COVID-19 Science Update released: October 8, 2021 Edition 108

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
Willingness of children and adolescents to have a COVID-19 vaccination: Results of a large whole schools survey in Englandexternal icon. Fazel et al. EClinicalMedicine (September 27, 2021).
Key findings:
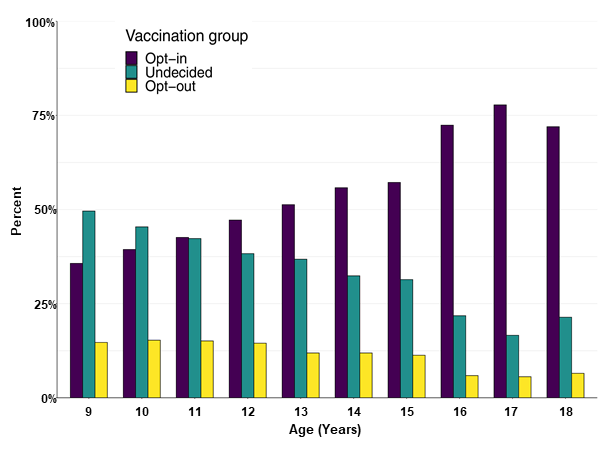
- Among students asked if they would get a COVID-19 vaccine if offered, 50.1% would opt-in, 37.0% were undecided, and 12.9% would opt-out.
- The proportion of students saying they would opt-in increased with age (Figure).
- Students aged 12–18 years who spent 4 hours or more daily on social media were more likely to be undecided (aOR 1.49, 95% CI 1.36-1.63, p <0.001) or to opt-out (aOR 1.51, 95% CI 1.33-1.72, p <0.001) compared to those spending less than 4 hours.
Methods: School-based survey of 27,910 students aged 9–18 years from 180 schools in 4 counties in England, May–July 2021. Responses to the question, “Would you take a COVID-19 vaccine (approved for use in the UK) if offered?” were classified as vaccine receptive (opt-in) or vaccine hesitant (undecided or opt-out). Limitations: Sample may not be representative; self-reported attitudes may not translate into vaccination behavior; findings may not be generalizable outside of England.
Implications: Now that COVID-19 vaccines are available for adolescents, efforts to increase uptake may benefit from focusing on vaccine hesitancy among this group. Social media may be a useful venue for reaching vaccine-hesitant adolescents.
Figure:
Note: Adapted from Fazel et al. Percent of 9–18-year-old students in 4 counties in England who self-reported that they would opt-into, opt-out of, or were undecided about getting COVID-19 vaccination. Licensed under CC-BY-NC-ND.
Titers of SARS CoV-2 antibodies in cord blood of neonates whose mothers contracted SARS CoV-2 (COVID-19) during pregnancy and in those whose mothers were vaccinated with mRNA to SARS CoV-2 during pregnancyexternal icon. Kashani-Ligumsky et al. Journal of Perinatology (September 25, 2021).
Key findings:
- Mean neonatal antibody titer was higher among neonates whose mothers received vaccination against SARS-CoV-2 during the 3rd trimester (225.5 U/ml) compared with neonates whose mothers had prior SARS-CoV-2 infection (83.7 U/ml).
- Mean maternal antibody titers (157 ± 112.8 u/ml) were strongly correlated with mean neonatal antibody titers (150.2 ± 113.2 u/ml) for a subgroup (n = 30) of the study sample.
Methods: Cohort study of Israeli women (n = 79) delivering live singleton births (February 29–March 8, 2021) who were previously infected with SARS CoV-2 (n = 29), received 2 doses of BNT162b2 (Comirnaty, Pfizer/BioNTech) in 3rd trimester (n = 29), or had no evidence of infection or vaccination (n = 21). Neonatal cord blood was tested for SARS-CoV-2 antibodies. Limitations: Small sample size; unknown timing of SARS-CoV-2 infection for 17 of 29 previously infected mothers.
Implications: COVID-19 vaccination during pregnancy might provide robust protection for neonates.
PREPRINTS (NOT PEER-REVIEWED)
COVID-19 vaccine breakthrough infections in Veterans Health Administrationexternal icon. Sharma et al. medRxiv (September 26, 2021).
Key findings:
- Among fully vaccinated Veterans Health Administration (VHA) patients, 11,197 (0.37%) had breakthrough SARS-CoV-2 infections and 2,080 (0.07%) were hospitalized for COVID-19.
- After mRNA-1273 (Moderna): 0.26% had infections; 0.05% were hospitalized.
- After BNT162b2 (Comirnaty, Pfizer/BioNTech): 0.45% had infections; 0.09% were hospitalized.
- After Ad26.COV2.S (Johnson & Johnson/Janssen): 0.57% had infections; 0.09% were hospitalized.
