New estimates reveal declines in hepatitis C treatment in the U.S. between 2015 and 2020
November 8, 2021 – Far too many remain untreated for curable hepatitis C virus infection
-
- Summary: Far too many remain untreated for curable hepatitis C virus infection
- *Update* Full Report Published February 16, 2022:Characteristics of persons treated for hepatitis c using national pharmacy claims data, United States, 2014-2020external icon
- Graphic
CDC’s first estimates of hepatitis C treatment, presented at the 2021 American Association of the Study of Liver Disease (AASLD) meetingexternal icon, show the number of people living with hepatitis C in the U.S., who initiated treatment with direct-acting antiviral agents (DAA), declined from 2015 to 2020.
The CDC analysis found about 843,000 people initiated treatment with DAAs from 2014 to 2020, with an average of approximately 120,000 people treated each year. This number is far short of national hepatitis C public health goals. In 2015, the National Academies of Science and Medicineexternal icon estimated that at least 260,000 people with hepatitis C should be treated annually to achieve hepatitis C elimination in the U.S. by 2030. Today, this is likely an underestimate of what is needed, given years of under-treatment coupled with the ongoing increases in new hepatitis C infections driven by the nation’s opioid crisis.
CDC estimates about 2.4 million people were living with hepatitis C in the United States during 2013-2016.
New challenges for hepatitis C treatment emerge as other barriers come down
Progress has been made against key barriers to hepatitis C treatment in recent years. Since 2015, many states have removed policy restrictions that prevented people living with hepatitis C from accessing treatment, and the new CDC treatment estimates show from 2014 to 2020, the proportion of claims for hepatitis C DAAs paid for by Medicaid increased by three-fold.
Additionally, the cost of hepatitis C treatment has decreased due to increased competition from drug makers, programs contracting for lower costs, and innovative state treatment models.
Despite these gains, some barriers remain, and new barriers – including the COVID-19 pandemic and opioid crisis – present challenges to closing the hepatitis C testing and treatment gaps.
Barriers to treatment still remain in many state Medicaid policies such as:
- Restrictions on provider-types who can manage treatment
- Patient sobriety requirements which can deter people from seeking life-saving treatment
- Prior authorization processes before treatment can begin
The COVID-19 pandemic has also caused major disruptions in access to hepatitis C testing and treatment services, including:
- Stay-at-home orders that suspended or delayed many routine healthcare visits
- Avoidance of seeking medical and preventative services in a health care setting, particularly in emergency departments and primary care settings where most hep C testing takes place
- Reduced operation of syringe service programs (SSPs) and other healthcare clinics or settings, which could provide hepatitis testing services and linkage to care for people at increased risk of hepatitis C virus infection
The opioid crisis continues to shift the course of the hepatitis C epidemic
Acute hepatitis C infections reported to CDC quadrupled from 2009 to 2019, with injection drug use being the most reported risk factor for hepatitis C among cases reporting risk factors (67 percent in 2019). The rate of new hepatitis C infections has increased the most among younger adults, with injection drug use as the primary route of transmission.
- 20-29 yrs. acute hep C case rate: 0.7 (2009) 2.9 (2019)
- 30-39 yrs. acute hep C case rate 0.5 (2009) 3.2 (2019)
Harm reduction programs and intervention such as syringe services programs and substance use disorder treatment are essential to reduce bloodborne infections, including hepatitis C, among people who inject drugs. Connecting people who inject drugs to hepatitis C testing and treatment services is critical to reducing hepatitis C transmission.
Hepatitis C testing & treatment is critical to saving lives and preventing transmission
Reaching more people with hepatitis C testing and treatment is critical to saving lives and preventing transmission of this deadly, but curable, infection. Hepatitis C treatment can cure more than 90 percent of hepatitis C cases, but testing is a critical first step. It’s estimated 40 percent of people with hepatitis C in the U.S. from 2015-2018 were unaware of their infection.
Since 2020, CDC has recommended hepatitis C screening for all adults once and pregnant persons during every pregnancy, and periodic testing for all people with risk factors.
Graphic:
These high-resolution, public domain images are ready to download and print in your publication. Click on a graphic to see it in high-resolution. These images are in the public domain and are thus free of any copyright restrictions. As a matter of courtesy, we ask that the content provider be credited and notified of any public or private usage of an image.
