConfidentialityThe accurate identification and timely reporting of STDs are integral components of successful disease control efforts. Timely reporting is important for assessing morbidity trends, targeting limited resources, and assisting local health authorities in identifying sex partners who may be infected. STD/HIV and acquired immunodeficiency syndrome (AIDS) cases should be reported in accordance with local statutory requirements. Syphilis, gonorrhea, chlamydia, and AIDS are reportable diseases in every state. HIV infection and chancroid are reportable in many states. The requirements for reporting other STDs differ by state, and clinicians should be familiar with local reporting requirements. Reporting can be provider- and/or laboratory-based. Clinicians who are unsure of local reporting requirements should seek advice from local health departments or state STD programs. STD and HIV reports are kept strictly confidential. In most jurisdictions, such reports are protected by statute from subpoena. Before public health representatives conduct a follow-up of a positive STD-test result, they should consult the patient's health-care provider to verify the diagnosis and treatment. Special PopulationsPregnant WomenIntrauterine or perinatally transmitted STDs can have severely debilitating effects on pregnant women, their partners, and their fetuses. All pregnant women and their sex partners should be asked about STDs, counseled about the possibility of perinatal infections, and ensured access to treatment, if needed. Recommended Screening Tests
Other Concerns Other STD-related concerns are as follows.
For a more detailed discussion of these guidelines, as well as infections not transmitted sexually, refer to the following references: Guide to Clinical Preventive Services (10), Guidelines for Perinatal Care (11), American College of Obstetricians and Gynecologists (ACOG) Educational Bulletin: Antimicrobial Therapy for Obstetric Patients (12), ACOG Committee Opinion: Primary and Preventive Care: Periodic Assessments (13), Recommendations for the Prevention and Management of Chlamydia trachomatis Infections (14), Hepatitis B Virus: A Comprehensive Strategy for Eliminating Transmission in the United States through Universal Childhood Vaccination --- Recommendations of the Immunization Practices Advisory Committee (ACIP) (1), Mother-to-infant transmission of hepatitis C virus (15), Hepatitis C: Screening in pregnancy (16), American College of Obstetricians and Gynecologists (ACOG) Educational Bulletin: Viral hepatitis in pregnancy (17), Human Immunodeficiency Virus Screening: Joint statement of the AAP and ACOG (18), Preventing Perinatal Transmission of HIV (19), and the Revised Public Health Service Recommendations for HIV Screening of Pregnant Women (20). These sources are not entirely consistent in their recommendations. The Guide to Clinical Preventive Services recommends screening of patients at high risk for chlamydia, but indicates that the optimal timing for screening is uncertain. The Guidelines for Perinatal Care recommend that pregnant women at high risk for chlamydia be screened for infection during the first prenatal-care visit and during the third trimester. Recommendations to screen pregnant women for STDs are based on disease severity and sequelae, prevalence in the population, costs, medicolegal considerations (e.g., state laws), and other factors. The screening recommendations in this report are more extensive (i.e., if followed, more women will be screened for more STDs than would be screened by following other recommendations) and are compatible with other CDC guidelines. AdolescentsHealth professionals who provide care for adolescents should be aware of several issues that relate specifically to persons within this age group. The rates of many STDs are highest among adolescents. For example, the reported rates of chlamydia and gonorrhea are highest among females aged 15--19 years, and young adults are also at highest risk for HPV infection. In addition, surveillance data indicate that 9% of adolescents who have acute HBV infection either have had sexual contact with a chronically infected person or with multiple sex partners or report their sexual preference as homosexual. As part of a comprehensive strategy to eliminate HBV transmission in the United States, ACIP has recommended that all children be administered hepatitis B vaccine (1). Younger adolescents (i.e., persons aged <15 years) who are sexually active are at particular risk for infection. Adolescents at especially high risk for STDs include youth in detention facilities, STD clinic patients, male homosexuals, and injection-drug users. Adolescents are at greater risk for STDs because they frequently have unprotected intercourse, are biologically more susceptible to infection, are engaged in partnerships often of limited duration, and face multiple obstacles to utilization of health care. Several of these issues can be addressed by clinicians who provide services to adolescents. Clinicians can address the lack of knowledge and awareness about the risks and consequences of STDs and offer guidance, constituting true primary prevention, to help adolescents develop healthy sexual behaviors and thus prevent the establishment of patterns of behavior that can undermine sexual health. With a few exceptions, all adolescents in the United States can consent to the confidential diagnosis and treatment of STDs. Medical care for STDs can be provided to adolescents without parental consent or knowledge. Furthermore, in many states adolescents can consent to HIV counseling and testing. Consent laws for vaccination of adolescents differ by state. Several states consider provision of vaccine similar to treatment of STDs and provide vaccination services without parental consent. Health-care providers should acknowledge the importance of confidentiality for adolescents and should strive to follow policies that comply with state laws to ensure the confidentiality of STD-related services. Despite the prevalence of STDs among adolescents, providers frequently fail to inquire about sexual behavior, assess risk for STDs, counsel about risk reduction, and screen for asymptomatic infection during clinical encounters. When addressing these sensitive areas with young people, the style and content of counseling and health education should be adapted for adolescents. Discussions should be appropriate for the patient's developmental level and should identify risky behaviors (e.g., sex and drug-use behaviors). Careful counseling and thorough discussions are particularly important for adolescents who may not acknowledge that they engage in high-risk behaviors. Care and counseling should be direct and nonjudgmental. ChildrenManagement of children who have STDs requires close cooperation between clinicians, laboratorians, and child-protection authorities. Investigations, when indicated, should be initiated promptly. Some diseases (e.g., gonorrhea, syphilis, and chlamydia), if acquired after the neonatal period, are almost 100% indicative of sexual contact. For other diseases (e.g., HPV infection and vaginitis), the association with sexual contact is not as clear (see Sexual Assault and STDs). Men Who Have Sex with MenSome MSM are at high risk for HIV infection and other viral and bacterial STDs. Although the frequency of unsafe sexual practices and reported rates of bacterial STDs and incident HIV infection has declined substantially in MSM during the last several decades, increased rates of infectious syphilis, gonorrhea, and chlamydial infection, largely among HIV-infected MSM, have been recently reported in many cities in the United States and other industrialized countries. Preliminary data also indicate higher frequencies of unsafe sex and suggest that the incidence of HIV infection may be rising among MSM in some cities. The underlying behavioral changes likely are related to effects of improved HIV/AIDS therapy on quality of life and survival, "safer sex burnout," and in some cities, adverse trends in substance abuse. Clinicians should assess sexual risk for all male patients, which includes routinely inquiring about the sex of patients' sex partners. MSM, including those with HIV infection, should routinely undergo straightforward, nonjudgmental STD/HIV risk assessment and client-centered prevention counseling to reduce the likelihood of acquisition or transmission of HIV and other STDs. In addition, screening for STDs should be considered for many MSM. The following screening recommendations are based on preliminary data; these tests should be performed at least annually for sexually active MSM:
In addition, vaccination against hepatitis is the most effective means of preventing sexual transmission of hepatitis A and B. Prevaccination serologic testing may be cost-effective in MSM, among whom the prevalence of hepatitis A and B infection is likely to be high. More frequent STD screening (e.g., at 3--6-month intervals) may be indicated for MSM at highest risk (e.g., those who acknowledge having multiple anonymous partners or having sex in conjunction with illicit drug use and patients whose sex partners participate in these activities). Screening tests usually are indicated regardless of a patient's history of consistent use of condoms for insertive or receptive anal intercourse. Providers also should be knowledgeable about the common manifestations of symptomatic STDs in MSM (e.g., urethral discharge, dysuria, anorectal symptoms [such as pain, pruritis, discharge, and bleeding], genital or anorectal ulcers, other mucocutaneous lesions, lymphadenopathy, and skin rash). If these symptoms are present, providers should perform appropriate diagnostic tests. HIV Infection: Detection, Counseling, and ReferralInfection with HIV produces a spectrum of disease that progresses from a clinically latent or asymptomatic state to AIDS as a late manifestation. The pace of disease progression varies. In untreated patients, the time between infection with HIV and the development of AIDS ranges from a few months to as long as 17 years (median: 10 years). Most adults and adolescents infected with HIV remain symptom-free for extended periods, but viral replication is active during all stages of infection, increasing substantially as the immune system deteriorates. In the absence of treatment, AIDS eventually develops in almost all HIV-infected persons; in one study of HIV-infected adults, AIDS developed in 87% within 17 years of infection. Additional cases are expected to occur among those who have remained AIDS-free for longer periods of time. Greater awareness among both patients and health-care providers of the risk factors associated with HIV transmission has led to increased testing for HIV and earlier diagnosis of the infection, often before symptoms develop. Prompt diagnosis of HIV infection is important for several reasons. Treatments are available that slow the decline of immune system function; use of these therapies has been associated with substantial declines in HIV-associated morbidity and mortality in recent years. HIV-infected persons who have altered immune function are at increased risk for infections for which preventive measures are available (e.g., Pneumocystis carinii pneumonia [PCP], toxoplasmic encephalitis [TE], disseminated Mycobacterium avium complex [MAC] disease, tuberculosis [TB], and bacterial pneumonia). Because of its effect on the immune system, HIV affects the diagnosis, evaluation, treatment, and follow-up of many other diseases and may affect the efficacy of antimicrobial therapy for some STDs. Finally, the early diagnosis of HIV enables health-care providers to counsel such patients, refer them to various support services, and help prevent HIV transmission to others. Proper management of HIV infection involves a complex array of behavioral, psychosocial, and medical services. Although some of these services may be available in the STD treatment facility, many services are often unavailable in this setting. Therefore, referral to a health-care provider or facility experienced in caring for HIV-infected patients is advised. Staff in STD treatment facilities should be knowledgeable about the options for referral available in their communities. While in STD treatment facilities, HIV-infected patients should be educated about HIV infection and the various options for available support services and HIV care. Because multiple, complex services are required for management of HIV infection, detailed information (particularly regarding medical care) is beyond the scope of this section and can be found elsewhere (8,21). This report provides information regarding diagnostic testing for HIV infection, counseling patients who have HIV infection, and referral of patients to support services (including medical care). Information also is provided regarding the management of sex partners, because such services can and should be provided in STD treatment facilities. In addition, the topics of HIV infection during pregnancy and in infants and children are addressed. Detection of HIV Infection: Diagnostic TestingTesting for HIV is recommended and should be offered to all persons who seek evaluation and treatment for STDs. Counseling before and after testing (i.e., pretest and posttest counseling) is an integral part of the testing procedure (see HIV Prevention Counseling). Informed consent must be obtained before an HIV test is performed. Some states require written consent. HIV infection usually is diagnosed by tests for antibodies against HIV-1 and HIV-2 (HIV-1/2). Antibody testing begins with a sensitive screening test (e.g., the enzyme immunoassay [EIA]). Reactive screening tests must be confirmed by supplemental test (e.g., the Western blot [WB]) or an immunofluorescence assay (IFA). If confirmed by a supplemental test, a positive antibody test result indicates that a person is infected with HIV and is capable of transmitting the virus to others. HIV antibody is detectable in at least 95% of patients within 3 months after infection. Although a negative antibody test result usually indicates that a person is not infected, antibody tests cannot exclude recent infection. Most HIV infections in the United States are caused by HIV-1; <100 cases of HIV-2 infection have been documented (22). However, HIV-2 infection should be suspected in persons who have epidemiologic risk factors for HIV-2. Examples of these risk factors include persons with sex partners from West Africa (where HIV-2 is endemic), those with sex partners known to be infected with HIV-2, and persons who received a blood transfusion or a non-sterile injection in a West African country. HIV-2 testing is also indicated when clinical evidence of HIV exists but tests for antibodies to HIV-1 are not positive, or when HIV-1 Western blot results include the unusual indeterminate pattern of gag plus pol bands in the absence of env bands (22). Health-care providers should be knowledgeable about the symptoms and signs of acute retroviral syndrome, which is characterized by fever, malaise, lymphadenopathy, and skin rash. This syndrome frequently occurs in the first few weeks after HIV infection, before antibody test results become positive. Suspicion of acute retroviral syndrome should prompt nucleic acid testing (HIV plasma RNA [i.e., viral load]) to detect the presence of HIV, although this test is not approved for diagnostic purposes; a positive test should be confirmed by another HIV test. Current guidelines suggest that persons with recently acquired HIV infection might benefit from antiretroviral drugs, and such patients may be candidates for clinical trials (23,24). Therefore, patients with acute HIV infection should be referred immediately to an HIV clinical care provider. Detection of HIV infection should prompt efforts to reduce the risk behavior that resulted in HIV infection and could result in transmission of HIV to others. Early counseling and education are particularly important for persons with recently acquired infection, because HIV plasma RNA levels are characteristically high during this phase of infection and likely constitute a risk factor for HIV transmission. The following are specific recommendations for diagnostic testing for HIV infection.
Counseling for Patients with HIV Infection and Referral to Support ServicesPatients can be expected to be distressed when first informed of a positive HIV test result. Such patients face several major adaptive challenges, including a) accepting the possibility of a shortened life span, b) coping with others' reactions to a stigmatizing illness, c) developing and adopting strategies for maintaining physical and emotional health, and d) initiating changes in behavior to prevent HIV transmission to others. Many patients also require assistance with making reproductive choices, gaining access to health services, and confronting possible employment or housing discrimination. Therefore, in addition to medical care, behavioral and psychosocial services are an integral part of health care for HIV-infected patients. Such services should be available on site or through referral when HIV infection is diagnosed. A comprehensive discussion of specific recommendations is available in the Guidelines for HIV Counseling, Testing, and Referral (8). Practice settings for offering HIV care differ depending on local resources and needs. Primary-care providers and outpatient facilities must ensure that appropriate resources are available for each patient to avoid fragmentation of care. Although a single source that is capable of providing comprehensive care for all stages of HIV infection is preferred, the limited availability of such resources often results in the need to coordinate care among medical and social service providers in different locations. Providers should avoid long delays between diagnosis of HIV infection and access to additional medical and psychosocial services. Recently identified HIV infection may not have been recently acquired. Persons newly diagnosed with HIV may be at any stage of infection. Therefore, health-care providers should be alert for symptoms or signs that suggest advanced HIV infection (e.g., fever, weight loss, diarrhea, cough, shortness of breath, and oral candidiasis). The presence of any of these symptoms should prompt urgent referral for medical care. Similarly, providers should be alert for signs of psychologic distress and be prepared to refer patients accordingly. Diagnosis of HIV infection reinforces the need to counsel patients regarding high risk behaviors, because the consequences of such behaviors include the risk for acquiring additional STDs and for transmitting HIV (and other STDs) to other persons. Such attention to behaviors in HIV-infected persons is consistent with national strategies for HIV prevention (25). Providers should be able to refer patients for prevention counseling and risk reduction support concerning high risk behaviors (e.g., substance abuse and high risk sexual behavior). HIV-infected patients in the STD treatment setting should be educated about what to expect as they enter medical care for HIV infection. In non-emergent situations, the initial evaluation of HIV-positive patients usually includes a) a detailed medical history, including sexual and substance-abuse history, previous STDs, and specific HIV-related symptoms or diagnoses; b) a physical examination (including a gynecologic examination for women); c) testing for N. gonorrhoeae and C. trachomatis (and for women, a Pap test and wet mount examination of vaginal secretions); d) complete blood and platelet counts and blood chemistry profile; e) toxoplasma antibody test; f) tests for hepatitis B, C, and for MSM, hepatitis A; g) syphilis serology; h) a CD4+ T-lymphocyte analysis and determination of HIV plasma RNA (i.e., HIV viral load); i) a tuberculin skin test (TST) (sometimes referred to as a purified protein derivative [PPD]); j) a urinalysis; and k) a chest radiograph (21). In subsequent visits, once the results of laboratory and skin tests are available, the patient may be offered antiretroviral therapy (23,24), if indicated, as well as specific medications to reduce the incidence of opportunistic infections (e.g., PCP, TE, disseminated MAC infection, and TB) (21,26). Hepatitis B vaccination should be offered to patients who lack hepatitis B serologic markers. Hepatitis A vaccination should be given to persons at increased risk for hepatitis A infection (e.g., MSM and illegal drug users) and to patients with chronic hepatitis B or hepatitis C who lack antibodies to hepatitis A. Influenza vaccination should be offered annually, and pneumococcal vaccination should be administered if not given in the previous 5 years (21). Providers must be alert to the possibility of new or recurrent STDs and treat such conditions aggressively. Occurrence of an STD in an HIV-infected person is an indication of high-risk behavior and should prompt referral for counseling. Because many STDs are asymptomatic, routine screening for curable STDs (e.g., syphilis, gonorrhea, and chlamydia) should be performed at least yearly for sexually active persons. More frequent screening may be appropriate depending on individual risk behaviors, the local epidemiology of STDs, and whether incident STDs are detected by screening or by the presence of symptoms. Patients should receive, or be referred for, a thorough psychosocial evaluation, including ascertainment of behavioral factors indicating risk for transmitting HIV. Patients may require referral for specific behavioral intervention (e.g., a substance abuse program), for mental health disorders (e.g., depression), or for emotional distress. They may require assistance with securing and maintaining employment and housing. Women should be counseled or appropriately referred regarding reproductive choices and contraceptive options. Patients with multiple psychosocial problems may be candidates for prevention case management (27). The following are specific recommendations for counseling and referral.
Management of Sex Partners and Injection-Drug PartnersClinicians evaluating HIV-infected persons should collect information to determine whether any partners should be notified about possible exposure to HIV (8). When referring to persons who are infected with HIV, the term "partner" includes not only sex partners but also injection-drug users who share syringes or other injection equipment. The rationale for partner notification is that the early diagnosis and treatment of HIV infection in these partners possibly reduces morbidity and provides the opportunity to encourage risk-reducing behaviors. Partner notification for HIV infection must be confidential and depends on the voluntary cooperation of the patient. Two complementary notification processes, patient referral and provider referral, can be used to identify partners. With patient referral, patients directly inform their partners of their exposure to HIV infection. With provider referral, trained health department personnel locate partners on the basis of the names, descriptions, and addresses provided by the patient. During the notification process, the confidentiality of patients is protected; their names are not revealed to partners who are notified. Many state health departments provide assistance, if requested, with provider-referral partner notification. The following are specific recommendations for implementing partner-notification procedures.
Special ConsiderationsPregnancy Voluntary counseling and HIV testing should be offered routinely to all pregnant women as early in pregnancy as possible (20). For women who decline these services, providers should continue to strongly encourage testing and to address concerns that pose obstacles to testing. Providing pregnant women with counseling and testing is particularly important not only to maintain the health of the patient, but also because interventions (antiretroviral and obstetrical) are available that can reduce perinatal transmission of HIV. Once identified as being HIV-infected, pregnant women should be informed specifically about the risk for perinatal infection. Current evidence indicates that, in the absence of antiretroviral and other interventions, 15%--25% of infants born to HIV-infected mothers will become infected with HIV; such evidence also indicates that an additional 12%--14% are infected during breastfeeding in resource-limited settings where HIV-infected women breastfeed their infants into the second year of life (28). However, the risk of HIV transmission can be reduced substantially to <2% through antiretroviral regimens and obstetrical interventions (i.e., AZT or nevirapine and elective c-section at 38 weeks of pregnancy) and by avoiding breastfeeding (29). Pregnant women who are HIV-infected should be counseled about their options (either on-site or by referral), given appropriate antenatal treatment, and (for women living in the United States, where infant formula is readily available and can be safely prepared) advised not to breastfeed their infants. HIV Infection Among Infants and Children Diagnosis of HIV infection in a pregnant woman indicates the need to consider whether additional children are infected. Infants and young children with HIV infection differ from adults and adolescents with respect to the diagnosis, clinical presentation, and management of HIV disease. For example, because maternal HIV antibody passes through the placenta, antibody tests for HIV are expected to be positive in the sera of both infected and uninfected infants born to seropositive mothers. A definitive determination of HIV infection for an infant aged <18 months should be based on laboratory evidence of HIV in blood or tissues by culture, nucleic acid, or antigen detection. Management of infants, children, and adolescents who are known or suspected to be infected with HIV requires referral to physicians familiar with the manifestations and treatment of pediatric HIV infection (21,30). Diseases Characterized by Genital UlcersManagement of Patients Who Have Genital UlcersIn the United States, most young, sexually active patients who have genital ulcers have either genital herpes, syphilis, or chancroid. The relative frequency of each differs by geographic area and patient population; however, genital herpes is the most prevalent of these diseases. More than one of these diseases sometimes is present in a patient who has genital ulcers. Each disease has been associated with an increased risk for HIV infection. Not all genital ulcers are caused by sexually transmitted infections. A diagnosis based only on the patient's medical history and physical examination often is inaccurate. Therefore, evaluation of all patients who have genital ulcers should include a serologic test for syphilis and a diagnostic evaluation for genital herpes; in settings where chancroid is prevalent, a test for Haemophilus ducreyi should also be performed. Specific tests for evaluation of genital ulcers include
No FDA-approved PCR test for these organisms is available in the United States, but such testing can be performed by commercial laboratories that have developed their own PCR tests. Type-specific serology for HSV type 2 may be helpful in identifying persons with genital herpes (see Genital Herpes). Biopsy of ulcers may be helpful in identifying the cause of unusual ulcers or ulcers that do not respond to initial therapy. HIV testing should be performed in the management of patients who have genital ulcers caused by T. pallidum or H. ducreyi. Such testing should be considered for those who have ulcers caused by HSV (see sections on Syphilis, Chancroid, and Genital Herpes). Health-care providers often must treat patients before test results are available because early treatment decreases the possibility of ongoing transmission and because successful treatment of genital herpes depends upon prompt initiation of therapy. In this circumstance, the clinician should treat for the diagnosis considered most likely on the basis of clinical presentation and epidemiologic circumstances. Sometimes treatment must be initiated for additional conditions because of diagnostic uncertainty. Even after complete diagnostic evaluation, at least 25% of patients who have genital ulcers have no laboratory-confirmed diagnosis. ChancroidIn the United States, chancroid usually occurs in discrete outbreaks, although the disease is endemic in some areas. Chancroid is a cofactor for HIV transmission; high rates of HIV infection among patients who have chancroid occur in the United States and other countries. About 10% of persons who have chancroid acquired in the United States are coinfected with T. pallidum or HSV; this percentage is higher in persons acquiring chancroid outside the United States. A definitive diagnosis of chancroid requires identification of H. ducreyi on special culture media that is not widely available from commercial sources; even using these media, sensitivity is <80%. No FDA-approved PCR test for H. ducreyi is available in the United States, but such testing can be performed by commercial laboratories that have developed their own PCR test. A probable diagnosis, for both clinical and surveillance purposes, can be made if all the following criteria are met: a) the patient has one or more painful genital ulcers; b) the patient has no evidence of T. pallidum infection by darkfield examination of ulcer exudate or by a serologic test for syphilis performed at least 7 days after onset of ulcers; c) the clinical presentation, appearance of genital ulcers and, if present, regional lymphadenopathy are typical for chancroid; and d) a test for HSV performed on the ulcer exudate is negative. The combination of a painful ulcer and tender inguinal adenopathy, symptoms occurring in one third of patients, suggests a diagnosis of chancroid; when accompanied by suppurative inguinal adenopathy, these signs are almost pathognomonic. Treatment Successful treatment for chancroid cures the infection, resolves the clinical symptoms, and prevents transmission to others. In advanced cases, scarring can result despite successful therapy.
NOTE: Ciprofloxacin is contraindicated for pregnant and lactating women. Azithromycin and ceftriaxone offer the advantage of single-dose therapy. Worldwide, several isolates with intermediate resistance to either ciprofloxacin or erythromycin have been reported. Other Management Considerations Patients who are uncircumcised and patients with HIV infection do not respond as well to treatment as those who are circumcised or HIV-negative. Patients should be tested for HIV infection at the time chancroid is diagnosed. Patients should be retested for syphilis and HIV 3 months after the diagnosis of chancroid if the initial test results were negative. Follow-Up Patients should be re-examined 3--7 days after initiation of therapy. If treatment is successful, ulcers usually improve symptomatically within 3 days and objectively within 7 days after therapy. If no clinical improvement is evident, the clinician must consider whether a) the diagnosis is correct, b) the patient is coinfected with another STD, c) the patient is infected with HIV, d) the treatment was not used as instructed, or e) the H. ducreyi strain causing the infection is resistant to the prescribed antimicrobial. The time required for complete healing depends on the size of the ulcer; large ulcers may require >2 weeks. In addition, healing is slower for some uncircumcised men who have ulcers under the foreskin. Clinical resolution of fluctuant lymphadenopathy is slower than that of ulcers and may require needle aspiration or incision and drainage, despite otherwise successful therapy. Although needle aspiration of buboes is a simpler procedure, incision and drainage may be preferred because of reduced need for subsequent drainage procedures. Management of Sex Partners Sex partners of patients who have chancroid should be examined and treated, regardless of whether symptoms of the disease are present, if they had sexual contact with the patient during the 10 days preceding the patient's onset of symptoms. Special Considerations Pregnancy The safety and efficacy of azithromycin for pregnant and lactating women have not been established. Ciprofloxacin is contraindicated during pregnancy and lactation. No adverse effects of chancroid on pregnancy outcome have been reported. HIV Infection HIV-infected patients who have chancroid should be monitored closely because, as a group, these patients are more likely to experience treatment failure and to have ulcers that heal more slowly. HIV-infected patients may require longer courses of therapy than those recommended for HIV-negative patients, and treatment failures can occur with any regimen. Because data are limited concerning the therapeutic efficacy of the recommended ceftriaxone and azithromycin regimens in HIV-infected patients, these regimens should be used for such patients only if follow-up can be ensured. Some specialists suggest using the erythromycin 7-day regimen for treating HIV-infected persons. Genital Herpes Simplex Virus InfectionsGenital herpes is a recurrent, life-long viral infection. Two serotypes of HSV have been identified: HSV-1 and HSV-2. Most cases of recurrent genital herpes are caused by HSV-2. At least 50 million persons in the United States have genital HSV infection. Most persons infected with HSV-2 have not been diagnosed. Many such persons have mild or unrecognized infections but shed virus intermittently in the genital tract. Most genital herpes infections are transmitted by persons unaware that they have the infection or who are asymptomatic when transmission occurs. Rarely, first-episode genital herpes is manifested by severe disease that may require hospitalization. Diagnosis of HSV Infection The clinical diagnosis of genital herpes is both insensitive and nonspecific. The typical painful multiple vesicular or ulcerative lesions are absent in many infected persons. Up to 30% of first-episode cases of genital herpes are caused by HSV-1, but recurrences are much less frequent for genital HSV-1 infection than genital HSV-2 infection. Therefore, the distinction between HSV serotypes influences prognosis and counseling. For these reasons, the clinical diagnosis of genital herpes should be confirmed by laboratory testing. Both virologic tests and type-specific serologic tests for HSV should be available in clinical settings that provide care for patients with STDs or those at risk for STDs. Virologic Tests Isolation of HSV in cell culture is the preferred virologic test in patients who present with genital ulcers or other mucocutaneous lesions. The sensitivity of culture declines rapidly as lesions begin to heal, usually within a few days of onset. Some HSV antigen detection tests, unlike culture and the direct fluorescent antibody test, do not distinguish HSV-1 from HSV-2. Polymerase chain reaction (PCR) assays for HSV DNA are highly sensitive, but their role in the diagnosis of genital ulcer disease has not been well-defined. However, PCR is available in some laboratories and is the test of choice for detecting HSV in spinal fluid for diagnosis of HSV-infection of the central nervous system (CNS). Cytologic detection of cellular changes of herpes virus infection is insensitive and nonspecific, both in genital lesions (Tzanck preparation) and cervical Pap smears, and should not be relied on for diagnosis of HSV infection. Type-specific Serologic Tests Both type-specific and nonspecific antibodies to HSV develop during the first several weeks following infection and persist indefinitely. Because almost all HSV-2 infections are sexually acquired, type-specific HSV-2 antibody indicates anogenital infection, but the presence of HSV-1 antibody does not distinguish anogenital from orolabial infection. Accurate type-specific assays for HSV antibodies must be based on the HSV-specific glycoprotein G2 for the diagnosis of infection with HSV-2 and glycoprotein G1 for diagnosis of infection with HSV-1. Such assays first became commercially available in 1999, but older assays that do not accurately distinguish HSV-1 from HSV-2 antibody, despite claims to the contrary, remain on the market. Therefore, the serologic type-specific gG-based assays should be specifically requested when serology is performed. Currently, the FDA-approved, gG-based type-specific assays include POCkit™HSV-2 (manufactured by Diagnology); HerpeSelect™-1 ELISA IgG or HerpeSelect™-2 ELISA IgG (manufactured by Focus Technology, Inc.); and HerpeSelect™ 1 and 2 Immunoblot IgG (manufactured by Focus Technology, Inc.). The POCkit™-HSV-2 assay is a point-of-care test that provides results for HSV-2 antibodies from capillary blood or serum during a clinic visit. The Focus Technology assays are laboratory-based. The sensitivities of these tests for detection of HSV-2 antibody vary from 80% to 98%, and false-negative results may occur, especially at early stages of infection. The specificities of these assays are >96%. False-positive results can occur, especially in patients with low likelihood of HSV infection. Therefore, repeat testing or a confirmatory test (e.g., an immunoblot assay if the initial test was an ELISA) may be indicated in some settings. Because false-negative HSV cultures are common, especially in patients with recurrent infection or with healing lesions, type-specific serologic tests are useful in confirming a clinical diagnosis of genital herpes. Additionally, such tests can be used to diagnose persons with unrecognized infection and to manage sex partners of persons with genital herpes. Although serologic assays for HSV-2 should be available for persons who request them, screening for HSV-1 or HSV-2 infection in the general population is not indicated. Principles of Management of Genital Herpes Antiviral chemotherapy offers clinical benefits to most symptomatic patients and is the mainstay of management. In addition, counseling regarding the natural history of genital herpes, sexual and perinatal transmission, and methods to reduce transmission is integral to clinical management. Systemic antiviral drugs partially control the symptoms and signs of herpes episodes when used to treat first clinical episodes and recurrent episodes or when used as daily suppressive therapy. However, these drugs neither eradicate latent virus nor affect the risk, frequency, or severity of recurrences after the drug is discontinued. Randomized trials indicate that three antiviral medications provide clinical benefit for genital herpes: acyclovir, valacyclovir, and famciclovir (31--41). Valacyclovir is the valine ester of acyclovir and has enhanced absorption after oral administration. Famciclovir, a pro-drug of penciclovir, also has high oral bioavailability. Topical therapy with antiviral drugs offers minimal clinical benefit, and its use is not recommended. First Clinical Episode of Genital Herpes Many patients with first-episode herpes present with mild clinical manifestations but later develop severe or prolonged symptoms. Therefore, most patients with initial genital herpes should receive antiviral therapy.
