COVID-19 Science Update released: November 19, 2021 Edition 114

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 database, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
Evaluation of the BNT162b2 COVID-19 vaccine in children 5 to 11 years of age. Walter et al. NEJM (November 9, 2021).
Key findings:
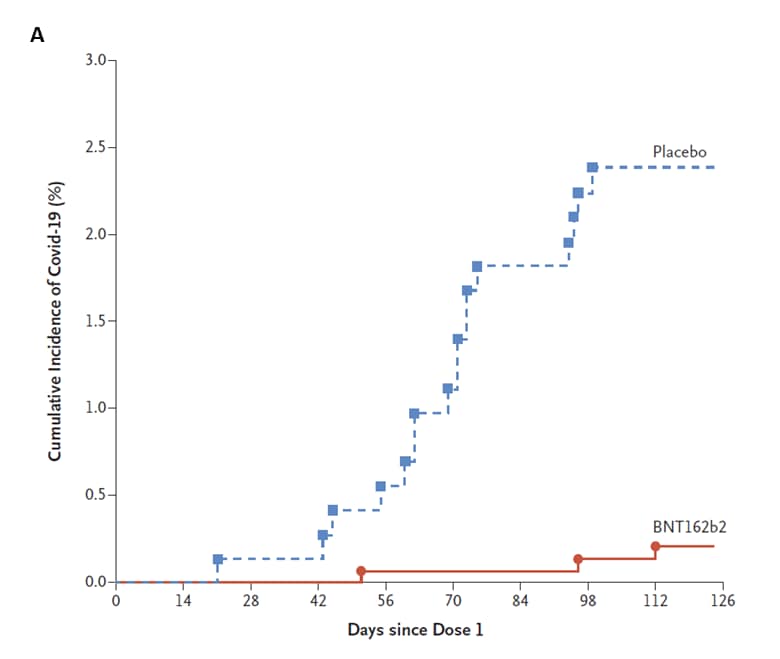
- In children aged 5–11 years, BNT162b2 (Comirnaty, Pfizer/BioNTech) vaccine efficacy for prevention of COVID-19 was 90.7% (95% CI 67.4%-98.3%) (Figure).
- SARS-CoV-2 neutralizing antibody titers 1 month after dose 2 among 5–11-year-olds (10 µg dose) were similar to those among 16–25-year-olds who received 30 µg doses (geometric mean ratio was 1.04, 95% CI 0.93-1.18).
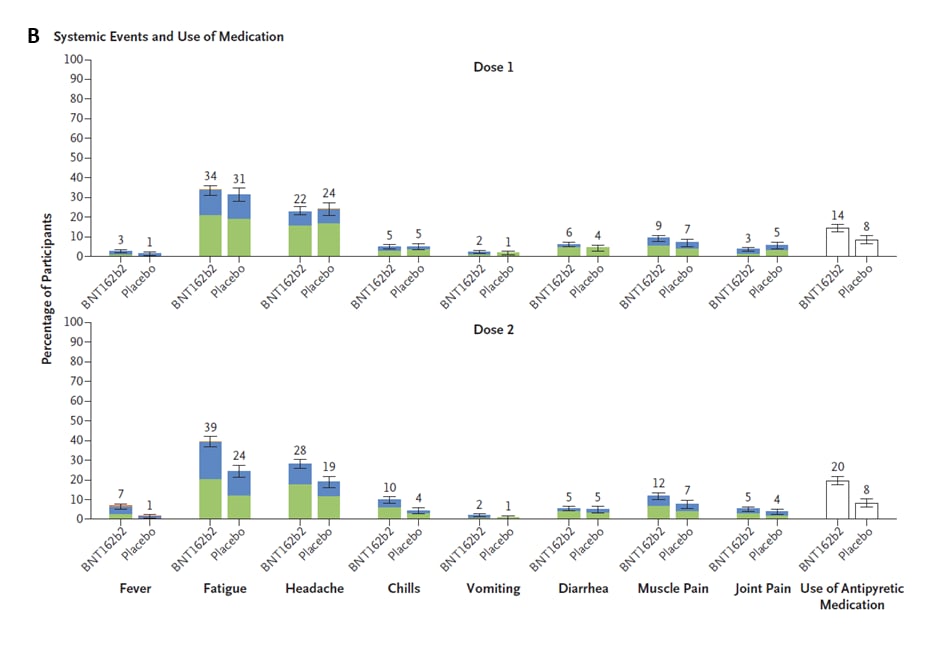
- BNT162b2 10 µg doses had a favorable safety profile among 5–11-year-olds (Figure).
- No serious vaccine-related adverse events were noted.
Methods: Ongoing phase 2–3 safety, immunogenicity, and efficacy trial of BNT162b2 vaccination in healthy children aged 5–11 years. Children were randomly assigned to receive either two 10 µg doses of BNT162b2 21 days apart or placebo; 1,517 received BNT162b2 and 751 received placebo. Vaccine efficacy was assessed ≥7 days after dose 2. Immune responses 1 month after dose 2 were immunologically bridged to those of 16–25-year-old participants from the pivotal trial of 2 BNT162b2 30 µg doses. Limitations: Short duration of follow up (median 2.3 months); study likely under-powered to detect rare adverse events.
Implications: Two 10 µg doses of BNT162b2 vaccine were safe, immunogenic, and efficacious in children 5–11 years of age.
Note: Adapted from Walter et al. Panel A shows the cumulative incidence of the 1st occurrence of COVID-19 after BNT162b2 dose 1 or placebo. Each symbol represents cases of COVID-19 on a given day. Panel B shows systemic events reported within 7 days after vaccine dose 1 (n = 1,511) and dose 2 (n = 1,501) and placebo (dose 1, n = 748 or 749; dose 2, n = 740 or 741 [number of children reporting at least 1 “yes” or “no” for the event after each dose]). Bar colors refer to adverse event severity: mild, moderate, severe, grade 4. Numbers above bars are percentage of participants in each group. I bars represent 95% CIs. From the New England Journal of Medicine, Walter et al., Evaluation of the BNT162b2 COVID-19 vaccine in children 5 to 11 years of age. November 9, 2021, online ahead of print. Copyright © 2021 Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
Distinct SARS-CoV-2 antibody reactivity patterns elicited by natural infection and mRNA vaccination. Assis et al. NPJ Vaccines (November 4, 2021).
