COVID-19 Science Update released: July 9, 2021 Edition 97

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update align with the CDC Science Agenda for COVID-19.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
Age-related immune response heterogeneity to SARS-CoV-2 vaccine BNT162b2.external icon Collier et al. Nature (June 30, 2021).
Key findings:
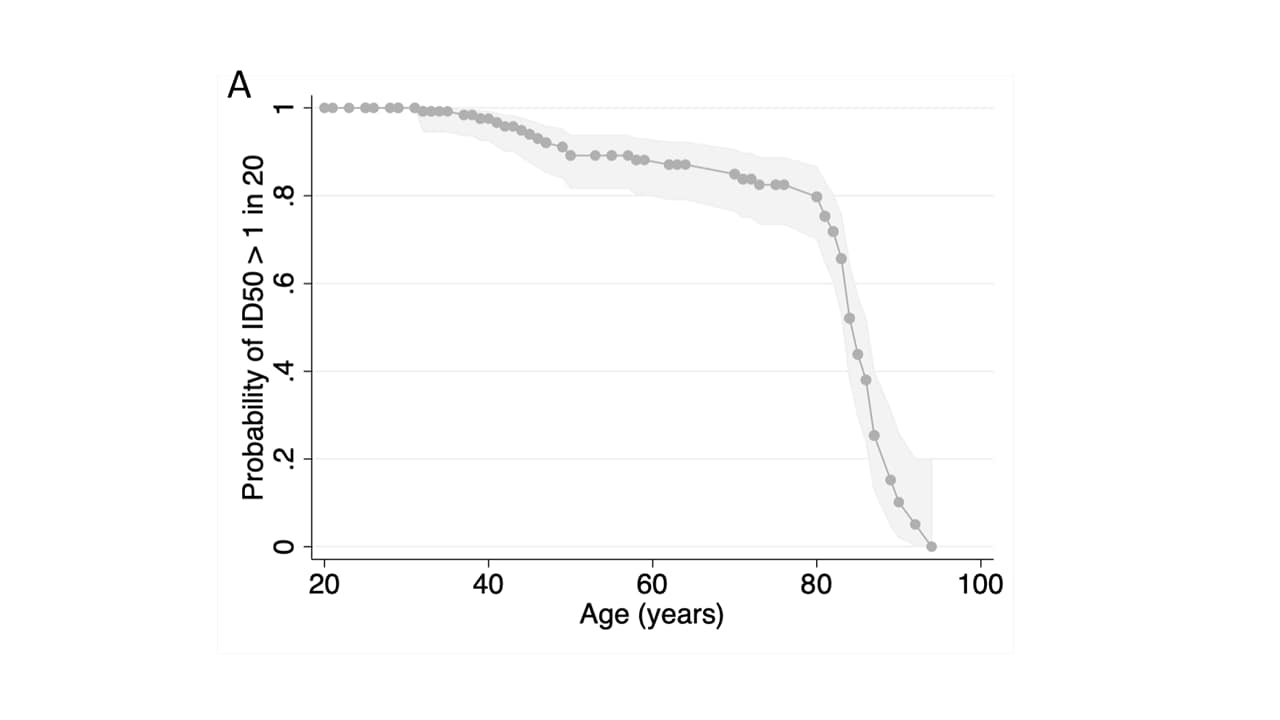
- SARS-CoV-2 virus neutralization after 1 dose of BNT162b2 (Pfizer/BioNTech) drops off precipitously at age 80 years (Figure A).
- Following 2 doses, persons <80 years (n = 15) and ≥80 years (n = 24) show detectable neutralizing titers against B.1.1.7 (Alpha), B.1.351 (Beta) and P.1 (Gamma) variants of concern (VOCs).
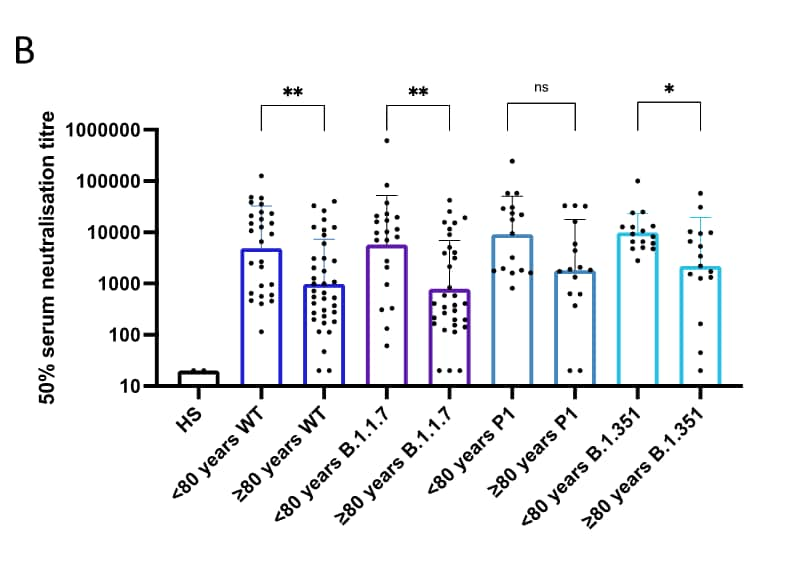
- Serum neutralization against wild-type, B.1.1.7, and B.1.351 was lower among persons ≥ 80 years compared to <80 years (Figure B).
Methods: UK community members and healthcare workers receiving 1st dose of BNT162b2 (n = 140, median age 72 years) were recruited December 14, 2020–February 10, 2021 and followed for up to 3 weeks after 2nd dose (n = 39). Antibody levels, serum neutralization and T-cell function were compared for persons <80 and ≥80 years of age after 1st and 2nd doses. Limitations: Results were limited to the BNT162b2 vaccine; study only considered 3 VOCs (B.1.1.7, B.1.351, and P.1); small number of participants may limit generalizability.