NOTE: Treatment may be extended if healing is incomplete after 10 days of therapy. Higher dosages of acyclovir (i.e., 400 mg orally five times a day) were used in treatment studies of first-episode herpes proctitis and first-episode oral infection. However, no comparative studies have been conducted, and whether these forms of HSV infection require higher doses of antiviral drugs than used for genital herpes is unknown. Valacyclovir and famciclovir probably are also effective for acute HSV proctitis or oral infection, but clinical experience is lacking. Recurrent Episodes of HSV Disease Most patients with symptomatic, first-episode genital HSV-2 infection subsequently experience recurrent episodes of genital lesions; recurrences are much less frequent following initial genital HSV-1 infection. Antiviral therapy for recurrent genital herpes can be administered either episodically, to ameliorate or shorten the duration of lesions, or continuously as suppressive therapy to reduce the frequency of recurrences. Many patients, including those with mild or infrequent recurrent outbreaks, benefit from antiviral therapy; therefore, options for treatment should be discussed with all patients. Episodic Therapy for Recurrent Genital Herpes Effective episodic treatment of recurrent herpes requires initiation of therapy within 1 day of lesion onset, or during the prodrome that precedes some outbreaks. The patient should be provided with a supply of drug or a prescription for the medication with instructions to self-initiate treatment immediately when symptoms begin.
For episodic therapy, a randomized controlled trial indicated that a 3-day course of valacyclovir 500 mg twice daily is as effective as a 5-day course. Similar studies have not been done with acyclovir and famciclovir. Suppressive Therapy for Recurrent Genital Herpes Suppressive therapy reduces the frequency of genital herpes recurrences by 70%--80% among patients who have frequent recurrences (i.e., >6 recurrences per year), and many patients report no symptomatic outbreaks. Treatment probably is also effective in patients with less frequent recurrences, although definitive data are lacking. Safety and efficacy have been documented among patients receiving daily therapy with acyclovir for as long as 6 years, and with valacyclovir or famciclovir for 1 year. Quality of life often is improved in patients with frequent recurrences who receive suppressive compared with episodic treatment. The frequency of recurrent outbreaks diminishes over time in many patients, and the patient's psychological adjustment to the disease may change. Therefore, periodically during suppressive treatment (e.g., once a year), discontinuation of therapy should be discussed with the patient to reassess the need for continued therapy. Suppressive antiviral therapy reduces but does not eliminate subclinical viral shedding. Therefore, the extent to which suppressive therapy prevents HSV transmission is unknown.
Valacyclovir 500 mg once a day might be less effective than other valacyclovir or acyclovir dosing regimens in patients who have very frequent recurrences (i.e., >10 episodes per year). Few comparative studies of valacyclovir or famciclovir with acyclovir have been conducted. The results of these studies suggest that valacyclovir and famciclovir are comparable to acyclovir in clinical outcome (35--39). Ease of administration and cost also are important considerations for prolonged treatment. Severe Disease IV acyclovir therapy should be provided for patients who have severe disease or complications that necessitate hospitalization, such as disseminated infection, pneumonitis, hepatitis, or complications of the central nervous system (e.g., meningitis or encephalitis). The recommended regimen is acyclovir 5--10 mg/kg body weight IV every 8 hours for 2--7 days or until clinical improvement is observed, followed by oral antiviral therapy to complete at least 10 days total therapy. Counseling Counseling of infected persons and their sex partners is critical to management of genital herpes. Counseling has two main goals: to help patients cope with the infection and to prevent sexual and perinatal transmission. Although initial counseling can be provided at the first visit, many patients benefit from learning about the chronic aspects of the disease after the acute illness subsides. Numerous resources, including the CDC National STD/HIV Hotline (tel: 800-227-8922), web sites (http://www.ashastd.org), and printed materials are available to assist patients and clinicians in counseling. HSV-infected persons may express anxiety about genital herpes that does not reflect the actual clinical severity of their disease; the psychological impact of infection often is substantial. Common concerns about genital herpes include the severity of initial clinical manifestations, recurrent episodes, sexual relationships and transmission to sex partners, and ability to bear healthy children. The misconception that HSV causes cancer should be dispelled, because the role of HSV-2 in cervical cancer is at most that of a cofactor, not a primary etiologic agent. Specific counseling messages should include the following information.
Management of Sex Partners The sex partners of patients who have genital herpes likely benefit from evaluation and counseling. Symptomatic sex partners should be evaluated and treated in the same manner as patients who have genital lesions. Asymptomatic sex partners of patients who have genital herpes should be questioned concerning histories of genital lesions, educated to recognize symptoms of herpes, and offered type-specific serologic testing for HSV infection. Special Considerations Allergy, Intolerance, and Adverse Reactions Allergic and other adverse reactions to acyclovir, valacyclovir, and famciclovir are rare. Desensitization to acyclovir has been described (42). HIV Infection Immunocompromised patients may have prolonged or severe episodes of genital, perianal, or oral herpes. Lesions caused by HSV are common among HIV-infected patients and may be severe, painful, and atypical. Episodic or suppressive therapy with oral antiviral agents is often beneficial.
In the doses recommended for treatment of genital herpes, acyclovir, valacyclovir, and famciclovir are safe for use in immunocompromised patients. For severe cases, initiating therapy with acyclovir 5--10 mg/kg body weight IV every 8 hours may be necessary. If lesions persist or recur in a patient receiving antiviral treatment, HSV resistance should be suspected and a viral isolate obtained for sensitivity testing. Such patients should be managed in consultation with a specialist, and alternate therapy should be administered. All acyclovir-resistant strains are resistant to valacyclovir and most are resistant to famciclovir. Foscarnet, 40 mg/kg body weight IV every 8 hours until clinical resolution is attained, is often effective for treatment of acyclovir-resistant genital herpes. Topical cidofovir gel 1% applied to the lesions once daily for 5 consecutive days also might be effective. This preparation is not commercially available and must be compounded at a pharmacy. Genital Herpes in Pregnancy Most mothers of infants who acquire neonatal herpes lack histories of clinically evident genital herpes. The risk for transmission to the neonate from an infected mother is high (30%--50%) among women who acquire genital herpes near the time of delivery and is low (<1%) among women with histories of recurrent herpes at term or who acquire genital HSV during the first half of pregnancy. However, because recurrent genital herpes is much more common than initial HSV infection during pregnancy, the proportion of neonatal HSV infections acquired from mothers with recurrent herpes remains high. Prevention of neonatal herpes depends both on preventing acquisition of genital HSV infection during late pregnancy and avoiding exposure of the infant to herpetic lesions during delivery. Women without known genital herpes should be counseled to avoid intercourse during the third trimester with partners known or suspected of having genital herpes. In addition, pregnant women without known orolabial herpes should be advised to avoid cunnilingus during the third trimester with partners known or suspected to have orolabial herpes. Some specialists believe type-specific serologic tests are useful to identify pregnant women at risk for HSV infection and to guide counseling with regard to the risk of acquiring genital herpes during pregnancy. Such testing and counseling may be especially important when a woman's sex partner has HSV infection. All pregnant women should be asked whether they have a history of genital herpes. At the onset of labor, all women should be questioned carefully about symptoms of genital herpes, including prodrome, and all women should be examined carefully for herpetic lesions. Women without symptoms or signs of genital herpes or its prodrome can deliver vaginally. Most specialists recommend that women with recurrent genital herpetic lesions at the onset of labor deliver by cesarean section to prevent neonatal herpes. However, abdominal delivery does not completely eliminate the risk for HSV transmission to the infant. The results of viral cultures during pregnancy in women with or without visible herpetic lesions do not predict viral shedding at the time of delivery, and therefore routine viral cultures of pregnant women with recurrent genital herpes are not recommended. The safety of systemic acyclovir, valacyclovir, and famciclovir therapy in pregnant women has not been established. Available data do not indicate an increased risk for major birth defects compared with the general population in women treated with acyclovir during the first trimester (43). These findings provide some assurance to women who have had prenatal exposure to acyclovir. However, available data are insufficient to reach definitive conclusions regarding the risks to the newborn associated with acyclovir treatment during pregnancy. The experience with prenatal exposure to valacyclovir and famciclovir is too limited to provide useful information on pregnancy outcomes. Acyclovir may be administered orally to pregnant women with first episode genital herpes or severe recurrent herpes and should be administered IV to pregnant women with severe HSV infection. Preliminary data suggest that acyclovir treatment late in pregnancy might reduce the frequency of cesarean sections among women who have recurrent genital herpes by diminishing the frequency of recurrences at term (44,45), and some specialists recommend such treatment. The risk for herpes is high in infants of women who acquire genital HSV in late pregnancy; such women should be managed in consultation with an HSV specialist. Some specialists recommend acyclovir therapy in this circumstance, some recommend routine cesarean section to reduce the risk for neonatal herpes, and others recommend both. Neonatal Herpes Infants exposed to HSV during birth, as documented by virologic testing or presumed by observation of lesions, should be followed carefully in consultation with a specialist. Some specialists recommend that such infants undergo surveillance cultures of mucosal surfaces to detect HSV infection before development of clinical signs of neonatal herpes. Some specialists recommend the use of acyclovir for infants born to women who acquired HSV near term, because the risk for neonatal herpes is high for these infants. All infants who have evidence of neonatal herpes should be promptly evaluated and treated with systemic acyclovir. The recommended regimen for infants treated for known or suspected neonatal herpes is acyclovir 20 mg/kg body weight IV every 8 hours for 21 days for disseminated and CNS disease, or 14 days for disease limited to the skin and mucous membranes. Granuloma Inguinale (Donovanosis)Granuloma inguinale is a genital ulcerative disease caused by the intracellular Gram-negative bacterium Calymmatobacterium granulomatis. The disease occurs rarely in the United States, although it is endemic in certain tropical and developing areas, including India; Papua, New Guinea; central Australia; and southern Africa. Clinically, the disease commonly presents as painless, progressive ulcerative lesions without regional lymphadenopathy. The lesions are highly vascular ("beefy red appearance") and bleed easily on contact. However, the clinical presentation can also include hypertrophic, necrotic, or sclerotic variants. The causative organism is difficult to culture, and diagnosis requires visualization of dark-staining Donovan bodies on tissue crush preparation or biopsy. The lesions may develop secondary bacterial infection or may be coinfected with another sexually transmitted pathogen. Treatment Treatment halts progression of lesions, although prolonged therapy may be required to permit granulation and reepithelialization of the ulcers. Relapse can occur 6--18 months after apparently effective therapy. Several antimicrobial regimens have been effective, but few controlled trials have been published.
Therapy should be continued at least 3 weeks or until all lesions have completely healed. Some specialists recommend addition of an aminoglycoside (e.g., gentamicin 1 mg/kg IV every 8 hours) to the above regimens if improvement is not evident within the first few days of therapy. Follow-Up Patients should be followed clinically until signs and symptoms have resolved. Management of Sex Partners Persons who have had sexual contact with a patient who has granuloma inguinale within the 60 days before onset of the patient's symptoms should be examined and offered therapy. However, the value of empiric therapy in the absence of clinical signs and symptoms has not been established. Special Considerations Pregnancy Pregnancy is a relative contraindication to the use of sulfonamides. Pregnant and lactating women should be treated with the erythromycin regimen, and consideration should be given to the addition of a parenteral aminoglycoside (e.g., gentamicin). Azithromycin may prove useful for treating granuloma inguinale in pregnancy, but published data are lacking. Doxycycline and ciprofloxacin are contraindicated in pregnant women. HIV Infection Persons with both granuloma inguinale and HIV infection should receive the same regimens as those who are HIV negative. Consideration should be given to the addition of a parenteral aminoglycoside (e.g., gentamicin). Lymphogranuloma VenereumLymphogranuloma venereum (LGV) is caused by C. trachomatis serovars L1, L2, or L3. The disease occurs rarely in the United States. The most common clinical manifestation of LGV among heterosexuals is tender inguinal and/or femoral lymphadenopathy that is most commonly unilateral. Women and homosexually active men may have proctocolitis or inflammatory involvement of perirectal or perianal lymphatic tissues resulting in fistulas and strictures. A self-limited genital ulcer sometimes occurs at the site of inoculation. However, by the time patients seek care, the ulcer usually has disappeared. The diagnosis of LGV is usually made serologically and by exclusion of other causes of inguinal lymphadenopathy or genital ulcers. Complement fixation titers >1:64 are consistent with the diagnosis of LGV. The diagnostic utility of serologic methods other than complement fixation is unknown. Treatment Treatment cures infection and prevents ongoing tissue damage, although tissue reaction can result in scarring. Buboes may require aspiration through intact skin or incision and drainage to prevent the formation of inguinal/femoral ulcerations. Doxycycline is the preferred treatment.
Some STD specialists believe azithromycin 1.0 g orally once weekly for 3 weeks is likely effective, although clinical data are lacking. Follow-Up Patients should be followed clinically until signs and symptoms have resolved. Management of Sex Partners Persons who have had sexual contact with a patient who has LGV within the 30 days before onset of the patient's symptoms should be examined, tested for urethral or cervical chlamydial infection, and treated. Special Considerations Pregnancy Pregnant and lactating women should be treated with erythromycin. Azithromycin may prove useful for treatment of LGV in pregnancy, but no published data are available regarding its safety and efficacy. Doxycycline is contraindicated in pregnant women. HIV Infection Persons with both LGV and HIV infection should receive the same regimens as those who are HIV-negative. Prolonged therapy may be required, and delay in resolution of symptoms may occur. SyphilisGeneral Principles Background Syphilis is a systemic disease caused by T. pallidum. Patients who have syphilis may seek treatment for signs or symptoms of primary infection (i.e., ulcer or chancre at the infection site), secondary infection (i.e., manifestations that include but are not limited to skin rash, mucocutaneous lesions, and lymphadenopathy), or tertiary infection (e.g., cardiac, ophthalmic, auditory abnormalities, and gummatous lesions). Latent infections (i.e., those lacking clinical manifestations) are detected by serologic testing. Latent syphilis acquired within the preceding year is referred to as early latent syphilis; all other cases of latent syphilis are either late latent syphilis or latent syphilis of unknown duration. Treatment for both late latent syphilis and tertiary syphilis theoretically may require a longer duration of therapy because organisms are dividing more slowly; however, the validity of this concept has not been assessed. Diagnostic Considerations and Use of Serologic Tests Darkfield examinations and direct fluorescent antibody tests of lesion exudate or tissue are the definitive methods for diagnosing early syphilis. A presumptive diagnosis is possible with the use of two types of serologic tests for syphilis: a) nontreponemal tests (e.g., Venereal Disease Research Laboratory [VDRL] and Rapid Plasma Reagin [RPR]) and b) treponemal tests (e.g., fluorescent treponemal antibody absorbed [FTA-ABS] and T. pallidum particle agglutination [TP-PA]). The use of only one type of serologic test is insufficient for diagnosis, because false-positive nontreponemal test results may occur secondary to various medical conditions. Nontreponemal test antibody titers usually correlate with disease activity, and results should be reported quantitatively. A fourfold change in titer, equivalent to a change of two dilutions (e.g., from 1:16 to 1:4 or from 1:8 to 1:32), is considered necessary to demonstrate a clinically significant difference between two nontreponemal test results that were obtained using the same serologic test. Sequential serologic tests in individual patients should be performed by using the same testing method (e.g., VDRL or RPR), preferably by the same laboratory. The VDRL and RPR are equally valid assays, but quantitative results from the two tests cannot be compared directly because RPR titers often are slightly higher than VDRL titers. Nontreponemal tests usually become nonreactive with time after treatment; however, in some patients, nontreponemal antibodies can persist at a low titer for a long period of time, sometimes for the life of the patient. This response is referred to as the "serofast reaction." Most patients who have reactive treponemal tests will have reactive tests for the remainder of their lives, regardless of treatment or disease activity. However, 15%--25% of patients treated during the primary stage revert to being serologically nonreactive after 2--3 years. Treponemal test antibody titers correlate poorly with disease activity and should not be used to assess treatment response. Some HIV-infected patients can have atypical serologic test results (i.e., unusually high, unusually low, or fluctuating titers). For such patients, when serologic tests and clinical syndromes suggestive of early syphilis do not correspond with one another, use of other tests (e.g., biopsy and direct microscopy) should be considered. However, for most HIV-infected patients, serologic tests are accurate and reliable for the diagnosis of syphilis and for following the response to treatment. No test can be used alone to diagnose neurosyphilis. The VDRL-CSF is highly specific, but it is insensitive. Most other tests are both insensitive and nonspecific and must be interpreted in relation to other test results and the clinical assessment. Therefore, the diagnosis of neurosyphilis usually depends on various combinations of reactive serologic test results, abnormalities of cerebrospinal fluid (CSF) cell count or protein, or a reactive VDRL-CSF with or without clinical manifestations. The CSF leukocyte count usually is elevated (>5 WBCs/mm3) in patients with neurosyphilis; this count also is a sensitive measure of the effectiveness of therapy. The VDRL-CSF is the standard serologic test for CSF, and when reactive in the absence of substantial contamination of CSF with blood, it is considered diagnostic of neurosyphilis. However, the VDRL-CSF may be nonreactive when neurosyphilis is present. Some specialists recommend performing an FTA-ABS test on CSF. The CSF FTA-ABS is less specific (i.e., yields more false-positive results) for neurosyphilis than the VDRL-CSF, but the test is highly sensitive. Therefore, some specialists believe that a negative CSF FTA-ABS test excludes neurosyphilis. Treatment Penicillin G, administered parenterally, is the preferred drug for treatment of all stages of syphilis. The preparation(s) used (i.e., benzathine, aqueous procaine, or aqueous crystalline), the dosage, and the length of treatment depend on the stage and clinical manifestations of disease. However, neither combinations of benzathine penicillin and procaine penicillin nor oral penicillin preparations are considered appropriate for the treatment of syphilis. The efficacy of penicillin for the treatment of syphilis was well established through clinical experience before the value of randomized controlled clinical trials was recognized. Therefore, almost all the recommendations for the treatment of syphilis are based on the opinions of persons knowledgeable about STDs and are reinforced by case series, clinical trials, and 50 years of clinical experience. Parenteral penicillin G is the only therapy with documented efficacy for syphilis during pregnancy. Pregnant women with syphilis in any stage who report penicillin allergy should be desensitized and treated with penicillin. Skin testing for penicillin allergy may be useful in pregnant women; such testing also is useful in other patients (see Management of Patients Who Have a History of Penicillin Allergy). The Jarisch-Herxheimer reaction is an acute febrile reaction frequently accompanied by headache, myalgia, and other symptoms that usually occurs within the first 24 hours after any therapy for syphilis. Patients should be informed about this possible adverse reaction. The Jarisch-Herxheimer reaction occurs most often among patients who have early syphilis. Antipyretics may be used, but they have not been proven to prevent this reaction. The Jarisch-Herxheimer reaction may induce early labor or cause fetal distress in pregnant women. This concern should not prevent or delay therapy (see Syphilis During Pregnancy). Sexual transmission of T. pallidum occurs only when mucocutaneous syphilitic lesions are present; such manifestations are uncommon after the first year of infection. However, persons exposed sexually to a patient who has syphilis in any stage should be evaluated clinically and serologically according to the following recommendations.
For identification of at-risk partners, the time periods before treatment are a) 3 months plus duration of symptoms for primary syphilis, b) 6 months plus duration of symptoms for secondary syphilis, and c) 1 year for early latent syphilis. Primary and Secondary Syphilis Parenteral penicillin G has been used effectively for more than 50 years to achieve clinical resolution (i.e., healing of lesions and prevention of sexual transmission) and to prevent late sequelae. However, no comparative trials have been adequately conducted to guide the selection of an optimal penicillin regimen (i.e., the dose, duration, and preparation). Substantially fewer data are available for nonpenicillin regimens.
NOTE: Recommendations for treating pregnant women and HIV-infected patients for syphilis are discussed in separate sections.
After the newborn period, children with syphilis should have a CSF examination to detect asymptomatic neurosyphilis, and birth and maternal medical records should be reviewed to assess whether such children have congenital or acquired syphilis (see Congenital Syphilis). Children with acquired primary or secondary syphilis should be evaluated (e.g., through consultation with child-protection services) (see Sexual Assault or Abuse of Children) and treated by using the following pediatric regimen.
Other Management Considerations All patients who have syphilis should be tested for HIV infection. In geographic areas in which the prevalence of HIV is high, patients who have primary syphilis should be retested for HIV after 3 months if the first HIV test result was negative. Patients who have syphilis and who also have symptoms or signs suggesting neurologic disease (e.g., meningitis) or ophthalmic disease (e.g., uveitis) should have an evaluation that includes CSF analysis and ocular slit-lamp examination. Treatment should be guided by the results of this evaluation. Invasion of CSF by T. pallidum accompanied by CSF abnormalities is common among adults who have primary or secondary syphilis. However, neurosyphilis develops in only a limited number of patients after treatment with the penicillin regimens recommended for primary and secondary syphilis. Therefore, unless clinical signs or symptoms of neurologic or ophthalmic involvement are present, CSF analysis is not recommended for routine evaluation of patients who have primary or secondary syphilis. Follow-Up Treatment failure can occur with any regimen. However, assessing response to treatment often is difficult, and definitive criteria for cure or failure have not been established. Nontreponemal test titers may decline more slowly for patients who previously had syphilis. Patients should be reexamined clinically and serologically 6 months and 12 months following treatment; more frequent evaluation may be prudent if follow-up is uncertain. Patients who have signs or symptoms that persist or recur or who have a sustained fourfold increase in nontreponemal test titer (i.e., compared with the maximum or baseline titer at the time of treatment) probably failed treatment or were reinfected. These patients should be re-treated and reevaluated for HIV infection. Because treatment failure usually cannot be reliably distinguished from reinfection with T. pallidum, a CSF analysis also should be performed. A recent clinical trial demonstrated that 15% of patients with early syphilis treated with the recommended therapy will not achieve a two dilution decline in nontreponemal titer used to define response at 1 year following treatment. Failure of nontreponemal test titers to decline fourfold within 6 months after therapy for primary or secondary syphilis is indicative of probable treatment failure. Persons for whom titers remain serofast should be reevaluated for HIV infection. Optimal management of such patients is unclear. At a minimum, these patients should have additional clinical and serologic follow-up. HIV-infected patients should be evaluated more frequently (i.e., at 3-month intervals instead of 6-month intervals). If additional follow-up cannot be ensured, re-treatment is recommended. Because treatment failure may be the result of unrecognized CNS infection, some specialists recommend CSF examination in such situations. When patients are re-treated, most STD specialists recommend administering weekly injections of benzathine penicillin G 2.4 million units IM for 3 weeks, unless CSF examination indicates that neurosyphilis is present. In rare instances, serologic titers do not decline despite a negative CSF examination and a repeated course of therapy. Additional therapy or repeated CSF examinations are not warranted in these circumstances. Management of Sex Partners See General Principles, Management of Sex Partners. Special Considerations Penicillin Allergy. Data to support the use of alternatives to penicillin in the treatment of early syphilis are limited. However, several therapies might be considered effective in nonpregnant, penicillin-allergic patients who have primary or secondary syphilis. Doxycycline (100 mg orally twice daily for 14 days) and tetracycline (500 mg four times daily for 14 days) are regimens that have been used for many years. Compliance is likely to be better with doxycycline than tetracycline, because tetracycline can cause gastrointestinal side effects. Although limited clinical studies, along with biologic and pharmacologic evidence, suggest that ceftriaxone is effective for treating early syphilis, the optimal dose and duration of ceftriaxone therapy have not been defined. However, some specialists recommend 1 gram daily either IM or IV for 8--10 days. Preliminary data suggest that azithromycin may be effective as a single oral dose of 2 grams. Because the efficacy of these therapies is not well documented, close follow-up of persons receiving these therapies is essential. The use of any of these therapies in HIV-infected persons has not been studied; the use of doxycycline, ceftriaxone, and azithromycin among such persons must be undertaken with caution. Patients with penicillin allergy whose compliance with therapy or follow-up cannot be ensured should be desensitized and treated with benzathine penicillin. Skin testing for penicillin allergy may be useful in some circumstances in which the reagents and expertise are available to perform the test adequately (see Management of Patients Who Have a History of Penicillin Allergy). Pregnancy. Pregnant patients who are allergic to penicillin should be desensitized and treated with penicillin (see Management of Patients Who Have a History of Penicillin Allergy and Syphilis During Pregnancy). HIV Infection. See Syphilis Among HIV-Infected Persons. Latent syphilis is defined as syphilis characterized by seroreactivity without other evidence of disease. Patients who have latent syphilis and who acquired syphilis within the preceding year are classified as having early latent syphilis. Patients can be diagnosed as having early latent syphilis if, within the year preceding the evaluation, they had a) a documented seroconversion, b) unequivocal symptoms of primary or secondary syphilis, or c) a sex partner documented to have primary, secondary, or early latent syphilis. Patients who have latent syphilis of unknown duration should be managed as if they have late latent syphilis. Nontreponemal serologic titers usually are higher during early latent syphilis than late latent syphilis. However, early latent syphilis cannot be reliably distinguished from late latent syphilis solely on the basis of nontreponemal titers. All patients with latent syphilis should have careful examination of all accessible mucosal surfaces (i.e., the oral cavity, the perineum in women, and underneath the foreskin in uncircumcised men) to evaluate for internal mucosal lesions. All patients who have syphilis should be tested for HIV infection. Treatment of latent syphilis usually does not affect transmission and is intended to prevent occurrence or progression of late complications. Although clinical experience supports the effectiveness of penicillin in achieving these goals, limited evidence is available for guidance in choosing specific regimens. The following regimens are recommended for nonallergic patients who have normal CSF examinations (if performed).
After the newborn period, children with syphilis should have a CSF examination to exclude neurosyphilis. In addition, birth and maternal medical records should be reviewed to assess whether children have congenital or acquired syphilis (see Congenital Syphilis). Older children with acquired latent syphilis should be evaluated as described for adults and treated using the following pediatric regimens (see Sexual Assault or Abuse of Children). These regimens are for non-allergic children who have acquired syphilis and who have normal CSF examination results.