Key findings:
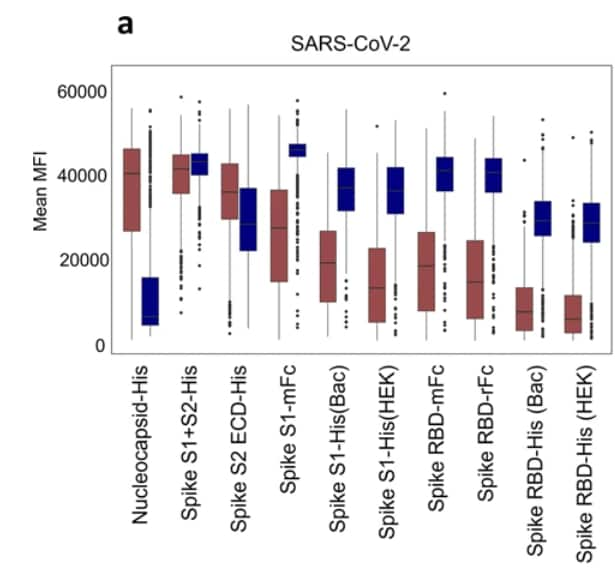
- Specimens from mRNA-vaccinated healthcare workers demonstrated higher antibody levels to the SARS-CoV-2 spike protein S1 and receptor binding domains (RBD) than specimens from a community sample of unvaccinated seropositive persons (Figure).
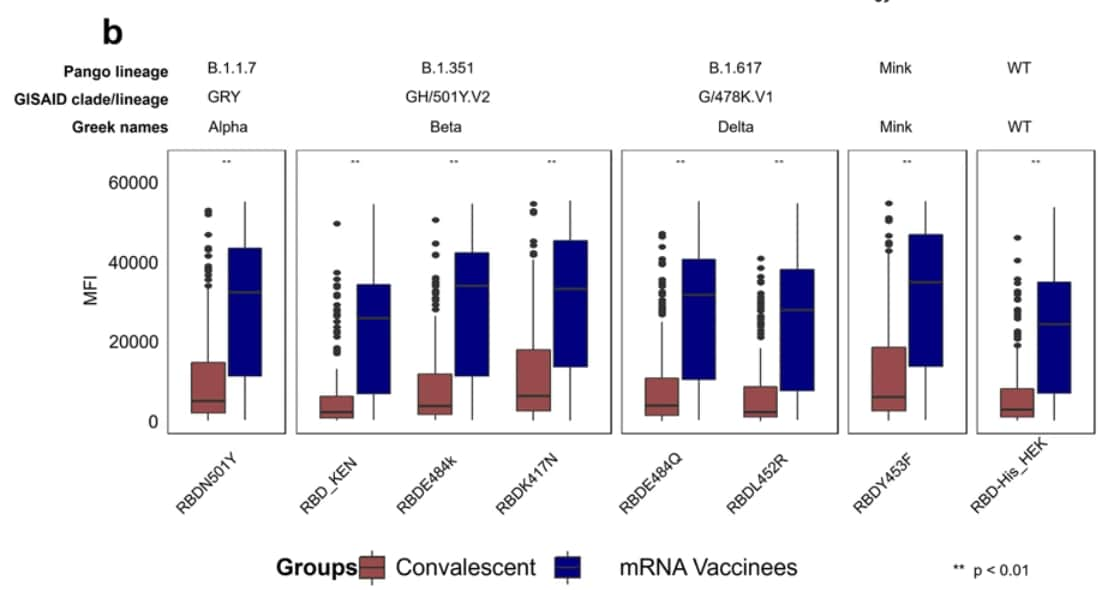
- When exposed to RBD domains from the Alpha (B.1.1.7), Beta (B.1.351), Delta (B.1.617.2), and wild-type lineages, higher anti-RBD antibody titers were observed in plasma from vaccinated persons than in plasma from people who recovered from confirmed COVID-19 (Figure).
- Specimens from mRNA-vaccinated healthcare workers had greater anti-RBD reactivity than specimens from unvaccinated hospitalized COVID-19 patients who required ICU care.
Methods: Samples were obtained from 2 ongoing COVID-19 longitudinal serological surveys of Orange County, CA residents (July and December 2020) and healthcare workers (May and December 2020–March 2021) and a hospital biorepository of samples from 93 hospitalized patients. IgG levels were determined using a multiplex antigen microarray containing antigens from SARS-CoV-2. Limitations: Unclear severity and timing of participants’ infections and timing of vaccination; SARS-CoV-2 exposure may have differed between groups; specimens collected during pre-Delta period.
Implications: mRNA vaccination appears to induce a broader antibody response than SARS-CoV-2 infection.
Figure:
Note: Adapted from Assis et al. Natural exposure (from Santa Ana cohort, December 2020) vs. mRNA vaccination (from February/March 2021 cohort) antibody reactivity against (a) SARS-CoV-2 antigens, and (b) RBD from Alpha, Beta, Delta, and Mink variants, and wild-type (WT) virus. Mean fluorescence intensity (MFI) signals for antibodies are plotted. The boxes represent the 1st quartile, median, and 3rd quartile and the whiskers extend 1.5 times the interquartile range (IQR). Wilcoxon test was performed for pairwise comparisons and p values <0.01 were considered significant and represented as **. Licensed under CC BY 4.0.
PREPRINTS (NOT PEER-REVIEWED)
Three doses of COVID-19 mRNA vaccination are safe based on adverse events reported in electronic health records.Niesen et al. medRxiv (November 9, 2021). Published in JAMA Network Open as Surveillance of safety of 3 doses of COVID-19 mRNA vaccination using electronic health records (April 14, 2022).
Key findings:
- Reports of severe adverse events after a 3rd dose of a COVID-19 mRNA vaccine were rare.
