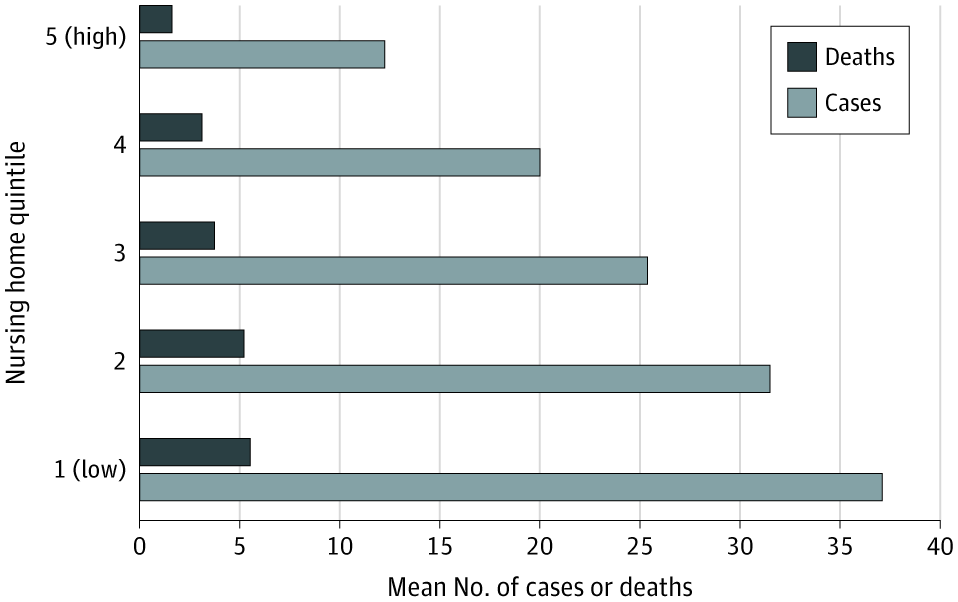COVID-19 Science Update released: February 26, 2021 Edition 78

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
Convergence of COVID-19 and chronic air pollution risks: racial/ethnic and socioeconomic inequities in the US.external icon Chakraborty. Environmental Research (February 2021).
Key findings:
- Counties with the most COVID-19 infections and significantly higher hazardous air pollutants (HAPs) have disproportionately higher numbers of non-Hispanic Black, socioeconomically disadvantaged, and uninsured residents than all other US counties.
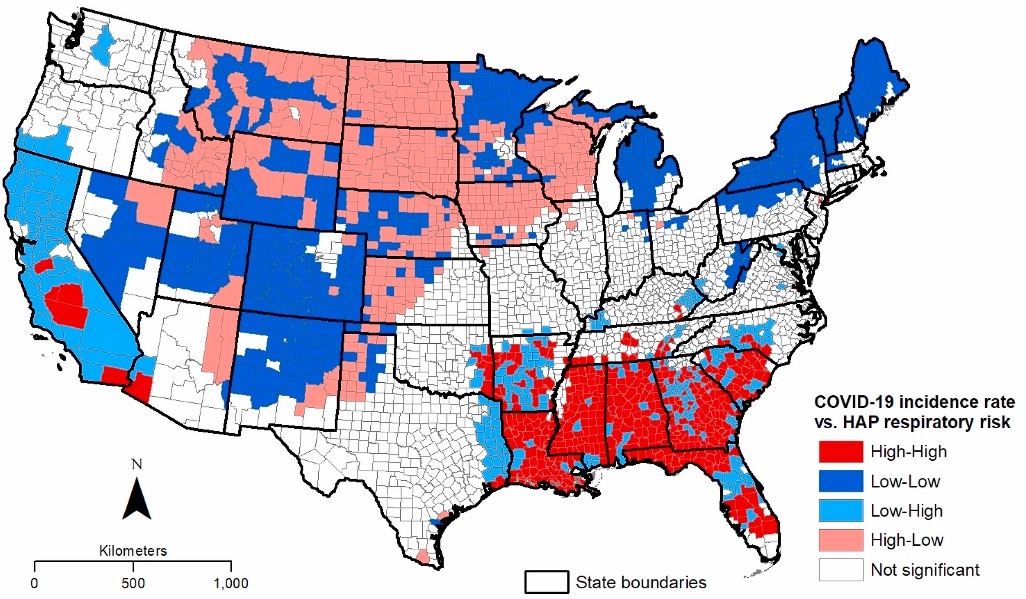
- There were significantly higher positive associations between COVID-19 and HAP respiratory risk in 14% (422) of US counties, all located in the southeastern US and southern California (High-High in Figure).