Other Management Considerations All patients who have latent syphilis should be evaluated clinically for evidence of tertiary disease (e.g., aortitis, gumma, and iritis). Patients who have syphilis and who demonstrate any of the following criteria should have a prompt CSF examination:
If dictated by circumstances and patient preferences, a CSF examination may be performed for patients who do not meet these criteria. Some specialists recommend performing a CSF examination on all patients who have latent syphilis and a nontreponemal serologic test of >1:32. The risk of neurosyphilis in this circumstance is unknown. If a CSF examination is performed and the results indicate abnormalities consistent with neurosyphilis, the patient should be treated for neurosyphilis (see Neurosyphilis). If a patient misses a dose of penicillin in the course of weekly therapy for late syphilis, the appropriate course of action is unclear. Pharmacologic considerations suggest that an interval of 10--14 days between doses of benzathine penicillin for late syphilis or latent syphilis of unknown duration might be acceptable before restarting the sequence of injections. Missed doses should not be considered acceptable for pregnant patients receiving therapy for late latent syphilis; pregnant women who miss any dose of therapy must repeat the full course of therapy. Follow-Up. Quantitative nontreponemal serologic tests should be repeated at 6, 12, and 24 months. Patients with a normal CSF examination should be re-treated for latent syphilis if a) titers increase fourfold, b) an initially high titer (>1:32) fails to decline at least fourfold (i.e., two dilutions) within 12--24 months of therapy, or c) signs or symptoms attributable to syphilis develop. In rare instances, despite a negative CSF examination and a repeated course of therapy, serologic titers may still not decline. In these circumstances, the need for additional therapy or repeated CSF examinations is unclear. Management of Sex Partners. See General Principles, Management of Sex Partners. Special Considerations Penicillin Allergy. The effectiveness of alternatives to penicillin in the treatment of latent syphilis has not been well documented. Nonpregnant patients allergic to penicillin who have clearly defined early latent syphilis should respond to therapies recommended as alternatives to penicillin for the treatment of primary and secondary syphilis (see Treatment of Primary and Secondary Syphilis). The only acceptable alternatives for the treatment of late latent syphilis or latent syphilis of unknown duration are doxycycline (100 mg orally twice daily) or tetracycline (500 mg orally four times daily) both for 28 days. These therapies should be used only in conjunction with close serologic and clinical follow-up. The efficacy of these alternative regimens in HIV-infected persons has not been studied, and thus must be considered with caution. Pregnancy. Pregnant patients who are allergic to penicillin should be desensitized and treated with penicillin (see Management of Patients Who Have a History of Penicillin Allergy and Syphilis During Pregnancy). HIV Infection. See Syphilis Among HIV-Infected Persons. Tertiary Syphilis Tertiary syphilis refers to gumma and cardiovascular syphilis, but not to all neurosyphilis. Patients who are not allergic to penicillin and have no evidence of neurosyphilis should be treated with the following regimen.
Other Management Considerations Patients who have symptomatic late syphilis should be given a CSF examination before therapy is initiated. Some providers treat all patients who have cardiovascular syphilis with a neurosyphilis regimen. The complete management of patients who have cardiovascular or gummatous syphilis is beyond the scope of these guidelines. These patients should be managed in consultation with an infectious diseases specialist. Follow-Up. Limited information is available concerning clinical response and follow-up of patients who have tertiary syphilis. Management of Sex Partners. See General Principles, Management of Sex Partners. Special Considerations Penicillin Allergy. Patients allergic to penicillin should be treated according to treatment regimens recommended for late latent syphilis. Pregnancy. Pregnant patients who are allergic to penicillin should be desensitized, if necessary, and treated with penicillin (see Management of Patients Who Have a History of Penicillin Allergy and Syphilis During Pregnancy). HIV Infection. See Syphilis Among HIV-Infected Persons. Treatment CNS disease can occur during any stage of syphilis. A patient who has clinical evidence of neurologic involvement with syphilis (e.g., cognitive dysfunction, motor or sensory deficits, ophthalmic or auditory symptoms, cranial nerve palsies, and symptoms or signs of meningitis) should have a CSF examination. Syphilitic uveitis or other ocular manifestations frequently are associated with neurosyphilis; patients with these symptoms should be treated according to the recommendations for patients with neurosyphilis. A CSF examination should be performed for all such patients to identify those with abnormalities who should have follow-up CSF examinations to assess treatment response. Patients who have neurosyphilis or syphilitic eye disease (e.g., uveitis, neuroretinitis, and optic neuritis) should be treated with the following regimen.
If compliance with therapy can be ensured, patients may be treated with the following alternative regimen.
The durations of the recommended and alternative regimens for neurosyphilis are shorter than that of the regimen used for late syphilis in the absence of neurosyphilis. Therefore, some specialists administer benzathine penicillin, 2.4 million units IM once per week for up to 3 weeks after completion of these neurosyphilis treatment regimens to provide a comparable total duration of therapy. Other Management Considerations Other considerations in the management of patients who have neurosyphilis are as follows.
Follow-Up. If CSF pleocytosis was present initially, a CSF examination should be repeated every 6 months until the cell count is normal. Follow-up CSF examinations also can be used to evaluate changes in the VDRL-CSF or CSF protein after therapy; however, changes in these two parameters are slower, and persistent abnormalities may be less important. If the cell count has not decreased after 6 months, or if the CSF is not normal after 2 years, re-treatment should be considered. Management of Sex Partners. See General Principles, Management of Sex Partners. Special Considerations Penicillin Allergy. Ceftriaxone can be used as an alternative treatment for patients with neurosyphilis, although the possibility of cross-reactivity between this agent and penicillin exists. Some specialists recommend ceftriaxone 2 grams daily either IM or IV for 10--14 days. Other regimens have not been adequately evaluated for treatment of neurosyphilis. Therefore, if concern exists regarding the safety of ceftriaxone for a patient with neurosyphilis, the patient should obtain skin testing to confirm penicillin allergy and, if necessary, be desensitized and managed in consultation with a specialist. Pregnancy. Pregnant patients who are allergic to penicillin should be desensitized, if necessary, and treated with penicillin (see Syphilis During Pregnancy). HIV Infection. See Syphilis Among HIV-Infected Patients. Syphilis Among HIV-Infected Persons Diagnostic Considerations Unusual serologic responses have been observed among HIV-infected persons who have syphilis. Most reports have involved serologic titers that were higher than expected, but false-negative serologic test results and delayed appearance of seroreactivity also have been reported. However, aberrant serologic responses are uncommon, and most specialists believe that both treponemal and non-treponemal serologic tests for syphilis can be interpreted in the usual manner for most patients who are coinfected with T. pallidum and HIV. When clinical findings are suggestive of syphilis, but serologic tests are nonreactive or the interpretation is unclear, alternative tests (e.g., biopsy of a lesion, darkfield examination, or direct fluorescent antibody staining of lesion material) may be useful for diagnosis. Neurosyphilis should be considered in the differential diagnosis of neurologic disease in HIV-infected persons. Treatment Compared with HIV-negative patients, HIV-positive patients who have early syphilis may be at increased risk for neurologic complications and may have higher rates of treatment failure with currently recommended regimens. The magnitude of these risks, although not defined precisely, is likely minimal. No treatment regimens for syphilis have been demonstrated to be more effective in preventing neurosyphilis in HIV-infected patients than the syphilis regimens recommended for HIV-negative patients. Careful follow-up after therapy is essential. Primary and Secondary Syphilis Among HIV-Infected Persons Treatment Treatment with benzathine penicillin G, 2.4 million units IM in a single dose is recommended. Some specialists recommend additional treatments (e.g., benzathine penicillin G administered at 1-week intervals for 3 weeks, as recommended for late syphilis) in addition to benzathine penicillin G 2.4 million units IM. Other Management Considerations Because CSF abnormalities (e.g., mononuclear pleocytosis and elevated protein levels) are common in patients with early syphilis and in persons with HIV infection, the clinical and prognostic significance of such CSF abnormalities in HIV-infected persons with primary or secondary syphilis is unknown. Although most HIV-infected persons respond appropriately to standard benzathine penicillin therapy, some specialists recommend intensified therapy when CNS syphilis is suspected in these persons. Therefore, some specialists recommend CSF examination before treatment of HIV-infected persons with early syphilis, with follow-up CSF examination following treatment in persons with initial abnormalities. Follow-Up. HIV-infected patients should be evaluated clinically and serologically for treatment failure at 3, 6, 9, 12, and 24 months after therapy. Although of unproven benefit, some specialists recommend a CSF examination 6 months after therapy. HIV-infected patients who meet the criteria for treatment failure should be managed in the same manner as HIV-negative patients (i.e., a CSF examination and re-treatment). CSF examination and re-treatment also should be strongly considered for patients whose nontreponemal test titers do not decrease fourfold within 6--12 months of therapy. Most specialists would re-treat patients with benzathine penicillin G administered as three doses of 2.4 million units IM each at weekly intervals, if CSF examinations are normal. Special Considerations Penicillin Allergy. Penicillin-allergic patients who have primary or secondary syphilis and HIV infection should be managed according to the recommendations for penicillin-allergic, HIV-negative patients. The use of alternatives to penicillin has not been well studied in HIV-infected patients. Latent Syphilis Among HIV-Infected Persons Diagnostic Considerations HIV-infected patients who have early latent syphilis should be managed and treated according to the recommendations for HIV-negative patients who have primary and secondary syphilis. HIV-infected patients who have either late latent syphilis or syphilis of unknown duration should have a CSF examination before treatment. Treatment Patients with late latent syphilis or syphilis of unknown duration and a normal CSF examination can be treated with benzathine penicillin G, at weekly doses of 2.4 million units for 3 weeks. Patients who have CSF consistent with neurosyphilis should be treated and managed as patients who have neurosyphilis (see Neurosyphilis). Follow-Up. Patients should be evaluated clinically and serologically at 6, 12, 18, and 24 months after therapy. If, at any time, clinical symptoms develop or nontreponemal titers rise fourfold, a repeat CSF examination should be performed and treatment administered accordingly. If in 12--24 months the nontreponemal titer does not decline fourfold, the CSF examination should be repeated and treatment administered accordingly. Special Considerations Penicillin Allergy. Patients with penicillin allergy whose compliance with therapy or follow-up cannot be ensured should be desensitized and treated with penicillin (see Management of Patients Who Have a History of Penicillin Allergy). The efficacy of alternative non-penicillin regimens in HIV-infected persons has not been studied. All women should be screened serologically for syphilis at the first prenatal visit. In populations in which prenatal care is not optimal, RPR-card test screening and treatment (if the RPR-card test is reactive) should be performed at the time a pregnancy is confirmed. For communities and populations in which the prevalence of syphilis is high or for patients at high risk, serologic testing should be performed twice during the third trimester, at 28 weeks' gestation, and at delivery in addition to routine early screening. Some states mandate screening at delivery for all women. Any woman who delivers a stillborn infant after 20 weeks' gestation should be tested for syphilis. No infant should leave the hospital if maternal serologic status has not been determined at least once during pregnancy and preferably again at delivery. Diagnostic Considerations Seropositive pregnant women should be considered infected unless an adequate treatment history is documented in the medical records and sequential serologic antibody titers have declined. Treatment Penicillin is effective for preventing maternal transmission to the fetus and for treating fetal infection. Evidence is insufficient to determine whether the specific, recommended penicillin regimens are optimal.
Other Management Considerations Some specialists recommend additional therapy in some patients. A second dose of benzathine penicillin 2.4 million units IM may be administered 1 week after the initial dose for women who have primary, secondary, or early latent syphilis. In the second half of pregnancy, management and counseling may be facilitated by a sonographic fetal evaluation for congenital syphilis, but this should not delay therapy. Sonographic signs of fetal syphilis (i.e., hepatomegaly, ascites, and hydrops) indicate a greater risk for fetal treatment failure; such cases should be managed in consultation with obstetric specialists. Evidence is insufficient to recommend specific regimens for these situations. Women treated for syphilis during the second half of pregnancy are at risk for premature labor and/or fetal distress if the treatment precipitates the Jarisch-Herxheimer reaction. These women should be advised to seek obstetric attention after treatment if they notice any contractions or decrease in fetal movements. Although stillbirth is a rare complication of treatment, concern about this complication should not delay necessary treatment. All patients who have syphilis should be offered testing for HIV infection. Follow-Up. Coordinated prenatal care, treatment follow-up, and syphilis case management are important in the management of pregnant women with syphilis. Serologic titers should be repeated in the third trimester and at delivery. Serologic titers may be checked monthly in women at high risk for reinfection or in geographic areas in which the prevalence of syphilis is high. The clinical and antibody response should be appropriate for the stage of disease. Most women will deliver before their serologic response to treatment can be assessed definitively. Management of Sex Partners. See General Principles, Management of Sex Partners. Special Considerations Penicillin Allergy. No alternatives to penicillin have been proved effective for treatment of syphilis during pregnancy. Pregnant women who have a history of penicillin allergy should be desensitized and treated with penicillin. Skin testing may be helpful (see Management of Patients Who Have a History of Penicillin Allergy). Tetracycline and doxycycline should not used during pregnancy. Erythromycin should not be used, because it does not reliably cure an infected fetus. Data are insufficient to recommend azithromycin or ceftriaxone. HIV Infection. See Syphilis Among HIV-Infected Patients. Congenital SyphilisEffective prevention and detection of congenital syphilis depends on the identification of syphilis in pregnant women and, therefore, on the routine serologic screening of pregnant women during the first prenatal visit. Serologic testing and a sexual history also should be obtained at 28 weeks of gestation and at delivery in communities and populations in which the risk for congenital syphilis is high. Moreover, as part of the management of pregnant women who have syphilis, information concerning treatment of sex partners should be obtained to assess the risk for reinfection. All pregnant women who have syphilis should be tested for HIV infection. Routine screening of newborn sera or umbilical cord blood is not recommended. Serologic testing of the mother's serum is preferred over testing infant serum, because the serologic tests performed on infant serum can be nonreactive if the mother's serologic test result is of low titer or if the mother was infected late in pregnancy. No infant or mother should leave the hospital unless the maternal serologic status has been documented at least once during pregnancy and preferably again at delivery. Evaluation and Treatment of Infants in the First Month of LifeThe diagnosis of congenital syphilis is complicated by the transplacental transfer of maternal nontreponemal and treponemal immunoglobulin G (IgG) antibodies to the fetus. This transfer of antibodies makes the interpretation of reactive serologic tests for syphilis in infants difficult. Treatment decisions often must be made on the basis of a) identification of syphilis in the mother; b) adequacy of maternal treatment; c) presence of clinical, laboratory, or radiographic evidence of syphilis in the infant; and d) comparison of maternal (at delivery) and infant nontreponemal serologic titers utilizing the same test and preferably the same laboratory. All infants born to mothers who have reactive nontreponemal and treponemal test results should be evaluated with a quantitative nontreponemal serologic test (RPR or VDRL) performed on infant serum, because umbilical cord blood can become contaminated with maternal blood and could yield a false-positive result. Conducting a treponemal test (i.e., TP-PA or FTA-ABS) on a newborn's serum is not necessary. Currently, no commercially available IgM test can be recommended. All infants born to women who have reactive serologic tests for syphilis should be examined thoroughly for evidence of congenital syphilis (e.g., nonimmune hydrops, jaundice, hepatosplenomegaly, rhinitis, skin rash, and/or pseudoparalysis of an extremity). Pathologic examination of the placenta or umbilical cord using specific fluorescent antitreponemal antibody staining is suggested. Darkfield microscopic examination or direct fluorescent antibody staining of suspicious lesions or body fluids (e.g., nasal discharge) also should be performed. The following scenarios describe the evaluation and treatment of infants for congenital syphilis. Scenario 1. Infants with proven or highly probable disease
Recommended Evaluation
If more than 1 day of therapy is missed, the entire course should be restarted. Data are insufficient regarding the use of other antimicrobial agents (e.g., ampicillin). When possible, a full 10-day course of penicillin is preferred, even if ampicillin was initially provided for possible sepsis. The use of agents other than penicillin requires close serologic follow-up to assess adequacy of therapy. In all other situations, the maternal history of infection with T. pallidum and treatment for syphilis must be considered when evaluating and treating the infant. Scenario 2. Infants who have a normal physical examination and a serum quantitative nontreponemal serologic titer the same or less than fourfold the maternal titer and the
Recommended Evaluation
A complete evaluation is not necessary if 10 days of parenteral therapy is administered. However, such evaluation may be useful; a lumbar puncture may document CSF abnormalities that would prompt close follow-up. Other tests (e.g., CBC, platelet count, and bone radiographs) may be performed to further support a diagnosis of congenital syphilis. If a single dose of benzathine penicillin G is used, then the infant must be fully evaluated (i.e., through CSF examination, long-bone radiographs, and CBC with platelets), the full evaluation must be normal, and follow-up must be certain. If any part of the infant's evaluation is abnormal or not performed, or if the CSF analysis is rendered uninterpretable because of contamination with blood, then a 10-day course of penicillin is required.¶
NOTE: Some specialists prefer the 10 days of parenteral therapy if the mother has untreated early syphilis at delivery. Scenario 3. Infants who have a normal physical examination and a serum quantitative nontreponemal serologic titer the same or less than fourfold the maternal titer and the
Recommended Evaluation No evaluation is required.
Scenario 4. Infants who have a normal physical examination and a serum quantitative nontreponemal serologic titer the same or less than fourfold the maternal titer and the
Recommended Evaluation No evaluation is required.
Evaluation and Treatment of Older Infants and ChildrenChildren who are identified as having reactive serologic tests for syphilis after the neonatal period (i.e., at >1 month of age) should have maternal serology and records reviewed to assess whether the child has congenital or acquired syphilis (for acquired syphilis, see Primary and Secondary Syphilis and Latent Syphilis). Any child at risk for congenital syphilis should receive a full evaluation and testing for HIV infection. Recommended Evaluation
Any child who is suspected of having congenital syphilis or who has neurologic involvement should be treated with aqueous penicillin G. Some specialists also suggest giving these patients a single dose of benzathine penicillin G, 50,000 units/kg IM following the 10-day course of IV aqueous penicillin. Follow-UpAll seroreactive infants (or infants whose mothers were seroreactive at delivery) should receive careful follow-up examinations and serologic testing (i.e., a nontreponemal test) every 2--3 months until the test becomes nonreactive or the titer has decreased fourfold. Nontreponemal antibody titers should decline by 3 months of age and should be nonreactive by 6 months of age if the infant was not infected (i.e., if the reactive test result was caused by passive transfer of maternal IgG antibody) or was infected but adequately treated. The serologic response after therapy may be slower for infants treated after the neonatal period. If these titers are stable or increase after 6--12 months of age, the child should be evaluated (e.g., given a CSF examination) and treated with a 10-day course of parenteral penicillin G. Treponemal tests should not be used to evaluate treatment response because the results for an infected child can remain positive despite effective therapy. Passively transferred maternal treponemal antibodies can be present in an infant until age 15 months. A reactive treponemal test after age 18 months is diagnostic of congenital syphilis. If the nontreponemal test is nonreactive at this time, no further evaluation or treatment is necessary. If the nontreponemal test is reactive at age 18 months, the infant should be fully (re)evaluated and treated for congenital syphilis. Infants whose initial CSF evaluations are abnormal should undergo a repeat lumbar puncture approximately every 6 months until the results are normal. A reactive CSF VDRL test or abnormal CSF indices that cannot be attributed to other ongoing illness requires re-treatment for possible neurosyphilis. Follow-up of children treated for congenital syphilis after the newborn period should be conducted as is recommended for neonates. Special ConsiderationsPenicillin Allergy Infants and children who require treatment for syphilis but who have a history of penicillin allergy or develop an allergic reaction presumed secondary to penicillin should be desensitized, if necessary, and then treated with penicillin (see Management of Patients With a History of Penicillin Allergy). Data are insufficient regarding the use of other antimicrobial agents (e.g., ceftriaxone); if a nonpenicillin agent is used, close serologic and CSF follow-up are indicated. HIV Infection Data are insufficient regarding whether infants who have congenital syphilis and whose mothers are coinfected with HIV require different evaluation, therapy, or follow-up for syphilis than is recommended for all infants. Management of Patients Who Have a History of Penicillin AllergyNo proven alternatives to penicillin are available for treating neurosyphilis, congenital syphilis, or syphilis in pregnant women. Penicillin is also recommended for use, whenever possible, in HIV-infected patients. Of the adult U.S. population, 3%--10% have experienced urticaria, angioedema, or anaphylaxis (i.e., upper airway obstruction, bronchospasm, or hypotension) after penicillin therapy. Re-administration of penicillin to these patients can cause severe, immediate reactions. Because anaphylactic reactions to penicillin can be fatal, every effort should be made to avoid administering penicillin to penicillin-allergic patients, unless they undergo acute desensitization to eliminate anaphylactic sensitivity. An estimated 10% of persons who report a history of severe allergic reactions to penicillin remain allergic. With the passage of time after an allergic reaction to penicillin, most persons who have had a severe reaction stop expressing penicillin-specific immunoglobulin E (IgE). These persons can be treated safely with penicillin. The results of many investigations indicate that skin testing with the major and minor determinants can reliably identify persons at high risk for penicillin reactions. Although these reagents are easily generated and have been available for >30 years, only benzylpenicilloyl poly-L-lysine (Pre-Pen® [i.e., the major determinant]) and penicillin G are available commercially. Testing with only the major determinant and penicillin G identifies an estimated 90%--97% of the currently allergic patients. However, because skin testing without the minor determinants would still miss 3%--10% of allergic patients and because serious or fatal reactions can occur among these minor-determinant-positive patients, specialists suggest exercising caution when the full battery of skin-test reagents is not available (Box 1). RecommendationsIf the full battery of skin-test reagents is available, including the major and minor determinants (see Penicillin Allergy Skin Testing), patients who report a history of penicillin reaction and are skin-test negative can receive conventional penicillin therapy. Skin-test-positive patients should be desensitized. If the full battery of skin-test reagents, including the minor determinants, is not available, the patient should be skin tested using benzylpenicilloyl poly-L-lysine (i.e., the major determinant) and penicillin G. Patients who have positive test results should be desensitized. Some specialists suggest that persons who have negative test results should be regarded as probably allergic and should be desensitized. Others suggest that those with negative skin-test results can be test-dosed gradually with oral penicillin in a monitored setting in which treatment for anaphylactic reaction can be provided. Penicillin Allergy Skin TestingPatients at high risk for anaphylaxis, including those who a) have a history of penicillin-related anaphylaxis, asthma, or other diseases that would make anaphylaxis more dangerous and b) are being treated with beta-adrenergic blocking agents, should be tested with 100-fold dilutions of the full-strength skin-test reagents before being tested with full-strength reagents. In these situations, patients should be tested in a monitored setting in which treatment for an anaphylactic reaction is available. If possible, the patient should not have taken antihistamines recently (e.g., chlorpheniramine maleate or terfenadine during the preceding 24 hours, diphenhydramine HCl or hydroxyzine during the preceding 4 days, or astemizole during the preceding 3 weeks). Procedures Dilute the antigens either a) 100-fold for preliminary testing if the patient has had a life-threatening reaction to penicillin or b) 10-fold if the patient has had another type of immediate, generalized reaction to penicillin within the preceding year. Epicutaneous (Prick) Tests Duplicate drops of skin-test reagent are placed on the volar surface of the forearm. The underlying epidermis is pierced with a 26-gauge needle without drawing blood. An epicutaneous test is positive if the average wheal diameter after 15 minutes is 4 mm larger than that of negative controls; otherwise, the test is negative. The histamine controls should be positive to ensure that results are not falsely negative because of the effect of antihistaminic drugs. Intradermal Test If epicutaneous tests are negative, duplicate 0.02 mL intradermal injections of negative control and antigen solutions are made into the volar surface of the forearm using a 26- or 27-gauge needle on a syringe. The crossed diameters of the wheals induced by the injections should be recorded. An intradermal test is positive if the average wheal diameter 15 minutes after injection is >2 mm larger than the initial wheal size and also is >2 mm larger than the negative controls. Otherwise, the tests are negative. Desensitization Patients who have a positive skin test to one of the penicillin determinants can be desensitized (Table 1). This is a straightforward, relatively safe procedure that can be done orally or IV. Although the two approaches have not been compared, oral desensitization is regarded as safer to use and easier to perform. Patients should be desensitized in a hospital setting because serious IgE-mediated allergic reactions rarely can occur. Desensitization usually can be completed in approximately 4 hours, after which the first dose of penicillin is administered. After desensitization, patients must be maintained on penicillin continuously for the duration of the course of therapy. Diseases Characterized by Urethritis and CervicitisManagement of Male Patients Who Have UrethritisUrethritis is caused by an infection characterized by urethral discharge of mucopurulent or purulent material and sometimes by dysuria or urethral pruritis. Asymptomatic infections are common. The principal bacterial pathogens of proven clinical importance in men who have urethritis are N. gonorrhoeae and C. trachomatis. Testing to determine the specific etiology is recommended because both chlamydia and gonorrhea are conditions that are reportable to state health departments, and a specific diagnosis may enhance partner notification and improve compliance with treatment, especially in the exposed partner. If diagnostic tools (e.g., a Gram stain and microscope) are unavailable, patients should be treated for both infections. The additional antibiotic exposure and expense of treating a person who has nongonococcal urethritis (NGU) for both infections also should encourage the health-care provider to make a specific diagnosis. Nucleic acid amplification tests enable detection of N. gonorrhoeae and C. trachomatis on all specimens. These tests are more sensitive than traditional culture techniques for C. trachomatis and are the preferred method for the detection of this organism. EtiologyNGU is diagnosed if Gram-negative intracellular diplococci cannot be identified on urethral smears. C. trachomatis is a frequent cause (i.e., 15%--55% of cases); however, the prevalence differs by age group, with lower prevalence of this organism among older men. The proportion of NGU cases caused by chlamydia has been declining gradually. Complications of NGU among men infected with C. trachomatis include epididymitis and Reiter's syndrome. Documentation of chlamydia infection is important because of the need for partner referral for evaluation and treatment. The etiology of most cases of nonchlamydial NGU is unknown. Ureaplasma urealyticum and Mycoplasma genitalium have been implicated as causes of NGU in some studies. Specific diagnostic tests for these organisms are not indicated, because the detection of these organisms is often difficult and would not alter therapy. T. vaginalis and HSV sometimes cause NGU. Diagnostic and treatment procedures for these organisms are reserved for situations in which these infections are suspected (e.g., contact with trichomoniasis and genital lesions suggestive of genital herpes) or when NGU is not responsive to therapy. Confirmed UrethritisClinicians should document that urethritis is present. Urethritis can be documented on the basis of any of the following signs.
If none of these criteria is present, then treatment should be deferred, and the patient should be tested for N. gonorrhoeae and C. trachomatis and followed closely if test results are negative. If the results demonstrate infection with either N. gonorrhoeae or C. trachomatis, the appropriate treatment should be given and sex partners referred for evaluation and treatment. Empiric treatment of symptoms without documentation of urethritis is recommended only for patients at high risk for infection who are unlikely to return for a follow-up evaluation. Such patients should be treated for gonorrhea and chlamydia. Partners of patients treated empirically should be evaluated and treated. Management of Patients Who Have Nongonococcal UrethritisDiagnosis All patients who have urethritis should be evaluated for the presence of gonococcal and chlamydial infection. Testing for chlamydia is strongly recommended because of the increased utility and availability of highly sensitive and specific testing methods, and because a specific diagnosis may enhance partner notification and improve compliance with treatment, especially in the exposed partner. Treatment Treatment should be initiated as soon as possible after diagnosis. Single-dose regimens have the advantage of improved compliance and of DOT. To improve compliance, the medication should be provided in the clinic or health-care provider's office.
Follow-Up for Patients Who Have Urethritis Patients should be instructed to return for evaluation if symptoms persist or recur after completion of therapy. Symptoms alone, without documentation of signs or laboratory evidence of urethral inflammation, are not a sufficient basis for re-treatment. Patients should be instructed to abstain from sexual intercourse until 7 days after therapy is initiated. Partner Referral Patients should refer for evaluation and treatment all sex partners within the preceding 60 days. Because a specific diagnosis may facilitate partner referral, testing for gonorrhea and chlamydia is encouraged. Recurrent and Persistent Urethritis Objective signs of urethritis should be present before initiation of antimicrobial therapy. Effective regimens have not been identified for treating patients who do not have objective signs of urethritis but who have persistent symptoms after treatment. Patients who have persistent or recurrent urethritis should be re-treated with the initial regimen if they did not comply with the treatment regimen or if they were reexposed to an untreated sex partner. Otherwise, a culture of an intra-urethral swab specimen and a first-void urine specimen for T. vaginalis should be performed. Some cases of recurrent urethritis following doxycycline treatment may be caused by tetracycline-resistant U. urealyticum. Urologic examinations usually do not reveal a specific etiology. If the patient was compliant with the initial regimen and re-exposure can be excluded, the following regimen is recommended.
Special Considerations HIV Infection Gonococcal urethritis, chlamydial urethritis, and nongoncoccal, nonchlamydial urethritis may facilitate HIV transmission. Patients who have NGU and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. Management of Patients Who Have Mucopurulent Cervicitis (MPC)MPC is characterized by a purulent or mucopurulent endocervical exudate visible in the endocervical canal or in an endocervical swab specimen. Some specialists also diagnose MPC on the basis of easily induced cervical bleeding. Although some specialists consider an increased number of polymorphonuclear leukocytes on endocervical Gram stain as being useful in the diagnosis of MPC, this criterion has not been standardized, has a low positive-predictive value (PPV), and is not available in some settings. MPC often is asymptomatic, but some women have an abnormal vaginal discharge and vaginal bleeding (e.g., after sexual intercourse). MPC can be caused by C. trachomatis or N. gonorrhoeae; however, in most cases neither organism can be isolated. MPC can persist despite repeated courses of antimicrobial therapy. Because relapse or reinfection with C. trachomatis or N. gonorrhoeae usually does not occur in persons with persistent cases of MPC, other non-microbiologic determinants (e.g., inflammation in the zone of ectopy) might be involved. Patients who have MPC should be tested for C. trachomatis and for N. gonorrhoeae with the most sensitive and specific test available. However, MPC is not a sensitive predictor of infection with these organisms; most women who have C. trachomatis or N. gonorrhoeae do not have MPC. Treatment The results of sensitive tests for C. trachomatis or N. gonorrhoeae (e.g., culture or nucleic acid amplification tests) should determine the need for treatment, unless the likelihood of infection with either organism is high or the patient is unlikely to return for treatment. Empiric treatment should be considered for a patient who is suspected of having gonorrhea and/or chlamydia if a) the prevalences of these infections are high in the patient population and b) the patient might be difficult to locate for treatment. If relapse and reinfection have been excluded, management options of persistent MPC are undefined. For such persons, additional antimicrobial therapy may be of minimal benefit. Follow-Up Follow-up should be conducted as recommended for the infections for which a woman is being treated. If symptoms persist, women should be instructed to return for reevaluation and to abstain from sexual intercourse, even if they have completed the prescribed therapy. Management of Sex Partners Management of sex partners of women treated for MPC should be appropriate for the identified or suspected STD. Partners should be notified, examined, and treated for the STD identified or suspected in the index patient. Because a microbiologic test of cure usually is not recommended, patients and their sex partners should abstain from sexual intercourse until therapy is completed (i.e., 7 days after a single-dose regimen or after completion of a 7-day regimen). Special Considerations HIV Infection Patients who have MPC and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. Chlamydial InfectionsIn the United States, chlamydial genital infection occurs frequently among sexually active adolescents and young adults. Asymptomatic infection is common among both men and women. Sexually active adolescent women should be screened for chlamydial infection at least annually, even if symptoms are not present. Annual screening of all sexually active women aged 20--25 years is also recommended, as is screening of older women with risk factors (e.g., those who have a new sex partner and those with multiple sex partners). An appropriate sexual risk assessment should always be conducted and may indicate more frequent screening for some women. Chlamydial Infections in Adolescents and Adults Several important sequelae can result from C. trachomatis infection in women; the most serious of these include pelvic inflammatory disease (PID), ectopic pregnancy, and infertility. Some women who have apparently uncomplicated cervical infection already have subclinical upper-reproductive--tract infection. A recent investigation of patients in a health maintenance organization demonstrated that screening and treatment of cervical infection can reduce the likelihood of PID. Treatment Treating infected patients prevents transmission to sex partners. In addition, treatment of chlamydia in pregnant women usually prevents transmission of C. trachomatis to infants during birth. Treatment of sex partners helps to prevent reinfection of the index patient and infection of other partners. Coinfection with C. trachomatis often occurs among patients who have gonococcal infection; therefore, presumptive treatment of such patients for chlamydia is appropriate (see Gonococcal Infection, Dual Therapy for Gonococcal and Chlamydial Infections). The following recommended treatment regimens and alternative regimens cure infection and usually relieve symptoms.
The results of clinical trials indicate that azithromycin and doxycycline are equally efficacious (46,47). These investigations were conducted primarily in populations in which follow-up was encouraged and adherence to a 7-day regimen was good. Azithromycin should always be available to health-care providers to treat patients for whom compliance is in question. In populations that have erratic health-care-seeking behavior, poor compliance with treatment, or unpredictable follow-up, azithromycin may be more cost-effective because it enables the provision of single-dose DOT. Doxycycline costs less than azithromycin, and it has been used extensively for a longer period. Erythromycin is less efficacious than either azithromycin or doxycycline, and gastrointestinal side effects frequently discourage patients from complying with this regimen. Ofloxacin is similar in efficacy to doxycycline and azithromycin, but it is more expensive to use and offers no advantage with regard to the dosage regimen. Levofloxacin has not been evaluated for treatment of C. trachomatis infection in clinical trials, but because its pharmacology and in vitro microbiologic activity are similar to that of ofloxacin, levofloxacin may be substituted in doses of 500 mg once a day for 7 days. Other quinolones either are not reliably effective against chlamydial infection or have not been adequately evaluated. To maximize compliance with recommended therapies, medications for chlamydial infections should be dispensed on site, and the first dose should be directly observed. To minimize further transmission of infection, patients treated for chlamydia should be instructed to abstain from sexual intercourse for 7 days after single-dose therapy or until completion of a 7-day regimen. To minimize the risk for reinfection, patients also should be instructed to abstain from sexual intercourse until all of their sex partners are treated. Follow-Up Patients do not need to be retested for chlamydia after completing treatment with doxycycline or azithromycin unless symptoms persist or reinfection is suspected. A test of cure may be considered 3 weeks after completion of treatment with erythromycin. The validity of chlamydial culture testing at <3 weeks after completion of therapy to identify patients who did not respond to therapy has not been established. False-negative results can occur resulting from infections involving small numbers of chlamydial organisms. In addition, nonculture tests conducted at <3 weeks after completion of therapy for patients who were treated successfully could yield false-positive results because of continued excretion of dead organisms. A high prevalence of C. trachomatis infection is found in women who have had chlamydial infection in the preceding several months. Most post-treatment infections result from reinfection, often occurring because patient's sex partners were not treated or because the patient resumed sex among a network of persons with a high prevalence of infection. Repeat infection confers an elevated risk of PID and other complications when compared with initial infection. Therefore, recently infected women are a high priority for repeat testing for C. trachomatis. For these reasons, clinicians and health-care agencies should consider advising all women with chlamydial infection to be rescreened 3--4 months after treatment. Some specialists believe rescreening is an especially high priority for adolescents. Providers are also strongly encouraged to rescreen all women treated for chlamydial infection whenever they next present for care within the following 12 months, regardless of whether the patient believes that her sex partners were treated. Rescreening is distinct from early retesting to detect therapeutic failure (test-of-cure). Except in pregnant women, test-of-cure is not recommended for persons treated with the recommended regimens, unless therapeutic compliance is in question. Management of Sex Partners Patients should be instructed to refer their sex partners for evaluation, testing, and treatment. The following recommendations on exposure intervals are based on limited evaluation. Sex partners should be evaluated, tested, and treated if they had sexual contact with the patient during the 60 days preceding onset of symptoms in the patient or diagnosis of chlamydia. The most recent sex partner should be evaluated and treated even if the time of the last sexual contact was >60 days before symptom onset or diagnosis. Patients should be instructed to abstain from sexual intercourse until they and their sex partners have completed treatment. Abstinence should be continued until 7 days after a single-dose regimen or after completion of a 7-day regimen. Timely treatment of sex partners is essential for decreasing the risk for reinfecting the index patient. Special Considerations Pregnancy. Doxycycline and ofloxacin are contraindicated in pregnant women. However, clinical experience and preliminary data suggest that azithromycin is safe and effective (48,49). Repeat testing (preferably by culture) 3 weeks after completion of therapy with the following regimens is recommended for all pregnant women, because these regimens may not be highly efficacious and the frequent side effects of erythromycin might discourage patient compliance with this regimen.
NOTE: Erythromycin estolate is contraindicated during pregnancy because of drug-related hepatotoxicity. HIV Infection. Patients who have chlamydial infection and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. Chlamydial Infections Among Infants Prenatal screening of pregnant women can prevent chlamydial infection among neonates. Pregnant women aged <25 years are at high risk for infection. Local or regional prevalence surveys of chlamydial infection can be conducted to confirm the validity of using these recommendations in particular settings. C. trachomatis infection of neonates results from perinatal exposure to the mother's infected cervix. The prevalence of C. trachomatis infection among pregnant women does not vary by race/ethnicity or socioeconomic status. Neonatal ocular prophylaxis with silver nitrate solution or antibiotic ointments does not prevent perinatal transmission of C. trachomatis from mother to infant. However, ocular prophylaxis with those agents does prevent gonococcal ophthalmia and therefore should be continued (see Prevention of Ophthalmia Neonatorum). Initial C. trachomatis perinatal infection involves mucous membranes of the eye, oropharynx, urogenital tract, and rectum. C. trachomatis infection in neonates is most often recognized by conjunctivitis that develops 5--12 days after birth. Chlamydia is the most frequent identifiable infectious cause of ophthalmia neonatorum. C. trachomatis also is a common cause of subacute, afebrile pneumonia with onset from 1--3 months of age. Asymptomatic infections also can occur in the oropharynx, genital tract, and rectum of neonates. Ophthalmia Neonatorum Caused by C. trachomatis A chlamydial etiology should be considered for all infants aged <30 days who have conjunctivitis. Diagnostic Considerations Sensitive and specific methods used to diagnose chlamydial ophthalmia in the neonate include both tissue culture and nonculture tests (e.g., direct fluorescent antibody tests, enzyme immunoassays, and nucleic acid amplification tests). Specimens must contain conjunctival cells, not exudate alone. Specimens for culture isolation and nonculture tests should be obtained from the everted eyelid using a dacron-tipped swab or the swab specified by the manufacturer's test kit. A specific diagnosis of C. trachomatis infection confirms the need for treatment not only for the neonate, but also for the mother and her sex partner(s). Ocular exudate from infants being evaluated for chlamydial conjunctivitis should also be tested for N. gonorrhoeae.
Topical antibiotic therapy alone is inadequate for treatment of chlamydial infection and is unnecessary when systemic treatment is administered. Follow-Up The efficacy of erythromycin treatment is approximately 80%; a second course of therapy may be required, and follow-up of infants to determine whether treatment was effective is recommended. The possibility of concomitant chlamydial pneumonia should be considered. Management of Mothers and Their Sex Partners The mothers of infants who have chlamydial infection and the sex partners of these women should be evaluated and treated (see Chlamydial Infection in Adolescents and Adults). Infant Pneumonia Caused by C. trachomatis Characteristic signs of chlamydial pneumonia in infants include a) a repetitive staccato cough with tachypnea and b) hyperinflation and bilateral diffuse infiltrates on a chest radiograph. Wheezing is rare, and infants are typically afebrile. Peripheral eosinophilia sometimes occurs in infants who have chlamydial pneumonia. Because clinical presentations differ, initial treatment and diagnostic tests should encompass C. trachomatis for all infants aged 1--3 months who possibly have pneumonia. Diagnostic Considerations Specimens for chlamydial testing should be collected from the nasopharynx. Tissue culture is the definitive standard for chlamydial pneumonia. Nonculture tests (e.g., EIA, direct flourescent antibody [DFA], and nucleic acid amplification [NAATs]) can be used, although nonculture tests of nasopharyngeal specimens produce lower sensitivity and specificity than nonculture tests of ocular specimens. Tracheal aspirates and lung biopsy specimens, if collected, should be tested for C. trachomatis. Because of the delay in obtaining test results for chlamydia, the decision to include an agent in the antibiotic regimen that is active against C. trachomatis must frequently be based on clinical and radiologic findings. The results of tests for chlamydial infection assist in the management of an infant's illness and determine the need for treating the mother and her sex partner(s).
Follow-Up The effectiveness of erythromycin in treating pneumonia caused by C. trachomatis is approximately 80%; a second course of therapy may be required. Follow-up of infants is recommended to determine whether the pneumonia has resolved. Some infants with chlamydial pneumonia have abnormal pulmonary function tests later in childhood. Management of Mothers and Their Sex Partners Mothers of infants who have chlamydial infection and the sex partners of these women should be evaluated and treated according to the recommended treatment of adults for chlamydial infections (see Chlamydial Infection in Adolescents and Adults). Infants Born to Mothers Who Have Chlamydial Infection Infants born to mothers who have untreated chlamydia are at high risk for infection; however, prophylatic antibiotic treatment is not indicated, and the efficacy of such treatment is unknown. Infants should be monitored to ensure appropriate treatment if infection develops. Chlamydial Infections Among Children Sexual abuse must be considered a cause of chlamydial infection in preadolescent children, although perinatally transmitted C. trachomatis infection of the nasopharynx, urogenital tract, and rectum may persist for >1 year (see Sexual Assault or Abuse of Children). Diagnostic Considerations Nonculture tests for chlamydia (e.g., non-amplified probes [EIA and DFA]) should not be used because of the possibility of false-positive test results. With respiratory tract specimens, false-positive results can occur because of cross-reaction of test reagents with Chlamydia pneumoniae; with genital and anal specimens, false-positive results occur because of cross-reaction with fecal flora.
Other Management Considerations See Sexual Assault or Abuse of Children Follow-Up. Follow-up cultures are necessary to ensure that treatment has been effective. Gonococcal InfectionsGonococcal Infections in Adolescents and Adults In the United States, an estimated 600,000 new N. gonorrhoeae infections occur each year. Most infections among men produce symptoms that cause them to seek curative treatment soon enough to prevent serious sequelae, but this may not be soon enough to prevent transmission to others. Among women, many infections do not produce recognizable symptoms until complications (e.g., PID) have occurred. Both symptomatic and asymptomatic cases of PID can result in tubal scarring that can lead to infertility or ectopic pregnancy. Because gonococcal infections among women often are asymptomatic, an important component of gonorrhea control in the United States continues to be the screening of women at high risk for STDs. Dual Therapy for Gonococcal and Chlamydial Infections Patients infected with N. gonorrhoeae often are coinfected with C. trachomatis; this finding led to the recommendation that patients treated for gonococcal infection also be treated routinely with a regimen effective against uncomplicated genital C. trachomatis infection. Routine dual therapy without testing for chlamydia can be cost-effective for populations in which chlamydial infection accompanies 10%--30% of gonococcal infections, because the cost of therapy for chlamydia (e.g., $0.50-- $1.50 for doxycycline) is less than the cost of testing. Some specialists believe that the routine use of dual therapy has resulted in substantial decreases in the prevalence of chlamydial infection. Because most gonococci in the United States are susceptible to doxycycline and azithromycin, routine cotreatment may hinder the development of antimicrobial-resistant N. gonorrhoeae. Since the introduction of dual therapy, the prevalence of chlamydial infection has decreased in some populations, and simultaneous testing for chlamydial infection has become quicker, more sensitive, and more widely available. In geographic areas in which the rates of coinfection are low, some clinicians might prefer a highly sensitive test for chlamydia rather than treating presumptively. However, presumptive treatment is indicated for patients who may not return for test results. Quinolone-resistant N. gonorrhoeae (QRNG) QRNG continues to spread, making the treatment of gonorrhea with quinolones inadvisable in many areas. QRNG is common in parts of Asia and the Pacific. In the United States, QRNG is becoming increasingly common in areas on the West Coast. Of 5,461 isolates collected by CDC's Gonococcal Isolate Surveillance Project (GISP) during 2000, 19 (0.4%) had minimum inhibitory concentrations (MICs) >1.0 µg/mL to ciprofloxacin. GISP indicated that the resistant isolates made up 0.2% of the samples collected from the 25 cities within the continental United States and Alaska; however, such isolates comprised 14.3% of the Honolulu GISP sample. Because of these and other data, quinolones are no longer recommended for the treatment of gonorrhea in the State of Hawaii and should not be used to treat infections that may have been acquired in Asia or the Pacific (including Hawaii). Recent data from several GISP sites in California demonstrate an increased prevalence of QRNG; therefore, the use of fluoroquinolones in California is probably inadvisable. Clinicians should obtain a recent travel history, including histories from sex partners, in those persons with gonorrhea to ensure appropriate antibiotic therapy. Resistance of N. gonorrhoeae to fluoroquinolones and other antimicrobials is expected to continue to spread; therefore, surveillance for antimicrobial resistance is crucial for guiding therapy recommendations. The GISP, which samples approximately 3% of all U.S. men who have gonococcal infections, is a mainstay of surveillance. However, surveillance by clinicians is also important. Clinicians who diagnose N. gonorrhoeae infection in a person who was treated with a recommended regimen and who likely has not been re-exposed should perform culture and susceptibility testing of relevant clinical specimens and report the case to the local health department. Uncomplicated Gonococcal Infections of the Cervix, Urethra, and Rectum
Cefixime has an antimicrobial spectrum similar to that of ceftriaxone, but the 400-mg oral dose does not provide as high nor as sustained a bactericidal level as that provided by the 125-mg dose of ceftriaxone. In published clinical trials, the 400-mg dose cured 97.4% of uncomplicated urogenital and anorectal gonococcal infections (50). The advantage of cefixime is that it can be administered orally. Ceftriaxone in a single injection of 125 mg provides sustained, high bactericidal levels in the blood. Extensive clinical experience indicates that ceftriaxone is safe and effective for the treatment of uncomplicated gonorrhea at all anatomic sites, curing 99.1% of uncomplicated urogenital and anorectal infections in published clinical trials (50). Ciprofloxacin is effective against most strains of N. gonorrhoeae in the United States (excluding Hawaii). At a dose of 500 mg, ciprofloxacin provides sustained bactericidal levels in the blood; in published clinical trials, it has cured 99.8% of uncomplicated urogenital and anorectal infections. Ciprofloxacin is safe, inexpensive, and can be administered orally. Ofloxacin also is effective against most strains of N. gonorrhoeae in the United States (excluding Hawaii), and it has favorable pharmacokinetics. The 400-mg oral dose has been effective for treatment of uncomplicated urogenital and anorectal infections, curing 98.6% of infections in published clinical trials. Levofloxacin, the active l-isomer of ofloxacin, can be used in place of ofloxacin as a single dose of 250 mg.
Many other antimicrobials are active against N. gonorrhoeae, but none have substantial advantages over the recommended regimens. Azithromycin 2 g orally is effective against uncomplicated gonococcal infection, but it is expensive and causes gastrointestinal distress, so it is not recommended for treatment of gonorrhea. At an oral dose of 1 g, azithromycin is insufficiently effective and is not recommended. Uncomplicated Gonococcal Infections of the Pharynx Gonococcal infections of the pharynx are more difficult to eradicate than infections at urogenital and anorectal sites. Few antimicrobial regimens can reliably cure >90% of infections. Although chlamydial coinfection of the pharynx is unusual, coinfection at genital sites sometimes occurs. Therefore, treatment for both gonorrhea and chlamydia is recommended.
Follow-Up Patients who have uncomplicated gonorrhea and who are treated with any of the recommended regimens need not return for a test to confirm that they are cured. Patients who have symptoms that persist after treatment should be evaluated by culture for N. gonorrhoeae, and any gonococci isolated should be tested for antimicrobial susceptibility. Infections identified after treatment with one of the recommended regimens usually result from reinfection rather than treatment failure, indicating a need for improved patient education and referral of sex partners. Persistent urethritis, cervicitis, or proctitis also may be caused by C. trachomatis and other organisms. Patients should be instructed to refer their sex partners for evaluation and treatment. All sex partners of patients who have N. gonorrhoeae infection should be evaluated and treated for N. gonorrhoeae and C. trachomatis infections if their last sexual contact with the patient was within 60 days before onset of symptoms or diagnosis of infection in the patient. If a patient's last sexual intercourse was >60 days before onset of symptoms or diagnosis, the patient's most recent sex partner should be treated. Patients should be instructed to avoid sexual intercourse until therapy is completed and until they and their sex partners no longer have symptoms. Special Considerations Allergy, Intolerance, and Adverse Reactions Persons who cannot tolerate cephalosporins or quinolones should be treated with spectinomycin. Because spectinomycin is unreliable (i.e., only 52% effective) against pharyngeal infections, patients who have suspected or known pharyngeal infection should have a pharyngeal culture evaluated 3--5 days after treatment to verify eradication of infection. Pregnancy Pregnant women should not be treated with quinolones or tetracyclines. Those infected with N. gonorrhoeae should be treated with a recommended or alternate cephalosporin. Women who cannot tolerate a cephalosporin should be administered a single, 2-g dose of spectinomycin IM. Either erythromycin or amoxicillin is recommended for treatment of presumptive or diagnosed C. trachomatis infection during pregnancy (see Chlamydial Infection). Administration of Quinolones to Adolescents Fluoroquinolones have not been recommended for persons aged <18 years because studies have indicated that they can damage articular cartilage in some young animals. However, no joint damage attributable to quinolone therapy has been observed in children treated with prolonged ciprofloxacin regimens. Thus, children who weigh >45 kg can be treated with any regimen recommended for adults (See Gonococcal Infections). HIV Infection Patients who have gonococcal infection and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. Gonococcal Conjunctivitis In the only published study of the treatment of gonococcal conjunctivitis among U.S. adults, all 12 study participants responded to a single 1-g IM injection of ceftriaxone (51). The following recommendations reflect the opinions of consultants knowledgeable in the field of STDs.
NOTE: Consider lavage of the infected eye with saline solution once. Management of Sex Partners Patients should be instructed to refer their sex partners for evaluation and treatment (see Gonococcal Infection, Management of Sex Partners). Disseminated Gonococcal Infection (DGI) DGI results from gonococcal bacteremia. DGI often results in petechial or pustular acral skin lesions, asymmetrical arthralgia, tenosynovitis, or septic arthritis. The infection is complicated occasionally by perihepatitis and rarely by endocarditis or meningitis. Some strains of N. gonorrhoeae that cause DGI may cause minimal genital inflammation. No recent studies of the treatment of DGI among U.S. adults have been published. The following recommendations reflect the opinions of consultants knowledgeable in the STD field. No treatment failures have been reported using the following recommended regimen. Treatment Hospitalization is recommended for initial therapy, especially for patients who may not comply with treatment, for those in whom diagnosis is uncertain, and for those who have purulent synovial effusions or other complications. Patients should be examined for clinical evidence of endocarditis and meningitis. Patients treated for DGI should be treated presumptively for concurrent C. trachomatis infection, unless appropriate testing excludes this infection.
Management of Sex Partners Gonococcal infection often is asymptomatic in sex partners of patients who have DGI. As with uncomplicated gonococcal infections, patients should be instructed to refer their sex partners for evaluation and treatment (see Gonococcal Infection, Management of Sex Partners). Gonococcal Meningitis and Endocarditis
Therapy for meningitis should be continued for 10--14 days; therapy for endocarditis should be continued for at least 4 weeks. Treatment of complicated DGI should be undertaken in consultation with a specialist. Management of Sex Partners Patients should be instructed to refer their sex partners for evaluation and treatment (see Gonococcal Infection, Management of Sex Partners). Gonococcal Infections Among Infants Gonococcal infection among infants usually results from exposure to infected cervical exudate at birth. It is usually an acute illness that becomes manifest 2--5 days after birth. The prevalence of infection among infants depends on the prevalence of infection among pregnant women, on whether pregnant women are screened for gonorrhea, and on whether newborns receive ophthalmia prophylaxis. The most severe manifestations of N. gonorrhoeae infection in newborns are ophthalmia neonatorum and sepsis, including arthritis and meningitis. Less severe manifestations include rhinitis, vaginitis, urethritis, and inflammation at sites of fetal monitoring. Ophthalmia Neonatorum Caused by N. gonorrhoeae In the United States, although N. gonorrhoeae causes ophthalmia neonatorum less often than C. trachomatis and nonsexually transmitted agents, identifying and treating this infection is especially important because ophthalmia neonatorum can result in perforation of the globe of the eye and blindness. Diagnostic Considerations Infants at increased risk for gonococcal ophthalmia are those who do not receive ophthalmia prophylaxis and those whose mothers have had no prenatal care or whose mothers have a history of STDs or substance abuse. Gonococcal ophthalmia is strongly suspected when intracellular Gram-negative diplococci are identified in conjunctival exudate, justifying presumptive treatment for gonorrhea after appropriate cultures for N. gonorrhoeae are obtained. Appropriate chlamydial testing should be done simultaneously. Presumptive treatment for N. gonorrhoeae may be indicated for newborns who are at increased risk for gonococcal ophthalmia and who have conjunctivitis but do not have gonococci in a Gram-stained smear of conjunctival exudate. In all cases of neonatal conjunctivitis, conjunctival exudate should be cultured for N. gonorrhoeae and tested for antibiotic susceptibility before a definitive diagnosis is made. A definitive diagnosis is important because of the public health and social consequences of a diagnosis of gonorrhea. Nongonococcal causes of neonatal ophthalmia include Moraxella catarrhalis and other Neisseria species that are indistinguishable from N. gonorrhoeae on Gram-stained smear but can be differentiated in the microbiology laboratory.
NOTE: Topical antibiotic therapy alone is inadequate and is unnecessary if systemic treatment is administered. Other Management Considerations Simultaneous infection with C. trachomatis should be considered when a patient does not improve after treatment. Both mother and infant should be tested for chlamydial infection at the same time that gonorrhea testing is conducted (see Ophthalmia Neonatorum Caused by C. trachomatis). Ceftriaxone should be administered cautiously to hyperbilirubinemic infants, especially those born prematurely. Follow-Up Infants who have gonococcal ophthalmia should be hospitalized and evaluated for signs of disseminated infection (e.g., sepsis, arthritis, and meningitis). One dose of ceftriaxone is adequate therapy for gonococcal conjunctivitis. Management of Mothers and Their Sex Partners The mothers of infants who have gonococcal infection and the mothers' sex partners should be evaluated and treated according to the recommendations for treating gonococcal infections in adults (see Gonococcal Infection in Adolescents and Adults). Disseminated Gonococcal Infection and Gonococcal Scalp Abscesses in Newborns Sepsis, arthritis, and meningitis (or any combination of these conditions) are rare complications of neonatal gonococcal infection. Localized gonococcal infection of the scalp can result from fetal monitoring through scalp electrodes. Detection of gonococcal infection in neonates who have sepsis, arthritis, meningitis, or scalp abscesses requires cultures of blood, CSF, and joint aspirate on chocolate agar. Specimens obtained from the conjunctiva, vagina, oropharynx, and rectum that are cultured on gonococcal selective medium are useful for identifying the primary site(s) of infection, especially if inflammation is present. Positive Gram-stained smears of exudate, CSF, or joint aspirate provide a presumptive basis for initiating treatment for N. gonorrhoeae. Diagnoses based on Gram-stained smears or presumptive identification of cultures should be confirmed with definitive tests on culture isolates.
Prophylactic Treatment for Infants Whose Mothers Have Gonococcal Infection Infants born to mothers who have untreated gonorrhea are at high risk for infection.
Other Management Considerations Both mother and infant should be tested for chlamydial infection. Follow-Up Follow-up examination is not required. Management of Mothers and Their Sex Partners The mothers of infants who have gonococcal infection and the mothers' sex partners should be evaluated and treated according to the recommendations for treatment of gonococcal infections in adults (see Gonococcal Infection). Gonococcal Infections Among Children Sexual abuse is the most frequent cause of gonococcal infection in pre-adolescent children (see Sexual Assault or Abuse of Children). Vaginitis is the most common manifestation of gonococcal infection in preadolescent girls. PID following vaginal infection is probably less common in children than among adults. Among sexually abused children, anorectal and pharyngeal infections with N. gonorrhoeae are common and frequently asymptomatic. Diagnostic Considerations Because of the legal implications of a diagnosis of N. gonorrhoeae infection in a child, only standard culture procedures for the isolation of N. gonorrhoeae should be used for children. Nonculture gonococcal tests for gonococci (e.g., Gram-stained smear, DNA probes, EIA, and NAAT tests) should not be used alone; none of these tests have been approved by FDA for use with specimens obtained from the oropharynx, rectum, or genital tract of children. Specimens from the vagina, urethra, pharynx, or rectum should be streaked onto selective media for isolation of N. gonorrhoeae, and all presumptive isolates of N. gonorrhoeae should be identified definitively by at least two tests that involve different principles (e.g., biochemical, enzyme substrate, or serologic). Isolates should be preserved to enable additional or repeated testing.
NOTE: Fluoroquinolones have not been recommended for persons aged <18 years because they have damaged articular cartilage in young animals. However, no such joint damage clearly attributable to quinolone therapy has been observed in children, even in those receiving multiple-dose regimens.