Implications: It is unknown how serum neutralization correlates with protection from infection. BNT162b2 has been found to prevent symptomatic COVID-19 in persons ≥80 years (Bernal et al.external icon).
Figures:
Note: Adapted from Collier et al. Neutralization effects by BNT162b2 sera: a. Proportion of people with detectable neutralization of pseudotyped virus after 1st dose as a function of age (cutoff ID50 = 20). b. Impact of SARS-CoV-2 variants of concern on 50% serum neutralization titer after 2nd dose of BNT162b2 vaccine sera by age group and variant: WT (n = 64), B.1.1.7 (n = 53) Spike mutant B.1.351 (n =32) Spike mutant, P.1 (n = 32). Geometric mean titer and SD are shown; p-values * <0.05, ** <0.01, ns not significant. Reprinted by permission from Springer Nature Customer Service Centre GmbH: Nature, Age-related immune response heterogeneity to SARS-CoV-2 vaccine BNT162b2external icon, Collier et al. Copyright 2021. Advance online publication, June 30, 2021.
SARS-CoV-2 mRNA vaccines induce persistent human germinal centre responses.external icon Turner et al. Nature (June 28, 2021).
Key findings:
- BNT162b2 (Pfizer/BioNTech) vaccination induced strong IgG-dominated plasmablast (PB) responses, peaking 1 week post 2nd dose.
- Robust S-binding germinal center (GC) B-cell responses were detected for up to 12 weeks in lymph node aspirates in a subset of 14 participants.
- PB responses preceded high levels of anti-S binding and neutralizing antibodies (NAbs) to several emerging variants, especially in 8 participants infected prior to vaccination.
Methods: Antigen-specific B cell responses in blood (n = 41) and draining lymph nodes (n = 14) were examined after 2 doses of BNT162b2. PBs binding to SARS-CoV-2 protein was measured by enzyme-linked immune absorbent spot (ELISpot). Limitations: Small sample size, especially for subset analysis.
Implications: BNT162b2 vaccination elicits prolonged GC responses for antibody-mediated immunity in humans. Durable memory B cell immunity may indicate longer lasting humoral immunity than NAb levels alone may suggest.
PREPRINTS (NOT PEER-REVIEWED)
Antibody development after SARS-CoV-2 vaccinations in elderly patients with autoimmune diseases: data from a prospective controlled cohort studyexternal icon. Boekel et al. SSRN (June 28, 2021).
Key findings:
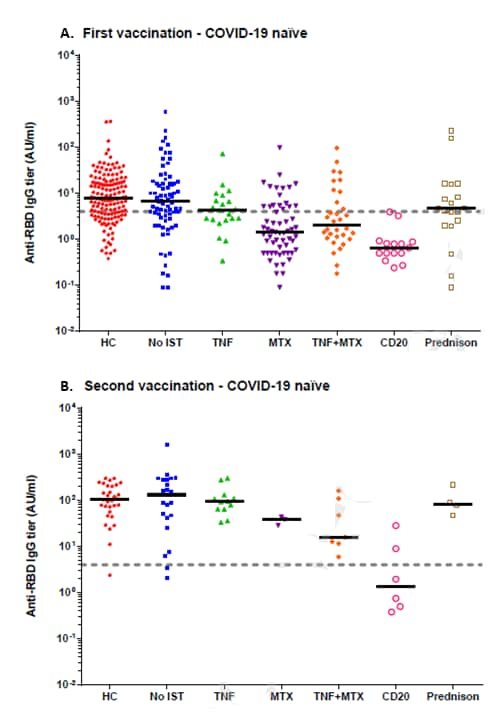
- After 1st dose of BNT162b2 (Pfizer/BioNTech), ChAdOx1 (AstraZeneca), or CX021414 (Moderna) COVID-19 vaccines, neutralizing antibody (NAb) anti-receptor binding domain IgG levels were lower for COVID-19 naïve patients on methotrexate or anti-CD20 vs. healthy controls (Figure A).
- Compared to 71% of healthy controls, 25% of 111 patients on methotrexate and none of 15 patients on anti-CD20 therapies seroconverted.
- After 2nd vaccine dose, except for those on anti-CD20 therapies, more than 88% of all patient groups seroconverted (Figure B).
Methods: Vaccine-elicited antibody responses of patients with autoimmune diseases (n = 480) were compared to health controls (n = 204). Post-vaccination sera were analyzed by receptor binding domain (RBD) antibody ELISAs and compared by treatment type. Limitations: Serology was not available longitudinally after a 2nd vaccination dose; some subgroups among immunocompromised persons are small.
Implications: Two doses of COVID-19 vaccines effectively generate an immune response among patients who are being treated with many immunomodulatory therapies, except anti-CD20 monoclonal antibodies.
Figure:
Note: Adapted from Boekel et al. IgG antibody concentrations after SARS-CoV-2 vaccinations in COVID-19-naïve healthy controls (HC), patients not being treated with immunosuppressive medication (No IST), or those treated with tumor necrosis factor (TNF), methotrexate (MTX), TNF and MTX combined, anti-CD20 therapies (CD20), or prednisone. Permission request in progress.
PEER-REVIEWED
AZD1222-induced neutralising antibody activity against SARS-CoV-2 Delta VOC.external icon Wall et al. The Lancet (June 28, 2020).