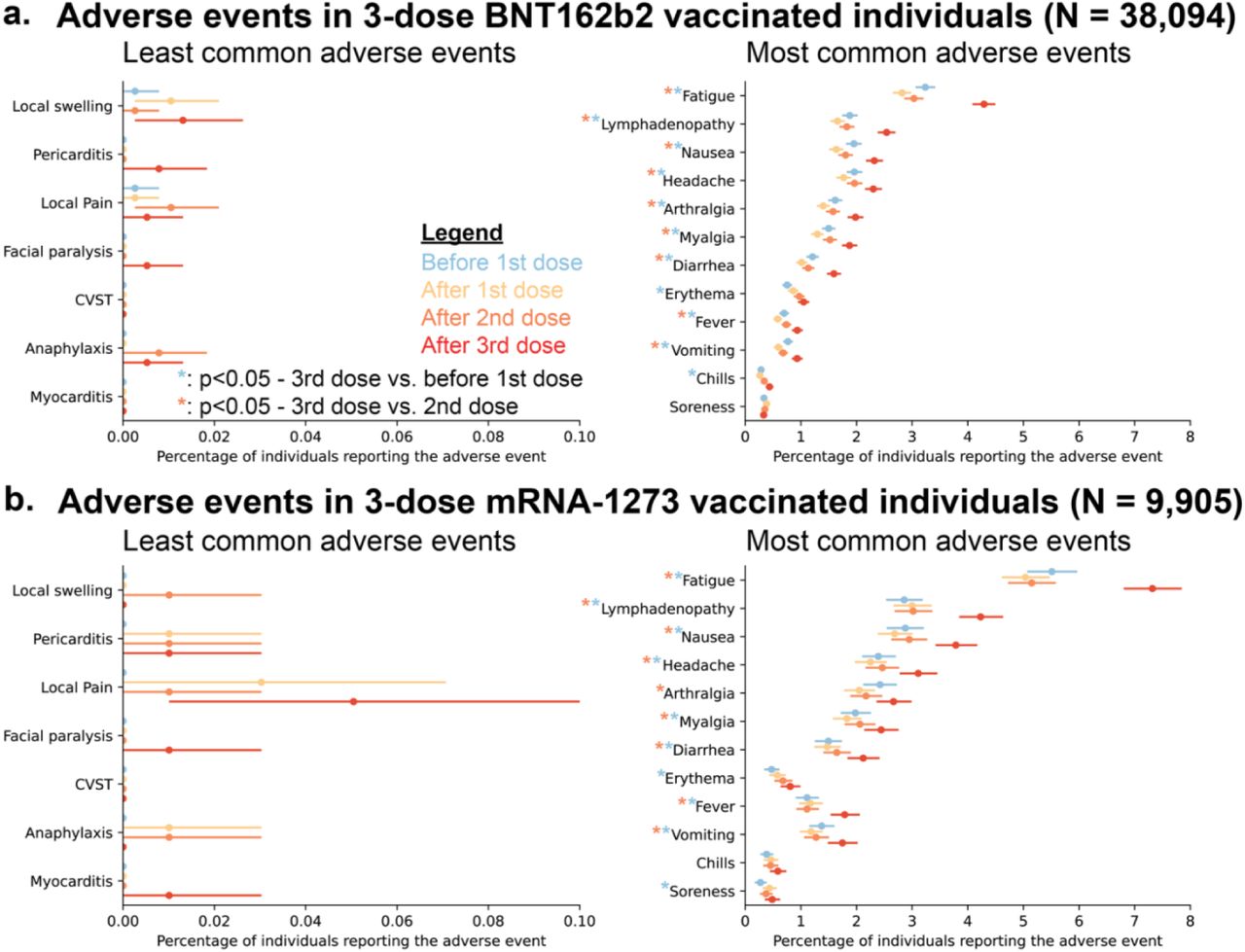
- Pericarditis, anaphylaxis, myocarditis, and cerebral venous sinus thrombosis after dose 3 were reported for ≤0.01% of vaccinated persons (similar to the occurrence after dose 2) (Figure).
- Fatigue, lymphadenopathy, nausea, and headache were reported slightly more often after dose 3 than dose 2 (Figure).
Methods: Retrospective study of patients vaccinated with 3 doses of BNT162b2 (Comirnaty, Pfizer/BioNTech, n = 38,094) or mRNA-1273 (Moderna, n = 9,905), December 1, 2020–October 17, 2021. Electronic health records were used to identify adverse events in the 2 weeks prior to the 1st dose and 2 weeks following the 1st, 2nd, and 3rd doses. Limitations: Limited to signs/symptoms included in electronic health records; persons who experienced post-vaccine adverse events might be less likely to get subsequent doses; results may not be generalizable.
Implications: The risk of severe adverse events after a 3rd dose of COVID-19 mRNA vaccine is low and comparable to the risk after a 2nd dose.
Figure:
Note: Adapted from Niesen et al. Prevalence of vaccine-associated adverse events in 3-dose vaccinated individuals during the 14-day period before 1st dose, after 1st dose, after 2nd dose, and after 3rd dose in (a) individuals that received 3 doses of BNT162b2, and (b) individuals that received 3 doses of mRNA-1273. Error bars indicate 95% confidence intervals, and asterisks indicate adverse events with significant (two-tailed p-value <0.05) difference in prevalence after the 3rd dose, compared with before the 1st dose (blue asterisk) or after the 2nd dose (orange asterisk). Used by permission of authors.
PEER-REVIEWED
Burdens of post-acute sequelae of COVID-19 by severity of acute infection, demographics and health status. Xie et al. Nature Communications (November 12, 2021).
Key findings:
- Among U.S. veterans with COVID-19, the overall excess burden of ≥1 post-COVID condition was 73.43 (95% CI 72.10-74.72) per 1,000 persons at 6 months.