Follow-Up Follow-up cultures are unnecessary if ceftriaxone is used. If spectinomycin is used to treat pharyngitis, a follow-up culture is necessary to ensure that treatment was effective. Other Management Considerations Only parenteral cephalosporins are recommended for use in children. Ceftriaxone is approved for all gonococcal infections in children; cefotaxime is approved for gonococcal ophthalmia only. Oral cephalosporins used for treatment of gonococcal infections in children have not been adequately evaluated. All children who have gonococcal infections should be evaluated for coinfection with syphilis and C. trachomatis. (For a discussion of concerns regarding sexual assault, refer to Sexual Assault or Abuse of Children.) Ophthalmia Neonatorum Prophylaxis To prevent gonococcal ophthalmia neonatorum, a prophylactic agent should be instilled into the eyes of all newborn infants; this procedure is required by law in most states. All of the recommended prophylactic regimens in this section prevent gonococcal ophthalmia. However, the efficacy of these preparations in preventing chlamydial ophthalmia is less clear, and they do not eliminate nasopharyngeal colonization by C. trachomatis. The diagnosis and treatment of gonococcal and chlamydial infections in pregnant women is the best method for preventing neonatal gonococcal and chlamydial disease. Not all women, however, receive prenatal care. Ocular prophylaxis is warranted because it can prevent sight-threatening gonococcal ophthalmia and because it is safe, easy to administer, and inexpensive. Prophylaxis
One of these recommended preparations should be instilled into both eyes of every neonate as soon as possible after delivery. If prophylaxis is delayed (i.e., not administered in the delivery room), a monitoring system should be established to ensure that all infants receive prophylaxis. All infants should be administered ocular prophylaxis, regardless of whether they are delivered vaginally or by cesarean section. Single-use tubes or ampules are preferable to multiple-use tubes. Bacitracin is not effective. Use of povidone iodine has not been studied adequately. Diseases Characterized by Vaginal DischargeManagement of Patients Who Have Vaginal InfectionsVaginal infection is usually characterized by a vaginal discharge or vulvar itching and irritation; a vaginal odor may be present. The three diseases most frequently associated with vaginal discharge are trichomoniasis (caused by T. vaginalis), bacterial vaginosis (caused by a replacement of the normal vaginal flora by an overgrowth of anaerobic microorganisms, mycoplasmas, and Gardnerella vaginalis), and candidiasis (usually caused by Candida albicans). MPC caused by C. trachomatis or N. gonorrhoeae can sometimes cause vaginal discharge. Although vulvovaginal candidiasis and bacterial vaginosis are not usually transmitted sexually, they are included in this section because these infections are often diagnosed in women being evaluated for STDs. The cause of vaginal infection can be diagnosed by pH and microscopic examination of the discharge. The pH of the vaginal secretions can be determined by narrow-range pH paper for the elevated pH (>4.5) typical of BV or trichomoniasis. Discharge can be examined by diluting one sample in one to two drops of 0.9% normal saline solution on one slide and a second sample in 10% potassium hydroxide (KOH) solution. An amine odor detected before or immediately after applying KOH suggests BV. A cover slip is placed on the slides, and they are examined under a microscope at low- and high-dry power. The motile T. vaginalis or the clue cells of BV usually are identified easily in the saline specimen. The yeast or pseudohyphae of Candida species are more easily identified in the KOH specimen. However, their absence does not preclude candidal or trichomonal infection, because several studies have demonstrated the presence of these pathogens by using polymerase chain reaction (PCR) after a negative microscopic exam. The presence of objective signs of external vulvar inflammation in the absence of vaginal pathogens, along with a minimal amount of discharge, suggests the possibility of mechanical, chemical, allergic, or other noninfectious irritation of the vulva. Culture for T. vaginalis is more sensitive than microscopic examination. Laboratory testing fails to identify the cause of vaginitis among a minority of women. Bacterial VaginosisBV is a clinical syndrome resulting from replacement of the normal H2O2-producing Lactobacillus sp. in the vagina with high concentrations of anaerobic bacteria (e.g., Prevotella sp. and Mobiluncus sp.), G. vaginalis, and Mycoplasma hominis. BV is the most prevalent cause of vaginal discharge or malodor; however, up to 50% of women with BV may not report symptoms of BV. The cause of the microbial alteration is not fully understood. BV is associated with having multiple sex partners, douching, and lack of vaginal lactobacilli; it is unclear whether BV results from acquisition of a sexually transmitted pathogen. Women who have never been sexually active are rarely affected. Treatment of the male sex partner has not been beneficial in preventing the recurrence of BV. Diagnostic Considerations BV can be diagnosed by the use of clinical or Gram-stain criteria. Clinical criteria require three of the following symptoms or signs:
When a Gram stain is used, determining the relative concentration of the bacterial morphotypes characteristic of the altered flora of BV is an acceptable laboratory method for diagnosing BV. Culture of G. vaginalis is not recommended as a diagnostic tool because it is not specific. However, a DNA probe based test for high concentrations of G. vaginalis (Affirm™ VP III, manufactured by Becton Dickinson, Sparks, Maryland) may have clinical utility. Cervical Pap tests have limited clinical utility for the diagnosis of BV because of low sensitivity. Other commercially available tests that may be useful for the diagnosis of BV include a card test for the detection of elevated pH and trimethylamine (FemExam® test card, manufactured by Cooper Surgical, Shelton, Connecticut) and prolineaminopeptidase (Pip Activity TestCard™, manufactured by Litmus Concepts, Inc., Santa Clara, California). Treatment The established benefits of therapy for BV in non-pregnant women are to a) relieve vaginal symptoms and signs of infection and b) reduce the risk for infectious complications after abortion or hysterectomy. Other potential benefits include the reduction of other infectious complications (e.g., HIV and other STDs). All women who have symptomatic disease require treatment. BV during pregnancy is associated with adverse pregnancy outcomes, including premature rupture of the membranes, preterm labor, preterm birth, and postpartum endometritis. The established benefit of therapy for BV in pregnant women is to relieve vaginal symptoms and signs of infection. Additional potential benefits of therapy include a) reducing the risk for infectious complications associated with BV during pregnancy and b) reducing the risk for other infections (e.g., other STDs or HIV). The results of several investigations indicate that treatment of pregnant women who have BV and who are at high risk for preterm delivery (i.e., those who previously delivered a premature infant) may reduce the risk for prematurity (52--54). Therefore, high-risk pregnant women who have asymptomatic BV may be evaluated for treatment. The bacterial flora that characterizes BV have been recovered from the endometria and salpinges of women who have PID. BV has been associated with endometritis, PID, and vaginal cuff cellulitis after invasive procedures, including endometrial biopsy, hysterectomy, hysterosalpingography, placement of an IUD, cesarean section, and uterine curettage. The results of two randomized controlled trials indicated that treatment of BV with metronidazole substantially reduced postabortion PID (55,56). Three trials that evaluated the use of anaerobic antimicrobial coverage (metronidazole) for routine operative prophylaxis before abortion and seven trials that evaluated this additional coverage for women undergoing hysterectomy found a substantial reduction (range: 10%--75%) in post-operative infectious complications (57--66). Because of the increased risk for postoperative infectious complications associated with BV, some specialists recommend that before performing surgical abortion or hysterectomy, providers screen and treat women with BV in addition to providing routine prophylaxis. However, more information is needed before recommending treatment of asymptomatic BV before other invasive procedures.
NOTE: Patients should be advised to avoid consuming alcohol during treatment with metronidazole and for 24 hours thereafter. Clindamycin cream and ovules are oil-based and might weaken latex condoms and diaphragms. Refer to condom product labeling for additional information. The recommended metronidazole regimens are equally efficacious. The vaginal clindamycin cream appears less efficacious than the metronidazole regimens. The alternative regimens have lower efficacy for BV.
One randomized trial evaluating the clinical equivalency of intravaginal metronidazole gel 0.75% once daily versus twice daily found similar cure rates 1 month after therapy (67). One randomized trial that evaluated the equivalency of clindamycin cream and clindamycin ovules found that cure rates did not differ significantly (68). Metronidazole 2 g single-dose therapy is an alternative regimen because of its lower efficacy for treatment of BV. Although FDA has approved metronidazole 750-mg extended release tablets once daily for 7 days, no data have been published on the clinical equivalency of this regimen with other regimens. Studies are currently underway to evaluate the efficacy of vaginal lactobacilli suppositories in addition to oral metronidazole for the treatment of BV. No data support the use of non-vaginal lactobacilli or douching for the treatment of BV. Follow-Up Follow-up visits are unnecessary if symptoms resolve. Because recurrence of BV is not unusual, women should be advised to return for additional therapy if symptoms recur. Another recommended treatment regimen may be used to treat recurrent disease. No long-term maintenance regimen with any therapeutic agent is recommended. Management of Sex Partners The results of clinical trials indicate that a woman's response to therapy and the likelihood of relapse or recurrence are not affected by treatment of her sex partner(s) (69--71). Therefore, routine treatment of sex partners is not recommended. Special Considerations Allergy or Intolerance to the Recommended Therapy Clindamycin cream or oral clindamycin is preferred in case of allergy or intolerance to metronidazole. Metronidazole gel can be considered for patients who do not tolerate systemic metronidazole, but patients allergic to oral metronidazole should not be administered metronidazole vaginally. Pregnancy All symptomatic pregnant women should be tested and treated. BV has been associated with adverse pregnancy outcomes (e.g., premature rupture of the membranes, chorioamnionitis, preterm labor, preterm birth, postpartum endometritis, and post-cesarean wound infection). Some specialists prefer using systemic therapy to treat possible subclinical upper genital tract infections among women at low risk for preterm delivery (i.e., those who have no history of delivering an infant before term). Existing data do not support the use of topical agents during pregnancy. Evidence from three trials suggests an increase in adverse events (e.g., prematurity and neonatal infections), particularly in newborns, after use of clindamycin cream (72--74). Multiple studies and meta-analyses have not demonstrated a consistent association between metronidazole use during pregnancy and teratogenic or mutagenic effects in newborns (75--77).
Because treatment of BV in asymptomatic pregnant women at high risk for preterm delivery (i.e., those who have previously delivered a premature infant) with a recommended regimen has reduced preterm delivery in three of four randomized controlled trials (52--54,78), some specialists recommend the screening and treatment of these women. However, the optimal treatment regimens have not been established. The screening (if conducted) and treatment should be performed at the first prenatal visit. The two trials that examined the use of metronidazole during pregnancy used the 250-mg regimen; the recommended regimen for BV in nonpregnant women is 500 mg twice daily. Some specialists also recommend this higher dose for treatment of pregnant women. In one published study, women with BV were treated at 19 weeks with a regimen of an initial dose of 2 g, followed by a 2-g dose 2 days later; the regimen was repeated 4 weeks later (78). This regimen was not effective in reducing preterm birth in any group of women. Data are conflicting regarding whether treatment of asymptomatic pregnant women who are at low risk for preterm delivery reduces adverse outcomes of pregnancy. Several unpublished trials have evaluated screening and treatment for BV among asymptomatic low-risk pregnant women in the first or early second trimester. One trial, using oral clindamycin, demonstrated a reduction in spontaneous preterm birth; another indicated a reduction in postpartum infectious complications (79). Follow-Up of Pregnant Women Treatment of BV in asymptomatic pregnant women who are at high risk for preterm delivery might prevent adverse pregnancy outcomes. Therefore, a follow-up evaluation 1 month after completion of treatment should be considered to evaluate whether therapy was effective. HIV Infection Patients who have BV and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. TrichomoniasisTrichomoniasis is caused by the protozoan T. vaginalis. Most men who are infected with T. vaginalis do not have symptoms; others have NGU. Many infected women have symptoms characterized by a diffuse, malodorous, yellow-green discharge with vulvar irritation. However, some women have minimal or no symptoms. Diagnosis of vaginal trichomoniasis is usually performed by microscopy of vaginal secretions, but this method has a sensitivity of only about 60%--70%. Culture is the most sensitive commercially available method of diagnosis. No FDA-approved PCR test for T. vaginalis is available in the United States, but such testing may be available from commercial laboratories that have developed their own PCR tests.
The nitroimidazoles comprise the only class of drugs useful for the oral or parenteral therapy of trichomoniasis. Of these, only metronidazole is readily available in the United States and approved by the FDA for the treatment of trichomoniasis. In randomized clinical trials, the recommended metronidazole regimens have resulted in cure rates of approximately 90%--95%; ensuring treatment of sex partners might increase this rate. Treatment of patients and sex partners results in relief of symptoms, microbiologic cure, and reduction of transmission. Metronidazole gel has been approved for treatment of BV. However, like other topically applied antimicrobials that are unlikely to achieve therapeutic levels in the urethra or perivaginal glands, it is considerably less efficacious for treatment of trichomoniasis (<50%) than oral preparations of metronidazole. Therefore, metronidazole gel is not recommended for use. Several other topically applied antimicrobials have occasionally been used for treatment of trichomoniasis, but it is unlikely that these preparations have greater efficacy than metronidazole gel. Follow-Up Follow-up is unnecessary for men and women who become asymptomatic after treatment or who are initially asymptomatic. Certain strains of T. vaginalis can have diminished susceptibility to metronidazole; however, infections caused by most of these organisms respond to higher doses of metronidazole. If treatment failure occurs with either regimen, the patient should be re-treated with metronidazole 500 mg twice a day for 7 days. If treatment failure occurs again, the patient should be treated with a single, 2-g dose of metronidazole once a day for 3--5 days. Patients with laboratory-documented infection who do not respond to the 3--5 day treatment regimen and who have not been reinfected should be managed in consultation with a specialist; evaluation of such cases should ideally include determination of the susceptibility of T. vaginalis to metronidazole. Consultation is available from CDC (tel: 770-488-4115; website: http://www.cdc.gov/std/). Management of Sex Partners Sex partners of patients with T. vaginalis should be treated. Patients should be instructed to avoid sex until they and their sex partners are cured (i.e., when therapy has been completed and patient and partner(s) are asymptomatic [in the absence of a microbiologic test of cure]). Special Considerations Allergy, Intolerance, and Adverse Reactions Patients with an immediate-type allergy to metronidazole can be managed by desensitization (80). Topical therapy with drugs other than nitroimidazoles can be attempted, but cure rates are low (<50%). Pregnancy Vaginal trichomoniasis has been associated with adverse pregnancy outcomes, particularly premature rupture of the membranes, preterm delivery, and low birthweight. Data have not indicated that treating asymptomatic trichomoniasis during pregnancy lessens that association (81). Women who are symptomatic with trichomoniasis should be treated to ameliorate symptoms. Women may be treated with 2 g of metronidazole in a single dose. Multiple studies and meta-analyses have not demonstrated a consistent association between metronidazole use during pregnancy and teratogenic or mutagenic effects in infants (75--77). HIV Infection Patients who have trichomoniasis and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. Vulvovaginal CandidiasisVulvovaginal candidiasis (VVC) usually is caused by C. albicans but occasionally is caused by other Candida sp. or yeasts. Typical symptoms of VVC include pruritus and vaginal discharge. Other symptoms include vaginal soreness, vulvar burning, dyspareunia, and external dysuria. None of these symptoms is specific for VVC. An estimated 75% of women will have at least one episode of VVC, and 40%--45% will have two or more episodes. On the basis of clinical presentation, microbiology, host factors, and response to therapy, VVC can be classified as either uncomplicated or complicated (Box 2). Approximately 10%--20% of women will have complicated VVC, suggesting diagnostic and therapeutic considerations. Uncomplicated VVC Diagnostic Considerations in Uncomplicated VVC A diagnosis of Candida vaginitis is suggested clinically by pruritus and erythema in the vulvovaginal area; a white discharge may be present. The diagnosis can be made in a woman who has signs and symptoms of vaginitis when either a) a wet preparation (saline, 10% KOH) or Gram stain of vaginal discharge demonstrates yeasts or pseudohyphae or b) a culture or other test yields a positive result for a yeast species. Candida vaginitis is associated with a normal vaginal pH (<4.5). Use of 10% KOH in wet preparations improves the visualization of yeast and mycelia by disrupting cellular material that might obscure the yeast or pseudohyphae. Identifying Candida by culture in the absence of symptoms is not an indication for treatment, because approximately 10%--20% of women harbor Candida sp. and other yeasts in the vagina. VVC can occur concomitantly with STDs, and treatment of all pathogens present is warranted. Most healthy women with uncomplicated VVC have no precipitating factors. However, in a minority of women who have asymptomatic Candida colonization, antibiotic use precipitates VVC. Treatment Short-course topical formulations (i.e., single dose and regimens of 1--3 days) effectively treat uncomplicated VVC. The topically applied azole drugs are more effective than nystatin. Treatment with azoles results in relief of symptoms and negative cultures in 80%--90% of patients who complete therapy.
NOTE: The creams and suppositories in this regimen are oil-based and may weaken latex condoms and diaphragms. Refer to condom product labeling for further information. Preparations for intravaginal administration of butaconazole, clotrimazole, miconazole, and tioconazole are available over-the-counter (OTC). Self-medication with OTC preparations should be advised only for women who have been diagnosed previously with VVC and who have a recurrence of the same symptoms. Any woman whose symptoms persist after using an OTC preparation or who has a recurrence of symptoms within 2 months should seek medical care. Unnecessary or inappropriate use of OTC preparations is common and can lead to delay of treatment of other etiologies of vulvovaginitis that could result in adverse clinical outcomes. Follow-Up Patients should be instructed to return for follow-up visits only if symptoms persist or recur within 2 months of onset of initial symptoms. Management of Sex Partners VVC is not usually acquired through sexual intercourse; treatment of sex partners is not recommended but may be considered in women who have recurrent infection. A minority of male sex partners may have balanitis, which is characterized by erythematous areas on the glans of the penis in conjunction with pruritus or irritation. These men benefit from treatment with topical antifungal agents to relieve symptoms. Special Considerations Allergy to or Intolerance of the Recommended Therapy. Topical agents usually cause no systemic side effects, although local burning or irritation may occur. Oral agents occasionally cause nausea, abdominal pain, and headache. Therapy with the oral azoles has been associated rarely with abnormal elevations of liver enzymes. Clinically important interactions might occur when these oral agents are administered with other drugs, including astemizole, calcium channel antagonists, cisapride, coumadin, cyclosporin A, oral hypoglycemic agents, phenytoin, protease inhibitors, tacrolimus, terfenadine, theophylline, trimetrexate, and rifampin. Complicated VVC Recurrent Vulvovaginal Candidiasis Recurrent VVC (RVVC), usually defined as four or more episodes of symptomatic VVC each year, affects a small percentage of women (<5%). The pathogenesis of RVVC is poorly understood, and most women who have RVVC have no apparent predisposing or underlying conditions. Vaginal cultures should be obtained from patients with RVVC to confirm the clinical diagnosis and to identify unusual species, including non-albicans species, particularly Candida glabrata (C. glabrata does not form pseudohyphae or hyphae and is not easily recognized on microscopy). C. glabrata and other non-albicans Candidia species are found in 10%--20% of patients with RVVC. Conventional antimycotic therapies are not as effective against these species as against C. albicans. Treatment Each individual episode of RVVC caused by C. albicans responds well to short duration oral or topical azole therapy. However, to maintain clinical and mycologic control, specialists recommend a longer duration of initial therapy (e.g., 7--14 days of topical therapy or a 150-mg, oral dose of fluconazole repeated 3 days later) to achieve mycologic remission before initiating a maintenance antifungal regimen. Maintenance Regimens Maintenance antifungals are selected on the basis of pharmacologic characteristics of individual agents and route of administration. Recommended regimens include clotrimazole (500-mg dose vaginal suppositories once weekly), ketoconazole (100-mg dose once daily), fluconazole (100--150-mg dose once weekly), and itraconazole (400-mg dose once monthly or 100-mg dose once daily). Although all maintenance regimens should be continued for 6 months, an estimated one in 10,000--15,000 persons exposed to ketoconazole may develop hepatotoxicity. Patients receiving long-term ketoconazole should be monitored for toxicity. Suppressive maintenance antifungal therapies are effective in reducing RVVC. However, 30%--40% of women will have recurrent disease once maintenance therapy is discontinued. Routine treatment of sex partners is controversial. Although C. albicans azole resistance is rare in vaginal isolates, surveillance of recurrent isolates for development of resistance is prudent. Severe VVC Severe vulvovaginitis (i.e., extensive vulvar erythema, edema, excoriation, and fissure formation) has lower clinical response rates in patients treated with short courses of topical or oral therapy. Either 7--14 days of topical azole or 150 mg of fluconazole in two sequential doses (second dose 72 hours after initial dose) is recommended. Non-albicans VVC The optimal treatment of non-albicans VVC remains unknown. Longer duration of therapy (7--14 days) with a non-fluconazole azole drug is recommended as first-line therapy. If recurrence occurs, 600 mg of boric acid in a gelatin capsule is recommended, administered vaginally once daily for 2 weeks. This regimen has clinical and mycologic eradication rates of approximately 70%. Additional options include topical 4% flucytosine; however, referral to a specialist is advised. Safety data regarding the long-term use of these regimens are lacking. If non-albicans VVC continues to recur, a maintenance regimen of 100,000 units of nystatin delivered daily via vaginal suppositories has been successful. Compromised Host Women with underlying debilitating medical conditions (e.g., those with uncontrolled diabetes or those receiving corticosteroid treatment) do not respond as well to short-term therapies. Efforts to correct modifiable conditions should be made, and more prolonged (i.e., 7--14 days) conventional antimycotic treatment is necessary. Pregnancy VVC often occurs during pregnancy. Only topical azole therapies, applied for 7 days, are recommended for use among pregnant women. HIV Infection The attack rate of VVC in HIV-infected women is unknown. Vaginal Candida colonization rates in HIV-infected women are higher than among seronegative women with similar demographic characteristics and high-risk behaviors, and the colonization rates correlate with increasing severity of immunosuppression. Symptomatic VVC is more frequent in seropositive women and similarly correlates with severity of immunodeficiency. In addition, among HIV-infected women, systemic azole exposure is associated with the isolation of non-albicans Candida species from the vagina. Based on available data, therapy for VVC in HIV-infected women should not differ from that for seronegative women. Although long-term prophylactic therapy with fluconazole at a dose of 200 mg weekly has been effective in reducing C. albicans colonization and symptomatic VVC, it is not recommended for routine primary prophylaxis in HIV-infected women in the absence of recurrent VVC. Given the frequency with which RVVC occurs in the immmunocompetent healthy population, RVVC should not be considered a sentinel sign to justify HIV testing. Pelvic Inflammatory DiseasePID comprises a spectrum of inflammatory disorders of the upper female genital tract, including any combination of endometritis, salpingitis, tubo-ovarian abscess, and pelvic peritonitis. Sexually transmitted organisms, especially N. gonorrhoeae and C. trachomatis, are implicated in many cases; however, microorganisms that comprise the vaginal flora (e.g., anaerobes, G. vaginalis, Haemophilus influenzae, enteric Gram-negative rods, and Streptococcus agalactiae) also have been associated with PID. In addition, cytomegalovirus (CMV), M. hominis, and U. urealyticum may be the etiologic agents in some cases of PID. Diagnostic ConsiderationsAcute PID is difficult to diagnose because of the wide variation in the symptoms and signs. Many women with PID have subtle or mild symptoms. Delay in diagnosis and effective treatment probably contributes to inflammatory sequelae in the upper reproductive tract. Laparoscopy can be used to obtain a more accurate diagnosis of salpingitis and a more complete bacteriologic diagnosis. However, this diagnostic tool often is not readily available, and its use is not easy to justify when symptoms are mild or vague. Moreover, laparoscopy will not detect endometritis and may not detect subtle inflammation of the fallopian tubes. Consequently, a diagnosis of PID usually is based on clinical findings. The clinical diagnosis of acute PID is imprecise. Data indicate that a clinical diagnosis of symptomatic PID has a PPV for salpingitis of 65%--90% compared with laparoscopy. The PPV of a clinical diagnosis of acute PID differs depending on epidemiologic characteristics and the clinical setting, with higher PPV among sexually active young women (particularly adolescents) and among patients attending STD clinics or from settings in which rates of gonorrhea or chlamydia are high. In all settings, however, no single historical, physical, or laboratory finding is both sensitive and specific for the diagnosis of acute PID (i.e., can be used both to detect all cases of PID and to exclude all women without PID). Combinations of diagnostic findings that improve either sensitivity (i.e., detect more women who have PID) or specificity (i.e., exclude more women who do not have PID) do so only at the expense of the other. For example, requiring two or more findings excludes more women who do not have PID but also reduces the number of women with PID who are identified. Many episodes of PID go unrecognized. Although some cases are asymptomatic, others are undiagnosed because the patient or the health-care provider fails to recognize the implications of mild or nonspecific symptoms or signs (e.g., abnormal bleeding, dyspareunia, and vaginal discharge). Because of the difficulty of diagnosis and the potential for damage to the reproductive health of women even by apparently mild or atypical PID, health-care providers should maintain a low threshold for the diagnosis of PID. The optimal treatment regimen and long-term outcome of early treatment of women with asymptomatic or atypical PID are unknown. The following recommendations for diagnosing PID are intended to help health-care providers recognize when PID should be suspected and when they need to obtain additional information to increase diagnostic certainty. Diagnosis and management of other common causes of lower abdominal pain (e.g., ectopic pregnancy, acute appendicitis, and functional pain) are unlikely to be impaired by initiating empiric antimicrobial therapy for PID. Empiric treatment of PID should be initiated in sexually active young women and other women at risk for STDs if the following minimum criteria are present and no other cause(s) for the illness can be identified:
Requiring all minimum criteria may result in low sensitivity in patients at high risk for infection. In patients with both pelvic tenderness and signs of lower genital tract inflammation, the diagnosis of PID should be considered. Treatment may be indicated based on a patient's risk profile. More elaborate diagnostic evaluation often is needed, because incorrect diagnosis and management might cause unnecessary morbidity. These additional criteria may be used to enhance the specificity of the minimum criteria. Additional criteria that support a diagnosis of PID include the following:
Most women with PID have either mucopurulent cervical discharge or evidence of WBCs on a microscopic evaluation of a saline preparation of vaginal fluid. If the cervical discharge appears normal and no white blood cells are found on the wet prep, the diagnosis of PID is unlikely, and alternative causes of pain should be investigated. The most specific criteria for diagnosing PID include the following:
A diagnostic evaluation that includes some of these more extensive studies may be warranted in certain cases. TreatmentPID treatment regimens must provide empiric, broad-spectrum coverage of likely pathogens. Antimicrobial coverage should include N. gonorrhoeae, C. trachomatis, anaerobes, Gram-negative facultative bacteria, and streptococci. Several antimicrobial regimens have been effective in achieving clinical and microbiologic cure in randomized clinical trials with short-term follow- up. However, few investigations have assessed and compared these regimens with regard to elimination of infection in the endometrium and fallopian tubes or determined the incidence of long-term complications (e.g., tubal infertility and ectopic pregnancy) of antimicrobial regimens. All regimens should be effective against N. gonorrhoeae and C. trachomatis, because negative endocervical screening does not preclude upper reproductive tract infection. The need to eradicate anaerobes from women who have PID has not been determined definitively. Anaerobic bacteria have been isolated from the upper reproductive tract of women who have PID, and data from in vitro studies have revealed that certain anaerobes (e.g., Bacteroides fragilis) can cause tubal and epithelial destruction. In addition, BV also is present in many women who have PID. Until treatment regimens that do not adequately cover these microbes have been demonstrated to prevent sequelae as successfully as the regimens that are effective against these microbes, the recommended regimens should provide anaerobic coverage. Treatment should be initiated as soon as the presumptive diagnosis has been made, because prevention of long-term sequelae has been linked directly with immediate administration of appropriate antibiotics. When selecting a treatment regimen, health-care providers should consider availability, cost, patient acceptance, and antimicrobial susceptibility. In the past, many specialists recommended that all patients who had PID be hospitalized so that bed rest and supervised treatment with parenteral antibiotics could be initiated. However, hospitalization is no longer synonymous with parenteral therapy. No currently available data compare the efficacy of parenteral with oral therapy or inpatient with outpatient treatment settings. The decision of whether hospitalization is necessary should be based on the discretion of the health-care provider. The following criteria for hospitalization are based on observational data and theoretical concerns:
No data are available that suggest that adolescent women benefit from hospitalization for treatment of PID. Whether women in their later reproductive years benefit from hospitalization for treatment of PID is also unclear, although women aged >35 years who are hospitalized with PID are more likely than are younger women to have a complicated clinical course. Parenteral Treatment No efficacy data compare parenteral with oral regimens. Many randomized trials have demonstrated the efficacy of both parenteral and oral regimens (82). Although most trials have used parenteral treatment for at least 48 hours after the patient demonstrates substantial clinical improvement, this time designation is arbitrary. Clinical experience should guide decisions regarding transition to oral therapy, which usually can be initiated within 24 hours of clinical improvement. Most clinicians recommend at least 24 hours of direct inpatient observation for patients who have tubo-ovarian abscesses, after which time home antimicrobial therapy is adequate.
