Invasive Mold Infections in Immunocompromised People
Physicians: After a flood, keep invasive mold infections in mind when treating people who are sick after exposure to mold.
Background

People, especially those with weakened immune systems, can develop invasive mold infections days to weeks after exposure to fungi that live in the environment. Exposure to indoor mold that grows as a result of water damage may increase this risk.
These infections are:
- Rare
- Typically caused by Aspergillus, but can also be caused by other types of mold, such as mucormycetes
- Difficult to diagnose
- Often life-threatening
Risk Factors
These include people who:
- Have had a transplant, especially hematopoietic stem cell transplants
- Have cancer, especially hematologic cancers like leukemia and lymphoma
- Are undergoing cancer treatment (chemotherapy)
- Are taking medications that weaken the immune system, such as corticosteroids and biologics
Signs and Symptoms
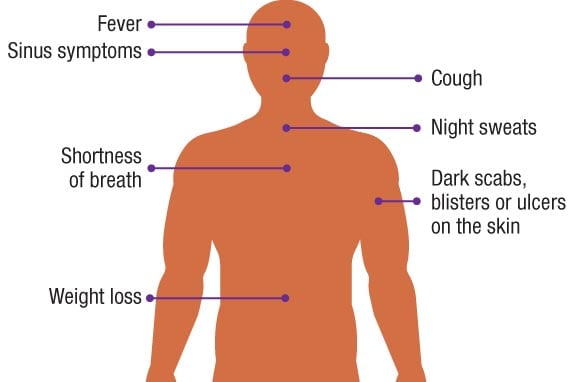
Signs and symptoms can vary depending on the patient, the type of mold, and the part of the body affected, but often include the following:
- Fever
- Cough
- Night sweats
- Weight loss
- Shortness of breath
- Sinus symptoms
- Dark scabs, blisters, or ulcers on the skin
If your patient has any of these symptoms and any of the risk factors described in this factsheet, consider testing for a mold infection.
Diagnosis and Treatment
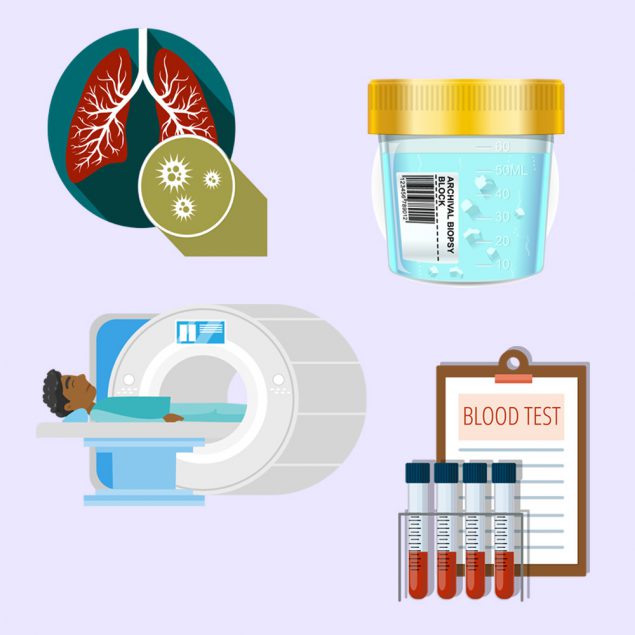
Diagnosing an invasive mold infection requires multiple diagnostic tests. Results of these tests should be interpreted in the context of each specific patient. These tests include:
- Culture of specimens from the affected area (such as bronchoalveolar lavage [BAL]), which is often used to detect lung infections)
- Biopsy of the suspected body part affected to obtain a sample for fungal culture and histopathology
- Imaging of the affected part of the body (e.g., chest computed tomography [CT] for respiratory symptoms)
- Blood tests (such as Aspergillus galactomannan), which are primarily used in immunocompromised patients
Starting treatment early can help prevent deaths. Treatment includes antifungal medications and, in some cases, urgent surgery. Consider consulting an infectious diseases specialist to help with diagnosis and treatment.
Prevention and Patient Resources

After major flooding or other exposure to water damage and mold, talk with your immunocompromised patients about how to protect themselves from mold:
- Mold grows where there is moisture, usually within 24-48 hours of flooding. Even if it is not visible, it is often present.
- Immunocompromised people should not enter moldy buildings or help clean up mold.
- If it is impossible for people with weakened immune systems to avoid a moldy building, they should talk with their doctor and consider wearing an N-95 respirator inside the building. Remind patients that this will still not fully protect them from becoming exposed to mold, but may reduce their risk.
- If there is mold in your patient’s home, someone who is healthy and able should clean it up and fix any water problems.
- Healthy people who clean up mold or spend time in areas affected by mold should wear full protective clothing including an N95 respirator, gloves, boots, long pants and long sleeves. An N95 respirator alone may not fully protect people from becoming exposed to mold and becoming sick.
For more information on mold cleanup, refer patients to the following CDC resources, or provide them with a printed copy:

