Preterm Birth

Preterm birth is when a baby is born too early, before 37 weeks of pregnancy have been completed. In 2022, preterm birth affected about 1 of every 10 infants born in the United States (see Births in the United States, 2022). The preterm birth rate declined 1% in 2022 to 10.4%, following an increase of 4% from 2020 to 2021. However, racial and ethnic differences in preterm birth rates remain. In 2022, the rate of preterm birth among African-American women (14.6%) was about 50 percent higher than the rate of preterm birth among white or Hispanic women (9.4% and 10.1% respectively).
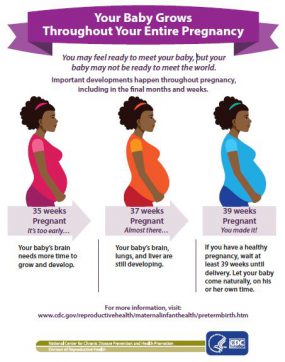
A developing baby goes through important growth throughout pregnancy─ including in the final months and weeks. For example, the brain, lungs, and liver need the final weeks of pregnancy to fully develop. Read Your Baby Grows Throughout Your Entire Pregnancy [PDF-312KB]. Babies born too early (especially before 32 weeks) have higher rates of death and disability. In 2021, preterm birth and low birth weight accounted for about 14.8% of infant deaths (deaths before 1 year of age). Babies who survive may have
- Breathing problems
- Feeding difficulties
- Cerebral palsy
- Developmental delay
- Vision problems
- Hearing problems
Preterm births may also take an emotional toll and be a financial burden for families.
Frequently Asked Questions: For Women and Their Families
CDC’s Division of Reproductive Health is engaged in a variety of activities to reduce preterm delivery and complications. CDC recently expanded support to 36 perinatal quality collaboratives (PQCs), which are state or multi-state networks of teams of healthcare providers and public health professionals working to improve the quality of care for mothers and babies. Funding supports the capabilities of PQCs to improve the quality of perinatal care in their states, including efforts to reduce preterm birth.
- Percentage of Births Born Preterm by State from CDC
- Birth Data (including preterm birth rates) from CDC
- Premature Babies – Information about health problems among and care of premature babies from the March of Dimes.