NOTE: Because of pain associated with infusion, doxycycline should be administered orally when possible, even when the patient is hospitalized. Both oral and IV administration of doxycycline provide similar bioavailability. Parenteral therapy may be discontinued 24 hours after a patient improves clinically, and oral therapy with doxycycline (100 mg twice a day) should continue to complete 14 days of therapy. When tubo-ovarian abscess is present, many health-care providers use clindamycin or metronidazole with doxycycline for continued therapy rather than doxycycline alone, because it provides more effective anaerobic coverage. Clinical data are limited regarding the use of other second- or third-generation cephalosporins (e.g., ceftizoxime, cefotaxime, and ceftriaxone), which also may be effective therapy for PID and may replace cefotetan or cefoxitin. However, these cephalosporins are less active than cefotetan or cefoxitin against anaerobic bacteria.
Although use of a single daily dose of gentamicin has not been evaluated for the treatment of PID, it is efficacious in other analogous situations. Parenteral therapy can be discontinued 24 hours after a patient improves clinically; continuing oral therapy should consist of doxycycline 100 mg orally twice a day or clindamycin 450 mg orally four times a day to complete a total of 14 days of therapy. When tubo-ovarian abscess is present, many health-care providers use clindamycin for continued therapy rather than doxycycline, because clindamycin provides more effective anaerobic coverage.
Limited data support the use of other parenteral regimens, but the following three regimens have been investigated in at least one clinical trial, and they have broad spectrum coverage.
IV ofloxacin has been investigated as a single agent; however because of concerns regarding its spectum, metronidazole may be included in the regimen. Preliminary data suggest that levofloxacin is as effective as ofloxacin and may be substituted; its single daily dosing makes it advantageous from a compliance perspective (83). Ampicillin/sulbactam plus doxycycline has good coverage against C. trachomatis, N. gonorrhoeae, and anaerobes and is effective for patients who have tubo-ovarian abscess. Oral Treatment As with parenteral regimens, clinical trials of outpatient regimens have provided minimal information regarding intermediate and long-term outcomes. The following regimens provide coverage against the frequent etiologic agents of PID, but evidence from clinical trials supporting their use is limited. Patients who do not respond to oral therapy within 72 hours should be reevaluated to confirm the diagnosis and should be administered parenteral therapy on either an outpatient or inpatient basis.
Oral ofloxacin has been investigated as a single agent in two well-designed clinical trials, and it is effective against both N. gonorrhoeae and C. trachomatis (84,85). Despite the results of these trials, lack of anaerobic coverage with ofloxacin is a concern; the addition of metronidazole to the treatment regimen provides this coverage. Preliminary data suggest that levofloxacin is as effective as ofloxacin and may be substituted (83); its single daily dosing makes it advantageous from a compliance perspective.
The optimal choice of a cephalosporin for Regimen B is unclear; although cefoxitin has better anaerobic coverage, ceftriaxone has better coverage against N. gonorrhoeae. Clinical trials have demonstrated that a single dose of cefoxitin is effective in obtaining short-term clinical response in women who have PID; however, the theoretical limitations in its coverage of anaerobes may require the addition of metronidazole to the treatment regimen (86). The metronidazole also will effectively treat BV, which is frequently associated with PID. No data have been published regarding the use of oral cephalosporins for the treatment of PID. Limited data suggest that the combination of oral metronidazole plus doxycycline after primary parenteral therapy is safe and effective (87,88). Alternative Oral Regimens Although information regarding other outpatient regimens is limited, one other regimen has undergone at least one clinical trial and has broad spectrum coverage. Amoxicillin/clavulanic acid plus doxycycline was effective in obtaining short-term clinical response in a single clinical trial; however, gastrointestinal symptoms might limit compliance with this regimen. Several recent investigations have evaluated the use of azithromycin in the treatment of upper reproductive tract infections; however, the data are insufficient to recommend this agent as a component of any of the oral treatment regimens for PID. Follow-UpPatients should demonstrate substantial clinical improvement (e.g., defervescence; reduction in direct or rebound abdominal tenderness; and reduction in uterine, adnexal, and cervical motion tenderness) within 3 days after initiation of therapy. Patients who do not improve within this period usually require hospitalization, additional diagnostic tests, and surgical intervention. If the health-care provider prescribes outpatient oral or parenteral therapy, a follow-up examination should be performed within 72 hours using the criteria for clinical improvement described previously. If the patient has not improved, hospitalization for parenteral therapy and further evaluation are recommended. Some specialists also recommend rescreening for C. trachomatis and N. gonorrhoeae 4--6 weeks after therapy is completed in women with documented infection with these pathogens. Management of Sex PartnersMale sex partners of women with PID should be examined and treated if they had sexual contact with the patient during the 60 days preceding the patient's onset of symptoms. Evaluation and treatment are imperative because of the risk for reinfection of the patient and the strong likelihood of urethral gonococcal or chlamydial infection in the sex partner. Male partners of women who have PID caused by C. trachomatis and/or N. gonorrhoeae often are asymptomatic. Sex partners should be treated empirically with regimens effective against both of these infections, regardless of the etiology of PID or pathogens isolated from the infected woman. Even in clinical settings in which only women are treated, arrangements should be made to provide care for male sex partners of women who have PID. When this is not feasible, health-care providers should ensure that sex partners are referred for appropriate treatment. PreventionPrevention of chlamydial infection by screening and treating high-risk women reduces the incidence of PID. Theoretically, most cases of PID can be prevented by screening all women or those determined to be at high-risk (based on age or other factors) using DNA amplification on cervical specimens (in women receiving pelvic exams) and on urine (in women not undergoing exams). Although BV is associated with PID, whether the incidence of PID can be reduced by identifying and treating women with BV is unclear. Special ConsiderationsPregnancy Because of the high risk for maternal morbidity, fetal wastage, and preterm delivery, pregnant women who have suspected PID should be hospitalized and treated with parenteral antibiotics. HIV Infection Differences in the clinical manifestations of PID between HIV-infected women and HIV-negative women have not been well delineated. In early observational studies, HIV-infected women with PID were more likely to require surgical intervention. In recent, more comprehensive observational and controlled studies, HIV-infected women with PID had similar symptoms when compared with uninfected controls (89--91). They were more likely to have a tubo-ovarian abscess, but responded equally well to standard parenteral and oral antibiotic regimens when compared with HIV-negative women. The microbiologic findings for HIV-positive and HIV-negative women were similar, except for a) higher rates of concomitant M. hominis, candida, streptococcal, and HPV infections and b) HPV-related cytologic abnormalities among those with HIV infection. Whether the management of immunodeficient HIV-infected women with PID requires more aggressive interventions (e.g., hospitalization or parenteral antimicrobial regimens) has not been determined. EpididymitisAmong sexually active men aged <35 years, epididymitis is most often caused by C. trachomatis or N. gonorrhoeae. Epididymitis caused by sexually transmitted enteric organisms (e.g., Escherichia coli) also occurs among men who are the insertive partner during anal intercourse. Sexually transmitted epididymitis usually is accompanied by urethritis, which often is asymptomatic. Nonsexually transmitted epididymitis that is associated with urinary-tract infections caused by Gram-negative enteric organisms occurs more frequently among men aged >35 years, men who have recently undergone urinary-tract instrumentation or surgery, and men who have anatomical abnormalities of the urinary tract. Although most patients can be treated on an outpatient basis, hospitalization should be considered when severe pain suggests other diagnoses (e.g., torsion, testicular infarction, or abscess) or when patients are febrile or might be noncompliant with an antimicrobial regimen. Diagnostic ConsiderationsMen who have epididymitis typically have unilateral testicular pain and tenderness; hydrocele and palpable swelling of the epididymis usually are present. Testicular torsion, a surgical emergency, should be considered in all cases, but it occurs more frequently among adolescents and in men without evidence of inflammation or infection. Emergency testing for torsion may be indicated when the onset of pain is sudden, pain is severe, or the test results available during the initial examination do not support a diagnosis of urethritis or urinary-tract infection. If the diagnosis is questionable, a specialist should be consulted immediately, because testicular viability may be compromised. The evaluation of men for epididymitis should include the following procedures.
TreatmentEmpiric therapy is indicated before culture results are available. Treatment of epididymitis caused by C. trachomatis or N. gonorrhoeae will result in a) microbiologic cure of infection, b) improvement of signs and symptoms, c) prevention of transmission to others, and d) a decrease in potential complications (e.g., infertility or chronic pain). As an adjunct to therapy, bed rest, scrotal elevation, and analgesics are recommended until fever and local inflammation have subsided.
Follow-UpFailure to improve within 3 days of the initiation of treatment requires reevaluation of both the diagnosis and therapy. Swelling and tenderness that persist after completion of antimicrobial therapy should be evaluated comprehensively. The differential diagnosis includes tumor, abscess, infarction, testicular cancer, TB, and fungal epididymitis. Management of Sex PartnersPatients who have epididymitis that has been confirmed or is suspected to be caused by N. gonorrhoeae or C. trachomatis should be instructed to refer sex partners for evaluation and treatment. Sex partners of these patients should be referred if their contact with the index patient was within the 60 days preceding onset of the patient's symptoms. Patients should be instructed to avoid sexual intercourse until they and their sex partners are cured (i.e., until therapy is completed and patient and partner[s] no longer have symptoms). Special ConsiderationsHIV Infection Patients who have uncomplicated epididymitis and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. Fungi and mycobacteria, however, are more likely to cause epididymitis in immunosuppressed patients than in those who are immunocompetent. Human Papillomavirus InfectionGenital WartsMore than 30 types of HPV can infect the genital tract. Most HPV infections are asymptomatic, unrecognized, or subclinical. Visible genital warts usually are caused by HPV types 6 or 11. Other HPV types in the anogenital region (e.g., types 16, 18, 31, 33, and 35) have been strongly associated with cervical neoplasia. Diagnosis of genital warts can be confirmed by biopsy, although biopsy is needed only under certain circumstances (e.g., if the diagnosis is uncertain; the lesions do not respond to standard therapy; the disease worsens during therapy; the patient is immunocompromised; or warts are pigmented, indurated, fixed, and ulcerated). No data support the use of type-specific HPV nucleic acid tests in the routine diagnosis or management of visible genital warts. In addition to the external genitalia (i.e., the penis, vulva, scrotum, perineum, and perianal skin), genital warts can occur on the uterine cervix and in the vagina, urethra, anus, and mouth; these warts are sometimes symptomatic. Intra-anal warts are seen predominantly in patients who have had receptive anal intercourse; these warts are distinct from perianal warts, which can occur in men and women who do not have a history of anal sex. In addition to the genital area, HPV types 6 and 11 have been associated with conjunctival, nasal, oral, and laryngeal warts. HPV types 6 and 11 rarely are associated with invasive squamous cell carcinoma of the external genitalia. Depending on the size and anatomic location, genital warts can be painful, friable, and pruritic, although they are commonly asymptomatic. HPV types 16, 18, 31, 33, and 35 are found occasionally in visible genital warts and have been associated with external genital (i.e., vulvar, penile, and anal) squamous intraepithelial neoplasia (i.e., squamous cell carcinoma in situ, bowenoid papulosis, Erythroplasia of Queyrat, or Bowen's disease of the genitalia). These HPV types also have been associated with vaginal, anal, and cervical intraepithelial dysplasia and squamous cell carcinoma. Patients who have visible genital warts can be infected simultaneously with multiple HPV types. Treatment The primary goal of treating visible genital warts is the removal of symptomatic warts. In most patients, treatment can induce wart-free periods. If left untreated, visible genital warts may resolve on their own, remain unchanged, or increase in size or number. Determining whether treatment of genital warts will reduce transmission is difficult, because no laboratory marker of infectivity has been established and because clinical studies evaluating the persistence of HPV DNA in genital tissue after treatment have shown variable results. Existing data indicate that currently available therapies for genital warts may reduce, but probably do not eradicate, infectivity. Whether the reduction in viral DNA that results from current treatment regimens impacts future transmission remains unclear. No evidence indicates that either the presence of genital warts or their treatment is associated with the development of cervical cancer. Regimens Treatment of genital warts should be guided by the preference of the patient, the available resources, and the experience of the health-care provider. No definitive evidence suggests that any of the available treatments is superior to the others, and no single treatment is ideal for all patients or all warts. The use of locally developed and monitored treatment algorithms has been associated with improved clinical outcomes and should be encouraged. Because of uncertainty regarding the effect of treatment on future transmission and the possibility for spontaneous resolution, an acceptable alternative for some patients is to forego treatment and await spontaneous resolution. Most patients have <10 genital warts, with a total wart area of 0.5--1.0 cm2. These warts respond to most treatment modalities. Factors that may influence selection of treatment include wart size, wart number, anatomic site of wart, wart morphology, patient preference, cost of treatment, convenience, adverse effects, and provider experience. Many patients require a course of therapy rather than a single treatment. In general, warts located on moist surfaces and/or in intertriginous areas respond better to topical treatment than do warts on drier surfaces. The treatment modality should be changed if a patient has not improved substantially after three provider-administered treatments or if warts have not completely cleared after six treatments. The risk-benefit ratio of treatment should be evaluated throughout the course of therapy to avoid overtreatment. Both patient-applied therapies and provider-administered therapies are available. Providers should be knowledgeable about, and have available to them, at least one patient-applied and one provider-administered treatment. Complications rarely occur if treatments for warts are employed properly. Patients should be warned that persistent hypopigmentation or hyperpigmentation are common with ablative modalities. Depressed or hypertrophic scars are uncommon but can occur, especially if the patient has had insufficient time to heal between treatments. Rarely, treatment can result in disabling chronic pain syndromes (e.g., vulvodynia or hyperesthesia of the treatment site).
For patient-applied treatments, patients must be able to identify and reach warts to be treated. Podofilox 0.5% solution or gel, an antimitotic drug that destroys warts, is relatively inexpensive, easy to use, safe, and self-applied by patients. Most patients experience mild/moderate pain or local irritation after treatment. Imiquimod is a topically active immune enhancer that stimulates production of interferon and other cytokines. Local inflammatory reactions are common with the use of imiquimod; these reactions usually are mild to moderate. Traditionally, follow-up visits are not required for patients using self-administered therapy. However, follow-up may be useful several weeks into therapy to determine appropriateness of medication use and response to treatment. Cryotherapy destroys warts by thermal-induced cytolysis. Health-care providers must be trained on the proper use of this therapy, because over- and under-treatment may result in poor efficacy or increased likelihood of complications. Pain after application of the liquid nitrogen, followed by necrosis and sometimes blistering, is common. Local anesthesia (topical or injected) may facilitate therapy if warts are present in many areas or if the area of warts is large. Podophyllin resin, which contains several compounds including antimitotic podophyllin lignans, is another treatment option. The resin is most frequently compounded at 10%--25% in a tincture of benzoin. However, podophyllin resin preparations differ in the concentration of active components and contaminants. The shelf life and stability of podophyllin preparations are unknown. A thin layer of podophyllin resin must be applied to the warts and allowed to air dry before the treated area comes into contact with clothing; over-application or failure to air dry can result in local irritation caused by spread of the compound to adjacent areas. Both TCA and BCA are caustic agents that destroy warts by chemical coagulation of the proteins. Although these preparations are widely used, they have not been investigated thoroughly. TCA solutions have a low viscosity comparable with that of water and can spread rapidly if applied excessively; thus, they can damage adjacent tissues. Both TCA and BCA should be applied sparingly and allowed to dry before the patient sits or stands. If pain is intense, the acid can be neutralized with soap or sodium bicarbonate. Surgical therapy is a treatment option that has the advantage of usually eliminating warts at a single visit. However, such therapy requires substantial clinical training, additional equipment, and a longer office visit. Once local anesthesia is applied, the visible genital warts can be physically destroyed by electrocautery, in which case no additional hemostasis is required. Care must be taken to control the depth of electrocautery to prevent scarring. Alternatively, the warts can be removed either by tangential excision with a pair of fine scissors or a scalpel or by curettage. Because most warts are exophytic, this can be accomplished with a resulting wound that only extends into the upper dermis. Hemostasis can be achieved with an electrosurgical unit or a chemical styptic (e.g., an aluminum chloride solution). Suturing is neither required nor indicated in most cases when surgical removal is done properly. Surgical therapy is most beneficial for patients who have a large number or area of genital warts. Carbon dioxide laser and surgery may be useful in the management of extensive warts or intraurethral warts, particularly for those patients who have not responded to other treatments. Interferons, either natural or recombinant, used for the treatment of genital warts have been administered systemically (i.e., subcutaneously at a distant site or IM) and intralesionally (i.e., injected into the warts). Systemic interferon is not effective. The efficacy and recurrence rates of intralesional interferon are comparable to other treatment modalities. Interferon is likely effective because of its anti-viral and/or immunostimulating effects. However, interferon therapy is not recommended for routine use because of inconvenient routes of administration, frequent office visits, and the association between its use and a high frequency of systemic adverse effects. Because of the shortcomings of all available treatments, some clinics employ combination therapy (i.e., the simultaneous use of two or more modalities on the same wart at the same time). However, some specialists believe that combining modalities may increase complications without improving efficacy. Cervical Warts For women who have exophytic cervical warts, high-grade squamous intraepithelial lesions (SIL) must be excluded before treatment is initiated. Management of exophytic cervical warts should include consultation with a specialist.
NOTE: Although data evaluating the use of podofilox and imiquimod for the treatment of distal meatal warts are limited, some specialists recommend their use in certain patients.
NOTE: Warts on the rectal mucosa should be managed in consultation with a specialist.
Education and counseling are important aspects of managing patients with genital warts. Patients can be educated through patient education materials, including pamphlets, hotlines, and web sites (http://www.ashastd.org). Attempts should be made to cover the following key messages.
Follow-Up After visible genital warts have cleared, a follow-up evaluation is not mandatory but may be helpful. Patients should be cautioned to watch for recurrences, which occur most frequently during the first 3 months. Because the sensitivity and specificity of self-diagnosis of genital warts are unknown, patients concerned about recurrences should be offered a follow-up evaluation 3 months after treatment. Earlier follow-up visits also may be useful for some patients to document the absence of warts, to monitor for or treat complications of therapy, and to provide an additional opportunity for patient education and counseling. Women should be counseled to undergo regular Pap screening as recommended for women without genital warts. The presence of genital warts is not an indication for a change in the frequency of Pap tests or for cervical colposcopy. Management of Sex Partners Examination of sex partners is not necessary for the management of genital warts because no data indicate that reinfection plays a role in recurrences. Additionally, providing treatment solely for the purpose of preventing future transmission cannot be recommended because the value of treatment in reducing infectivity is not known. However, because self- or partner-examination has not been evaluated as a diagnostic method for genital warts, sex partners of patients who have genital warts may benefit from examination to assess the presence of genital warts and other STDs. The counseling of sex partners provides an opportunity for these partners to a) learn about implications of having a partner who has genital warts and about their potential for future disease transmission and b) receive STD and Pap screening. Female sex partners of patients who have genital warts should be reminded that cytologic screening for cervical cancer is recommended for all sexually active women. Special Considerations Pregnancy Imiquimod, podophyllin, and podofilox should not be used during pregnancy. Because genital warts can proliferate and become friable during pregnancy, many specialists advocate their removal during pregnancy. HPV types 6 and 11 can cause respiratory papillomatosis in infants and children. The route of transmission (i.e., transplacental, perinatal, or postnatal) is not completely understood. The preventive value of cesarean section is unknown; thus, cesarean delivery should not be performed solely to prevent transmission of HPV infection to the newborn. Cesarean delivery may be indicated for women with genital warts if the pelvic outlet is obstructed or if vaginal delivery would result in excessive bleeding. Immunodeficient Patients Persons who are immunosuppressed because of HIV or other reasons may not respond as well as immunocompetent persons to therapy for genital warts, and they may have more frequent recurrences after treatment. Squamous cell carcinomas arising in or resembling genital warts may occur more frequently among immunosuppressed persons, thus requiring biopsy for confirmation of diagnosis. Because of the increased incidence of anal cancer in HIV-infected homosexual men, screening for anal SIL by cytology in this population is advocated by some specialists. However, until more data about the natural history of anal SIL and treatment efficacy are available, such a screening approach is not recommended. Squamous Cell Carcinoma in Situ Patients in whom squamous cell carcinoma in situ of the genitalia is diagnosed should be referred to a specialist for treatment. Ablative modalities usually are effective, but careful follow-up is important. The risk for these lesions leading to invasive squamous cell carcinoma of the external genitalia in immunocompetent patients is unknown but is probably low. Female partners of male patients who have squamous cell carcinoma in situ are at high risk for cervical abnormalities. Subclinical Genital HPV Infection (Without Exophytic Warts)Subclinical genital HPV infection is a term often used to refer to manifestations of infection in the absence of genital warts, including situations where infection is detected on the cervix by Pap test, colposcopy, or biopsy; on the penis, vulva, or other genital skin by the appearance of white areas after application of acetic acid; or on any genital skin by a positive test for HPV. Subclinical genital HPV infection occurs more frequently than visible genital warts among both men and women. Subclinical infection of the cervix is most commonly diagnosed by Pap screening with the detection of squamous intraepithelial lesions. The application of 3%--5% acetic acid usually turns HPV-infected genital mucosal tissue a whitish color. However, acetic acid application is not a specific test for HPV infection, and the specificity and sensitivity of this procedure for screening have not been defined. Thus, the routine use of this procedure for screening to detect subclinical infection is not recommended. However, some experienced clinicians find this test useful for identification of flat genital warts. A definitive diagnosis of HPV infection is based on detection of viral nucleic acid (DNA or RNA) or capsid protein. Pap-test diagnosis of HPV does not always correlate with detection of HPV DNA in cervical cells. Cell changes attributed to HPV in the cervix are similar to those of SIL and often regress spontaneously without treatment. Tests that detect several types of HPV DNA in cells scraped from the cervix are available and may be useful in the triage of women with atypical squamous cells of undetermined significance (ASCUS) but not other types of cytologic abnormalities. Screening for subclinical genital HPV infection using DNA or RNA tests is not recommended. Treatment In the absence of coexistent SIL, treatment is not recommended for subclinical genital HPV infection diagnosed by colposcopy, biopsy, acetic acid application, or the detection of HPV by laboratory tests. The diagnosis of subclinical genital HPV infection is often not definitive, and no therapy has been identified that eradicates infection. In the presence of coexistent SIL, management should be based on histopathologic findings. Management of Sex Partners Examination of sex partners is unnecessary. Most sex partners of infected patients probably are already infected subclinically with HPV. No screening tests for subclinical infection are available. Likewise, whether patients who have subclinical HPV infection are as infectious as patients who have exophytic warts is unknown. Cervical Cancer Screening for Women Who Attend STD Clinics or Have a History of STDsWomen with a history of STD may be at increased risk for cervical cancer, and women attending STD clinics may have other risk factors that place them at even greater risk. Prevalence studies have determined that precursor lesions for cervical cancer occur about five times more frequently among women attending STD clinics than among women attending family planning clinics (92). The cervical Pap test is an effective, low-cost screening test for preventing invasive cervical cancer. Recommendations regarding Pap testing intervals vary in the United States (93,94,10). However, if a woman has three consecutive negative annual Pap tests, future screening tests may be performed less frequently. RecommendationsAt the time of a pelvic examination for STD screening, the health-care provider should inquire about the result of the patient's last Pap test and discuss the following information with the patient:
If a woman has not had a Pap test during the previous 12 months, a Pap test may be obtained as part of the routine pelvic examination. Health-care providers should be aware that many women believe they have had a Pap test when they actually have received only a pelvic examination, and thus may report having had a recent Pap test. Therefore, in STD clinics, a Pap test should be strongly considered during the routine clinical evaluation of women who do not have clinical-record documentation of having had a normal Pap test within the preceding 12--36 months. A woman may benefit from receiving printed information about Pap tests and a report containing a statement that a Pap test was obtained during her clinic visit. If possible, a copy of the Pap test result should be provided to the patient for her records. Follow-Up Clinicians who offer Pap test screening services are encouraged to use cytopathology laboratories that report results using the Bethesda System of classification†††. If the results of the Pap test are abnormal, care should be provided according to the Interim Guidelines for Management of Abnormal Cervical Cytology published by the National Cancer Institute Consensus Panel (95). Appropriate follow-up of Pap tests showing high-grade SIL always includes referral to a clinician who can provide a colposcopic examination of the lower genital tract and, if indicated, colposcopically directed biopsy. For patients who have a Pap test indicative of low-grade SIL or ASCUS, follow-up without colposcopy may be acceptable in some circumstances. Such follow-up would involve repeat Pap tests every 4--6 months for 2 years until the results of three consecutive tests are negative. If repeat tests show persistent abnormalities, colposcopy and directed biopsy may be indicated. However, if compliance with follow-up is in question, women with low-grade SIL or ASCUS may be considered for colposcopy. If specific infections other than HPV are identified, the patient should be reevaluated after appropriate treatment for those infections. In all follow-up strategies using repeat Pap tests, the tests not only must be negative but also must be interpreted by the laboratory as "satisfactory for evaluation." Tests determined by the laboratory to be "satisfactory but limited by…" in conjunction with a diagnosis of "negative" or "within normal limits" are also considered negative. Another strategy for management of patients with ASCUS Pap tests involves testing for HPV DNA. If high-risk types of HPV DNA are detected, women with ASCUS tests are referred immediately for colposcopy. Because many public health clinics, including most STD clinics, cannot provide clinical follow-up of abnormal Pap tests, women with Pap tests demonstrating high grade SIL, persistent low-grade SIL, or ASCUS usually need a referral to other local health-care providers or clinics for colposcopy and biopsy. Clinics and health-care providers who offer Pap test screening services but cannot provide appropriate colposcopic follow-up of abnormal Pap tests should arrange referral to services in which a) a patient will be promptly evaluated and treated and b) the results of the evaluation will be reported to the referring clinic or health-care provider. Clinics and health-care providers should develop protocols that identify women who miss follow-up appointments so that these women can be scheduled for repeat Pap tests, and they should reevaluate such protocols routinely. Pap test results, type and location of follow-up appointments, and results of follow-up should be clearly documented in the clinic record. The establishment of colposcopy and biopsy services in local health departments, especially in circumstances where referrals are difficult and follow-up is unlikely, should be considered. Other Management Considerations Other considerations in performing Pap tests are as follows.