Methods: COVID-19 incidence rates were estimated by county (n = 3,108) based on 10,355,623 cases from January 22–November 13, 2020 across the continental US. These data were linked to respiratory risk data from EPA and analyzed to identify geographic clusters based on spatial associations. Limitations: Statistical analyses does not include individual level data and utilized respiratory risk data from 2014 may not represent current conditions or exposure risks.
Implications: The convergence of COVID-19 prevalence and high air pollution, which increases respiratory health risk, in communities where socially disadvantaged persons are more likely to reside, highlights the need to address social disparities through policy and other mitigation strategies.
Figure:
Note: Adapted from Chakraborty et al. COVID-19 incidence rate vs hazard air pollutant (HAP) respiratory risk by county. Local Indicators of Spatial Association (LISA) identify geographic clusters of counties based on the statistical association between COVID-19 incidence and the respiratory hazard index for HAP exposure. The categories of spatial association are High-High and Low-Low (positive associations); Low-High and High-Low (negative associations). Reprinted from Environmental Research, Chakraborty, Convergence of COVID-19 and chronic air pollution risks: racial/ethnic and socioeconomic inequities in the US, Copyright (2021), with permission from Elsevier.
Estimating the unknown: greater racial and ethnic disparities in COVID-19 burden after accounting for missing race and ethnicity data.external icon Labgold et al. Epidemiology (March 2021).
Key findings:
- When comparing complete case and imputed results, SARS-CoV-2 notification rates (per 1000 persons) among non-Hispanic Black persons increased 1.3-fold (16.0 vs. 23.0 per 1,000). Among Hispanic persons, notification increased 1.6-fold (22.0 vs. 36.0 per 1,000).
- Among non-Hispanic Black persons, compared with complete cases, imputed analyses showed lower SARS-CoV-2 related hospitalization (17.0% vs. 12.0% respectively) and fatality (4.6% vs. 3.1%, respectively) prevalence.
Methods: Case reports (n = 19,623) of SARS-CoV-2 infection reported in Fulton County, Georgia from March 2, 2020—August 18, 2020 were used to assess the impact of missing race and ethnicity data. Case reports (notification) were considered complete if they contained race and/or ethnicity. The Bayesian Improved Surname Geocoding method and quantitative bias analysis were used to impute race and/or ethnicity data in 36% of case reports with missing information (n = 7,131). Limitations: Results not generalizable to the US population; imputation methods limited to Black, Hispanic, Asian, White, and Other race and ethnicity categories; algorithm’s imputation accuracy varied by race/ethnicity group.
Implications: National estimates that exclude COVID-19 cases with missing race/ethnicity data may be leading to inaccurate estimates of notification, morbidity, and mortality among non-Hispanic Black persons.
Factors associated with racial differences in deaths among nursing home residents with COVID-19 infection in the USexternal icon. Gorges et al. JAMA (February 10, 2021)
Key findings:
- Deaths were highest (mean 5.6, SD 9.2) in facilities with the lowest proportion of non-Hispanic White residents (quintile 1) and lowest (mean 1.7, SD 4.8) in facilities with the highest proportions of White residents (quintile 5) (Figure).
- There were 3.9 (SE 0.2) more deaths on average per facility in quintile 1 than quintile 5
- Adjustment for number of certified beds and for county-level COVID-19 prevalence reduced the mean difference between these 2 quintiles to 2.2 (SE 0.2) and 1.0 (SE 0.2)
- Nursing homes in quintile 1, compared with those in quintile 5, had more confirmed COVID-19 cases per capita (mean [SD] 12.1 [8.9] vs. 23.2 [10.7] cases per 1000 people) and more residents with Medicaid coverage (mean [SD] 53.5% [21.0%] vs 69.7% [20.8%]).
Methods: Cross-sectional study of confirmed or suspected COVID-19 cases and deaths reported by 13,312 nursing homes between January 1, 2020 and September 13, 2020. Modeled marginal effects of quintile based on percentage of non-Hispanic White nursing home residents on number of deaths per facility, sequentially adjusting for bed number, case mix, other facility characteristics, and county-level COVID-19 cases. Limitations: Limited individual-level COVID-19 case and death data; data did not allow for racial classifications other than non-Hispanic White, non-Hispanic Black, and Hispanic; nursing homes were not required to report COVID-19 case and death counts prior to mid-May 2020.
Implications: The COVID-19 pandemic has highlighted disparities between nursing homes. Policymakers should promote and enforce quality standards across nursing homes to assure equity in care.