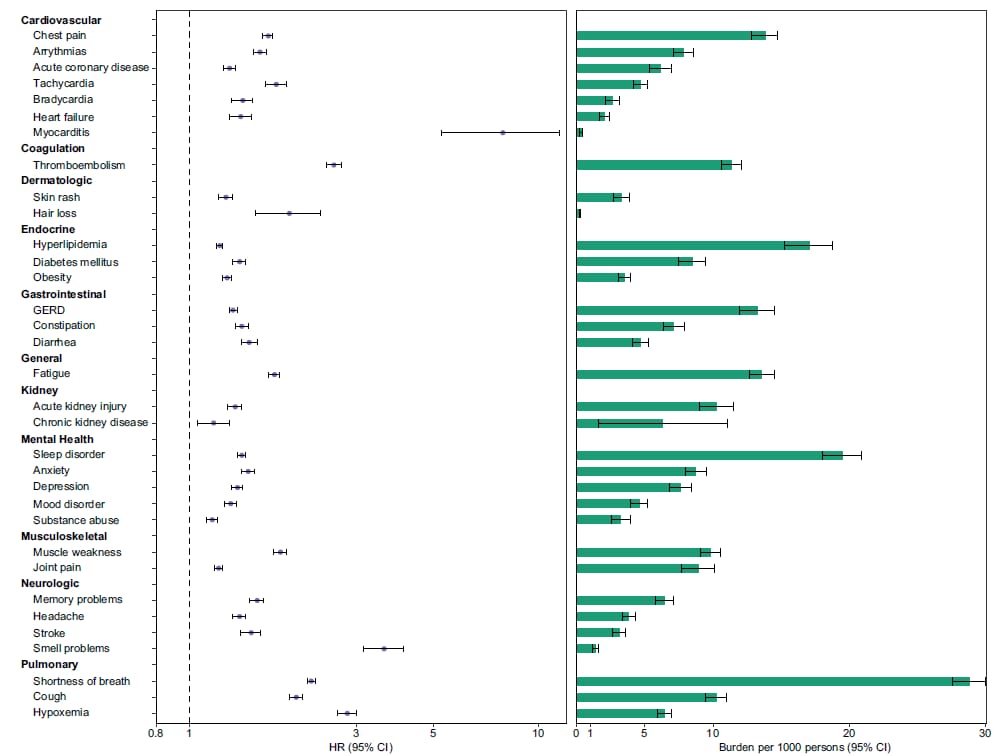
- Conditions with the largest excess burdens included shortness of breath (28.80 per 1,000 persons), sleep disorders (19.51), and hyperlipidemia (17.09) (Figure).
- Excess burden of post-COVID conditions was 360.16 per 1,000 persons in those admitted to an ICU, 217.08 in hospitalized patients, and 44.51 in non-hospitalized patients.
Methods: Retrospective cohort study of COVID-19 patients who tested positive March 2020–March 2021 (n = 181,384) and uninfected controls (n = 4.4 million) using Veterans Health Administration data. Outcomes ascertained from 30 days after infection until the end of follow-up. Burden defined as having conditions in excess of the uninfected control group; models adjusted for multiple factors, including comorbid conditions. Limitations: Predominantly male participants; burdens may be underestimated if conditions not recorded in medical records; findings might not be generalizable.
Implications: Post-COVID conditions encompass a wide range of syndromes and likely pose significant challenges to patients and the U.S. healthcare system.
Figure:
Note: Adapted from Xie et al. Risks and burdens of post-COVID conditions. Hazard ratio (HR) and 95% CIs are presented in the left panel and burdens per 1,000 COVID-19 patients at 6 months are presented in the right panel; right limit of the bar represents estimated burden and error bars represent the 95% CI. Estimated burden was defined as having conditions in excess of the control group. Licensed under CC BY 4.0.
PEER-REVIEWED
Disparities in COVID-19 outcomes by race, ethnicity, and socioeconomic status: A systematic-review and meta-analysis. Magesh et al. JAMA Network Open (November 11, 2021).
Key findings:
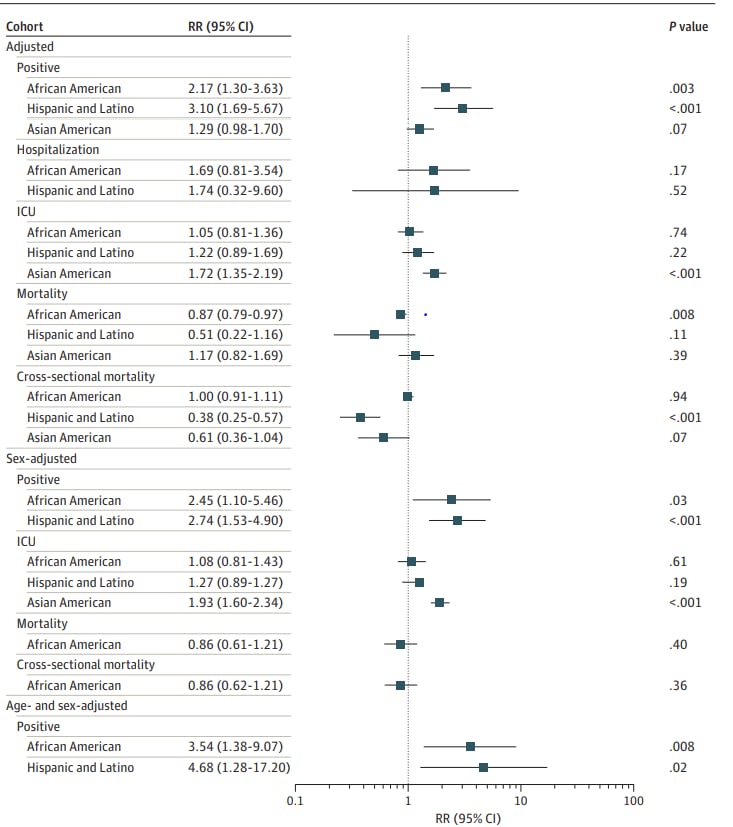
- In a meta-analysis of 68 studies (>4 million persons), Black or African American individuals and Hispanic or Latino individuals were more likely than White individuals to test positive for COVID-19 (Figure).
- Asian American individuals had the highest risk of ICU admission (Figure).
- Among Black or African American individuals, lower county median income was associated with increased rates of test positivity and mortality.
- Among Hispanic/Latino individuals, the linear association between median income and morbidity or mortality was inconsistent and differed by study type (cross-sectional vs. cohort).
Methods: Systematic review and meta-analysis of 68 U.S. based-studies (>4 million individuals) that were published January 1, 2020–January 6, 2021. Data were pooled using a random-effects model. Metaregression conducted to evaluate adjusted associations. Limitations: Race/ethnicity data missing for large proportion (~40%) of individuals; incomplete data for several racial and ethnic groups prevented inclusion of these groups in some analyses; many studies lacked variables of interest; susceptible to biases of included studies.
Implications: Even after correction for demographic and socioeconomic factors, COVID-19 positivity and ICU admission varied by race/ethnicity. Socioeconomic and racial inequities should be factored into efforts to reduce COVID-19 incidence and mortality.