Special ConsiderationsPregnancy Pregnant women should have a Pap test as part of routine prenatal care. A cytobrush may be used for obtaining Pap tests in pregnant women, although care should be taken not to disrupt the mucous plug. HIV Infection Several studies have documented an increased prevalence of SIL in HIV-infected women (96). The following recommendations for Pap test screening among HIV-infected women are consistent with other guidelines published by the U.S. Department of Health and Human Services (21) and are based partially on the opinions of professionals knowledgeable in the care and management of cervical cancer and HIV infection in women. After obtaining a complete history of previous cervical disease, HIV-infected women should be provided a comprehensive gynecologic examination, including a pelvic examination and Pap test, as part of their initial evaluation. A Pap test should be obtained twice in the first year after diagnosis of HIV infection and, if the results are normal, annually thereafter. If the results of the Pap test are abnormal, care should be provided according to the Interim Guidelines for Management of Abnormal Cervical Cytology (97). Women who have a cytological diagnosis of high-grade SIL or squamous cell carcinoma should undergo colposcopy and directed biopsy. HIV infection is not an indication for colposcopy in women who have normal Pap tests. Vaccine Preventable STDsThe most effective means to prevent transmission of infectious diseases, including STDs, is through preexposure immunization. Vaccines are available for prevention of HAV and HBV, both of which can be transmitted sexually. Vaccines are under development or are undergoing clinical trials for other STDs, including HIV, HPV, and HSV; however, current efforts regarding vaccination focus largely on integrating use of currently available vaccines into STD prevention and treatment activities. Every person seeking treatment for an STD should be considered a candidate for hepatitis B vaccination, and some persons (e.g., MSM and injection-drug users) should be considered for hepatitis A vaccination. Evaluation for vaccination is most effectively done through a screening and education process that both inquires about risk factors for infection (e.g., sex partners and use of illegal drugs), educates patients about the importance of vaccination, and excludes persons who are not candidates for vaccination (e.g., laboratory confirmed diagnosis of infection and previous vaccination). Although it is uncommon, patients may present with signs, symptoms, or laboratory findings of acute or chronic viral hepatitis. When this occurs, a precise diagnosis must be made and appropriate clinical services provided, including postexposure immunization of contacts and medical referral. Hepatitis AHepatitis A, caused by infection with HAV, has an incubation period from time of exposure to onset of symptoms of approximately 4 weeks (range: 15--50 days). HAV replicates in the liver and is shed in high concentrations in feces from 2 weeks before to 1 week after the onset of clinical illness. HAV is most commonly transmitted by the fecal-oral route. Although viremia occurs early in infection and can persist for several weeks after onset of symptoms, bloodborne transmission of HAV is uncommon. HAV infection produces a self-limited disease that does not result in chronic infection or chronic liver disease. However, 10%--15% of patients may experience a relapse of symptoms during the 6 months after acute illness. Acute liver failure from hepatitis A is rare (0.3% overall case-fatality rate), but occurs more frequently in older persons (1.8% case fatality rate in adults >50 years of age) and persons with underlying chronic liver disease. The risk for symptomatic infection is directly related to age, with >80% of adults having symptoms compatible with acute viral hepatitis and most children having either asymptomatic or unrecognized infection. Antibody produced in response to HAV infection persists for life and confers protection against reinfection. Approximately 33% of the U.S. population has serologic evidence of prior HAV infection, which increases directly with age and reaches 75% among persons aged >70 years. Most cases of hepatitis A result from person-to-person transmission during community-wide outbreaks. The most frequently reported source of infection (12%--26%) is either household or sexual contact with a person who had hepatitis A. In addition, outbreaks regularly occur among users of injection and non-injection drugs and among MSM. In the United States, up to 10% of reported cases of HAV occur among persons reporting these behaviors. Approximately 50% of persons with hepatitis A do not have an identified source for their infection. Hepatitis A, like other enteric infections, can be transmitted during sexual activity. Recent outbreaks of hepatitis A among MSM have occurred in urban areas in the United States. Although some studies have associated having a greater number of sex partners, frequent oral-anal contact, insertive anal intercourse, or serologic evidence of other STDs with HAV infection, other studies have not found specific risk factors for infection. Unlike persons with most other STDs, HAV-infected persons are infectious for only a relatively brief period of time. However, many sexual practices facilitate fecal-oral transmission of HAV, and inapparent fecal contamination is commonly present during sexual intercourse. Measures typically used to prevent the transmission of other STDs (e.g., use of condoms) do not prevent HAV transmission, and maintenance of "good personal hygiene" has not been successful in interrupting outbreaks of hepatitis A. Vaccination is the most effective means of preventing HAV transmission among persons at risk for sexual transmission of this virus and among persons who use injection and non-injection illegal drugs, many of whom may seek services in STD clinics. Diagnosis The diagnosis of hepatitis A cannot be made on clinical grounds alone and requires serologic testing, which is available commercially. The presence of IgM antibody to HAV is diagnostic of acute HAV infection. A positive test for total anti-HAV indicates immunity to HAV infection but does not differentiate acute from past HAV infection. Tests can be positive after hepatitis A vaccination. Treatment Patients with hepatitis A usually require only supportive care, with no restrictions in diet or activity. Hospitalization may be necessary for patients who become dehydrated because of nausea and vomiting and for patients with signs or symptoms of acute liver failure. Medications that might cause liver damage or are metabolized by the liver should be used with caution among persons with HAV. Prevention Two products are available for the prevention of hepatitis A: hepatitis A vaccine (Table 2) and immune globulin (IG) for IM administration (2). Inactivated hepatitis A vaccines are prepared from formalin-inactivated, cell-culture-derived HAV and have been available in the United States since 1995 for persons aged >2 years. Administered in a two-dose series, these vaccines induce protective antibody levels in virtually all adults. By 1 month after the first dose, 94%--100% of adults have protective antibody levels; 100% of adults develop protective antibody following a second dose. In randomized controlled trials, the equivalent of one dose of hepatitis A vaccine administered before exposure has been 94%--100% effective in preventing clinical hepatitis A (3). Kinetic models of antibody decline indicate that protective levels of antibody persist for at least 20 years. A combined hepatitis A and B vaccine has been developed for adults. When administered on a 0-, 1-, 6-month schedule, the vaccine has equivalent immunogenicity to that of the monovalent vaccines. IG is a sterile solution of concentrated immunoglobulins prepared from pooled human plasma processed by cold ethanol fractionation. In the United States, IG is produced only from plasma that has tested negative for HBV, antibody to HIV, and antibody to HCV. In addition, the manufacturing process must either include a viral inactivation step or the final product must test negative for HCV RNA. When administered before or within 2 weeks after exposure to HAV, IG is >85% effective in preventing hepatitis A. Preexposure Immunization Persons in the following groups should be offered hepatitis A vaccine:
Hepatitis A vaccine currently is available for children and adolescents aged <19 years through the Vaccines for Children (VFC) program (tel: 800-232-2522). Prevaccination Serologic Testing for Susceptibility Screening for HAV infection may be cost-effective in populations where the prevalence of infection is likely to be high (e.g., older persons and persons born in areas of high HAV endemicity). The potential cost-savings of testing should be weighed against the likelihood that testing will interfere with initiating vaccination. Vaccination of a person who is already immune is not harmful. Postvaccination Serologic Testing Postvaccination serologic testing is not indicated because most persons respond to vaccine. In addition, the commercially available serologic test is not sensitive enough to detect the low, but protective, levels of antibody produced by vaccination. Postexposure Prophylaxis Previously unvaccinated persons exposed to HAV (e.g., through household or sexual contact or by sharing illegal drugs with a person who has hepatitis A) should be administered a single IM dose of IG (0.02 mL/kg) as soon as possible, but not >2 weeks after exposure. Persons who have had one dose of hepatitis A vaccine at least 1 month before exposure to HAV do not need IG. If hepatitis A vaccine is recommended for a person receiving IG, it can be administered simultaneously at a separate anatomic injection site. The use of hepatitis A vaccine alone is not recommended for postexposure prophylaxis. Special Considerations Limited data indicate that vaccination of HIV-infected persons results in lower seroprotection rates and antibody concentrations (3). Antibody response may be directly related to CD4+ levels. Hepatitis BHepatitis B is caused by infection with HBV. The incubation period from time of exposure to onset of symptoms is 6 weeks to 6 months. HBV is hepatotropic, is found in highest concentrations in the blood, and is found in lower concentrations in other body fluids (e.g., semen, vaginal secretions, and wound exudates). HBV infection can be self-limited or chronic. In adults, only 50% of acute HBV infections are symptomatic, and about 1% of cases result in acute liver failure and death. Risk for chronic infection is associated with age at infection: about 90% of infected infants and 60% of infected children aged <5 years become chronically infected compared with 2%--6% of adults. Among persons with chronic HBV infection, the risk of death from cirrhosis or hepatocellular carcinoma is 15%--25%. In the United States, an estimated 181,000 persons were infected with HBV in 1998, and about 5,000 deaths occurred from HBV-related cirrhosis or hepatocellular carcinoma. An estimated 1.25 million people are chronically infected with HBV, serve as a reservoir for infection, and are at increased risk for death from chronic liver disease. HBV is efficiently transmitted by percutaneous or mucous membrane exposure to infectious body fluids. Sexual transmission among adults accounts for most HBV infections in the United States. In the 1990s, transmission among hetero-sexual partners accounted for about 40% of infections, and transmission among MSM accounted for another 15% of infections. The most common risk factors for heterosexual transmission include having multiple sex partners (i.e., more than one partner in a 6-month period) or a recent history of an STD. Risk factors for infection among MSM include having multiple sex partners, engaging in unprotected receptive anal intercourse, and having a history of other STDs. Changes in sexual practices among MSM to prevent HIV infection have resulted in a lower risk for HBV infection than that observed in the late 1970s, when studies found up to 70% prevalence of HBV markers among adult MSM. Recent surveys of young MSM (aged 15--22 years) indicated that 6%--13% of participants had evidence of HBV infection, whereas 3%--27% had evidence of having been immunized against hepatitis B (98). Among persons with acute hepatitis B, up to 70% have previously received care in settings where they could have been vaccinated (e.g., STD clinics, drug treatment programs, and correctional facilities). A 1997 survey of STD clinics demonstrated that hepatitis B vaccine was routinely offered in only 5% of these settings. Diagnosis The diagnosis of acute or chronic HBV infection cannot be made on clinical grounds, but requires serologic testing (Table 3). Hepatitis B surface antigen (HBsAg) is present in either acute or chronic infection. The presence of IgM antibody to hepatitis B core antigen (IgM anti-HBc) is diagnostic of acute HBV infection. Antibody to HBsAg (anti-HBs) is produced following a resolved infection and is the only HBV antibody marker present following immunization. The presence of HBsAg with a negative test for IgM anti-HBc is indicative of chronic HBV infection. The presence of anti-HBc may indicate either acute, resolved, or chronic infection. Treatment Laboratory testing should be used to confirm suspected acute or chronic HBV infection, and infected persons should be referred for medical follow-up and possible treatment of chronic infection. In addition, contacts should be vaccinated (see Exposure to Persons who have Acute Hepatitis B) and receive postexposure prophylaxis. No specific therapy is available for persons with acute HBV infection; treatment is supportive. Antiviral agents (i.e., alpha-interferon or lamivudine) are available for treatment of persons with chronic hepatitis B. To determine the likelihood of response to treatment, an initial evaluation is required to determine the status of the chronic HBV infection and the extent of liver disease. For this reason, treatment should be offered by health-care professionals with experience in the treatment of hepatitis B. Prevention Two products have been approved for hepatitis B prevention: hepatitis B immune globulin (HBIG) and hepatitis B vaccine. HBIG is prepared from plasma known to contain a high titer of anti-HBs and is used for postexposure prophylaxis. The recommended dose of HBIG for children and adults is 0.06 mL/kg. The dose is 0.5 mL to prevent perinatal HBV infection among infants born to HBsAg-positive mothers. Hepatitis B vaccine uses HBsAg produced in yeast by recombinant DNA technology and provides protection from HBV infection when used for both preexposure immunization and postexposure prophylaxis. The two available monovalent hepatitis B vaccines for use in adolescents and adults are Recombivax HB® (Merck and Co., Inc.) and Engerix-B (SmithKline Beecham Biologicals). The recommended vaccine dose varies by product and age of recipient (Table 4). Vaccine should be administered IM in the deltoid muscle and can be administered simultaneously with other vaccines. Many vaccination schedules have been used for both adults and adolescents. A two-dose schedule has been approved for adolescents aged 11--15 years using the adult dose of Recombivax HB®. If the vaccination series is interrupted after the first or second dose of vaccine, the missed dose should be administered as soon as possible. The series does not need to be restarted if a dose has been missed. In adolescents and healthy adults aged <40 years, approximately 50% develop a protective antibody response (anti-HBs >10 mIU/mL) after the first vaccine dose, 70% after the second, and >90% after the third dose. Because relatively high rates of protection are achieved following each vaccine dose, hepatitis B vaccination should be initiated even if completion of the series cannot be ensured. Because most fully vaccinated persons have long-lasting protection from HBV infection, periodic testing to determine antibody levels in immune competent persons is not necessary, and booster doses of vaccine are not recommended. Hepatitis B vaccine has been shown to be safe; more than 20 million adolescents and adults have been vaccinated in the United States. The vaccine is well tolerated by most recipients. Pain at the injection site or low grade fever are reported by a minority of recipients. Anaphylaxis is estimated to occur in one in 600,000 doses of vaccine administered; no deaths have been reported following anaphylaxis. Hepatitis B vaccine has not been associated with multiple sclerosis, diabetes, or other autoimmune or neurologic diseases in any controlled epidemiologic study. Vaccine is contraindicated in persons with a history of anaphylaxis after a previous dose of hepatitis B vaccine and in persons with a known anaphylactic reaction to yeast. CDC's national immunization strategy to eliminate transmission of HBV infection includes a) prevention of perinatal infection through maternal HBsAg screening and postexposure prophylaxis of at-risk infants, b) universal infant immunization, c) universal immunization of previously unvaccinated adolescents aged 11--12 years (99), and d) vaccination of adolescents and adults at increased risk for infection (100). Although high immunization coverage rates have been achieved among infants and younger adolescents, hepatitis B incidence rates remain high because most infections now occur in adults. Although the cost of vaccine remains a barrier to adult vaccination, vaccine purchase and provider reimbursement should not be a barrier for vaccination of adolescents aged <19 years, who may be eligible for free vaccine under the Vaccines for Children (VFC) program (tel: 800-232-2522). Preexposure Immunizations Hepatitis B vaccine is recommended for all persons who attend STD clinics who have not been previously vaccinated. In the non-STD clinic setting, the following persons should be vaccinated: a) persons with history of an STD, persons who have had multiple sex partners, those who have had sex with an injection-drug user, and sexually active MSM; b) persons engaging in illegal drug use; c) household members, sex partners, and drug-sharing partners of a person with chronic HBV infection; and d) persons on hemodialysis, persons receiving clotting factor concentrates, or persons who have occupational exposure to blood. In addition, hepatitis B vaccine should be offered to all persons who have not been previously vaccinated who receive services in drug treatment programs and long-term correctional facilities. Prevaccination Antibody Screening Based on the current cost of hepatitis B vaccine, revaccination serologic testing may be cost-effective in adult populations with a high prevalence of HBV infection (>2% HBsAg positive or >30% anti-HBc positive). However, prevaccination testing is not cost-effective in any adolescent populations. Adult populations with high prevalence of HBV infection include injection-drug users, MSM, sexual contacts of persons with chronic HBV infection, and persons from countries with endemic HBV infection. When testing is performed, anti-HBc is the test of choice. Testing should not be a barrier to vaccination of susceptible persons, especially in populations that are difficult to access, and the first dose of vaccine should be administered at the same time that serologic testing is initiated. As hepatitis B vaccination becomes more widespread, more persons will present with a history of vaccination and most will not have a personal vaccination record. However, serologic testing in persons with a history of previous hepatitis B vaccination may not be helpful because of the loss of detectable antibody. Without a vaccination record, obtaining a careful history (e.g., number of doses, schedule, and age at immunization) is the only way to determine if the person most likely received the complete hepatitis B vaccine series. Administration of additional doses of vaccine beyond the three-dose series is not harmful. Postexposure Prophylaxis Exposure to Persons Who Have Acute Hepatitis B Sex Contacts. Previously unvaccinated sex partners of persons with acute hepatitis B should receive postexposure immunization with HBIG and hepatitis B vaccine within 14 days after the most recent sexual contact. HBIG has been shown to be required for effective postexposure protection in this setting. Administration of vaccine with HBIG in this setting confers long-term protection in the event the person with acute hepatitis B becomes chronically infected; simultaneous administration of HBIG and hepatitis B vaccine does not reduce vaccine effectiveness. Testing sex partners for susceptibility to HBV infection (anti-HBc) can be considered if it does not delay postexposure immunization beyond 14 days. Nonsexual Household Contacts. Nonsexual household contacts of patients who have acute hepatitis B are not at increased risk for infection unless they have other risk factors or are exposed to the patient's blood (e.g., by sharing a toothbrush or razor blade). However, vaccination of household contacts is encouraged, especially for children and adolescents. If the patient with acute hepatitis B becomes chronically infected (i.e., remains HBsAg-positive after 6 months), all household contacts should be vaccinated. Exposure to Persons Who Have Chronic HBV Infection Most HBsAg-positive persons are identified during routine screening (e.g., blood donation and prenatal evaluation) or clinical evaluation. Active postexposure prophylaxis with hepatitis B vaccine alone is recommended for sex or needle-sharing partners and non-sexual household contacts of persons with chronic HBV infection. Because identifying the time of the last contact can be difficult, hepatitis B vaccination provides both preexposure and postexposure protection. Although the effectiveness of active postexposure immunization has not been evaluated for sex contacts of persons with chronic HBV infection, it provides high-level protection (90%) against perinatal HBV infection, where the intensity of exposure is greater than that among household or sex contacts of chronically infected persons. Postvaccination testing (anti-HBs) should be considered for sex partners of persons with chronic HBV infection. Although most persons are expected to respond to vaccination, those found to be antibody-negative should receive a second, complete vaccination series. Those persons found to be antibody-negative after revaccination should be counseled about abstinence and the use of other methods to protect themselves from sexual HBV transmission. Special Considerations Pregnancy All pregnant women receiving STD services should be tested for HBsAg, regardless of whether they have been previously tested. If positive, this test result should be reported to state perinatal immunization or HBV prevention programs to ensure proper case management of the mother and appropriate postexposure immunization of her at-risk infant. HBsAg-negative pregnant women seeking STD treatment who have not been previously vaccinated should receive hepatitis B vaccine, as pregnancy is not a contraindication to vaccination. HIV Infection HBV infection in HIV-infected persons is more likely to result in chronic HBV infection. HIV infection also can impair the response to hepatitis B vaccine. Therefore, HIV-infected persons who are vaccinated should be tested for anti-HBs 1--2 months after the third vaccine dose. Revaccination with three more doses should be considered for persons who do not respond initially to vaccination. Those who do not respond to additional doses should be advised that they might remain susceptible to HBV infection and should be counseled in the use of methods to prevent HBV infection. Victims of Sexual Assault Studies have not determined the frequency with which HBV infection occurs following sexual abuse or rape. Fully vaccinated victims of sexual assault are protected from HBV infection and do not need further doses. For a victim who is not fully vaccinated, the vaccine series should be completed as scheduled. Unvaccinated persons in this setting should be administered active postexposure prophylaxis (i.e., vaccine alone) upon the initial clinical evaluation. Unless the offender is known to have acute hepatitis B, HBIG is not required. Because sexual abuse of children frequently occurs over a prolonged period of time, the last exposure is often difficult to determine. However, when sexual abuse is identified, hepatitis B vaccination should be initiated in previously unvaccinated children. Hepatitis CHCV infection is the most common chronic bloodborne infection in the United States; an estimated 2.7 million persons are chronically infected (101). More than two thirds of all infected persons are aged <50 years. Persons with acute HCV infection typically are either asymptomatic or have a mild clinical illness. The average time from exposure to seroconversion is 8--9 weeks, and antibodies to HCV (anti-HCV) can be detected in >97% of persons by 6 months after exposure. Chronic HCV infection develops in most persons (75%--85%) after acute infection; 60%--70% have evidence of active liver disease. Most infected persons may not be aware of their infection because they are not clinically ill. However, infected persons serve as a source of transmission to others and are at risk for chronic liver disease or other HCV-related chronic diseases for at least 2 decades after infection. HCV is most efficiently transmitted by direct percutaneous exposure to infected blood (e.g., by receipt of blood transfusion from an infected donor or through use of injection drugs). Although less efficient, occupational, perinatal, and sexual exposures also can result in transmission of HCV. No association has been documented between HCV and military service or HCV and exposures resulting from medical, dental, or surgical procedures; tattooing; acupuncture; ear piercing; or foreign travel (102). The greatest variation in prevalence of HCV infection occurs among persons with different risk factors for infection. The highest prevalence of infection is found among those with substantial or repeated direct percutaneous exposures to blood (e.g., IDUs, persons with hemophilia treated with clotting factor concentrates produced before 1987, and recipients of transfusions from HCV-positive donors). Moderate prevalence is found among persons with frequent but limited direct percutaneous exposures (e.g., long-term hemodialysis patients). Lower prevalence occurs among persons with inapparent percutaneous or mucosal exposures or sexual exposure and among those with limited, sporadic percutaneous exposures (e.g., health-care workers). Lowest prevalence of HCV infection is found among persons with no high-risk characteristics (e.g., blood donors). Sexual ActivityAlthough the role of sexual activity in the transmission of HCV remains controversial, results from several types of studies indicate that sexual activity is associated with HCV transmission (103,104). These studies reported independent associations between HCV infection and a) exposure to an infected sex partner, b) increasing numbers of partners, c) failure to use a condom, d) history of STD, e) heterosexual sex with a male IDU, and f) sexual activities involving trauma. In contrast, a low prevalence (average: 1.5%; range: 0%--4.4%) of HCV infection has been demonstrated in studies of long-term spouses of patients with chronic HCV infection who had no other risk factors for infection. One study has found an association between HCV infection and male homosexual activity, and at least in STD clinic settings, the prevalence rate of HCV infection among MSM generally has been similar to that of heterosexuals (105). Because sexual transmission of bloodborne viruses is more efficient among homosexual men compared with heterosexual men and women, it is unclear why HCV infection rates are not substantially higher among MSM compared with heterosexuals. This observation and the low prevalence of HCV infection observed among the long-term steady sex partners of persons with chronic HCV infection have raised doubts about the importance of sexual activity in the transmission of HCV. Unacknowledged percutaneous exposures (i.e., illegal injection-drug use) might contribute to increased risk for HCV infection among such persons. Although inconsistencies exist between studies, data indicate overall that sexual transmission of HCV can occur and accounts for up to 20% of HCV infections (102). The substantial contribution of sexual transmission to the disease burden in the United States relative to the inefficiency with which the virus appears to be spread in this manner can be explained. Because sexual activity with multiple partners is a common behavior among chronically infected persons and because of the substantial number of these persons, multiple exposure opportunities exist. However, more data are needed to determine the risk for, and factors related to, transmission of HCV between sex partners, including whether other STDs promote the transmission of HCV by influencing viral load or modifying mucosal barriers. Increased HCV viral load or coinfection with HIV (known to increase perinatal transmission of HCV) may increase the risk for sexual transmission. A recent study involving hemophilic men demonstrated that dually infected men had a higher HCV load than those infected with HCV alone, and that a higher HCV load was associated, though not significantly, with an increased risk for HCV transmission to female partners (106). Diagnosis and TreatmentThe diagnosis of HCV infection can be made by detecting either anti-HCV or HCV RNA. Anti-HCV is recommended for routine testing of asymptomatic persons and should include use of both EIA to test for anti-HCV and a supplemental antibody test (i.e., recombinant immunoblot assay [RIBA]) for all positive anti-HCV results. In settings where clinical services for liver disease are provided, use of reverse transcriptase polymerase chain reaction (RT-PCR) to detect HCV RNA might be appropriate to confirm the diagnosis of HCV infection (e.g., in patients with abnormal alanine aminotransferase [ALT] levels or with indeterminant supplemental anti-HCV test results), although RT-PCR assays are not currently FDA-approved. Current approved therapy for HCV-related chronic liver disease includes alpha interferon alone or in combination with the oral agent ribavirin for a duration of 6--12 months. Because of advances in the field of antiviral therapy for chronic hepatitis C, standards of practice might change, and clinicians should consult with specialists knowledgeable about this virus. The National Institutes of Health Consensus Development Conference Panel recommended that therapy for hepatitis C be limited to those patients with persistently elevated ALT levels, detectable HCV RNA, and histologic evidence of progressive disease (as characterized by liver biopsy findings indicating either portal or bridging fibrosis or at least moderate degrees of inflammation and necrosis). PreventionNo vaccine for hepatitis C is available, and prophylaxis with immune globulin is not effective in preventing HCV infection after exposure. Reducing the burden of HCV infection and disease in the United States requires implementation of both primary and secondary prevention activities. Primary prevention reduces or eliminates HCV transmission; secondary prevention activities reduce liver and other chronic diseases in HCV-infected persons by identifying them and providing appropriate medical management and antiviral therapy, if necessary (102). Persons seeking care in STD clinics or other primary-care settings should be screened for risk factors for HCV infection, and those with the following risk factors should be offered counseling and testing:
Regardless of test results, persons who use illegal drugs or have multiple sex partners should be provided with information regarding how to reduce their risk for acquiring bloodborne and sexually transmitted infections and how to avoid transmitting infectious agents to others (e.g., through vaccination against hepatitis B and, if appropriate, hepatitis A). Persons who inject drugs should be counseled to stop using and get into a treatment program. If they are found at any follow-up visit to be continuing the use of these drugs, they should be counseled on how to inject safely (i.e., use of sterile, single-use equipment, including needles, syringes, cookers, cottons, and water each and every time they inject). Persons with multiple sex partners should be counseled regarding how to reduce the transmission of STDs (e.g., through abstinence or by decreasing the number of sex partners). Persons who test negative for HCV who had a previous exposure should be reassured that they have not been exposed. Persons who test positive for HCV infection should be provided information regarding how to protect their liver from further harm, how to prevent transmission to others, and the need for medical evaluation for chronic liver disease (CLD) and possible treatment. To protect their liver from further harm, HCV-positive persons should be advised to avoid alcohol, avoid taking any new medicines (including over-the-counter and herbals) without checking with their doctor, and become vaccinated against hepatitis A or hepatitis B if they are not immune. To reduce the risk for transmission to others, HCV-positive persons should be advised not to donate blood, body organs, other tissue, or semen and not to share any personal items that may have blood on them (e.g., toothbrushes and razors). HCV-positive persons with one long-term, steady sex partner do not need to change their sexual practices. They should discuss the low but present risk for transmission with their partner and discuss the need for counseling and testing. HCV-positive women do not need to avoid pregnancy or breastfeeding. Postexposure Follow-UpNo postexposure prophylaxis is effective against HCV. Testing to determine whether HCV infection has developed is recommended for health-care workers after percutaneous or permucosal exposures to HCV-positive blood and for children born to HCV-positive women. Proctitis, Proctocolitis, and EnteritisSexually transmitted gastrointestinal syndromes include proctitis, proctocolitis, and enteritis. Evaluation for these syndromes should include appropriate diagnostic procedures (e.g., anoscopy or sigmoidoscopy, stool examination, and culture). Proctitis is inflammation limited to the rectum (the distal 10--12 cm) that may be associated with anorectal pain, tenesmus, or rectal discharge. N. gonorrhoeae, C. trachomatis (including LGV serovars), T. pallidum, and HSV are the most common sexually transmitted pathogens involved. In patients coinfected with HIV, herpes proctitis may be especially severe. Proctitis occurs predominantly among persons who participate in receptive anal intercourse. Proctocolitis is associated with symptoms of proctitis plus diarrhea or abdominal cramps and inflammation of the colonic mucosa extending to 12 cm above the anus. Fecal leukocytes may be detected on stool examination depending on the pathogen. Pathogenic organisms include Campylobacter sp., Shigella sp., Entamoeba histolytica, and, rarely, LGV serovars of C. trachomatis. CMV or other opportunistic agents may be involved in immunosuppressed HIV-infected patients. Proctocolitis can be acquired by the oral route or by oral-fecal contact, depending on the pathogen. Enteritis usually results in diarrhea and abdominal cramping without signs of proctitis or proctocolitis; it occurs among persons whose sexual practices include oral-fecal contact. In otherwise healthy persons, Giardia lamblia is most frequently implicated. When outbreaks of gastrointestinal illness occur among social or sexual networks of MSM, clinicians should consider sexual transmission as a mode of spread and counsel accordingly. Among HIV-infected patients, gastrointestinal illness can be caused by other infections that usually are not sexually transmitted, including CMV, Mycobacterium avium-intracellulare, Salmonella sp., Campylobacter sp., Shigella sp., Cryptosporidium, Microsporidium, and Isospora. Multiple stool examinations may be necessary to detect Giardia, and special stool preparations are required to diagnose cryptosporidiosis and microsporidiosis. Additionally, enteritis may be directly caused by HIV infection. When laboratory diagnostic capabilities are available, treatment decisions should be based on the specific diagnosis. Diagnostic and treatment recommendations for all enteric infections are beyond the scope of these guidelines. TreatmentAcute proctitis of recent onset among persons who have recently practiced receptive anal intercourse is usually sexually acquired. Such patients should be examined by anoscopy and should be evaluated for infection with HSV, N. gonorrhoeae, C. trachomatis, and T. pallidum. If an anorectal exudate is found on examination, or if polymorphonuclear leukocytes are found on a Gram-stained smear of anorectal secretions, the following therapy may be prescribed pending results of additional laboratory tests.
NOTE: Patients with suspected or documented herpes proctitis should be managed in the same manner as those with genital herpes (see Management of HSV Infection). If painful perianal ulcers are present or mucosal ulcers are seen on anoscopy, presumptive therapy should include a regimen for treating genital herpes. Follow-UpFollow-up should be based on specific etiology and severity of clinical symptoms. Reinfection may be difficult to distinguish from treatment failure. Management of Sex PartnersPartners of patients with sexually transmitted enteric infections should be evaluated for any diseases diagnosed in the index patient. Ectoparasitic InfectionsPediculosis PubisPatients who have pediculosis pubis (i.e., pubic lice) usually seek medical attention because of pruritus or because they notice lice or nits on their pubic hair. Pediculosis pubis is usually transmitted by sexual contact.