Figure:
Note: Adapted from Gorges et al. Unadjusted total (confirmed and suspected) COVID-19 cases and deaths among residents by nursing home racial composition quintile, based on the percentage of White residents, with quintile 1 indicating 0%−59.73%, quintile 2 indicating 59.75%−80.99%, quintile 3 indicating 81.00%−91.77%, quintile 4 indicating 91.78−97.32%, and quintile 5 indicating 97.33%−100.00%. Licensed under CC BY.
Racial disparities in excess all-cause mortality during the early COVID-19 pandemic varied substantially across states.external icon Polyakova et al. Health Affairs (February 1, 2021).
Key findings:
- Nationwide, age-, sex-, and state-adjusted excess all-cause mortality during April 2020 was 6.8 per 10,000 for non-Hispanic Black, 4.3 for Hispanic, 2.7 for Asian, and 1.5 for non-Hispanic White persons.
- Non-Hispanic Black and Hispanic persons experienced higher adjusted excess mortality than White persons in nearly every state, with substantial variation by state (Figures 1 and 2).
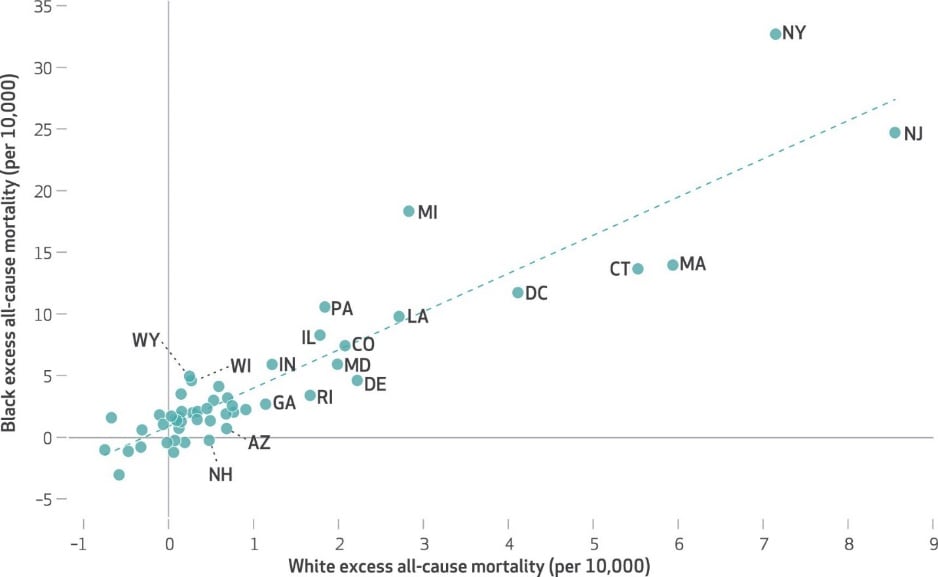
- Despite similar excess mortality among non-Hispanic White persons (2.8 and 2.7 per 10,000, respectively), Michigan had markedly greater excess mortality compared with Louisiana among non-Hispanic Black persons (18.3 and 9.8 per 10,000, respectively).
Methods: Analysis of individual-level demographic data from the US census (from January 2011 through April 2020) to estimate state-specific age- and sex-adjusted excess all-cause mortality in April 2020 by race and ethnicity. Limitations: Potential selection bias given some people were excluded for missing data; excluded persons born after 2010 as race/ethnicity data were not available.
Implications: While geographic variation in overall excess mortality likely reflects the timing of COVID-19’s spread through different U.S. regions, further investigation is needed to understand potential factors driving dramatic variation in racial and ethnic disparities across states and to address substantially increased excess mortality among non-Hispanic Black and Hispanic persons. A recent reportpdf icon noted declines in life expectancy in the first half of 2020, the lowest level since 2006, with the largest decline among non-Hispanic Black persons.
Figure 1:
Note: Adapted from Polyakova et al. Association of sex- and age-adjusted all-cause excess mortality in April 2020 by state among non-Hispanic Black persons versus non-Hispanic White persons. The trend line marks the line of best fit for the relationship between non-Hispanic White and non-Hispanic Black excess mortality by state. Used by permission of publisher.