Key findings:
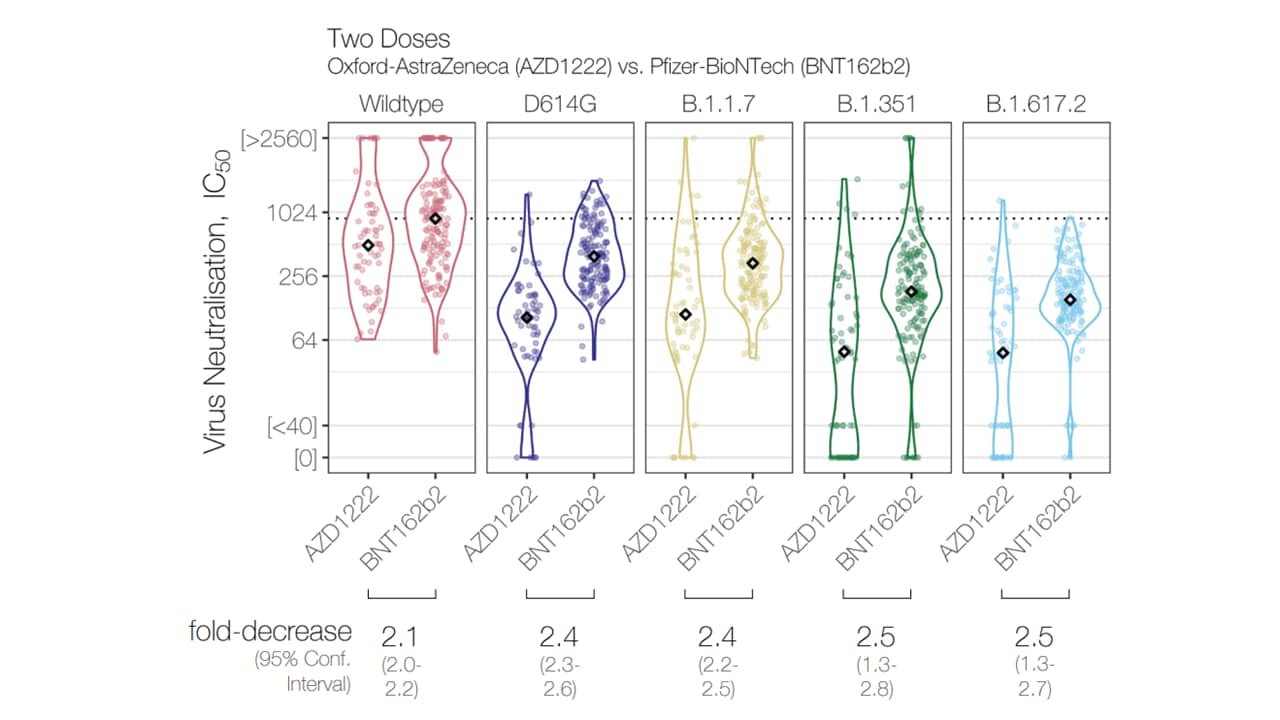
- Virus neutralizing antibody (NAb) response elicited against 5 variants [Wild-type, D614G, B.1.1.7 (Alpha), B.1.351 (Beta), B.1.617.2 (Delta)] after 2 doses of AZD1222 (Oxford/AstraZeneca) was at least 2-fold lower relative to 2 doses of BNT162b2 (Pfizer/BioNTech).
- Neutralizing antibodies were reduced 2.5-fold against B.1.351 and B.1.617.2 (Figure).
Methods: Prospective UK serological study of vaccine-induced neutralizing antibody activity in recipients of AZD1222 (n = 63) compared with BNT162b2 (n = 159). Median NAb titers were measured against 5 variants, after 1 and 2 vaccine doses. Limitations: AZD1222 cohort significantly younger than BNT162b2.
Implications: Neutralizing antibody levels were greater following 2 doses of BNT162b2 compared with 2 doses of AZD1222, suggesting that AZD1222 offers less protection against SARS-CoV-2 variants, including the B.1.617.2 Delta variant.
Figure:
Note: Adapted from Wall et al. NAb activity against 5 SARS-CoV-2 variants, from study participants receiving 2 doses of AZD1222 or BNT162b2. NAb titers are expressed as serum fold-dilution required to achieve 50% virus neutralization (IC50). These authors previouslyexternal icon reported on the neutralizing antibody activity of the 159 2-dose BNT162b2 recipients only. Reprinted from The Lancet, online June 28, 2021, Wall et al., AZD1222-induced neutralising antibody activity against SARS-CoV-2 Delta VOC. Copyright 2021, with permission from Elsevier.
Prevention and attenuation of COVID-19 with the BNT162b2 and mRNA-1273 vaccines.external icon Thompson et al. NEJM (June 30, 2021).
Key findings:
- Adjusted vaccine effectiveness of BNT162b2 (Pfizer/BioNTech) and mRNA-1273 (Moderna) combined was 91% (95% CI 76%-97%) after full vaccination and 81% (95% CI 64%-90%) after partial vaccination.
- Compared to infections in unvaccinated persons, persons with breakthrough infections had:
- 40.2% (95% CI 16.3%-57.3%) lower viral RNA load.
- Reduced illness severity, including fewer days with symptoms (mean days 10.3 vs. 16.7).
Methods: Prospective cohort study of 3,975 vaccinated and unvaccinated health care personnel and essential workers (without prior COVID-19). Weekly RT-PCR nasal swab tests and symptom status collected between December 2020 and April 2021, to determine the effectiveness of full (≥14 days after dose 2) and partial (<14 days after dose 2) mRNA vaccination. Limitations: Genetic sequencing not conducted for all variants; estimates lack precision due to small number of breakthrough infections.
Implications: BNT162b2 and mRNA-1273 are effective in preventing SARS-CoV-2 infection. On the rare occasion of breakthrough infection, mRNA vaccination may reduce viral load and mitigate illness duration and severity.