Figure:
Note: Adapted from Magesh et al. Adjusted, sex-adjusted, and sex- and age-adjusted risk ratios (RRs) for African American, Hispanic/Latino, and Asian American individuals (compared with White individuals) according to COVID-19 positivity, hospitalization, ICU admission, and mortality. Licensed under CC BY.
Supporting health equity through data-driven decision-making: A local health department response to COVID-19. Hansotte et al. American Journal of Public Health (October 28, 2021).
Key findings:
- The Marion County Public Health Department (Indiana) integrated COVID-19 case data from multiple sources, created a community-based dashboard, solicited input and support from long-standing partners with community influence, and used the data and partner input to strategically place testing sites near populations with higher disease burden.
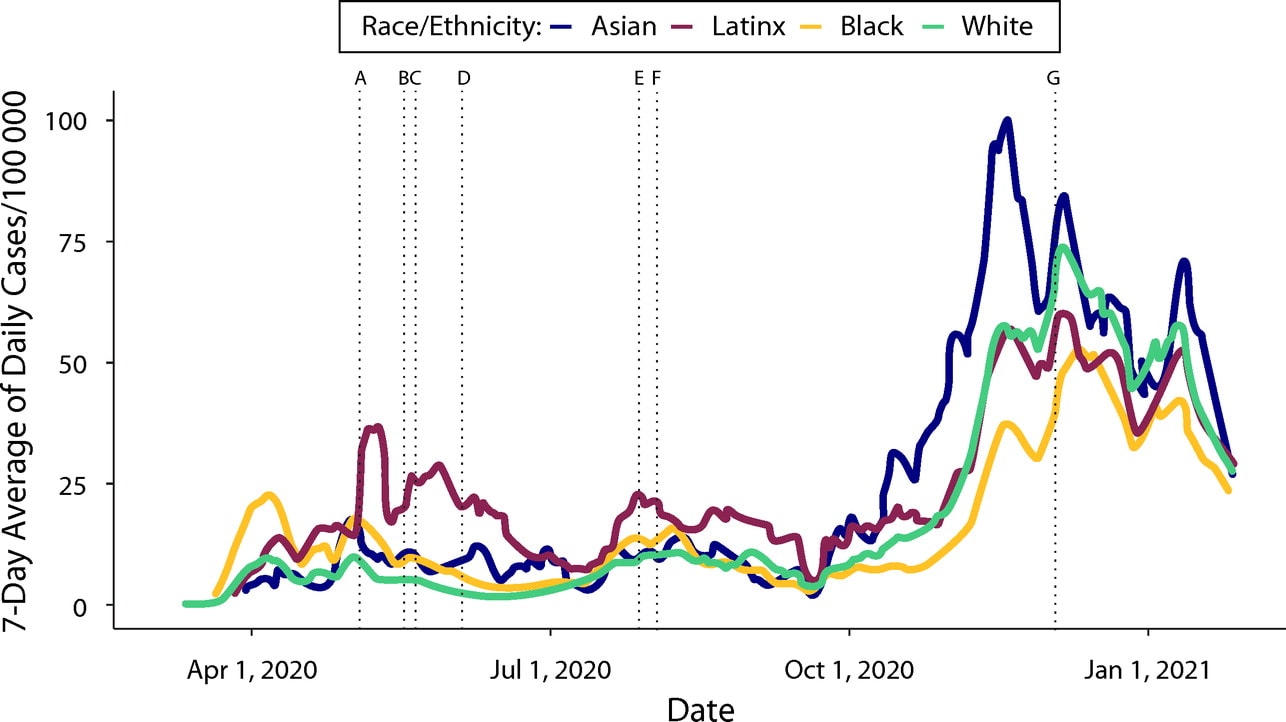
- Testing rates increased and case rates declined among Black or African American, Hispanic/Latino, and Burmese residents in the 2 months after strategic placement of testing sites and the launch of information campaigns for the communities of interest (Figure).
Methods: Trends of COVID-19 cases and tests over time were examined in relation to dates testing sites were opened, March 2020–January 2021. Limitations: Non-experimental design and no control of confounding factors, findings might not be generalizable to other populations.
Implications: A data- and community-based, integrated intervention by local public health partners may contribute to more equitable access to COVID-19 testing.
Figure:
Note: Adapted from Hansotte et al. COVID-19 cases per 100 000 by race/ethnicity: Marion County, IN, March 6, 2020–January 27, 2021 showing trends among Asian (including Burmese), Hispanic or Latino, Black or African American, and White residents. Dotted vertical lines indicate opening dates of MCPHD community testing sites: A = Eastside church (near Black or African American communities), B = educational campus (Hispanic or Latino communities), C = Westside racetrack (Hispanic or Latino communities), D = Marion County Public Health Department main site, E = Southside clinic (Burmese communities), F = Westside commercial, G = county fairgrounds. Permission request in process.
Vaccines
- Describing the population experiencing COVID-19 vaccine breakthrough following second vaccination in England: A cohort study from OpenSAFELY. Green et al. medRxiv (Preprint; November 8, 2021). Among ~10.8 million fully vaccinated individuals in England as of June 30, 2021, incidence of breakthrough infections was 12.33 per 1,000 person-years of follow-up. Breakthrough infections were mostly mild; incidence rates for hospital admissions and deaths were 0.70 (95% CI 0.65-0.74) and 0.12 (95% CI 0.1-0.14) per 1,000 person-years, respectively. Comorbidities associated with the highest rates of breakthrough COVID-19 hospitalization included renal replacement therapy, organ transplant, and hematological malignancy.
- Parents’ intention to vaccinate their 5-11 years old children with the COVID-19 vaccine: Rates, predictors and the role of incentives. Shmueli. medRxiv (Preprint; November 9, 2021). Among parents of children aged 5–11 years in Israel who were surveyed September 23–October 4, 2021 (n = 1,012), 27% intended to vaccinate their children against COVID-19 immediately (within 1 month of availability), 26% intended to vaccinate between 1–3 months, 24% would wait, and 23% would not vaccinate their children at all. The main reasons provided for not vaccinating immediately included: concerns about vaccine safety in children (64%), fear of severe side effects (60%), and fear that the clinical trials and authorization process were carried out too quickly (56%). Additional reasons included feeling that COVID-19 isn’t dangerous for children so there is no reason to vaccinate them (33%), and belief that vaccine effectiveness was low (25%).