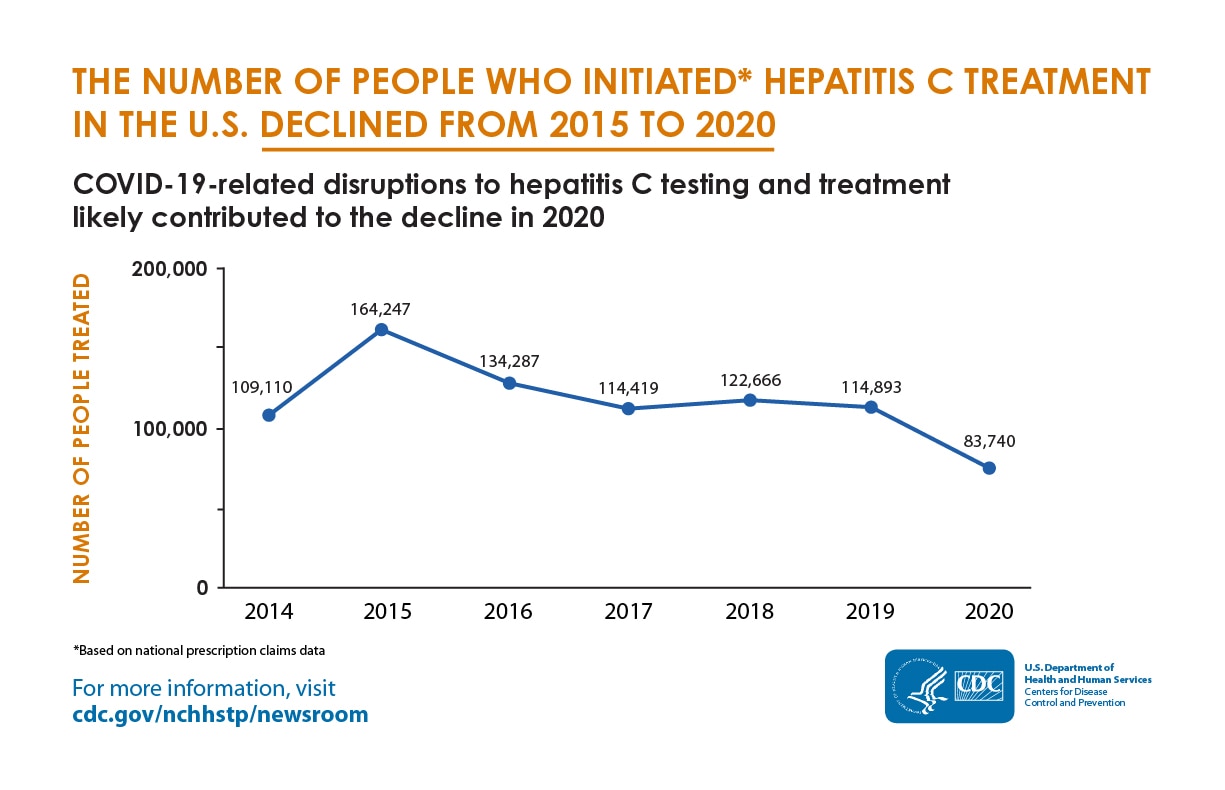
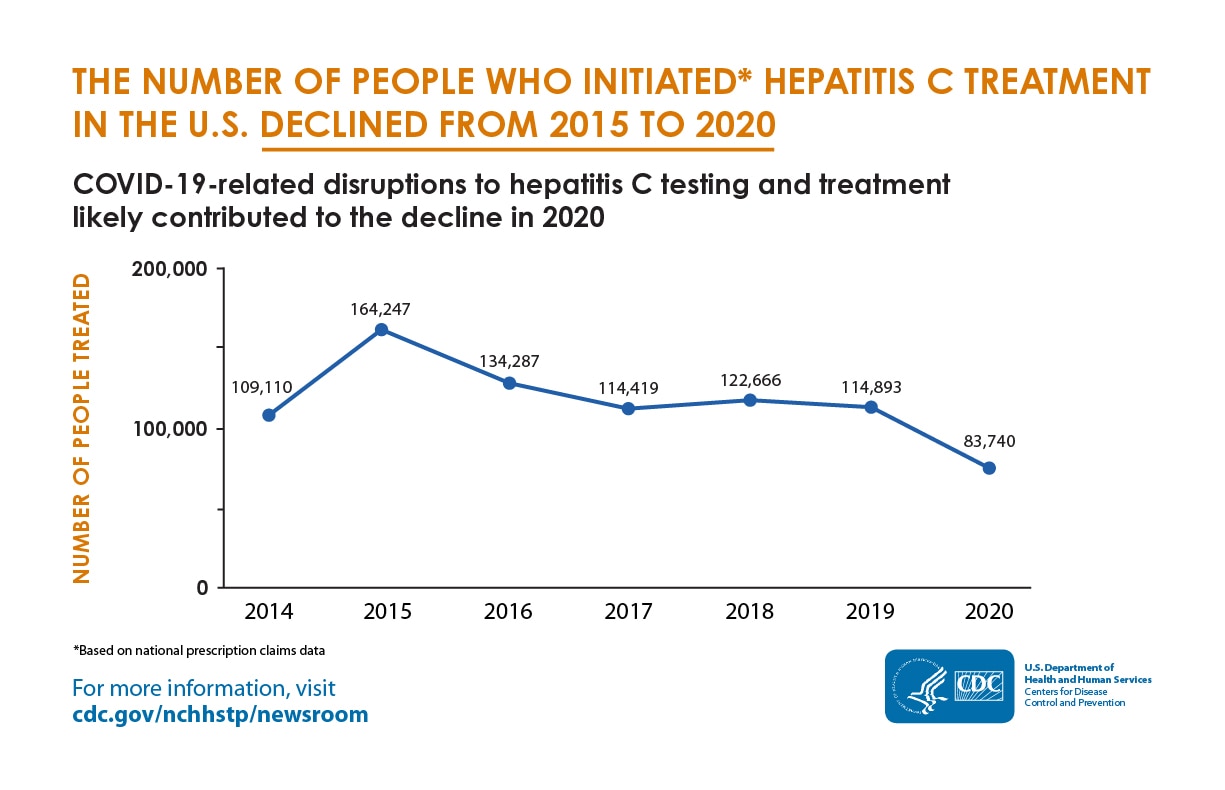
The line chart shows the estimated annual numbers of people treated for hepatitis C in the U.S. from 2014 to 2020. The number is highest in 2015, and lowest in 2020. In 2014, 109,110 people were treated; in 2015, 164,247 people were treated; in 2016, 134,287 people were treated; in 2017, 114,419 people were treated; in 2018, 122,666 people were treated; in 2019, 114,893 people were treated; in 2020, 83,740 people were treated.