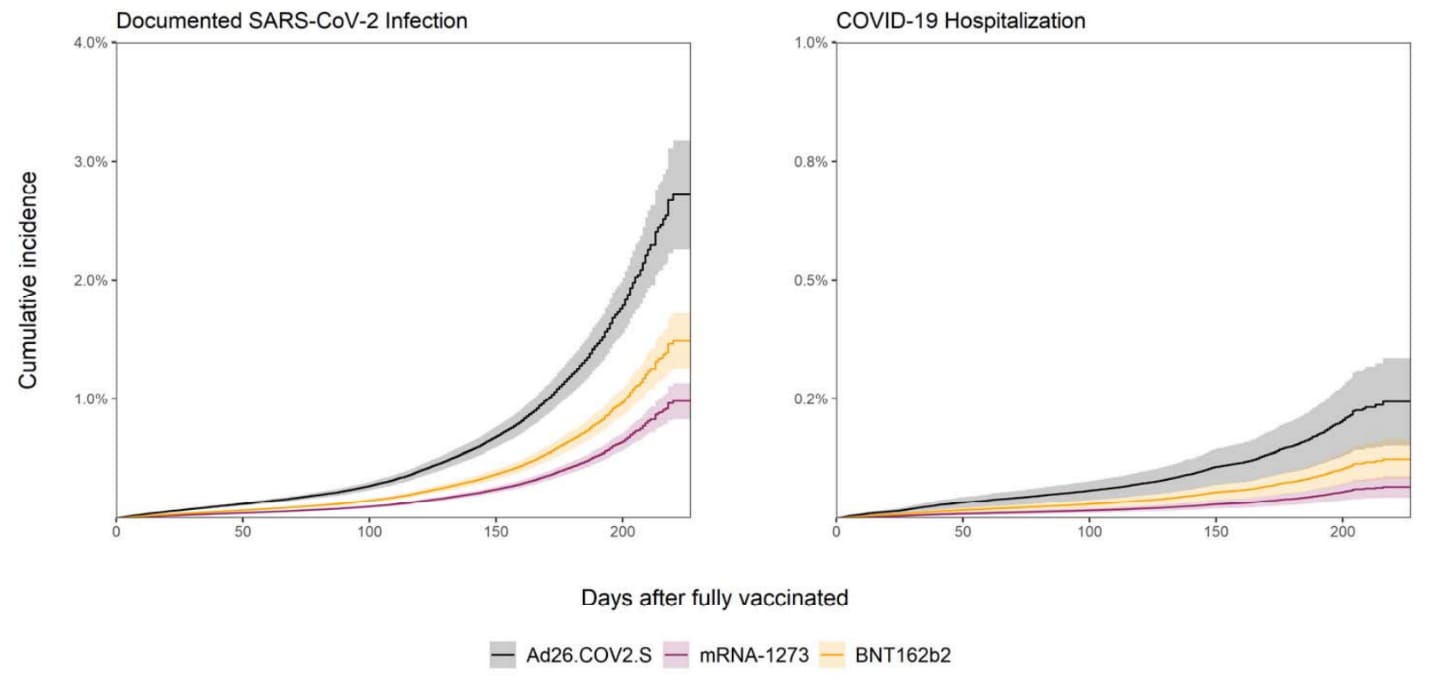
- BNT162b2 and mRNA-1273 vaccinees had fewer infections (adjusted Hazard Ratio [aHR] 0.54, 95% CI 0.51-0.58 and aHR 0.36, 95% CI 0.33-0.38, respectively) and hospitalizations (aHR 0.51, 95% CI 0.43-0.60 and aHR 0.27, 95% CI 0.23-0.32, respectively) than Ad26.COV2.S vaccinees (Figure).
Methods: Retrospective cohort study of 3,032,561 fully-vaccinated persons (aged ≥18 years) in the Veterans Health Administration, January–August 31, 2021. Hazard ratios adjusted for demographics, co-morbidities, and geographic characteristics. Limitations: May not be representative of other populations (sample was >90% male, median age 70 years; nursing home residents were excluded).
Implications: Patients who received the mRNA-1273 or BNT162b2 vaccines had lower risks of infection and hospitalization than those who received the Ad26.COV2.S vaccine, but post-vaccination SARS-CoV-2 infection and hospitalization rates were very uncommon for all authorized vaccines.
Note: Adapted from Sharma et al. Adjusted estimated cumulative incidence of breakthrough infections and hospitalizations by vaccine received, starting from 14 days after full vaccination by: Ad26.COV2.S, mRNA-1273, or BNT162b2. Estimates adjusted for demographics, comorbidities, prior SARS-CoV-2 infection, county-level COVID-19 incidence and vaccine coverage, and regional Delta variant predominance. Cumulative incidence calculated as 1-survival probability. Shaded areas represent 95% CI. U.S. Government work not subject to copyright.
PEER-REVIEWED
Symptoms and health outcomes among survivors of COVID-19 infection 1 year after discharge from hospitals in Wuhan, Chinaexternal icon. Zhang et al. JAMA Network Open (September 29, 2021).
Key findings:
- 45% of surviving patients reported at least 1 post-infection symptom after recovery from hospitalization for COVID-19; the most common symptoms were fatigue, sweating, chest tightness, anxiety, and myalgia.
- Female sex (OR 1.27; 95% CI 1.06-1.52; p = 0.008) and severe disease while hospitalized (OR 1.43; 95% CI 1.18-1.74; p <0.001) were associated with higher risks of fatigue.
- Greater post-infection symptom severity was associated with severe COVID-19 (OR 1.84; 95% CI 1.31-2.58; p <0.001) and coexisting cerebrovascular diseases (OR 1.95; 95% CI 1.07-3.54; p = 0.03).
Methods: Descriptive study of long-term health outcomes associated with COVID-19 among patients (n = 2,433, median age 60 years) discharged from 2 hospitals in Wuhan, China. Outcomes and symptom severity (as measured by chronic obstructive pulmonary disease assessment [CAT] scores) at 1 year were evaluated through telephone interviews, March 1–March 20, 2021. Limitations: Symptoms may be due to other causes; nearly 40% of surviving patients declined participation or were lost to follow-up.
Implications: The population-level burden of long-term effects from COVID-19 is likely to be substantial. Prevention of COVID-19, and particularly of severe COVID-19, through vaccination and other non-pharmaceutical interventions might reduce this burden.
PEER-REVIEWED
The tiny effects of respiratory masks on physiological, subjective, and behavioral measures under mental load in a randomized controlled trialexternal icon. Spang et al. Scientific Reports (October 1, 2021).
Key findings:
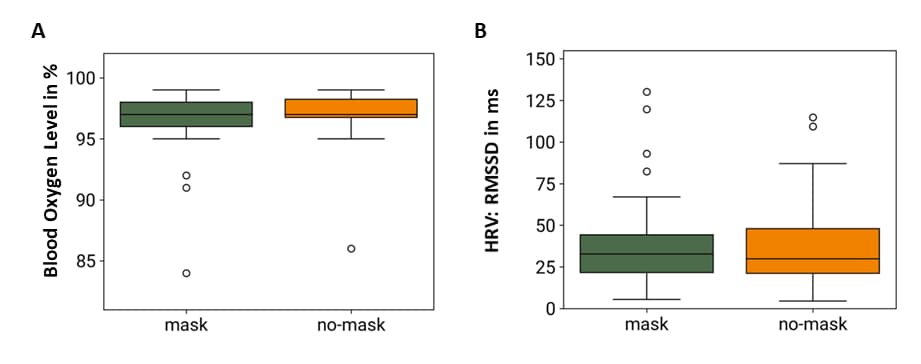
- Performing a cognitive task while wearing an N95 mask was not statistically different than when not wearing a mask, based on key subjective and physiological measurements, such as blood oxygen saturation levels and heart rate variability (Figure).