Variants
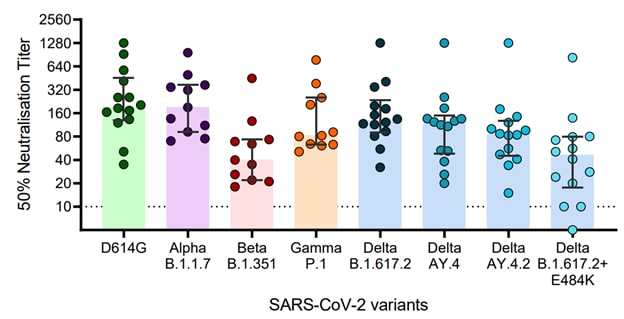
- Neutralisation of SARS-CoV-2 Delta sub-lineage AY.4.2 and B.1.617.2+E484K by BNT162b2 mRNA vaccine-elicited sera. Lassauniere et al. medRxiv (Preprint; November 09, 2021). In sera of individuals vaccinated with BNT162b2 (n = 14) in Denmark, the AY.4.2 variant was not more resistant to neutralization than the parental Delta, showing only 2.3-fold reduction in neutralization compared to wild type. The Delta variant with the E484K mutation was found to be 4.2-fold more resistant to neutralization.
Note: Adapted from Lassauniere et al. SARS-CoV-2 neutralizing antibody titers against variants of concern Alpha, Beta, Gamma, and Delta lineage/sub-lineages B.1.617.2, AY.4, AY.4.2, and B.1.617.2+E484K, 2 months after the 2nd dose of BNT162b2 vaccination. Neutralization titers for variants of concern Alpha, Beta, and Gamma were available for 11 of 14 vaccinated sera. Licensed under CC BY 4.0.
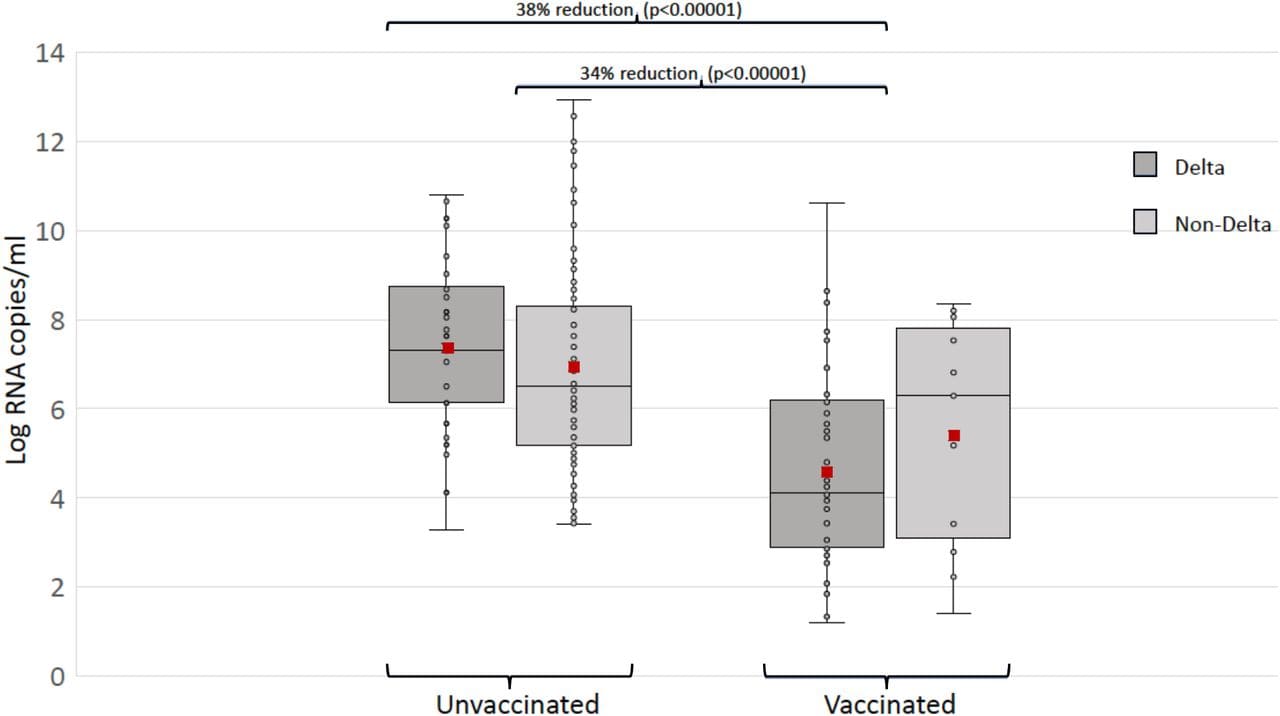
- SARS-CoV-2 Delta vaccine breakthrough transmissibility in Alachua, Florida. Magalis et al. medRxiv (Preprint; November 11, 2021). Published in Clinical Infectious Diseases (March 10, 2022). Viral load (VL) among breakthrough cases infected with the Delta variant (n = 56) and those infected with other variants (n = 13) were similar. When compared with unvaccinated age- and gender-matched cases infected with Delta (n = 36) or other variants (n = 75), Delta breakthroughs exhibited 38% lower VL than unvaccinated Delta cases (p <0.00001).
Note: Adapted from Magalis et al. VL distribution in vaccinated and unvaccinated SARS-CoV-2 infected patients. Each box plot (with line at median and red dot indicating the mean) represents a group of patients infected with either the Delta variant or other variants according to the legend in the figure. For each group pair, a two-tailed Mann–Whitney U test was executed. P-value and effect size are shown on top for those comparisons between groups that were significant at the 5% level after Bonferroni correction for multiple tests. Licensed under CC-BY-NC-ND 4.0.