Lindane toxicity, as indicated by seizure and aplastic anemia, has not been reported when treatment was limited to the recommended 4-minute period. Permethrin has less potential for toxicity than lindane. Other Management Considerations The recommended regimens should not be applied to the eyes. Pediculosis of the eyelashes should be treated by applying occlusive ophthalmic ointment to the eyelid margins twice a day for 10 days. Bedding and clothing should be decontaminated (i.e., machine-washed, machine-dried using the heat cycle, or dry-cleaned) or removed from body contact for at least 72 hours. Fumigation of living areas is not necessary. Patients with pediculosis pubis should be evaluated for other sexually transmitted diseases. Follow-Up Patients should be evaluated after 1 week if symptoms persist. Re-treatment may be necessary if lice are found or if eggs are observed at the hair-skin junction. Patients who do not respond to one of the recommended regimens should be re-treated with an alternative regimen. Management of Sex Partners Sex partners within the last month should be treated. Patients should avoid sexual contact with their sex partner(s) until patients and partners have been treated and reevaluated to rule out persistent disease. Special Considerations Pregnancy Pregnant and lactating women should be treated with either permethrin or pyrethrins with piperonyl butoxide; lindane is contraindicated in pregnancy. HIV Infection Patients who have pediculosis pubis and also are infected with HIV should receive the same treatment regimen as those who are HIV-negative. ScabiesThe predominant symptom of scabies is pruritus. Sensitization to Sarcoptes scabiei must occur before pruritus begins. The first time a person is infected with S. scabiei, sensitization takes up to several weeks to develop. However, pruritus might occur within 24 hours after a subsequent reinfestation. Scabies in adults often is sexually acquired, although scabies in children usually is not.
NOTE: Lindane should not be used immediately after a bath or shower, and it should not be used by persons who have extensive dermatitis, pregnant or lactating women, or children aged <2 years. Permethrin is effective and safe but costs more than lindane. Lindane is effective in most areas of the United States; however, lindane resistance has been reported in some areas of the world, including parts of the United States. Seizures have occurred when lindane was applied after a bath or used by patients who had extensive dermatitis. Aplastic anemia following lindane use also has been reported. One study has demonstrated increased mortality among elderly, debilitated persons who received ivermectin, but this observation has not been confirmed in subsequent reports. Other Management Considerations Bedding and clothing should be decontaminated (i.e., either machine-washed, machine-dried using the hot cycle, or dry-cleaned) or removed from body contact for at least 72 hours. Fumigation of living areas is unnecessary. Crusted Scabies Crusted scabies (i.e., Norwegian scabies) is an aggressive infestation that usually occurs in immunodeficient, debilitated, or malnourished persons. Patients who are receiving systemic or potent topical glucocorticoids, organ transplant recipients, mentally retarded or physically incapacitated persons, HIV-infected or human T-lymphotrophic virus-1 (HTLV-1)-infected persons, and persons with various hematologic malignancies are at risk for developing crusted scabies. Crusted scabies is associated with greater transmissibility than scabies. No controlled therapeutic studies for crusted scabies have been conducted, and the appropriate treatment remains unclear. Substantial treatment failure might occur with single topical scabicide or oral ivermectin treatment. Some specialists recommend combined treatment with a topical scabicide and oral ivermectin or repeated treatments with ivermectin. Lindane should be avoided because of risks of neurotoxicity with heavy applications and denuded skin. Patient's fingernails should be closely trimmed to reduce injury from excessive scratching. Follow-Up Patients should be informed that the rash and pruritus of scabies may persist for up to 2 weeks after treatment. Symptoms or signs that persist for >2 weeks can be attributed to several factors. Treatment failure may be caused by resistance to medication or by faulty application of topical scabicides. Patients with crusted scabies may have poor penetration into thick scaly skin and harbor mites in these difficult-to-penetrate layers. Particular attention must be given to the fingernails of these patients. Reinfection from family members or fomites may occur in the absence of appropriate contact treatment and washing of bedding and clothing. Even when treatment is successful and reinfection is avoided, symptoms may persist or worsen as a result of allergic dermatitis. Finally, household mites might cause symptoms to persist as a result of cross-reactivity between antigens. Some specialists recommend re-treatment after 1--2 weeks for patients who are still symptomatic; others recommend re-treatment only if live mites are observed. Patients who do not respond to the recommended treatment should be re-treated with an alternative regimen. Management of Sex Partners and Household Contacts Both sexual and close personal or household contacts within the preceding month should be examined and treated. Management of Outbreaks in Communities, Nursing Homes, and Other Institutional Settings Scabies epidemics often occur in nursing homes, hospitals, residential facilities, and communities. Control of an epidemic can only be achieved by treatment of the entire population at risk. Ivermectin can be considered in this setting, especially if treatment with topical scabicides fails. Epidemics should be managed in consultation with a specialist. Special Considerations Infants, Young Children, and Pregnant or Lactating Women Infants, young children, and pregnant or lactating women should not be treated with lindane. They can be treated with permethrin. Ivermectin is not recommended for pregnant or lactating patients. The safety of ivermectin in children who weigh <15 kg has not been determined. HIV Infection Patients who have uncomplicated scabies and also are infected with HIV should receive the same treatment regimens as those who are HIV-negative. HIV-infected patients and others who are immunosuppressed are at increased risk for crusted scabies. Such patients should be managed in consultation with a specialist. Sexual Assault and STDsAdults and AdolescentsThe recommendations in this report are limited to the identification, prophylaxis, and treatment of sexually transmitted infections and conditions commonly identified in the management of such infections. The documentation of findings, collection of non-microbiologic specimens for forensic purposes, and the management of potential pregnancy or physical and psychological trauma are beyond the scope of this report. Examinations of survivors of sexual assault should be conducted so as to minimize further trauma to the survivor and should be performed by an experienced clinician. The decision to obtain genital or other specimens for STD diagnosis should be made on an individual basis. Mechanisms to ensure continuity of care (including timely review of the results of any tests obtained) and to monitor compliance with and adverse reactions to any therapeutic or prophylactic regimens should be in place in any setting where survivors of sexual assault are examined. Laws in all 50 states strictly limit the evidentiary use of a survivor's prior sexual history, including evidence of previously acquired STDs, as part of an effort to undermine the credibility of the survivor's testimony. Evidentiary privilege against revealing any aspect of the examination or treatment is enforced in most states. In unanticipated, exceptional situations, STD diagnoses may later be accessed, and the survivor and clinician may opt to defer testing for this reason. However, collection of specimens at initial examination for laboratory STD diagnosis gives the survivor and clinician the option to defer empiric prophylactic antimicrobial treatment. Among sexually active adults, the identification of sexually transmitted infection after an assault is usually more important for the psychological and medical management of the patient than for legal purposes, because the infection could have been acquired before the assault. Trichomoniasis, BV, gonorrhea, and chlamydial infection are the most frequently diagnosed infections among women who have been sexually assaulted. Because the prevalence of these infections is high among sexually active women, their presence after an assault does not necessarily signify acquisition during the assault. A post-assault examination is, however, an opportunity to identify or prevent sexually transmitted infections, regardless of whether they were acquired during an assault. Chlamydial and gonococcal infections in women are of particular concern because of the possibility of ascending infection. In addition, post-assault evaluation can detect HBV infection, which may be prevented by postexposure administration of hepatitis B vaccine. Reproductive-aged female survivors should be evaluated for pregnancy, if appropriate. Evaluation for Sexually Transmitted InfectionsInitial Examination An initial examination should include the following procedures.
Follow-Up Examinations Although persons may have difficulty in complying with follow-up examinations several weeks following an assault, such examinations are essential because they provide an opportunity to a) detect new infections acquired during or after the assault; b) complete hepatitis B immunization, if indicated; and c) complete counseling and treatment for other STDs. Examination for STDs should be repeated within 1--2 weeks of the assault. Because infectious agents acquired through assault may not have produced sufficient concentrations of organisms to result in positive test results at the initial examination, a culture (or cultures), a wet mount, and other tests should be repeated at the follow-up visit unless prophylactic treatment was provided. If treatment was provided, testing should be done only if the survivor reports having symptoms. If treatment was not provided, follow-up examination should be conducted within a week to ensure that results of positive tests can be discussed promptly with the survivor and that treatment is provided. Serologic tests for syphilis and HIV infection should be repeated 6, 12, and 24 weeks after the assault if initial test results were negative and these infections are likely to be present in the assailant (see Risk of Acquiring HIV Infection). Prophylaxis Many specialists recommend routine preventive therapy after a sexual assault because follow-up of survivors of sexual assault can be difficult and because these persons may be reassured if offered treatment or prophylaxis for possible infection. The following prophylactic regimen is suggested as preventive therapy.
NOTE: For patients requiring alternative treatments, see the sections in this report that specifically address the appropriate agent. The efficacy of these regimens in preventing gonorrhea, trichomoniasis, BV, and C. trachomatis genitourinary infections after sexual assault has not been evaluated. Clinicians should counsel patients regarding the possible benefits, as well as the possible toxicity, associated with these treatment regimens; gastrointestinal side effects can occur with this combination. Providers may also consider anti-emetic medications if prophylaxis is administered, particularly if emergency contraception is also provided. Other Management Considerations At the initial examination and, if indicated, at follow-up examinations, patients should be counseled regarding the following:
Risk for Acquiring HIV Infection Although HIV-antibody seroconversion has been reported among persons whose only known risk factor was sexual assault or sexual abuse, the risk for acquiring HIV infection through a single episode of sexual assault is likely low. The overall probability of HIV transmission during a single act of intercourse from a person known to be HIV-infected, however, depends on many factors, and in specific circumstances could be high. These factors may include the type of sexual intercourse (i.e., oral, vaginal, or anal); presence of oral, vaginal, or anal trauma (including bleeding); site of exposure to ejaculate; viral load in ejaculate; and presence of an STD or genital lesions in assailant or survivor. Children may be at higher risk for transmission, because child sexual abuse is often associated with multiple episodes of assault and may result in mucosal trauma (see Sexual Assault or Abuse of Children). In certain circumstances, the potential of HIV transmission has been reduced by postexposure therapy for HIV with antiretroviral agents. Postexposure therapy with zidovudine has been associated with a reduced risk for HIV infection in a study of health-care workers who had percutaneous exposures to HIV-infected blood. On the basis of these results and the biologic plausibility of the effectiveness of antiretroviral agents in preventing infection, postexposure therapy has been recommended for health-care workers who have occupational exposures to HIV. The degree to which these findings can be extrapolated to other HIV-exposure situations, including sexual assault, is unknown. Although a definitive recommendation cannot be made regarding postexposure antiretroviral therapy after sexual exposure to HIV, such therapy should be considered in cases in which the risk for HIV exposure during the assault is likely high. Health-care providers who consider offering postexposure therapy should take into account the likelihood of exposure to HIV, the potential benefits and risks of such therapy, and the interval between the exposure and initiation of therapy. Timely determination of the HIV-infection status of the assailant is not possible in many sexual assaults. Therefore, the health-care provider should assess the local epidemiology of HIV/AIDS, the nature of the assault, and any available information about HIV-risk behaviors exhibited by the assailant(s) (e.g., high-risk sexual practices and injection-drug or crack cocaine use). When an assailant's HIV status is unknown, factors that should be considered in determining whether an increased risk of HIV transmission exists include a) whether oral, vaginal, or anal penetration occurred; b) whether ejaculation occurred on mucous membranes; c) whether multiple assailants were involved; d) whether mucosal lesions are present in assailant or survivor; and e) other characteristics of the assault, survivor, or assailant. If antiretroviral postexposure prophylaxis is offered, the following information should be discussed with the patient: a) the unknown efficacy and known toxicities of antiretrovirals; b) the close follow-up that is necessary; c) the importance of strict compliance with the recommended therapy; and d) the necessity of immediate initiation of treatment for maximal likelihood of effectiveness (as soon as possible after, and up to 72 hours following, the most recent assault). Providers should emphasize that although data are limited, postexposure antiretroviral therapy appears to be well tolerated in both adults and children, and severe adverse effects are rare. Personnel likely to examine survivors of sexual assault should consult with federal or state health departments or other professionals knowledgeable in STDs to develop algorithms and protocols for the determination of risk for exposure to HIV and management in their community. Clinical management of the patient should be implemented according to the following guidelines (107,108). If postexposure HIV prophylaxis is being considered, consultation with an HIV specialist is recommended. Recommendations for Postexposure Assessment of Adolescent and Adult Survivors within 72 hours of Sexual Assault§§§
Sexual Assault or Abuse of ChildrenRecommendations in this report are limited to the identification and treatment of STDs. Management of the psychosocial aspects of the sexual assault or abuse of children is beyond the scope of these recommendations. The identification of sexually transmissible agents in children beyond the neonatal period suggests sexual abuse. The significance of the identification of a sexually transmitted agent in such children as evidence of possible child sexual abuse varies by pathogen. Postnatally acquired gonorrhea; syphilis; and non-transfusion, non-perinatally acquired HIV are usually diagnostic of sexual abuse. Sexual abuse should be suspected in the presence of genital herpes. The investigation of sexual abuse among children who possibly have a sexually transmitted infection should be conducted in compliance with recommendations by clinicians who have experience and training in all elements of the evaluation of child abuse, neglect, and assault (109--111). The social significance of each sexually transmitted infection and the recommended action regarding reporting of suspected child sexual abuse varies by STD (Table 5). In all cases in which a sexually transmitted infection has been diagnosed in a child, efforts should be made to detect evidence of sexual abuse, including conducting diagnostic testing for other commonly occurring sexually transmitted infections (109,110). The general rule that sexually transmissible infections beyond the neonatal period are evidence of sexual abuse has exceptions. For example, rectal or genital infection with C. trachomatis among young children may be the result of perinatally acquired infection and has, in some cases, persisted for as long as 2--3 years. Genital warts have been diagnosed in children who have been sexually abused, but also in children who have no other evidence of sexual abuse. BV has been diagnosed in children who have been abused, but its presence alone does not prove sexual abuse. Most HBV infections in children result from household exposure to persons who have chronic HBV infection. The possibility of sexual abuse should be strongly considered if no conclusive explanation for non-sexual transmission of a sexually transmitted infection can be identified. When the only evidence of sexual abuse is the isolation of an organism or the detection of antibodies to a sexually transmissible agent, findings should be confirmed and the implications considered carefully. Evaluation for Sexually Transmitted Infections Examinations of children for sexual assault or abuse should be conducted so as to minimize pain and trauma to the child. Collection of vaginal specimens in prepubertal children can be very uncomfortable and should be performed by an experienced clinician to avoid psychological and physical trauma to the child. The decision to obtain genital or other specimens from a child to conduct an STD evaluation must be made on an individual basis. The following situations involve a high risk for STDs and constitute a strong indication for testing.
If a child has symptoms, signs, or evidence of an infection that might be sexually transmitted, the child should be tested for other common STDs before the initiation of any treatment that could interfere with the diagnosis of those other STDs. Because of the legal and psychosocial consequences of a false-positive diagnosis, only tests with high specificities should be used. The potential social benefit to the child of a reliable diagnosis of an STD justifies deferring presumptive treatment until specimens for highly specific tests are obtained by providers with experience in the evaluation of sexually abused and assaulted children. The scheduling of examination should depend on the history of assault or abuse. If the initial exposure was recent, the infectious agents acquired through the exposure may not have produced sufficient concentrations of organisms to result in positive test results. A follow-up visit approximately 2 weeks after the most recent sexual exposure may include a repeat physical examination and collection of additional specimens. To allow sufficient time for antibodies to develop, another follow-up visit approximately 12 weeks after most recent sexual exposure may be necessary to collect sera. A single examination may be sufficient if the child was abused for an extended time period and if the last suspected episode of abuse occurred well before the child received medical evaluation. The following recommendations for scheduling examinations serve as a general guide. The exact timing and nature of follow-up examinations should be determined on an individual basis and should be performed so as to minimize the possibility for psychological trauma and social stigma. Compliance with follow-up appointments might be improved when law enforcement personnel or child protective services are involved. Initial and 2-Week Follow-Up Examinations During the initial examination and 2-week follow-up examination (if indicated), the following should be performed.
HIV infection has been reported in children whose only known risk factor was sexual abuse. Serologic testing for HIV infection should be considered for abused children. The decision to test for HIV infection should be made on a case-by-case basis, depending on the likelihood of infection among assailant(s). Data are insufficient concerning the efficacy and safety of postexposure prophylaxis among both children and adults. However, antiretroviral treatment is well tolerated by infants and children with and without HIV infection; in addition, children who receive such treatment have a minimal risk for serious adverse reactions because of the short period of time recommended for prophylaxis (30,114). In those cases in which a child presents to a health-care provider shortly after a sexual exposure (i.e., within 72 hours), the assailant(s) are likely to be at risk for HIV infection, and likelihood of compliance with treatment regimens is high, the potential benefit of treating a sexually abused child should be weighed against the risk for adverse reactions. If antiretroviral postexposure prophylaxis is being considered, a professional specializing in HIV-infected children should be consulted. Recommendations for Postexposure Assessment of Children within 72 Hours of Sexual Assault
Examination 12 Weeks After Assault In circumstances in which transmission of syphilis, HIV, or hepatitis B is a concern but baseline tests are negative, an examination approximately 12 weeks after the last suspected sexual exposure is recommended to allow time for antibodies to infectious agents to develop. The prevalence of these infections differs substantially by community. In addition, results of HBsAg testing must be interpreted carefully, because HBV can be transmitted non-sexually. Decisions regarding which tests should be performed must be made on an individual basis. Presumptive Treatment The risk of a child acquiring an STD as a result of sexual abuse or assault has not been determined. Presumptive treatment for children who have been sexually assaulted or abused is not recommended because a) the prevalence of most STDs is low following abuse/assault, b) pre-pubertal girls appear to be at lower risk for ascending infection than adolescent or adult women, and c) regular follow-up of children usually can be ensured. However, some children or their parent(s) or guardian(s) may be concerned about the possibility of infection with an STD, even if the risk is perceived to be low by the health-care provider. Such concerns may be an appropriate indication for presumptive treatment in some settings and may be considered after all specimens for diagnostic tests relevant to the investigation have been collected. Reporting Every state and U.S. territory has laws that require the reporting of child abuse. Although the exact requirements differ by state, if a health-care provider has reasonable cause to suspect child abuse, a report must be made. Health-care providers should contact their state or local child-protection service agency about child-abuse reporting requirements in their areas. References
* The absence of a fourfold or greater titer for an infant does not exclude congenital syphilis. † CSF test results obtained during the neonatal period can be difficult to interpret; normal values differ by gestational age and are higher in preterm infants. Values as high as 25 white blood cells (WBCs)/mm3 and/or protein of 150 mg/dL might occur among normal neonates; some specialists, however, recommend that lower values (i.e., 5 WBCs/mm3 and protein of 40 mg/dL) be considered the upper limits of normal. Other causes of elevated values also should be considered when an infant is being evaluated for congenital syphilis. § A woman treated with a regimen other than those recommended in these guidelines for treatment should be considered untreated. ¶ If the infant's nontreponemal test is nonreactive and the likelihood of the infant being infected is low, some specialists recommend no evaluation but treatment of the infant with a single IM dose of benzathine penicillin G 50,000 units/kg for possible incubating syphilis, after which the infant should receive close serologic follow-up. ** Some specialists would not treat the infant but would provide close serologic follow-up. †† An association between oral erythromycin and infantile hypertrophic pyloric stenosis (IHPS) has been reported in infants aged <6 weeks who were treated with this drug. Infants treated with erythromycin should be followed for signs and symptoms of IHPS. Data on use of other macrolides (e.g., azithromycin and clarithromycin) for the treatment of neonatal chlamydia infection are limited. The results of one study involving a limited number of patients suggests that a short course of azithromycin, 20 mg/kg/day orally, one dose daily for 3 days, may be effective. §§ Quinolones should not be used for infections acquired in Asia or the Pacific, including Hawaii. In addition, use of quinolones is probably inadvisable for treating infections acquired in California and in other areas with increased prevalence of quinolone resistance. ¶¶ The availability of silver nitrate in the United States may be limited. *** Over-the-counter (OTC) preparations. ††† The Bethesda System for Reporting Cervical/Vaginal Cytologic Diagnoses uses the terms "low-grade SIL" and "high-grade SIL" (95). Low-grade SIL encompasses cellular changes associated with HPV and mild dysplasia/cervical intraepithelial neoplasia 1 (CIN1). High-grade SIL includes moderate dysplasia/CIN2, severe dysplasia/CIN3, and carcinoma in situ/CIN3. §§§ Assistance with postexposure prophylaxis decisions can be obtained by calling the National HIV Telephone Consultation Service (tel: 800-933-3413). Table 1 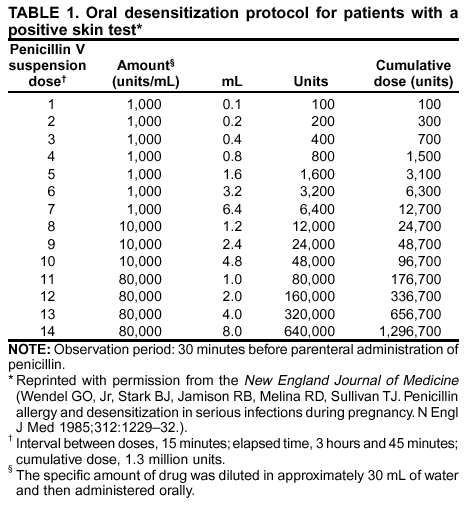 Return to top. Box 1 Box 1. Skin-test reagents for identifying persons at risk for adverse reactions to penicillin*
Return to top.
Box 2
Return to top.
Abbreviations Used in This Publication
ConsultantsChairpersons: David Atkins, M.D., M.P.H., Agency for Healthcare Research and Quality, Rockville, MD; Kimberly A. Workowski, M.D., Division of STD Prevention, CDC and Emory University, Atlanta, GA. Presenters: Adaora A. Adimora, M.D., M.P.H., University of North Carolina, Chapel Hill, NC; Michael H. Augenbraun, M.D., State University of New York (SUNY) Health Science Center, Brooklyn, NY; Willard Cates, Jr., M.D., M.P.H., Family Health International, Research Triangle Park, NC; Jane Cecil, M.D., Johns Hopkins, Baltimore, MD; Lynne Fukumoto, UCLA School of Nursing, Los Angeles, CA; Margaret Hammerschlag, M.D., SUNY Health Science Center, Brooklyn, NY; Anne M. Rompalo, M.D., Johns Hopkins University, Baltimore, MD; Richard Rothenberg, M.D., Emory University School of Medicine, Atlanta, GA; Pablo J. Sanchez, M.D., University of Texas Southwestern Medical Center, Dallas, TX; Bradley Stoner, M.D., Ph.D., Washington University School of Medicine, St. Louis, MO; Jane R. Schwebke, M.D., Department of Medicine, University of Alabama, Birmingham, AL; Anna Wald, M.D., M.P.H., University of Washington, Seattle, WA; Cheryl K. Walker, M.D., Stanford University Medical Center, Stanford, CA; George D. Wendel, M.D., University of Texas Southwestern Medical Center, Dallas, TX; Karen Wendel, M.D., Johns Hopkins University, Baltimore, MD; Dorothy J. Wiley, Ph.D., UCLA School of Nursing, Los Angeles, CA; Jonathan M. Zenilman, M.D., Johns Hopkins University, Baltimore, MD. Moderators: King K. Holmes, M.D., Ph.D., Center for AIDS and STDs, University of Washington, Seattle, WA; Edward W. Hook, III, M.D., University of Alabama, School of Medicine, Birmingham, AL; William McCormack, M.D., SUNY Health Science Center, Brooklyn, NY. Rapporteurs: John M. Douglas, Jr., M.D., Denver Department of Public Health and University of Colorado Health Science Center, Denver, CO; H. Hunter Handsfield, M.D., University of Washington and Public Health-Seattle & King County, Seattle, WA; Walter Stamm, M.D., University of Washington Medical Center, Seattle, WA. Consultants: Gail Bolan, M.D., California Dept. of Health, Berkeley, CA; Toye H. Brewer, M.D., University of Miami, Miami, FL; Virginia A. Caine, M.D., Indiana University School of Medicine, Indianapolis, MN; Connie Celum, M.D., M.P.H., University of Washington, Seattle, WA; Myron S. Cohen, M.D., University of North Carolina, Chapel Hill, NC; Thomas A. Farley, M.D., M.P.H., Tulane University School of Public Health and Tropical Medicine, New Orleans, LA; Laura T. Gutman, M.D., Duke University, Durham, NC; Penelope J. Hitchcock, D.V.M., M.S., National Institute for Allergy and Infectious Diseases, NIH, Bethesda, MD; Sharon Hillier, Ph.D, Magee Women’s Hospital, Pittsburgh, PA; Franklyn N. Judson, M.D., Denver Department of Health, Denver, CO; David Martin, M.D., LSU Medical Center, New Orleans, LA; Daniel M. Musher, M.D., Veterans Affairs Medical Center, Houston, TX; Newton G. Osborne, M.D., M.P.H., Howard University Hospital, Washington, DC; Jeff Peipert, M.D., M.P.H., Women and Infants Hospital, Providence, RI; Peter Rice, M.D., Boston Medical Center, Boston, MA; Mary Sawyer, M.D., Emory University, Atlanta, GA; Jack Sobel, M.D., Wayne State University, Detroit, MI; David Soper, M.D., Medical University of South Carolina, Charleston, SC; Lawrence R. Stanberry, M.D., Ph.D., University of Texas Medical Branch, Galveston, TX; Barbara Stoll, M.D., Emory University School of Medicine, Atlanta, GA; Richard Sweet, M.D., Magee Women’s Hospital, Pittsburgh, PA; Eugene Washington, M.D., UCSF/Mt. Zion Medical Center, San Francisco, CA; Heather Watts, M.D., National Institutes of Health, Bethesda, MD. Liaison Participants: Vagan A. Akovbian, M.D., Ph.D., Russian Ministry of Health Central Institute, Moscow, Russia; Gale Burstein, M.D., M.P.H, American Academy of Pediatrics; Willa Brown, M.D., M.P.H., American College of Preventative Medicine; Mike Catchpole, M.D., PHLS Communicable Disease Surveillance, England; Tom Cox, M.D., American Social Health Association; William Dumas, R.N., National Coalition of STD Directors; Antonio C. Gerbase, M.D., World Health Organization; Sharon Hillier, Ph.D., Infectious Disease Society of Obstetrics and Gynecology; Louella Klein, M.D., American College of Obstetrics and Gynecology; David J. Magid, M.D., M.P.H, Managed Care Colorado; Rafael Mazin, M.D., Pan American Health Organization; Gregory J. Moran, M.D., American College of Emergency Physicians; Donna Richmond, M.P.H., R.N., Association of Reproductive Health Professionals; Anthony Schaeffer, M.D., American Urological Association; Felicia Stewart, M.D., American Social Health Association; Stephen K. Tyring, M.D., Ph.D., American Academy of Dermatology; Leonard B. Weiner, M.D., American Academy of Pediatrics; Tom Wong, M.D., M.P.H., Health Canada. CDC/Division of STD Prevention (DSTDP)/STD Treatment Guidelines 2002 Project Coordinators: Kimberly A. Workowski, M.D., DSTDP; William C. Levine, M.D., M.Sc., DSTDP. Project Manager: Donald F. Dowda, DSTDP. Co-Moderators: Lyn Finelli, Ph.D., DSTDP; Robert Johnson, M.D., DSTDP; Lauri Markowitz, M.D., DSTDP. Presenters: Consuelo M. Beck-Sague, M.D., Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP); Jonathan E. Kaplan, M.D., DHAP/NCHSTP; Emilia Koumans, M.D., DSTDP; John Moran, M.D., DSTDP; Juliette Morgan, M.D., NCID; George P. Schmid, M.D., M.Sc, DSTDP; Madeline Sutton, M.D., DSTDP; Susan Wang, M.D, MPH, DSTDP; Consultants: Sevgi O. Aral, Ph.D., DSTDP; Stuart M. Berman, M.D., DSTDP; Joanna Buffington, M.D., DVRD/NCID; Carol Ciesielski, M.D., DSTDP; George Counts, M.D., DSTDP; Julia Schillinger, M.D., M.Sc., DSTDP; Katherine Stone, M.D., DSTDP; Judith N. Wasserheit, M.D., M.P.H., DSTDP; Support Staff: Valerie Barner, DSTDP; Garrett K. Mallory, DSTDP; Deborah McElroy, DSTDP; Porsha Williams, Contractor.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 5/3/2002 |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
This page last reviewed 5/3/2002
|