- Behavioral measures during the task, such as number of correct answers and time spent on each task, did not differ between performance while wearing and not wearing a mask.
Methods: Randomized controlled crossover trial (Germany) of the effect of mask wearing on cognitive performance, October–November 2020. Participants (n = 44) performed 15 minutes of basic arithmetic while wearing either an N95 mask or no face mask. Physiological, subjective, and behavioral performance measures (e.g., number of correctly solved problems) were compared between groups. Limitations: Some participants may have guessed the research question and recorded biased results.
Implications: Cognitive performance does not appear to be affected by N95 mask use.
Figure:
Note: Adapted from Spang et al. Comparison of the physiological metrics of (A) blood oxygen level and (B) heart rate variability (HRV) while wearing an N95 respirator (mask) and not wearing an N95 respirator (no-mask). Box and whisker plots compare the median and the interquartile range (IQR); circles denote potential outliers. RMSSD = root mean square of successive RR interval differences, a measure of HRV. Licensed under CC BY 4.0.
Evaluation of different types of face masks to limit the spread of SARS-CoV-2 – a modeling studyexternal icon. Gurbaxani et al. medRxiv (September 30, 2021). Published in Scientific Reportsexternal icon (May 23, 2022).
Key findings:
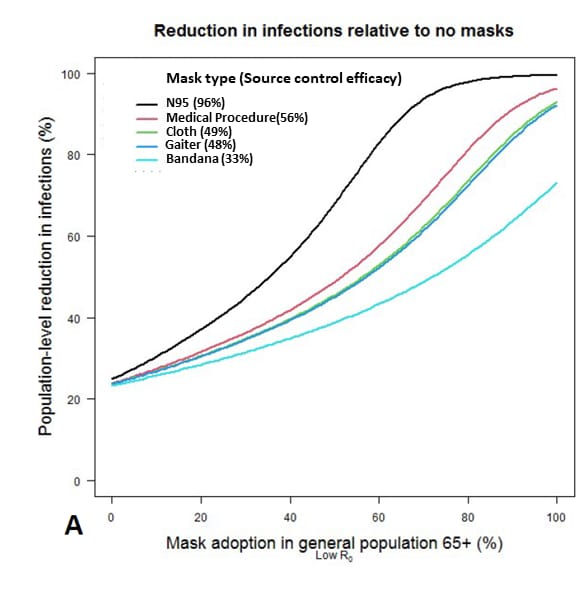
- Based on modeling, face masks reduce cumulative infections (cloth: 69%; medical procedure mask: 78%) when the basic reproductive number (R0) is 2.5 and face masks are worn by 80% of persons aged ≥65 years and by 60% of persons <65 years (Figure).
- Increasing cloth or medical procedure mask efficacies by 30% (by improving mask fit) could reduce the effective reproductive number to 2.3.
Methods: A previously published SARS-CoV-2 transmission model was adapted to include updated laboratory-derived source control and wearer protection efficacy estimates for a variety of face coverings including N95 respirators. The impact of mask wearing on COVID-19 incidence in the United States was estimated. Limitations: Model outcomes are dependent on the parameters and assumptions used.
Implications: Face masks can substantially reduce SARS-CoV-2 transmission. For highly contagious variants such as B.1.617.2 (Delta), mask wearing and other prevention strategies (e.g., vaccination, ventilation, and physical distancing) are needed to limit spread.
Figure:
Note: Adapted from Gurbaxani et al. Percentage reduction in cumulative infections after 6 months of model simulation, relative to no mask use in the population, for N95 respirators, medical procedure masks, cloth masks, gaiters, and bandanas. Mask source control parameters are fixed according to estimates for the given types, and wearer protection efficiency is assumed to be half of source control effectiveness. Younger susceptible persons are assumed to use masks at 70% of the rate of persons aged ≥65 years. Known infected people ≥65 years old are masked at a 90% rate, with younger persons at 70%. The baseline R0 in the absence of mask use is 2.5. U.S. Government work not subject to copyright.
PREPRINTS (NOT PEER-REVIEWED)
Feasibility of a surveillance programme based on gargle samples and pool testing to prevent SARS-CoV-2 outbreaks in schoolsexternal icon. Sweeney-Reed et al. Scientific Reports (September 30, 2021).
Key findings:
- 54% of students agreed to participate in the 16-week program, a response rate deemed high.
- Reasons for program acceptance included an interest in science (83.3%), reducing infection spread (69.5%), and maintaining open schools (24.5%).
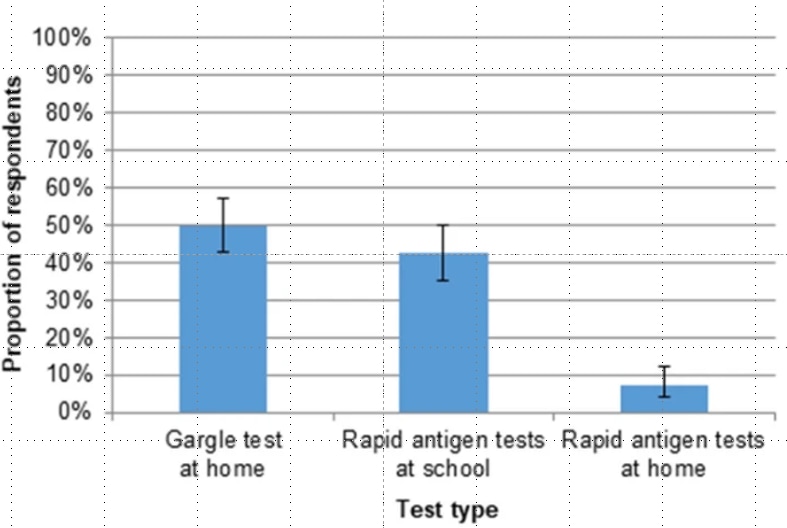
- Home-based gargle specimen collection was preferred over home-based nasal swab collection (for rapid antigen testing) (Figure).