Figure 2:
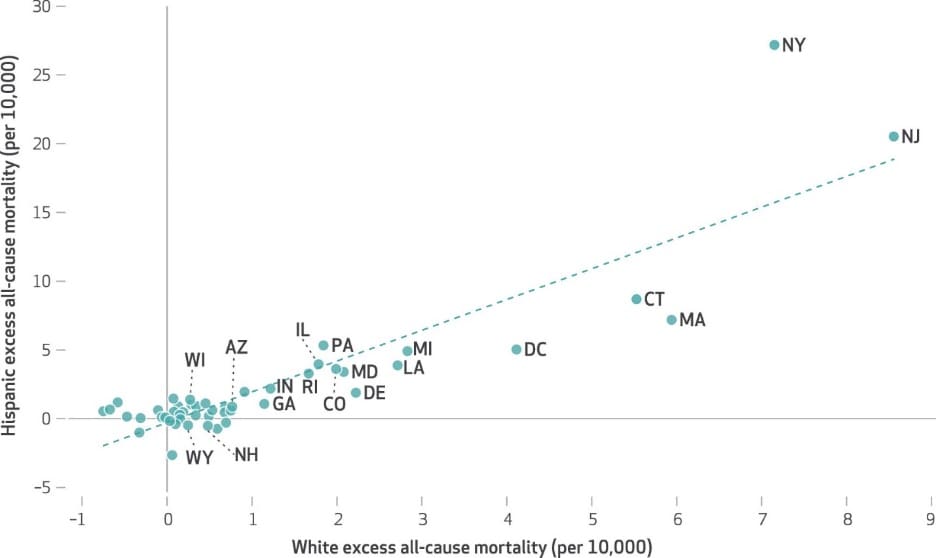
Note: Adapted from Polyakova et al. Association of sex- and age-adjusted all-cause excess mortality in April 2020 by state among Hispanic versus non-Hispanic White persons. The trend line marks the line of best fit for the relationship between non-Hispanic White and Hispanic excess mortality by state. Permission request in process.
Association of social and economic inequality with coronavirus disease 2019 incidence and mortality across US counties.external icon Liao et al. JAMA Network Open (January 20, 2021).
Key findings:
- A 1% increase in a county’s income inequality was associated with increased COVID-19 incidence (aRR, 1.02: 95% CI 1.01-1.03) and mortality (aRR, 1.03: 95% CI 1.01-1.05).
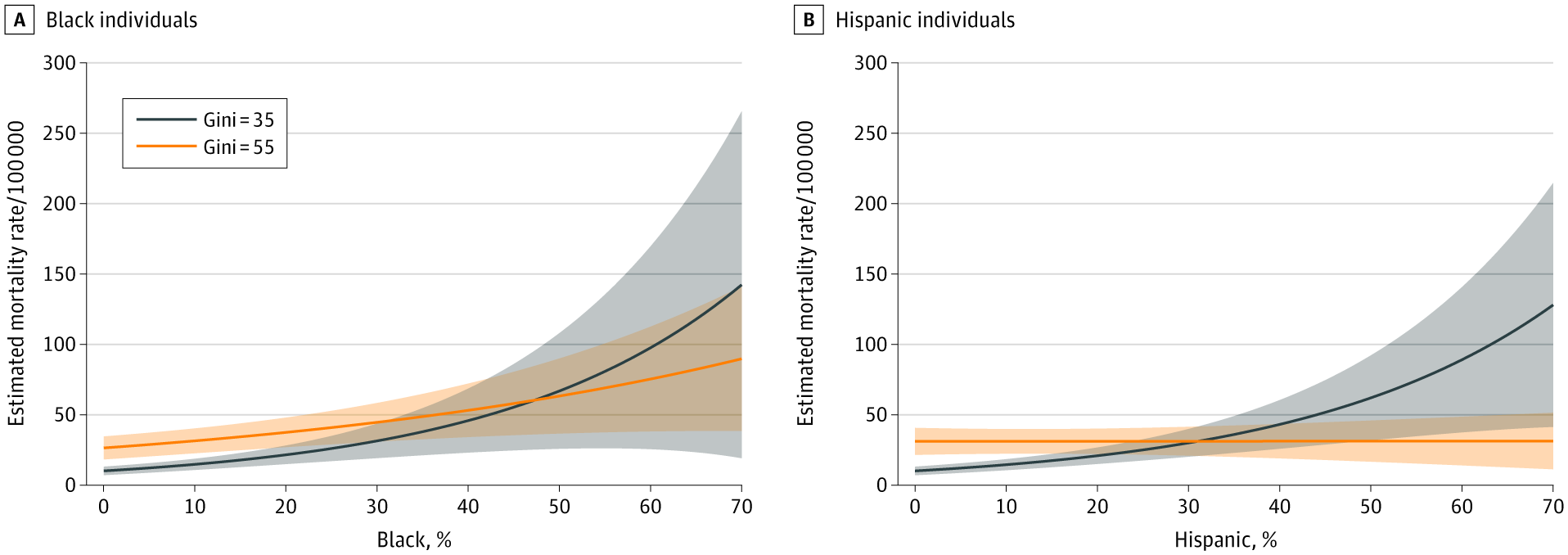
- In communities with both lower (Gini = 35) and higher (Gini = 55) income inequality, mortality was positively associated with Black composition but there was no association between mortality and Hispanic composition in communities with higher income inequality (Figure).