Two reports of myocarditis after 2 doses of either BNT162b2 (Pfizer/BioNTech) or mRNA-1273 (Moderna) highlight the importance of post-vaccination surveillance in identifying events too rare to be encountered even during Phase 3 clinical trials.
A. Myocarditis following immunization with mRNA COVID-19 vaccines in members of the US military.external icon Montgomery et al. JAMA Cardiology (June 29, 2021).
B. Patients with acute myocarditis following mRNA COVID-19 vaccinationexternal icon. Kim et al. JAMA Cardiology (June 29, 2021).
Key findings for Montgomery et al. and Kim et al.:
- The Military Health System identified 23 cases of acute myocarditis among >2.8 M vaccinees (Montgomery et al). At a tertiary care center in North Carolina (NC) that serves a population of >560,000 vaccinees, 4 cases were found (Kim et al).
- Both BNT162b2 and mRNA-1273 were represented among cases: in the military, 7 received BNT162b2 and 16, mRNA-1273; in NC, 2 received BNT162b2 and 2, mRNA-1273.
- All cases reported symptoms within 5 days after 2nd dose. Ages: median 25 years (20-51) for the military and 23, 24, 36 and 70 years for NC.
- All presented with severe acute chest pain, had abnormal electrocardiogram results, and elevated troponin. Tests did not uncover alternative etiologies or underlying heart disease. All recovered uneventfully.
Methods: Adverse events identified through referrals within the military Defense Health System and review of Vaccine Adverse Events Reporting System (VAERS) reports were used to find cases for a retrospective review (Montgomery et al.). A database of cardiac magnetic imaging at a NC tertiary care center was searched for patients diagnosed with acute myocarditis between February–April in 2017–2021 with recent history of vaccination (Kim et al.). Combined Limitations: Lack of control groups precludes ability to establish causal relationship or estimate rates of myocarditis in vaccinated versus non-vaccinated populations.
Implications for both studies (Montgomery et al. and Kim et al.): As described in an editorialexternal icon, the mechanisms underlying these events are not yet known although are likely to be an immune mediated response to the mRNA SARS-CoV vaccines. Although surveillance is both informal and formal, including VAERS, Clinical Immunization Safety Assessment Project, V-safe, and reports to journals, editors of JAMA Cardiologyexternal icon suggest the system as a whole is invaluable.
PREPRINTS (NOT PEER-REVIEWED)
Ad26.COV2.S elicited neutralizing activity against Delta and other SARS-CoV-2 variants of concern.external icon Jongeneelen et al. bioRxiv (July 1, 2021).
Key findings:
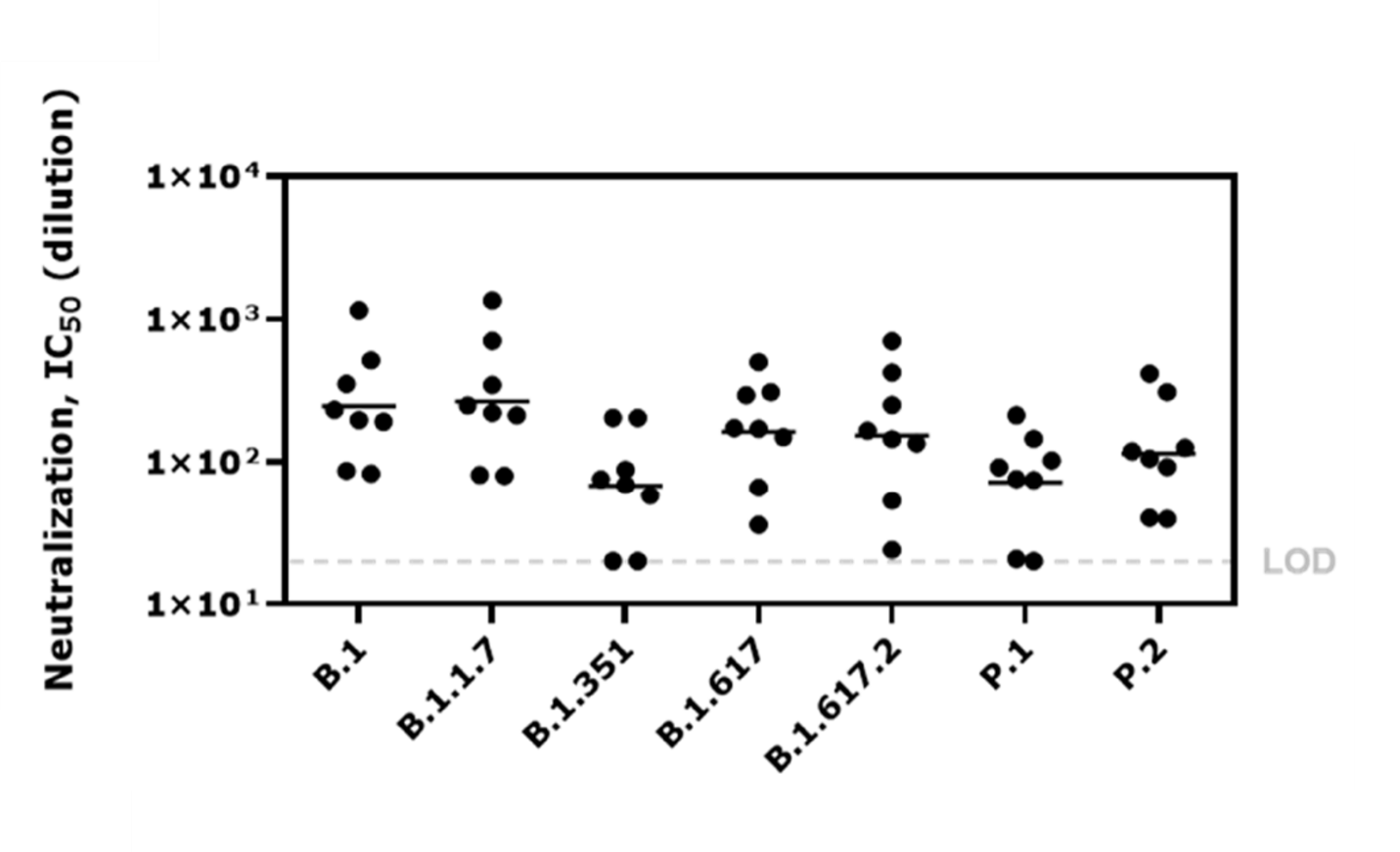
- Compared to B.1, a single dose of Ad26.COV1.2 (Johnson & Johnson/Janssen) vaccine had reduced neutralization sensitivity to SARS-Cov-2 variants B.1.351 (3.6-fold less), P.1 (3.4-fold less), and B.1.617.2 (1.6-fold less).