Methods: Feasibility study of a voluntary SARS-CoV-2 school surveillance program in Germany that included bi-weekly home gargle sample collection and PCR-based pooled testing (December 2020–June 2021) among students aged 6–18 years. Questionnaires for student and families addressed household contacts, COVID-19 symptoms, and preferred testing methods. Limitations: Motivation levels may have been high to support the schools remaining open; response to questionnaires declined over study period.
Implications: Gargle and pooled PCR testing among students may be an acceptable and efficient testing method to maintain open schools during the pandemic.
Figure:
Note: Adapted from Sweeney-Reed et al. Responses to questionnaires in which participants were provided with multiple choice options regarding preferences for a particular SARS-CoV-2 test type (N = 188). Error bars: 95% CI. Licensed under CC BY 4.0.
PREPRINTS (NOT PEER-REVIEWED)
Performance of self-collected anterior nasal swabs and saliva specimens for detection of SARS-COV-2 during symptomatic and asymptomatic periods.external icon Grijalva et al. Open Forum Infectious Diseases (September 25, 2021).
Key findings:
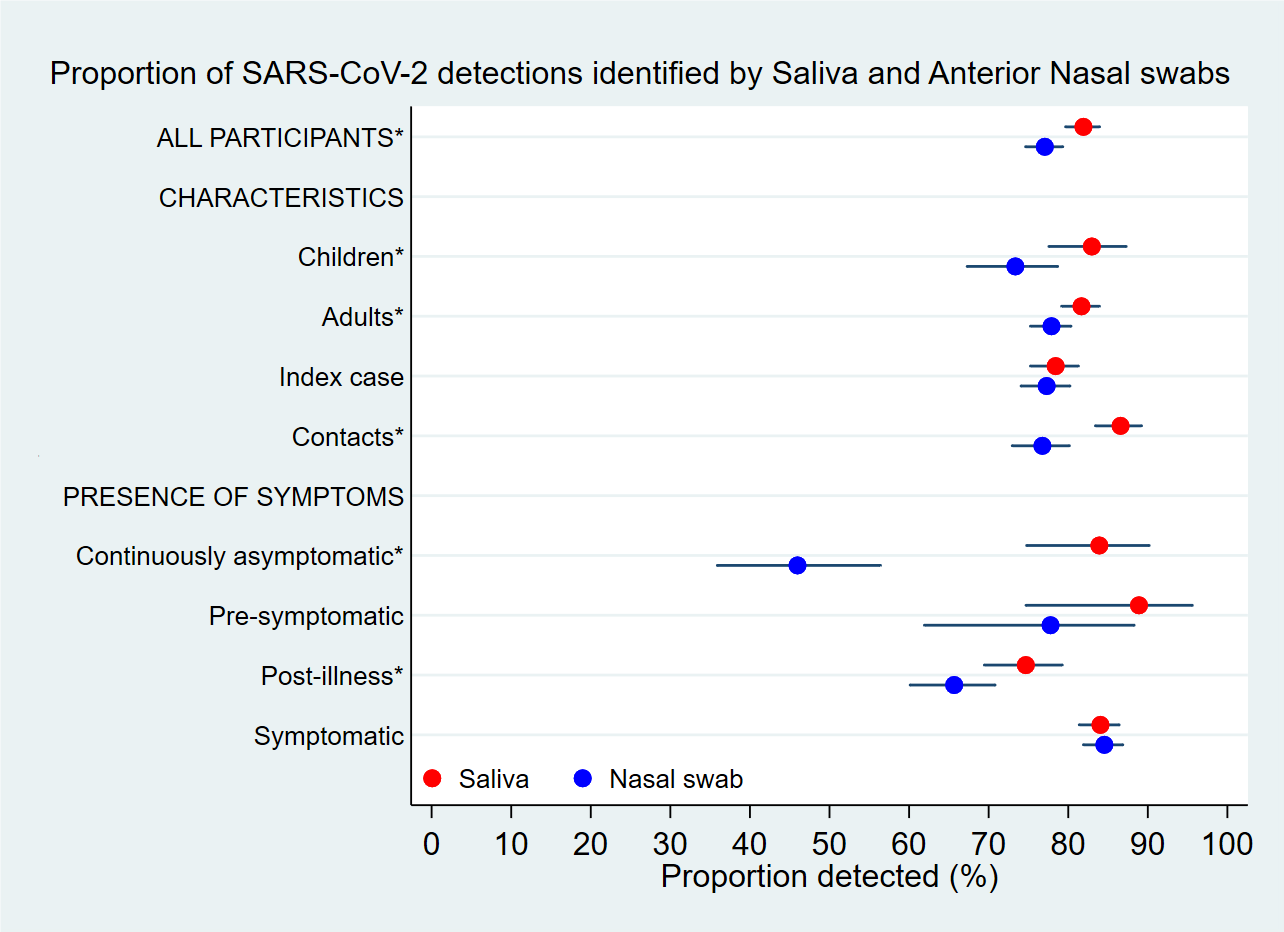
- Among 1,238 SARS-CoV-2 RT-PCR positive specimens, saliva detected 81.9% (95% CI 79.7-84.0) and anterior nasal (AN) swabs detected 77.1% (95% CI 74.6-79.3) (Figure).
- Among specimens from asymptomatic people, saliva outperformed AN swabs by a difference of 51.2% (Figure).
- Agreement was high (83.9%) between paired AN swabs and saliva specimens (n = 2,535).
Methods: A prospective household transmission study in Tennessee (April–November 2020). Paired self-collected AN swabs and saliva specimens were collected daily for 14 days by SARS-CoV-2 positive participants (index cases, n = 83) and household contacts (n = 133). Limitations: No nasopharyngeal swab comparison; study conducted prior to the emergence of the Delta (B.1.617.2) variant.
Implications: Self-collection of saliva specimens may be a viable collection method, particularly in household settings.