Methods: Cross-sectional ecological analysis of COVID-19 incidence and mortality in 3,141 US counties using population data from multiple data sources during the first 200 days (January 22–August 8, 2020) of the pandemic. Income inequality was measured using the Gini index. Analysis was conducted with multi-level negative binomial regression. Limitations: Incidence may vary by testing availability, which was not assessed.
Implications: Income inequality should be considered as a driver of the disproportionate burden of COVID-19 afflicting minority communities. However, irrespective of race/ethnic composition, income inequality in communities is harmful to population health.
Figure:
Note: Adapted from Liao et al. COVID-19 mortality rate predictions by racial/ethnic composition and income inequality with their interaction and controlling for covariates including state-level political variates (term-limited governor, political party of governor, and Medicaid expansion under the Affordable Care Act). Gini index ranges from 0 (perfect equality) to 100, (perfect inequality). Mortality at high levels of income inequality (Gini = 55), mortality at low levels of income inequality (Gini = 35). Licensed under CC BY.
PREPRINTS (NOT PEER-REVIEWED)
Racial and ethnic disparities in years of potential life lost attributable to COVID-19 in the United States: an analysis of 45 States and the District of Columbia.external icon Xu et al. medRxiv (January 31, 2021). Published in International Journal of Environmental Research and Public Healthexternal icon (March 12, 2021).
Key findings:
- Over 925,058 years of potential lives lost (YPLL) before age 75 were attributable to COVID-19, corresponding to 301,679 deaths as of December 30, 2020.
- Substantial racial/ethnic disparities in YPLL across states were noted with non-Hispanic Black and Hispanic persons experiencing disproportionately high YPLL, while non-Hispanic White persons experienced disproportionately low YPLL.
Methods: Analyzed US national COVID-19 mortality data stratified by race/ethnicity and age from the National Center for Health Statistics through December 30, 2020 to estimate YPLL attributable to COVID-19 at the state level. 2019 data from CDC WONDER were used to standardize estimates by age. Monte Carlo simulation was used to estimate age-adjusted mortality rates and quantify uncertainty. Limitations: Lag-time in reporting death data, unknown race/ethnicity, suppression of death count for values between 1 and 9.
Implications: Substantial variation between states in the magnitude of the estimated racial/ethnic disparities in COVID-19 mortality suggests that they are driven in part by social determinants of health which also vary by state.
PEER-REVIEWED
Feasibility of separate rooms for home isolation and quarantine for COVID-19 in the United States.external icon Sehgal et al. Annals of Internal Medicine. (January 2021).
Key findings:
- More than 1 in 5 US homes (which include about a quarter of all Americans) lack sufficient space and/or plumbing facilities to comply with recommendations to isolate or quarantine to limit household spread of COVID-19.
- Native American and Hispanic persons had 2.7 and 3.3 times higher odds respectively, and non-Hispanic Black and Asian persons had 1.7 times higher odds of occupying units unsuitable for isolation or quarantine relative to non-Hispanic White persons.
Methods: Data collected by the US Census Bureau from the nationally representative 2017 American Housing Survey (n = 57,984 dwellings) with a response rate of 80.5%, were analyzed using descriptive statistics and logistic regression. Limitations: Unable to assess individual’s ability to optimally isolate and quarantine, the direct impact of prevention measures (face masks, physical distancing, surface disinfection), and size of rooms.
Implications: These findings highlight the potential benefit of using underutilized hotels for isolation or quarantine which in turn might decrease COVID-19 transmission in vulnerable communities as well as reduce medical costs, economic damage from work absenteeism, and job loss.
Assessment of the inclusion of racial/ethnic minority, female, and older individuals in vaccine clinical trials.external icon Flores et al. JAMA Network Open (February 19, 2021).