Methods: Sera collected 71 days post vaccination with Ad26.COV2.Sfrom 8 participants in a phase 3 clinical trial (age range: 47–91) were tested for neutralizing activity against SARS-CoV-2 variants of concern including B.1.351 (Beta), P.1 (Gamma), and B.1.617.2 (Delta). Limitations: Results from a clinical trial may not be representative of real-world vaccine effectiveness; small sample size.
Implications: In a small in-vitro study, Ad26.COV2.S vaccine neutralization was reduced against a variety of variants, though less so for B.1.617.2. Real world evidence will be necessary to evaluate the effectiveness of this vaccine against variant 1.617.2.
Figure:
Note: Adapted from Jongeneelen et al. Neutralization activity of serum antibodies elicited by Ad26.COV2.S vaccine against SARS-CoV-2 spike pseudotyped virus variants. Dots are independent measurements per virus variant with geometric mean titers as solid horizontal lines. Dotted line = limit of detection. Licensed under CC-BY-NC-ND 4.0.
Reduced neutralisation of the Delta (B.1.617.2) SARS-CoV-2 variant of concern following vaccinationexternal icon. Davis et al. medRxiv (June 28, 2021). Published in PLOS Pathogens (December 2, 2021).
Key findings:
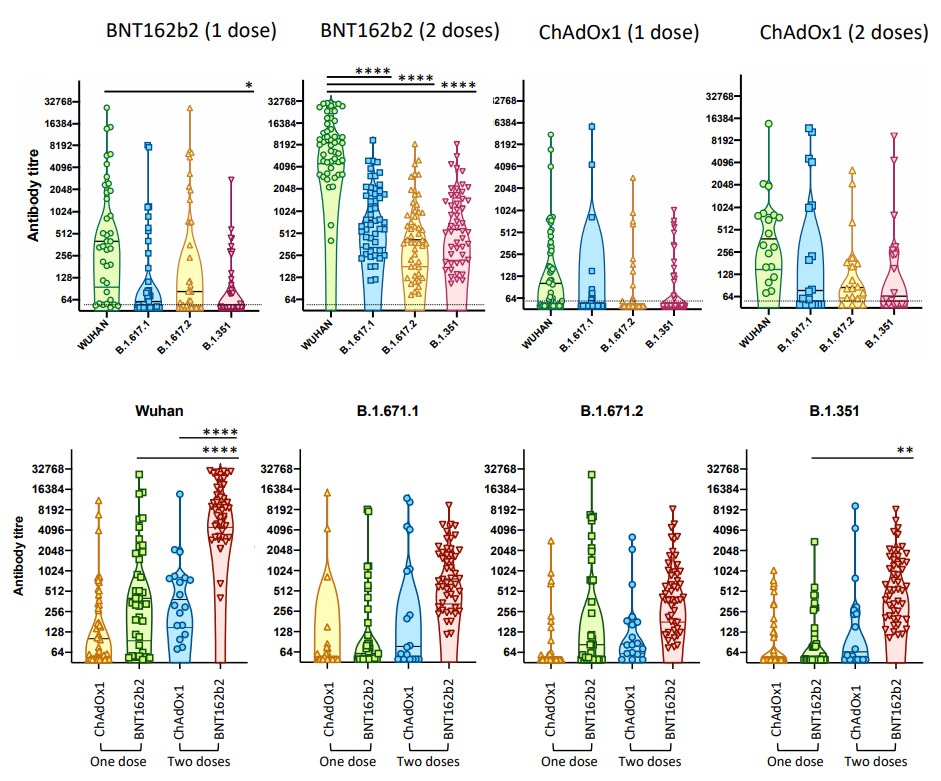
- Antibody titers produced by 2 doses of BNT162b2 (Pfizer/BioNTech) neutralized B.1.617.2, B.1.617.1, and B.1.351 variants 7.8-, 11.3-, and 9.6-fold less effectively than wild-type SARS-CoV-2 (Figure A).
- Differences in neutralization against variants produced by ChAdOx1 (Oxford/AstraZeneca) were not significant.
- Mean antibody titers against all Wuhan were significantly higher in individuals vaccinated with BNT162b2 than in those vaccinated with ChAdOx1 (Figure B).
Methods: Post-vaccination BNT162b2 or ChAdOx1 sera from 155 healthy individuals (≥18 years old) in the UK COVID-19 Deployed Vaccine Cohort Study (DOVE) were tested for neutralizing antibody production against SARS-CoV-2 spike protein-pseudotyped HIV for the indicated variants. Limitations: The average age of individuals vaccinated with ChAdOx1 was 15 years older than those vaccinated with BNT162b2, which could confound comparisons across the vaccine groups.