Figure:
Note: Adapted from Grijalva et al. Percent positive RT-PCR of saliva and nasal swabs relative to total detected positives of both combined; subdivided by age, index, and symptomatic subgroups. Horizontal bars = 95% confidence intervals; * = statistically significant. Licensed under CC-BY-NC-ND 4.0.
PREPRINTS (NOT PEER-REVIEWED)
Linguistic fairness in the U.S.: The case of multilingual public health information about COVID-19external icon. Blasi et al. medRxiv (September 29, 2021).
Key findings:
- Among 51 jurisdictional English-language websites, 30 (59%) included automated translation; 29 (57%) provided links to CDC’s multilingual COVID-19 web resources.
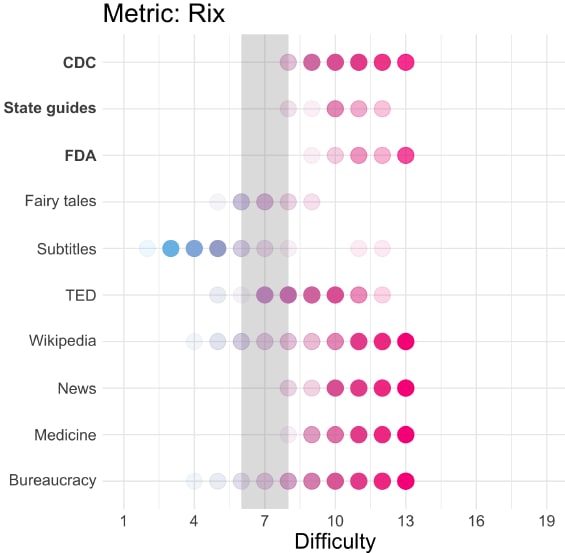
- Foreign language material about COVID-19 available on CDC, FDA, and state websites often exceeded the recommended maximum 8th-grade reading level (Figure).
Methods: Health department websites for all 50 states and Washington D.C. were reviewed for non-English information about COVID-19, March 1–5, 2021. Spanish language web pages from CDC, FDA, and 12 state health departments were analyzed for readability with multiple measures. Limitations: Readability measures may not fully reflect reading comprehension levels.
Implications: Greater emphasis on availability of non-English language information, especially when written in plain language, may improve dissemination of health information about COVID-19.
Figure:
Note: Adapted from Blasi et al. Readability of official Spanish-language information about COVID-19 based on Rate Index (Rix) readability metrics. The gray bar indicates the recommended reading level for medical information written for the general public (grades 6–8). TED = transcripts of TED (Technology, Entertainment, Design) talks. Used by permission of authors.
PREPRINTS (NOT PEER-REVIEWED)
Racial and ethnic inequalities in COVID-19 mortality within Texas carceral settings.external icon Marquez et al. medRxiv (September 28, 2021).
Key findings:
- All-cause mortality among incarcerated persons during the pandemic increased overall by 85% from the pre-pandemic period.
- The increase in mortality was greater among Black/African American (126%) and Hispanic/Latino incarcerated persons (107%) compared to White incarcerated persons (52%).
- COVID-19 mortality among Black/African American (adjusted relative risk [aRR] 1.66, 95% CI 1.10-2.52) and Hispanic/Latino incarcerated persons (aRR 1.96, 95% CI 1.32-2.93) was higher than among White incarcerated persons.
Methods: COVID-19-related mortality within the Texas Department of Criminal Justice (TDCJ) was assessed from April 1, 2019–March 31, 2021 (average monthly prison population = 131,873). Standardized all-cause and COVID-19 mortality rates were adjusted by age and sex to match the TDCJ population distribution prior to the pandemic. Limitations: Results may not be generalizable to other carceral settings.
Implications: Within this carceral setting, COVID-19 mortality disproportionately impacted Black/African American and Hispanic/Latino persons. Efforts to understand and address the causes of such disparities are needed to advance health equity.
Vaccines
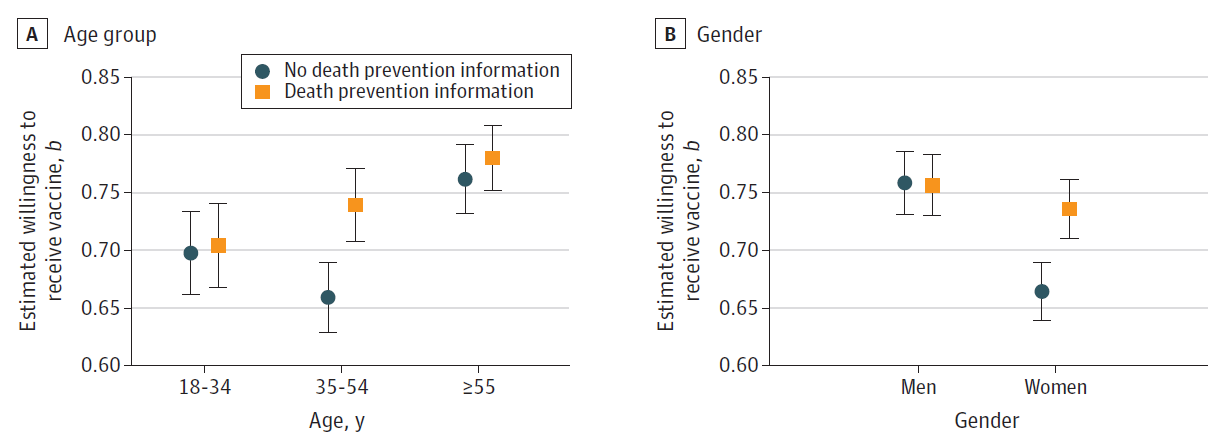
- Assessment of communication strategies for external iconmitigating COVID-19 vaccine-specific hesitancy in Canada. Merkley et al. JAMA Network Open (September 30, 2021). Respondents to an online study (March 2021) in Canada were more confident in vaccine effectiveness and were more willing to receive less-preferred vaccines (i.e., those produced by AstraZeneca or Johnson & Johnson) if they were informed about the vaccine’s effectiveness at preventing death from COVID-19. Among persons aged 35–54 years and women, intention was 0.08 and 0.07 point higher, respectively, on a scale of 0–1, for those informed about death prevention compared with those who were not informed.