Natural History, Reinfection, and Health Impact
- Association of self-reported COVID-19 infection and SARS-CoV-2 serology test results with persistent physical symptoms among French adults during the COVID-19 pandemic. Matta et al. JAMA Internal Medicine (November 8, 2021). In 26,823 French adults surveyed December 2020–January 2021, self-reported SARS-COV-2 infection (n = 914) was associated with all persistent physical symptoms surveyed (ORs ranging from 1.39 [95% CI 1.03-1.86] for joint pain to 16.37 [95% CI 10.21-26.24] for anosmia) except hearing impairment and sleep problems. A seropositive test result (n = 1,091) was associated only with persistent anosmia (OR 2.72, 95% CI 1.66-4.46).
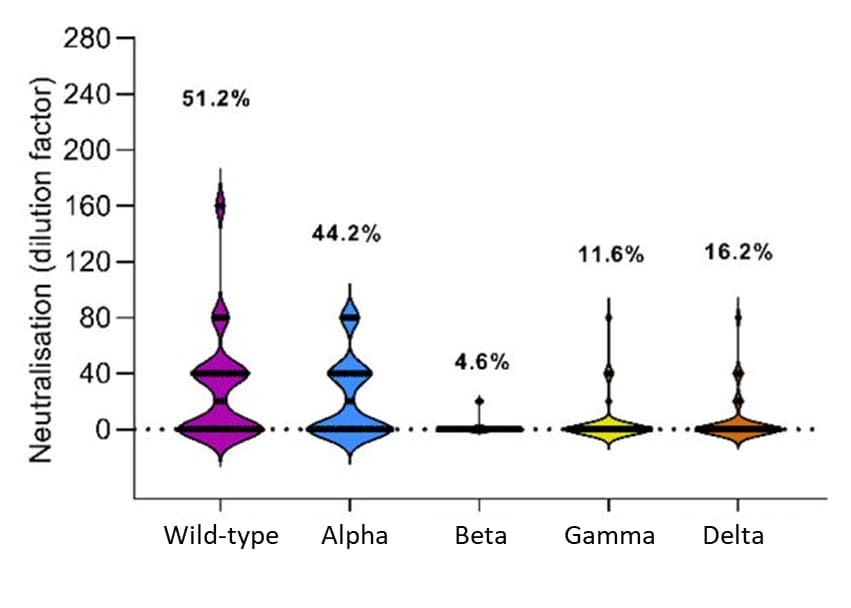
- COVID-19 convalescents exhibit deficient humoral and T cell responses to variant of concern spike antigens at 12 month post-infection. Garcia-Valtanen et al. medRxiv (Preprint; November 11, 2021). In 43 persons who had mild COVID-19 (Australia, March–Apr 2020), 51.2% maintained neutralizing activity against ancestral wild-type virus 12 months after infection. The proportion of persons with neutralizing activity against VOCs was 44.2% (Alpha), 4.6% (Beta), 11.6% (Gamma), and 16.2% (Delta).
Note: Adapted from Garcia-Valtanen et al. Patient serum neutralization end-point cut-off titers (highest dilution factor that yields ≥50% inhibition of cell death after live virus infection) at 12 months against ancestral wild-type, Alpha (B.1.1.7), Beta (B.1.351), Gamma (P.1) and Delta (B.1.617.2) live virus particles. Forty was the initial dilution for all serum samples. Neutralization activity was considered negative, value of zero, when neutralization of initial serum dilution was <50%. Licensed under CC-BY-NC-ND 4.0.
Testing
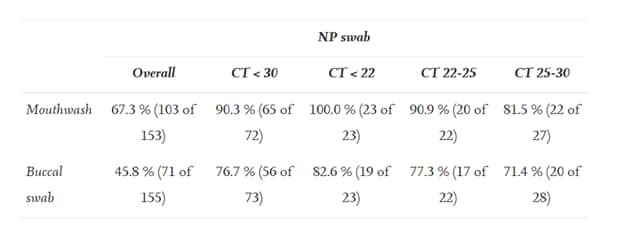
- Evaluation of RT-qPCR of mouthwash and buccal swabs for detection of SARS-CoV-2 in children and adults. Laferl et al. American Journal of Infection Control (October 28, 2021). In hospitalized COVID-19 patients (137 adults and 18 children), the sensitivity of RT-qPCR using mouthwash or buccal swab specimens (compared to NP swabs) was 90.3% and 76.7%, respectively, when NP swab samples had a CT value <30. Sensitivity decreased for both mouthwash and buccal swabs as CT values increased.
Note: Adapted from Laferl et al. Sensitivity of RT-qPCR mouthwash and buccal swab compared to RT-qPCR of NP swab depending on the CT value. Reprinted from American Journal of Infection Control, October 28, 2021, online ahead of print, Laferl et al., Evaluation of RT-qPCR of mouthwash and buccal swabs for detection of SARS-CoV-2 in children and adults, Copyright 2021, with permission from Elsevier and The Association for Professionals in Infection Control and Epidemiology, Inc.
