 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Cigarette Smoking Among Adults --- United States, 2003One of the national health objectives for 2010 is to reduce the prevalence of cigarette smoking among adults to 12% (objective 27-1a) (1). To assess progress toward this objective, CDC analyzed self-reported data from the 2003 National Health Interview Survey (NHIS). The results of that analysis indicated that, in 2003, approximately 21.6% of U.S. adults were current smokers. Although this prevalence is lower than the 22.5% prevalence among U.S. adults in 2002 and significantly lower than the 22.8% prevalence in 2001, the rate of decline is not sufficient to meet the national health objective for 2010 (2). Comprehensive, sustained interventions that reduce the rate of smoking initiation and increase the rate of cessation are needed to further the decline in cigarette smoking among adults (3). Questions on smoking in the 2003 NHIS were included in the adult core questionnaire, which was administered by in-person interview to a nationally representative sample of 30,852 persons aged >18 years in the civilian, noninstitutionalized U.S. population; survey response rate for adults was 74.2%. Respondents were asked, "Have you smoked at least 100 cigarettes in your entire life?" and "Do you now smoke cigarettes every day, some days, or not at all?" Ever smokers were defined as those who reported smoking >100 cigarettes during their lifetimes. Current smokers were defined as those who reported smoking >100 cigarettes during their lifetimes and currently smoking every day or some days. Former smokers were defined as ever smokers who no longer smoked. Poverty-level status was calculated on the basis of U.S. Census Bureau 2002 poverty thresholds. Data were adjusted for nonrespondents and weighted to provide national estimates of cigarette smoking prevalence; 95% confidence intervals (CIs) were calculated to account for the multistage probability sample design. In 2003, an estimated 21.6% (45.4 million) of U.S. adults were current smokers; of these, 81.0% (36.8 million) smoked every day, and 19.0% (8.6 million) smoked some days. Among those who currently smoked every day, 41.1% (15.1 million) reported they had stopped smoking for at least 1 day during the preceding 12 months because they were trying to quit. Among the estimated 43.4% (91.5 million) of persons who had ever smoked, 50.3% (45.9 million) were former smokers. Prevalence of current cigarette smoking varied substantially across populations and subpopulations (Table). More men (24.1%) than women (19.2%) reported current smoking. Among racial/ethnic populations, Asians (11.7%) and Hispanics (16.4%) had the lowest prevalence, and American Indians/Alaska Natives had the highest prevalence (39.7%). By education level, smoking prevalence was highest among adults who had earned a General Educational Development diploma (44.4%) and lowest among those with graduate degrees (7.5%). Among age groups, persons aged >65 years had the lowest prevalence of cigarette smoking (9.1%), and persons aged 25--44 years had the highest prevalence (25.6%). Current smoking prevalence was higher among adults living below the poverty level (30.5%) than among those at or above the poverty level (21.7%). Persons in certain subpopulations had cigarette smoking prevalence rates below the 2010 health objective target of 12%. These subpopulations included women with undergraduate (11.0%) or graduate degrees (6.7%), men with graduate degrees (8.1%), Hispanic women (10.3%), Asian women (6.5%), and men and women aged >65 years (10.1% and 8.3%, respectively) (Table). During 1983--2003, a sustained decline in cigarette smoking occurred in all age groups except persons aged 18--24 years (Figure). In this group, prevalence increased during 1993--2002, before declining significantly from 28.5% in 2002 to 23.9% in 2003, the lowest reported prevalence for persons aged 18--24 years since 1991 (4). Reported by: A Trosclair, MS, R Caraballo, PhD, A Malarcher, MD, C Husten, MD, T Pechacek, PhD, Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Editorial Note:The findings in this report indicate that cigarette smoking continues to decline among adults in the United States. In 2003, for the first time since NHIS began collecting