Key findings:
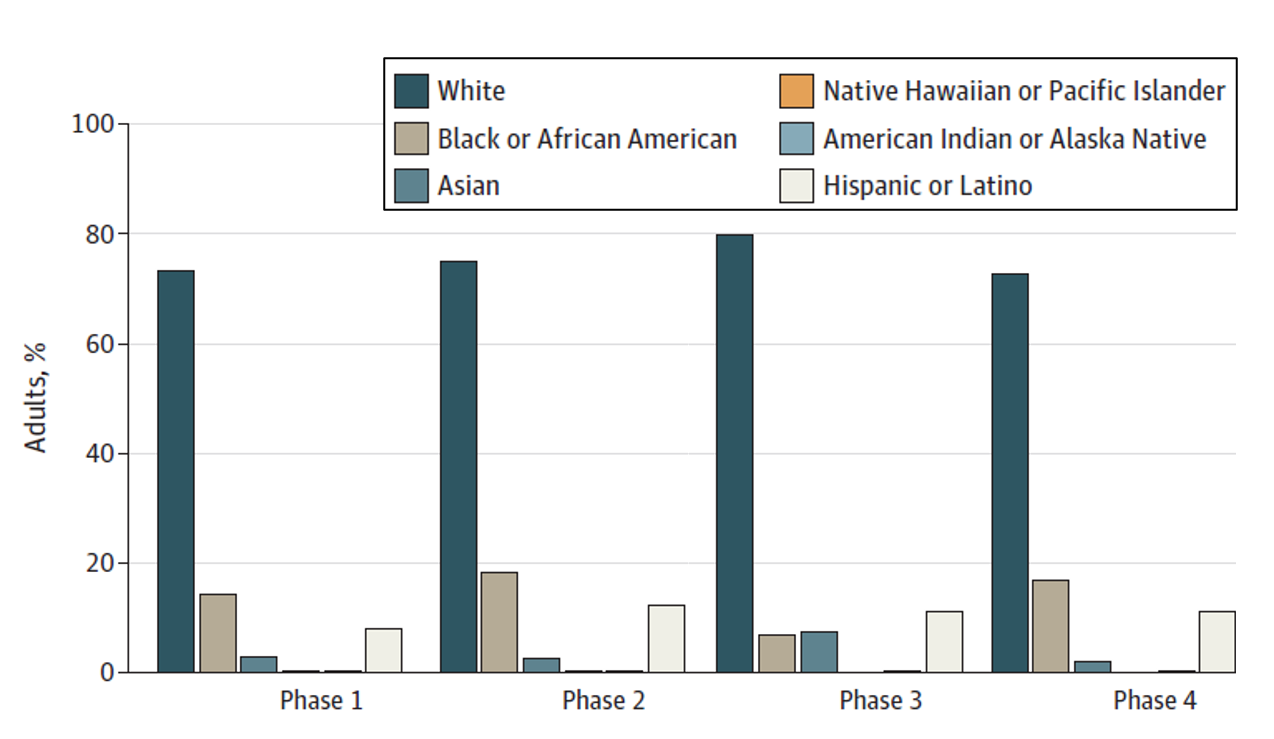
- In adult vaccine trials, African American persons (10.6% [95% CI, 10.2-11.0] and American Indian or Alaska Native persons (0.4% [95% CI 0.3%-0.5%] were underrepresented overall and by trial phase (Figure).
- White persons (77.9%; 95% CI 77.4%-78.4%) and female participants (56.0%; 95% CI 55.7-56.2) were overrepresented and persons >65 years old (12.1%; 95% CI 12.0%-12.3%) were underrepresented.
- Among the limited number of trials that reported ethnicity data (34.3%), Hispanic persons were also underrepresented (11.6%; 95% CI 11.1%-12.0%).
Methods: Cross-sectional study using data from 230 vaccine trials with 219,555 participants from July 1, 2011–June 30, 2020 were compared with US census data from 2011 and 2018 for race/ethnicity, gender, and age overall and by trial phase. Limitations: Many trials did not meet federal reporting requirements and had missing race (41.7%) and ethnicity (65.7%) data.
Implications: Racial and ethnic minority groups and older persons, who experience disproportionate burden of infectious diseases such as COVID-19, are underrepresented in vaccine trials. A significant amount of missing race and ethnicity data underscores the need for these data to truly understand representation. Equitable representation in these trials may have downstream effects of addressing vaccine hesitancy in these groups, leading to improved vaccination rates.
Figure:
Note: Adapted from Flores et al. Proportion of participants by race (White, Black or African American, Asian, Native Hawaiian or Pacific Islander, American Indian or Alaska native) or ethnicity (Hispanic or Latino) by phase among adult vaccine trials. Licensed under CC BY.
Understanding drivers of COVID-19 vaccine hesitancy among Blacks.external icon Momplaisir et al. Clinical Infectious Diseases (February 9, 2021).
Key findings:
- COVID-19 vaccine hesitancy was high because of safety concerns due to rushed vaccine development process and limited data on short- and long-term side effects, historic racial injustice towards African American persons, and mistrust in the medical community.
- Facilitators toward getting the vaccine included reassuring record of vaccine safety and recommendation by a trusted health provider.
Methods: 4 virtual focus groups (n = 24 participants) conducted among African American barbershop and salon owners living in areas with elevated COVID-19 prevalence in July and August 2020. Attitudes, beliefs, and norms around COVID-19 vaccines were assessed. Limitations: Convenience sample; small sample size; current vaccine perceptions may differ as vaccines have now been shown to be efficacious.