Health Equity
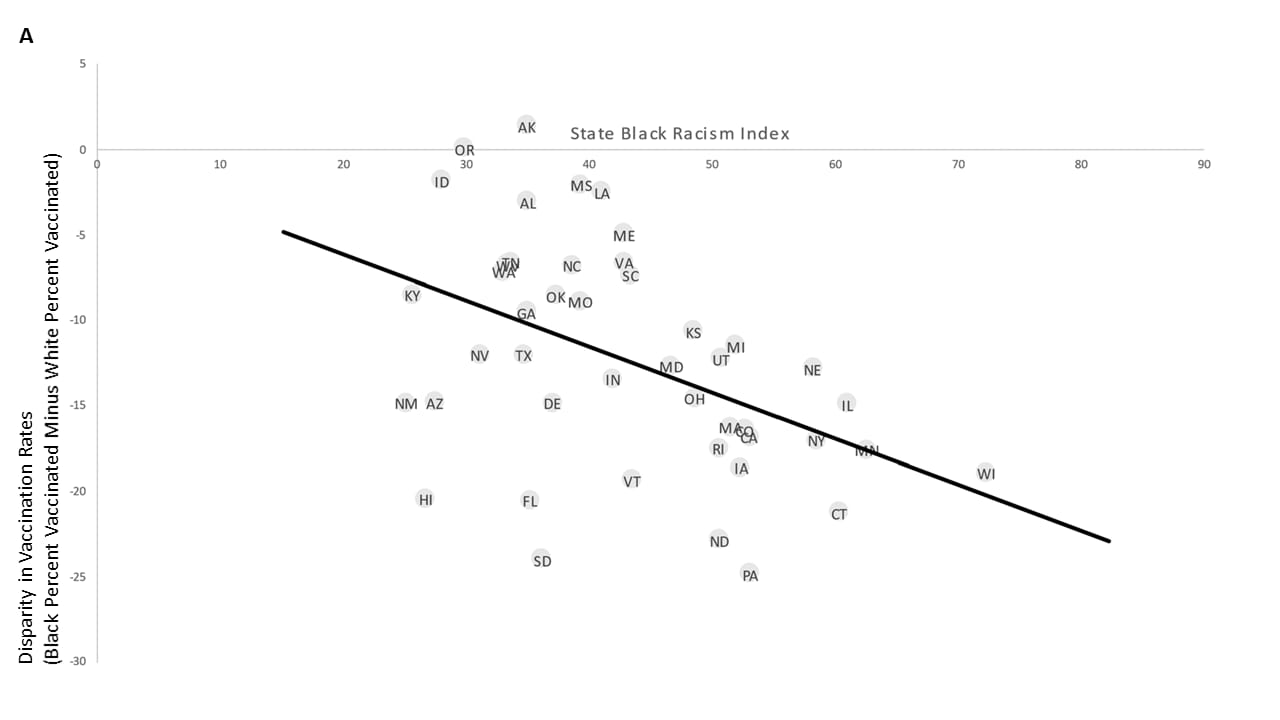
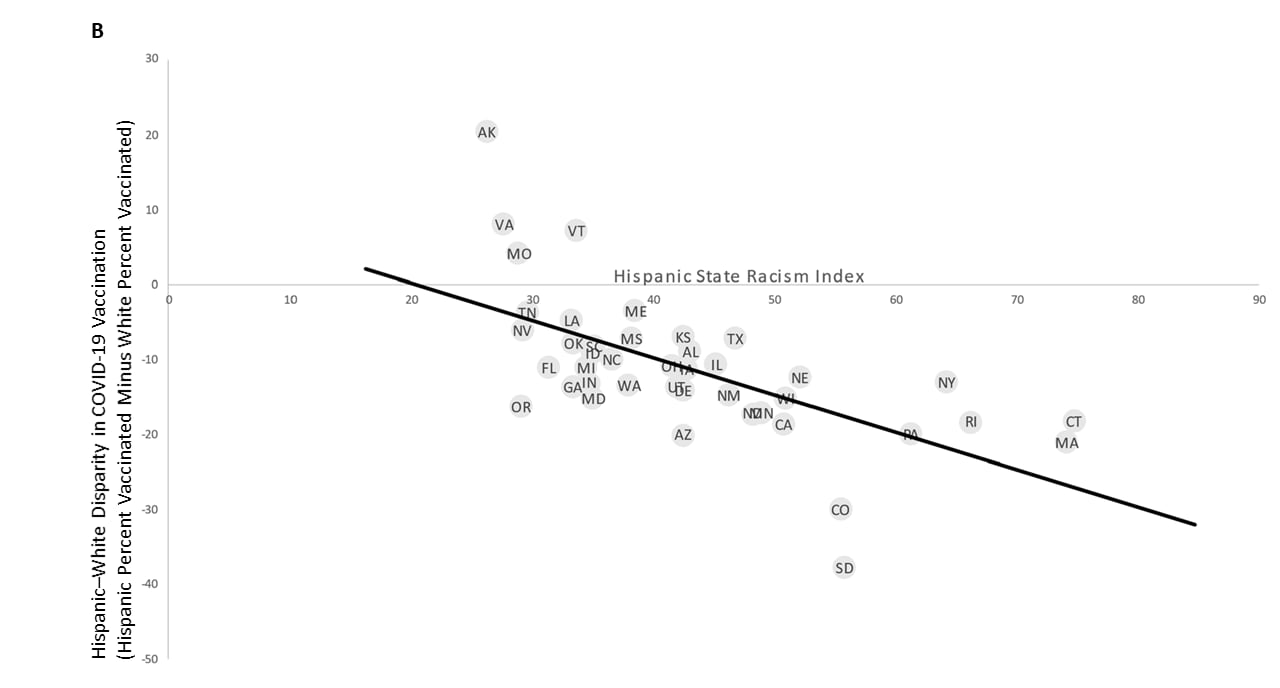
- Racial/ethnic disparities in state-level COVID-19 vaccination rates and their association with structural racism. Siegel et al. Journal of Racial and Ethnic Health Disparities (October 28, 2021). A U.S. state-based structural racism index, based on employment, incarceration, education, residential segregation, and economic indicators, was associated with vaccination coverage among both Black or African American and Hispanic or Latino populations compared with White populations. For each one standard deviation increase in the state racism index, the vaccination rate among Black or African American persons and Hispanic or Latino persons was 3.15 percentage points and 6.27 percentage points lower than the White vaccination rate, respectively.
Note: Adapted from Siegel et al. Scatterplots of the magnitude of the A) Black or African American-to-White and B) Hispanic or Latino-to-White COVID-19 vaccination disparity in each state in relation to the Black or African American or Hispanic state racism index, respectively. Two-letter state abbreviations are shown in each datapoint. Reprinted by permission from Springer Nature Customer Service Centre GmbH: Journal of Racial and Ethnic Health Disparities. Racial/ethnic disparities in state-level COVID-19 vaccination rates and their association with structural racism, Siegel et al., COPYRIGHT 2021.
- Cross-sector monitoring and evaluation framework: social, economic, and health conditions impacted during the COVID-19 pandemic. Wong et al. American Journal of Public Health (October 28, 2021). To guide public health decision-making during the COVID-19 pandemic, Public Health‒Seattle and King County (PHSKC) used a cross-sector framework to monitor changes in selected measures of economic, social, and overall health and well-being. During March–December 2020, almost 554,000 unemployment claims were filed; social service calls more than doubled in mid-March 2020 compared with February 2020; behavioral health crisis calls increased and were 24% higher in November 2020 compared with November 2019; and domestic violence calls increased 25% from January to December 2020. Disproportionate impacts on communities of color were observed.
From the Morbidity and Mortality Weekly Report (November 19, 2021).
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.