Implications: BNT162b2 and ChAdOx1 vaccines induced neutralizing antibodies may be less efficient at targeting the B.1.617.2 variant compared to wild-type SARS-CoV-2.
Figure:
Note: Adapted from Davis et al. Neutralizing antibody titers produced by individuals vaccinated with 1 dose of BNT162b2 (n = 37), 2 doses of BNT162b2 (n = 50), 1 dose of ChAdOx1 (n = 50), and 2 doses of ChAdOx1 (n=18) against Wuhan (wild-type) compared to 3 variants (B.1.617.1, B.1.617.2, or B.1.351) (Top row), and comparisons between ChAdOx1 and BNT162b2 by dose for each variant (bottom row). Violin plot indicates median and quartiles; horizontal bars at top indicate significant differences. Licensed under CC-BY-ND 4.0.
PEER-REVIEWED
Lottery-based incentive in Ohio and COVID-19 vaccination ratesexternal icon. Walkey et al. JAMA (July 2, 2021).
Key findings:
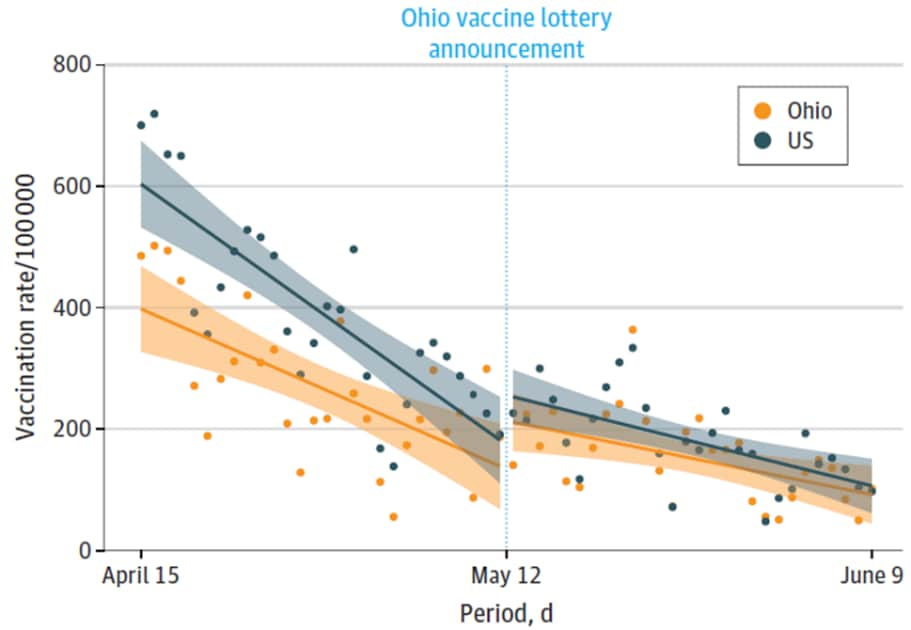
- Daily vaccination rates in adults decreased steadily in Ohio and the US from April to May 2021 (Figure):
- Ohio: −8/100,000 persons (95% CI −12 to −4).
- US: −14/100,000 persons (95% CI −18 to −11).
- After Ohio announced its vaccination lottery incentive on May 12, 2021, daily rates did not increase significantly in Ohio and changes were nearly identical to changes seen in the US as a whole (Figure):
- Ohio: +30/100,000 persons; (95% CI -53 to 113).
- US: +27/100,000 persons (95% CI -53 to 106).
Methods: Vaccination rates among adults >18 years in Ohio and the US from April 15–May 12, 2021 (pre-lottery) were compared with rates from May 13–June 9, 2021 (post-lottery). The days after 10 other states announced lotteries were omitted from US data. Limitations: There may be potential unmeasured confounding variables related to the dates of the lottery announcement; study may be under powered to detect small changes in vaccination rate.
Implications: There was no evidence that lottery-based incentives significantly increased vaccine uptake in adults in Ohio. Decrease in rate of vaccination decline may be related to expanding eligibility of the BNT162b2 (Pfizer/BioNTech) vaccine to 12–15 years on May 10, 2021.
Figure:
Note: Adapted from Walkey et al. Daily rates of adults receiving 1st vaccination dose for the US and Ohio before and after the May 12, 2021 Ohio vaccine lottery announcement (dashed blue line). Shaded areas are 95% CIs. Reproduced with permission from JAMA, 2021. Published online June 21, 2021. https://doi.org/10.1001/jama.2021.11048. Copyright© 2021 American Medical Association. All rights reserved.
Natural History of SARS-CoV-2 Infection
- Broseta et al. Humoral and cellular responses to mRNA-1273 and BNT162b2 SARS-CoV-2 vaccines administered to hemodialysis patients.external icon American Journal of Kidney Diseases (June 24, 2021). Among 175 hemodialysis patients, 97.7% developed an immune response after full vaccination with an mRNA vaccine. Lower antibody levels were found in older age groups and in patients on immunosuppresive treatment (n = 10).
- Van Oekelen et al. Highly variable SARS-CoV-2 spike antibody responses to two doses of COVID-19 RNA vaccination in patients with multiple myelomaexternal icon. Cancer Cell (June 28, 2021). Among 260 fully vaccinated multiple myeloma patients, 84.2% mounted measurable SARS-CoV-2 spike-binding IgG antibody levels at least 10 days after 2nd mRNA vaccine dose. The remaining patients were on anti-CD38 antibody-containing therapy (n = 24) or anti-BCMA bispecific antibody therapy (n = 13) at time of vaccination or had undergone anti-BCMA CAR-T therapy more than 3 months before vaccination (n = 4).