Note: Adapted from Merkley et al. Estimated vaccine intention for those given death prevention information and those not given death prevention information. Mean coefficient estimates and 95% error bars (b) for age group (A) and gender (B). Licensed under CC BY.
- Age and smoking predict antibody titres at 3 months after the second dose of the BNT162b2 COVID-19 vaccine.external icon Nomura et al. Vaccines (September 18, 2021). Among 378 fully vaccinated (BNT16b2) healthcare workers (255 women, 123 men; median age 44 years) in Japan, male gender and having ever smoked were risk factors for lower antibody (Ab) titers against SARS-CoV-2 spike antigen, after adjusting for age. In the study, 61% of men and 31% of women had ever smoked, and median Ab titers among those who ever smoked did not differ by sex. Median Ab titers were lower in current smokers than in ex-smokers (p = 0.019).
Variants
- Associations between SARS-CoV-2 variants and risk of COVID-19 hospitalization among confirmed cases in Washington state: A retrospective cohort studyexternal icon. Paredes et al. medRxiv (Preprint; September 30, 2021). Published in Clinical Infectious Diseasesexternal icon (April 12, 2022). Among 23,170 SARS-CoV-2-positive persons in Washington state (December 2020–July 2021), 726 were hospitalized. Persons infected with a variant of concern (VOC) had a higher hospitalization risk than those infected with ancestral lineages.
Natural History, Reinfection, and Health Impact
- Methods for estimation of SARS-CoV-2 seroprevalence and reported COVID-19 cases in U.S. children, August 2020—May 2021external icon. Couture et al. medRxiv (Preprint; September 29, 2021). Published in Open Forum Infectious Diseases as Severe Acute Respiratory Syndrome coronavirus 2 seroprevalence and reported coronavirus disease 2019 cases in US children, August 2020–May 2021external icon (January 30, 2022). Monthly population-weighted SARS-CoV-2 seropositivity among children aged 0–17 years in 14 states in the United States from August 2020–May 2021 using 67,321 residual serum specimens from 3 commercial laboratories found higher rates of COVID-19 among children than detected by case-based surveillance.
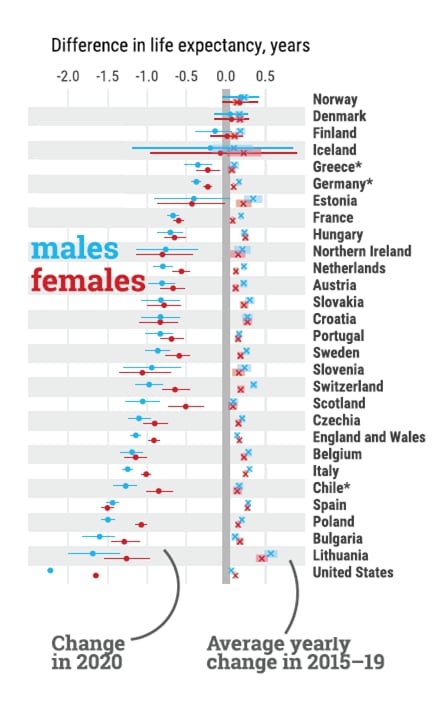
- Quantifying impacts of the COVID-19 pandemic through life-expectancy losses: A population-level study of 29 countries.external iconAburto et al. International Journal of Epidemiology (September 26, 2021). An analysis of mortality data from 29 countries found that average life expectancy declined in all countries for both sexes from 2019–2020, except for females in Finland and both sexes in Denmark and Norway. The largest declines in life expectancy at birth (≥1.5 years) were found among males in the U.S., Lithuania, Bulgaria, and Poland, and among females in the United States and Spain.
Note: Adapted from Aburto et al. Change in life expectancy at birth from 2019–2020 (•) and average yearly change in life expectancy at birth from 2015–2019 (x) for males and females by country. Lines represent 95% confidence intervals. Countries are sorted from smallest to largest losses between 2019 and 2020 in male life expectancy at birth. *Estimates for Chile, Greece, and Germany were only available since 2016. Licensed under CC BY.
Prevention Strategies and Non-Pharmaceutical Interventions
- Prevalence and risk factors for in-school transmission of SARS-CoV-2 in Massachusetts K-12 public schools, 2020-2021.external icon Nelson et al. medRxiv (Preprint; September 26, 2021). In a convenience sample of 8 Massachusetts public school districts (>33,000 students), secondary attack rates for SARS-CoV-2 infections were low, likely owing to comprehensive mitigation measures prior to the emergence of the Delta variant. Of 1,327 contacts who were tested for SARS-CoV-2, only 29 staff and students who tested positive were from probable in-school transmissions. Inconsistent mask use and staff eating lunch together were associated with an increased risk of transmission.
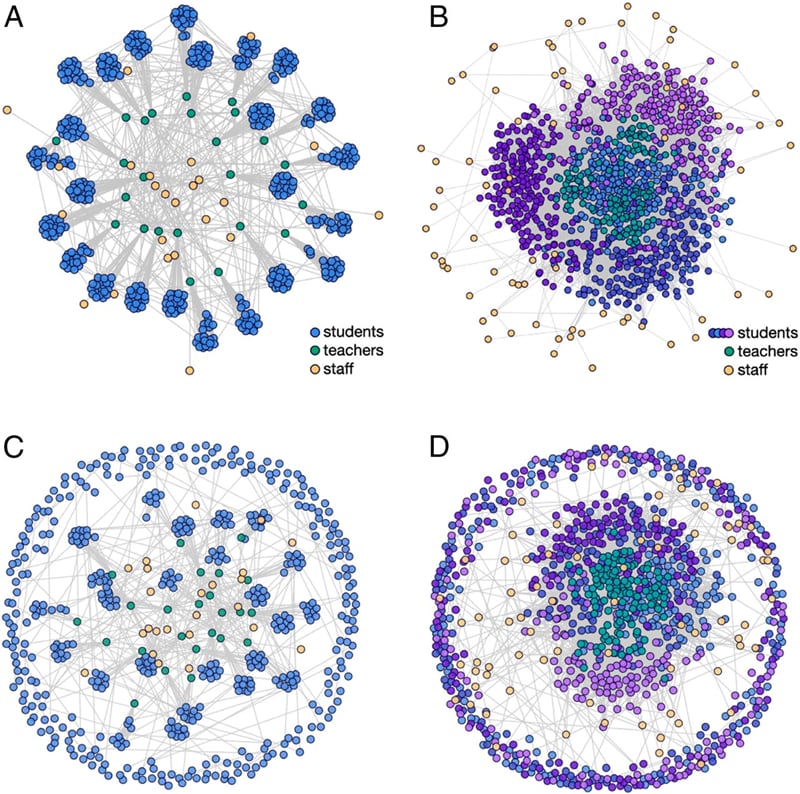
- Model-driven mitigation measures for reopening schools during the COVID-19 pandemicexternal icon. McGee et al. Proceedings of the National Academy of Science (September 28, 2021).Based on modeling, school outbreak risk increases with prevalence of COVID-19 in the community and is harder to control in secondary than in primary schools. Measures to reduce risk include student cohorts that alternate in-school attendance, frequent testing, and vaccination. Mask use, social distancing, and ventilation remain essential.
