Data and Statistics on Zika and Pregnancy
Since the Zika virus outbreak in the Americas began in 2015, CDC scientists and clinicians have collaborated to understand the effects of Zika virus infection on the mother and developing baby during pregnancy. There is still much to learn about Zika virus, and CDC continues to study the effects of Zika virus infections to learn how to protect pregnant people and their babies.
Proportion with Birth Defects is about 5%
Among people with confirmed or possible Zika virus infection during pregnancy in U.S. states and territories, Zika-associated birth defects occurred in about 5% of babies.1


Several Individual Brain and Eye Defects more Commonly Reported1
- The brain and eye defects most frequently reported include:
- Microcephaly (smaller than expected head size),
- corpus callosum abnormalities (problems with the area of the brain that connects the two sides/hemispheres),
- intracranial calcification,
- abnormal cortical gyral patterns,
- ventriculomegaly (fluid spaces in the brain are larger than normal),
- cerebral/cortical atrophy,
- chorioretinal abnormalities (damage to the back of the eye), and
- optic nerve abnormalities.
Among pregnancies with confirmed Zika virus infection, Zika-associated birth defects were reported with exposures throughout pregnancy but were more prevalent among infants born to mothers with exposure early in pregnancy.1
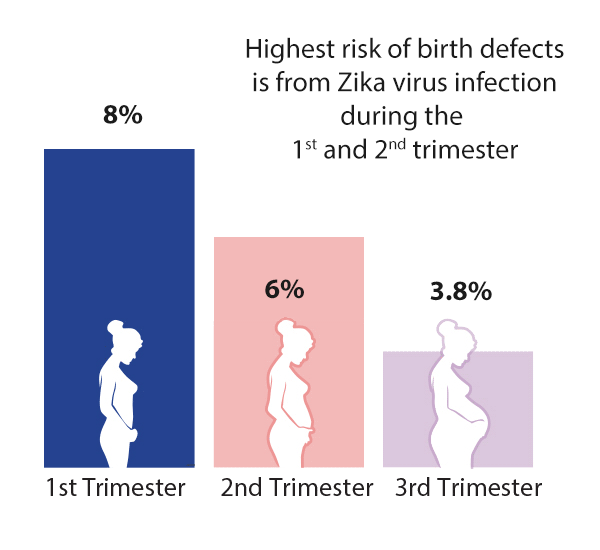
- In U.S. states and territories, about 2 in 25 (8%) pregnant people with confirmed Zika virus infection in the 1st trimester had babies with Zika-associated birth defects.1
The proportion of babies affected by birth defects was similar for people with Zika virus infection during pregnancy who experienced symptoms (e.g. fever, rash, joint pain, or conjunctivitis) compared to those who did not experience symptoms.1
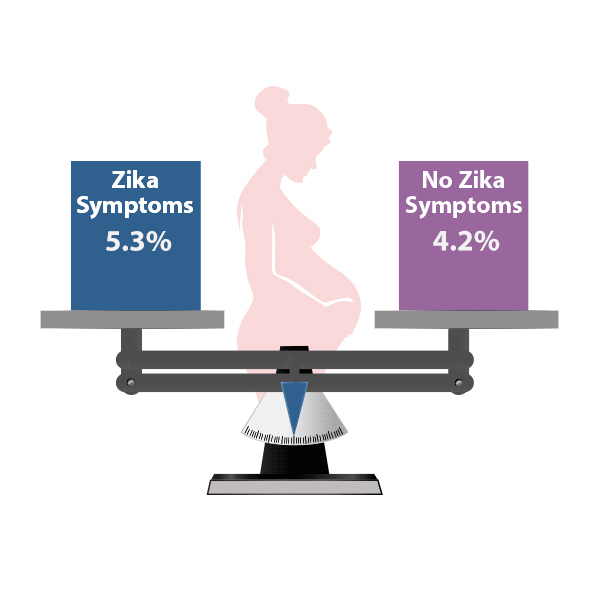
- In the U.S. states and territories, about 1 in 20 (5.3%), people with symptoms of Zika virus infection during pregnancy had a baby with Zika-associated birth defects, compared with about 1 in 25 (4.2%) people without symptoms of Zika virus infection during pregnancy.
Babies Exposed to Zika Before Birth Might Have Long-Term Health Problems
Some babies with possible Zika infection during pregnancy might look healthy at birth but can develop long-term health problems as they grow. Careful monitoring and evaluation of children born to mothers with evidence of possible Zika virus infection during pregnancy is essential to ensure babies receive the care they need.
In the August 2018 Vital Signs Report, scientists looked at babies who were at least 1 year old born to people with Zika during pregnancy in the U.S. territories. Out of 1,450 babies, approximately 1 in 7 (or 14%) had one or more reported health problems possibly caused by Zika.

Increase in Birth Defects in Areas with Widespread Local Zika Transmission
The peak of the Zika virus outbreak in areas with widespread local transmission occurred in August 2016.
Six months later, in February 2017, areas with widespread local transmission saw a peak in the number of birth defects linked to Zika virus infection.
States can use this information to plan for referral services and follow-up care for affected infants.

Scientists compared the number of population-level birth defects potentially linked to Zika virus infection from January-March 2017 to January-March 2016

They found a 4x increase in associated birth defects in areas with widespread local transmission of Zika virus3

Birth defects potentially linked to Zika virus infection include:
-
Brain abnormalities and/or microcephaly
-
Eye abnormalities

The highest number of birth defects occurred 6 months after the peak of the Zika virus outbreak
References
- Roth NM, Reynolds MR, Lewis EL, et al. Zika-associated Birth Defects Reported in Pregnancies with Laboratory Evidence of Confirmed or Possible Zika Virus Infection — U.S. Zika Pregnancy and Infant Registry, December 1, 2015–March 31, 2018. MMWR Morb Mortal Wkly Rep 2022;71:73–79. DOI: http://dx.doi.org/10.15585/mmwr.mm7103a1external icon.
- Rice ME, Galang RR, Roth NM, et al. Vital Signs:Zika-Associated Birth Defects and Neurodevelopmental Abnormalities Possibly Associated with Congenital Zika Virus Infection — U.S. Territories and Freely Associated States, 2018. MMWR Morb Mortal Wkly Rep.2018;67:858-867. DOI: http://dx.doi.org/10.15585/mmwr.mm6731e1external iconexternal icon
- Smoots AN, Olson SM, Cragan J, et al. Population-Based Surveillance for Birth Defects Potentially Related to Zika Virus Infection — 22 States and Territories, January 2016–June 2017. MMWR Morb Mortal Wkly Rep 2020;69:67–71. DOI: http://dx.doi.org/10.15585/mmwr.mm6903a3.external icon