smoking data in 1965, the prevalence of cigarette smoking among women declined below 20%, to 19.2%. For the second consecutive year, more than half of U.S. adults who ever smoked reported they were no longer smokers. In addition, cigarette smoking among persons aged 18--24 years declined to the lowest level since 1991. The increase in smoking prevalence among young adults during 1991--2002 was similar to an increase in smoking among youths in 8th, 10th, and 12th grades during the early 1990s (5). Factors associated with the increase in smoking among adolescents (e.g., increased tobacco industry marketing to youths) might have had a similar influence on smoking prevalence among young adults (6). A cohort effect might also have contributed to the increase in smoking prevalence among young adults, as youths with high rates of smoking during the early 1990s entered the young adult age group during 1992--2002 (5--7). Although tobacco use usually begins during adolescence, initiation also can occur during young adulthood (6,7). Preventing smoking initiation and tobacco use among youths and young adults is critical to reducing tobacco use in the United States. Young adults, who constitute the youngest legal market for the tobacco industry in the United States, and adolescents continue to be the target of intensive tobacco industry marketing efforts, including sponsorship of age-specific promotions and other marketing strategies that appeal to persons in these age groups (7,8). Efforts to reduce cigarette smoking prevalence among all adults include increasing the retail price of tobacco products and implementing complete smoking bans in all worksites, campuses, sports arenas, concert venues, bars, restaurants, and nightclubs. Strategies for reducing cigarette smoking prevalence among young adults include 1) providing effective smoking-cessation interventions and quitlines tailored to youths and young adults in school, work, and community settings; 2) conducting countermarketing campaigns designed to help young persons reject messages promoting cigarette use, reduce access by minors to tobacco products, and increase access to school programs for preventing tobacco use; and 3) monitoring smoking trends among youths and young adults (6--10). Ongoing surveillance of smoking patterns among young adults and evaluation of tobacco-control programs can identify those interventions that are most effective for this age group. The findings in this report are subject to at least four limitations. First, the wording of questions about cigarette smoking and NHIS data collection procedures have changed since 1993. Before 1993, current smokers were defined as those who had smoked at least 100 cigarettes and currently smoked. Starting in 1993, current smokers were defined as those who had smoked at least 100 cigarettes and currently smoked either every day or some days. Therefore, any comparison of data collected before 1993 with data collected since 1993 should be interpreted with caution. Second, many young adults view themselves as "social smokers" and might not identify themselves as smokers even on "some days" when completing the NHIS questionnaire, leading to underestimates of current smoking. Third, the NHIS questionnaire is administered only in English and Spanish, which might lead to imprecise estimates of smoking prevalence among other racial/ethnic populations who are unable to respond to the survey. Finally, because NHIS sample sizes for some subpopulations are minimal (e.g., Asians and American Indians/Alaska Natives), estimates derived from 1 year of data are less precise for these groups. Effective interventions for tobacco-use prevention and cessation should be implemented in the United States among persons of all ages to accelerate the decline in smoking prevalence among adults and decrease the public health burden of tobacco-related diseases (3,6--10). In addition, tailored interventions for populations and subpopulations at high risk are needed to reduce disparities in cigarette smoking by age, race/ethnicity, and education level. References
Table 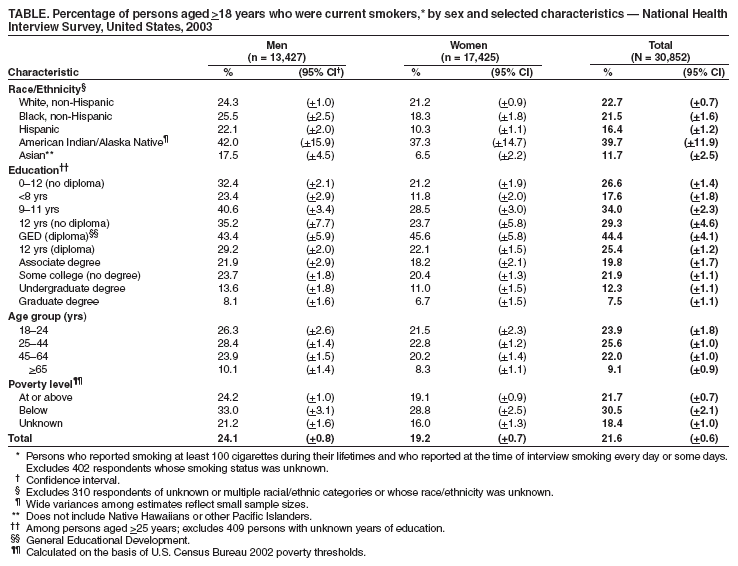 Return to top. Figure 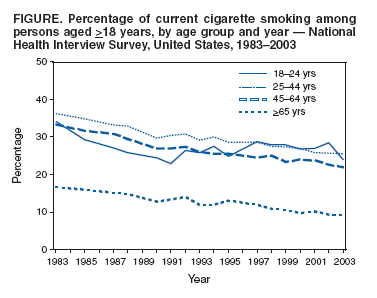 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Date last reviewed: 5/26/2005 |
|||||||||
|