- Flaxman et al. Tolerability and immunogenicity after a late second dose or a third dose of ChAdOx1 nCoV-19 (AZD1222).external icon SSRN (Preprint; June 28, 2021). Median antibody titers after dose 2 of ChAdOx1 increased from 923 EU at 8–12 weeks to 3738 EU at 44–46 weeks. Among a subset of 75 participants, antibody titers further increased after a third dose of ChAdOx1 compared with 28 days after dose 2, including against Alpha (B.1.1.7), Beta (B.1.351) and Delta (B.1.617.2) variants in 45 participants. T-cell responses were also boosted after a 3rd dose.
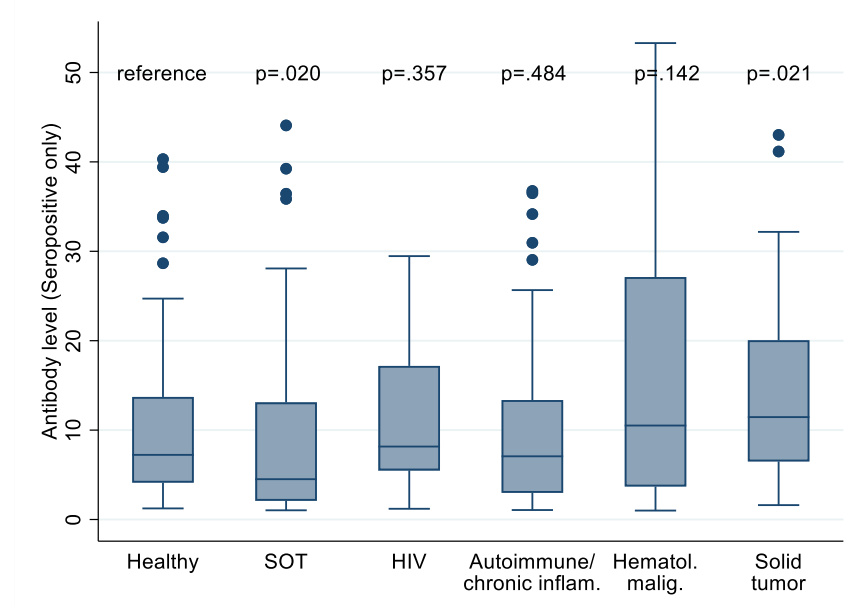
- Haidar et al. Immunogenicity of COVID-19 vaccination in immunocompromised patients: an observational, prospective cohort study interim analysis.external icon medRxiv (Preprint; June 30, 2021). After full SARS-CoV-2 vaccination, 37.2% of 183 solid organ transplant (SOT) patients, 54.7% of 75 hematological malignancies patients, 83.6% of 160 autoimmune disease patients, and 82.4% of 34 solid tumor patients were seropositive, significantly lower than the 98.1% of 107 healthcare worker controls; over 94% of 37 HIV patients were seropositive after vaccination. Among seropositive individuals, antibody levels were lower in SOT patients than healthy controls.
Note: Adapted from Haider et al. Comparison of antibody levels among seropositive immunocompromised patients compared to health healthcare workers. Whiskers denote 95% confidence intervals. SOT, solid organ tumor. HIV, human immunodeficiency virus. Used by permission of author.
- Apostolidis et al. Altered cellular and humoral immune responses following SARS-CoV-2 mRNA vaccination in patients with multiple sclerosis on anti-CD20 therapy.external icon medRxiv (Preprint; June 30, 2021). Published in Nature Medicine as Cellular and humoral immune responses following SARS-CoV-2 mRNA vaccination in patients with multiple sclerosis on anti-CD20 therapyexternal icon (September 14, 2021). Compared to all 10 healthy controls who generated both anti-pike and anti-RBD IgG responses after vaccination, of 20 multiple sclerosis patients on anti-CD20 therapy, 85% developed detectable anti-Spike IgG and 50% mounted detectable anti-RBD responses 25-30 days after 2nd vaccine dose. There was increased serologic response as time from last aCD20 infusion increased.
- Ramirez et al. SARS-CoV-2 breakthrough infections in fully vaccinated individualsexternal icon. medRxiv (Preprint; June 25, 2021). 2,551/68,428 random surveillance nasal-pharyngeal swabs collected on a university campus between February and May 2021 were from fully vaccinated individuals, 14 of whom tested positive by Nucleic acid amplification testing (0.55%, 95% CI: 0.30 – 0.92). The single B.1.617.2 (Delta) breakthrough was in a symptomatic female (56-65 years old) previously vaccinated with Ad26.COV2.S (Johnson & Johnson/Janssen) who had three Ct values <18.