Implications: Vaccine mistrust might be a substantial barrier against COVID-19 vaccine uptake among African American persons. Recommendation by a trusted health provider was a key facilitator of vaccine uptake; both Bajaj et alexternal icon. and Opel et al.external icon highlight the importance of the physician-patient relationship, particularly clinicians of the same race, in outcomes for African American persons. Improved public health messaging from trusted messengers, particularly around vaccine safety, might also increase vaccine acceptance.
PEER-REVIEWED
The relationship between social determinants of health and racial disparities in COVID-19 mortality.external icon Dalsania et al. Journal of Racial and Ethnic Health Disparities (January 5, 2021).
Key findings:
- Counties in the highest quartile compared with the lowest quartile of COVID-19 deaths had a higher proportion of Black residents (22.7% vs. 5.0%, respectively).
- Less privileged counties were associated with increased COVID-19 death rates by 67.5% (95% CI 35.9%-106.6%) compared with the most privileged counties.
Methods: Case and death rates were estimated using US county-level data (n = 2,026) from all states and DC, for January 22–October 28, 2020, from the Johns Hopkins University Center for Systems Science and Engineering. Final analysis included % Black residents, 6 social determinants of health variables: % uninsured; insurance status; % low birthweight; % adults without high school diploma; incarceration rate; and % households without internet, and an index of economic privilege. Limitations: Excluded 805 (28%) counties due to <5 deaths or incomplete data; limitations of COVID-19 mortality data due to inaccurate cause-of-death determination early in the outbreak.
Implications: Findings from this study suggest that COVID-19 racial disparities are due to social constructs and policies. In a related study, Saini et al.external icon reports that a mix of environmental, social, and biological factors may be at fault for racial differences in COVID-19 outcomes. To eliminate disparities related to race and social inequality, a focus on less privileged communities is needed, especially those that have limited access to internet and consistently low education rates.