Note: Adapted from McGee et al. Network structures for primary and secondary schools. Individuals are represented by a circle; gray lines connect close contacts. A) Primary school students have close contacts with students within each classroom and a single teacher. School staff interact with teachers and other staff. B) Secondary school students (blue and purple) move between classrooms and have close contact with 6 teachers. Secondary students cluster in loose social groups and interact with other students in the same grade. Cohorting strategy in primary (C) and secondary schools (D), respectively. Licensed under CC BY 4.0.
Transmission Risk and Dynamics
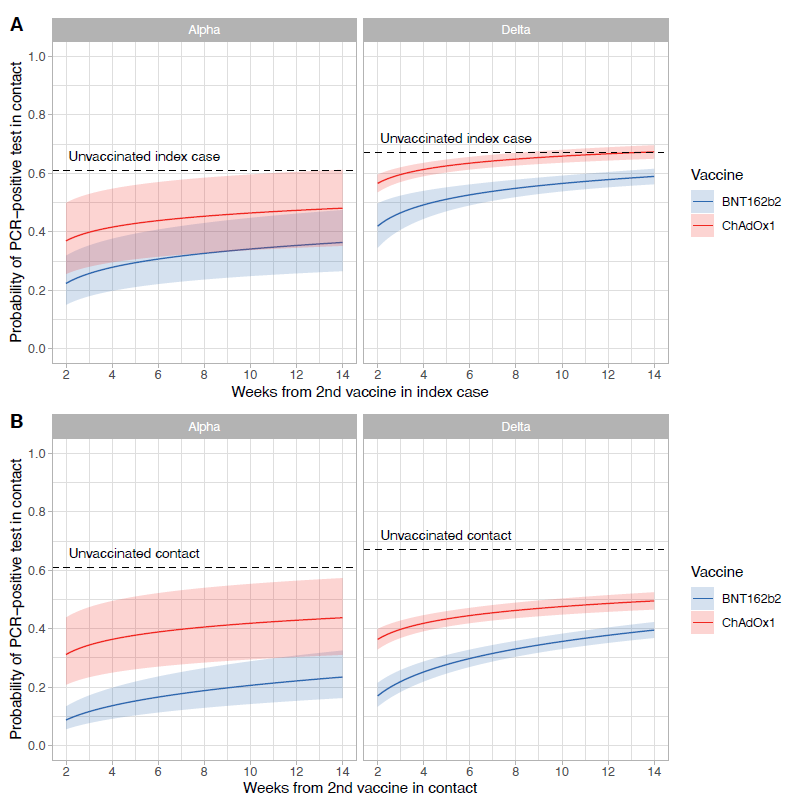
- The impact of SARS-CoV-2 vaccination on Alpha and Delta variant transmissionexternal icon. Eyre et al. medRxiv (Preprint; September 29, 2021). Published in NEJM as Effect of COVID-19 vaccination on transmission of Alpha and Delta variantsexternal icon (January 5, 2022). In a cohort study in England (January–July 2021), 2 doses of ChAdOx1 or BNT162b2 vaccine among SARS-CoV-2 infected persons (index cases, n = 95,716) or their contacts (n = 139,164) reduced transmission of the infection. Both vaccines were more effective against the Alpha than the Delta variant; however, the odds of reducing transmission of Delta was greater for BNT162b2 (aOR 0.35, 95% CI 0.26-0.48) than for ChAdOx1 (aOR 0.64, 95% CI 0.57-0.72). After 12 weeks, vaccine protection declined to levels similar to unvaccinated persons for ChAdOx1, and was attenuated for BNT162b2.
Note: Adapted from Eyre et al. Probability estimates of SARS-CoV-2 infection (y-axis) by variant (Alpha or Delta) and vaccine type (AstraZeneca or Pfizer) versus time after vaccination (x-axis) in (A) index cases and (B) contacts. Licensed under CC BY 4.0.