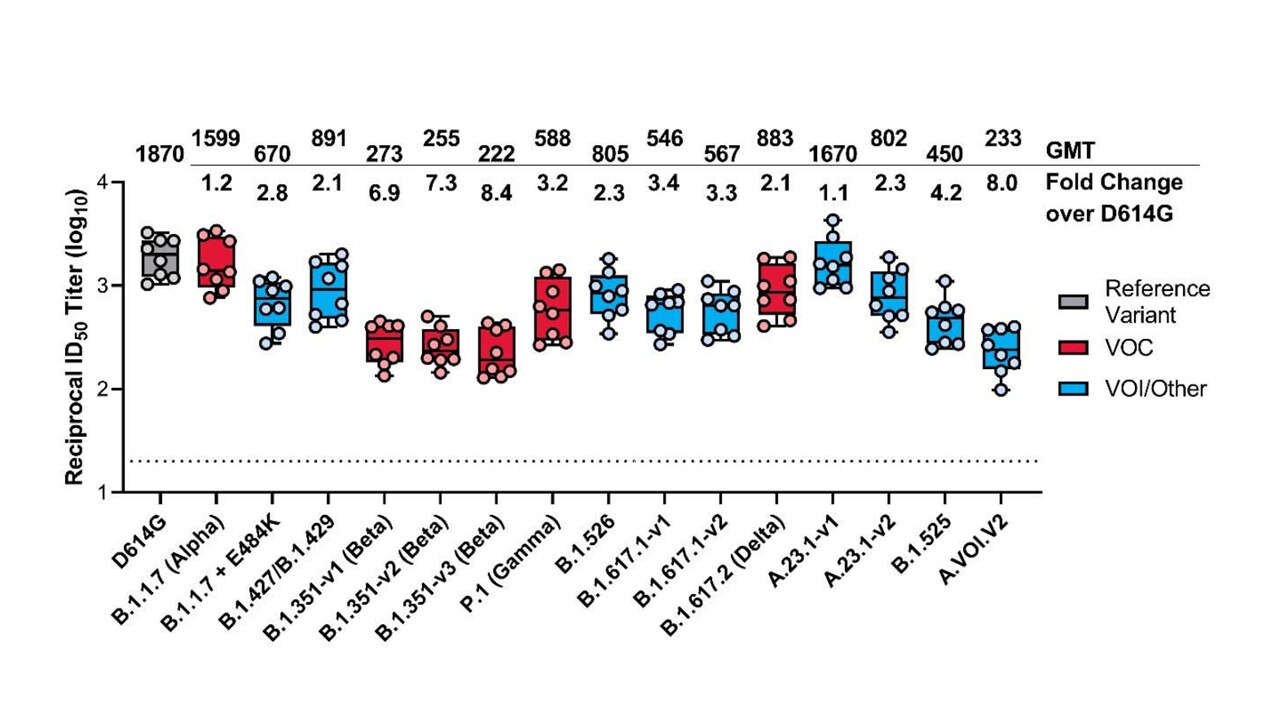
- Choi et al. Serum neutralizing activity of mRNA-1273 against SARS-CoV-2 variantsexternal icon. bioRxiv (Preprint; June 28, 2021). Published in Journal of Virologyexternal icon (November 9, 2021). One week after 2nd dose of mRNA-1273 (Moderna), sera from 8 individuals showed reduced neutralization (range 1.2- to 8.4-fold) for SARS-CoV-2 variants of concern compared to wild-type.
Note: Adapted from Choi et al. Reciprocal neutralizing titers on the pseudovirus neutralization assay at a 50% inhibitory dilution (ID50) for SARS-CoV-2 variants of interest (VOIs) and variants of concern (VOCs). Boxes and horizontal bars denote the interquartile range (IQR) and the geometric mean titer. Whisker end points are equal to the maximum and minimum values below or above the median at 1.5 times the IQR. The fold change over D614G for each variant is shown below the long solid line and GMT above the line. Used by permission of author.
Prevention, Mitigation, and Intervention Strategies
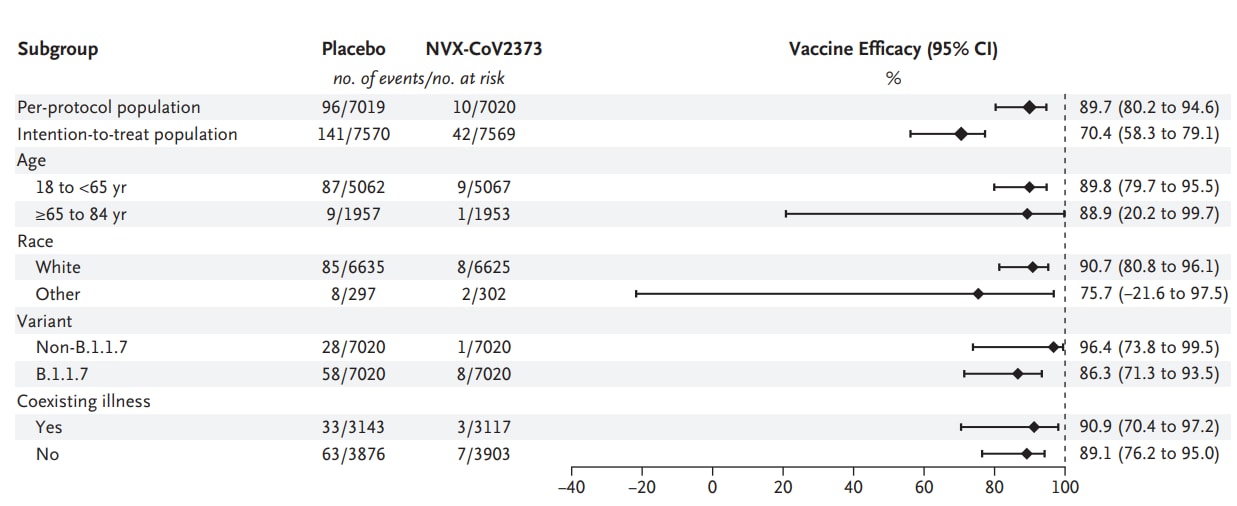
- Heath et al. Safety and efficacy of NVX-CoV2373 COVID-19 vaccine.external icon NEJM (June 30, 2021). Two-dose regimen of NVX-CoV2373 (Novavax) provided 89.7% protection overall, with high efficacy demonstrated against the B.1.1.7 variant in a UK-based 33 site trial with 14,039 participants conducted between September 28 and November 28, 2020.
Note: Adapted from Heath et al. Efficacy of the NVX-CoV2373 vaccine in preventing COVID-19 in various subgroups. From the New England Journal of Medicine, Heath et al., Safety and efficacy of NVX-CoV2373 COVID-19 vaccine. June 30, 2021, online ahead of print. Copyright © 2021 Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.