Health Equity
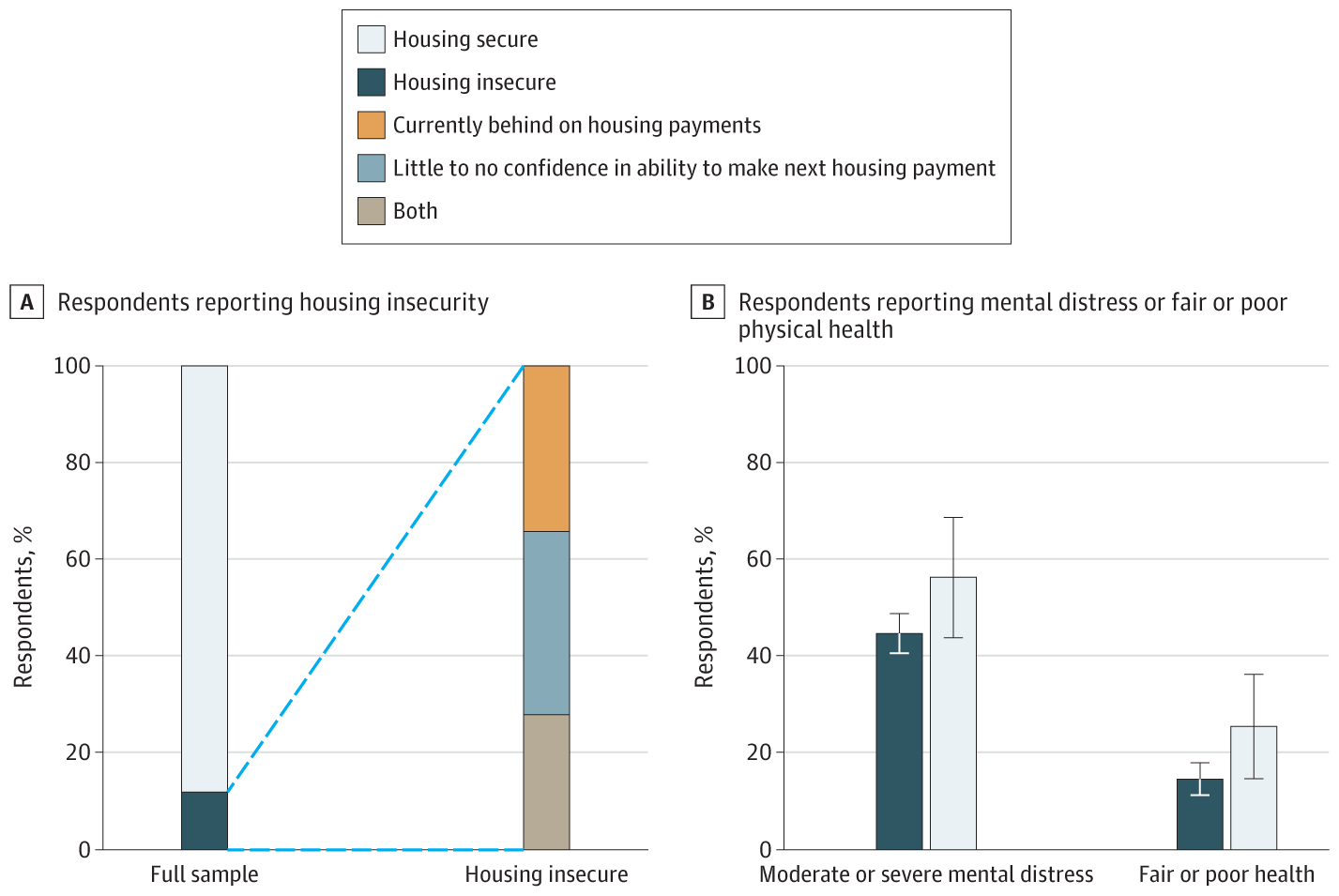
- Association between housing insecurity, psychological distress, and self-rated health among US adults during the COVID-19 pandemicexternal icon. Linton et al. JAMA Network Open (September 30, 2021). Among 1,218 adults responding to an online survey (November 2020), 128 (12%) reported experiencing housing insecurity, which was associated with lower self-rated health but was not associated with greater psychological distress, potentially due to the presence of an eviction moratorium.
Note: Adapted from Linton et al. Weighted percentage of persons reporting (A) housing insecurity (behind on rent or mortgage; or having no/low confidence in ability to pay next rent or mortgage, or both). (B) Mental distress (Kessler 6 Psychological Distress Scale; scores of ≥5 moderate or severe psychological distress) or self-reported fair or poor physical health among a nationally representative sample of 1,218 US adults, Johns Hopkins COVID-19 Civic Life and Public Health Survey, November 11–November 30, 2020. Error bars denote 95% confidence intervals. Licensed under CC BY.
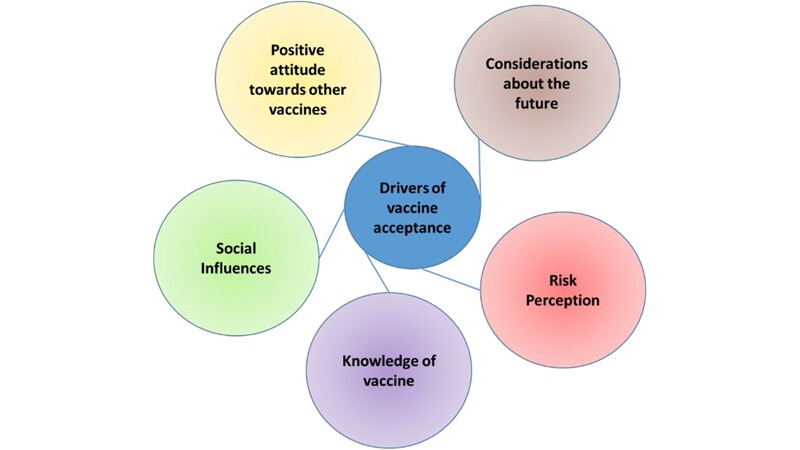
- “The vaccination is positive; I don’t think it’s the panacea”: A qualitative study on COVID-19 vaccine attitudes among ethnically diverse healthcare workers in the United Kingdom. Gogoi et al. medRxiv (Preprint; September 28, 2021). In-depth interviews of healthcare workers (HCWs) in the United Kingdom uncovered diverse attitudes about vaccines, from active acceptance among those who felt privileged to lingering hesitation among some who had received vaccination. Perceptions of mandatory vaccination among HCWs also were mixed with concerns for both individual freedom and societal implications.
Note: Adapted from Gogoi et al. Drivers of vaccine acceptance based on analysis of interviews with 82 participants, United Kingdom, December 2020–July 2021. Licensed under CC BY 4.0.
From the Morbidity and Mortality Weekly Report (October 8, 2021).
- Distribution of SARS-CoV-2 Variants in a Large Integrated Health Care System — California, March–July 2021
- Multicomponent Strategies to Prevent SARS-CoV-2 Transmission — Nine Overnight Youth Summer Camps, United States, June–August 2021
- COVID-19 Outbreaks at Youth Summer Camps — Louisiana, June–July 2021
- National and State Trends in Anxiety and Depression Severity Scores Among Adults During the COVID-19 Pandemic — United States, 2020–2021
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.