Detection, Burden, and Impact
- Kidd et al. S-variant SARS-CoV-2 lineage B1.1.7 is associated with significantly higher viral loads in samples tested by ThermoFisher TaqPath RT-qPCR.external icon The Journal of Infectious Diseases (February 13, 2021).The SARS-CoV-2 variant, B.1.1.7, has an identifiable S-gene target failure and typically has low Ct values and thus, higher viral loads; this might explain the higher infectivity rates and rapid spread exhibited by this variant.
- Boyarsky et al. Safety of the first dose of SARS-CoV-2 vaccination in solid organ transplant recipients.external icon Transplantation (February 4, 2021). Among 187 solid organ transplant recipients who received the mRNA COVID-19 vaccine, mostly mild local reactions were noted and only two participants reported development of a new infection (acute-on-chronic pouchitis and influenza A) requiring treatment; transplant rejection was not seen in early-follow-up.
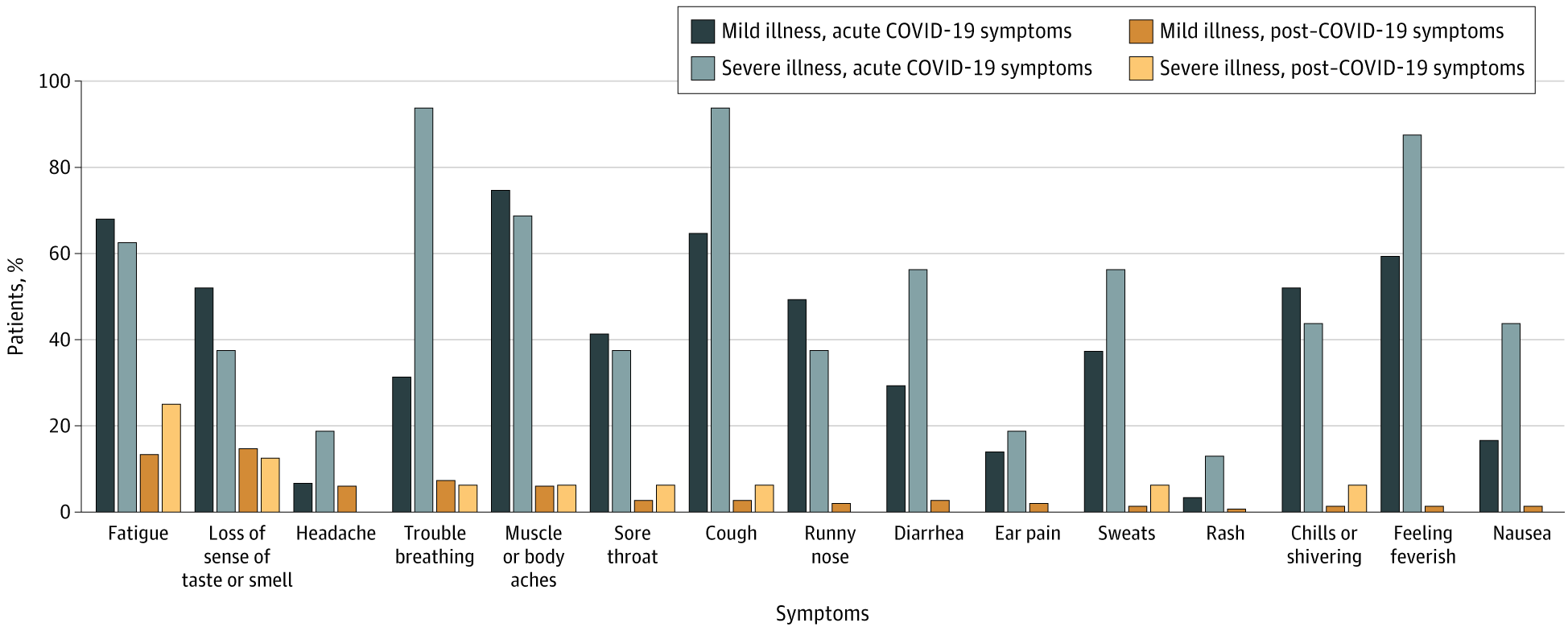
- Logue et al. Sequelae in adults at 6 months after COVID-19 infection.external icon JAMA (February 19, 2021). In a longitudinal prospective cohort study of adults with RT-PCR-confirmed SARS-CoV-2 infection, the most common persistent symptoms (i.e. orange and yellow bars below) were fatigue (24/177 [13.6%]) and loss of smell or taste (24/177 [13.6%]).
Figure.
Note. Adapted from Logue et al. COVID-19 symptoms by severity of illness and timing of symptoms. Licensed under CC BY.
Natural History of SARS-CoV-2 Infection
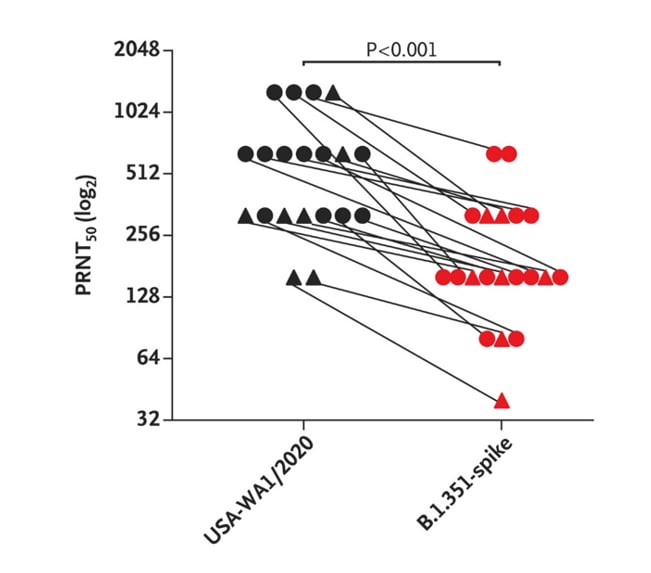
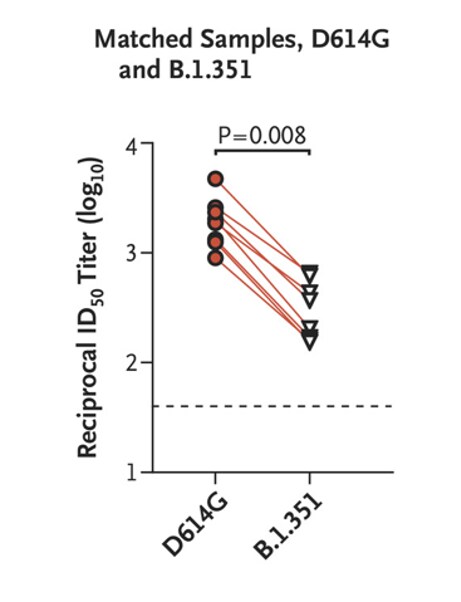
- Liu et al. Neutralizing activity of BNT162b2-elicited serum — preliminary report.external icon NEJM (February 17, 2021). A two-thirds reduction in neutralization of sera from persons who had received the BNT162b2 (Pfizer) vaccine was noted in virus with 1.351-spike mutations compared with other strains of the SARS-CoV-2.
Figure.
Note: Adapted from Liu et al. Results of 50% plaque reduction neutralization testing (PRNT50) with the use of 20 samples obtained from 15 trial participants 2 weeks (circles) or 4 weeks (triangles) after the administration of the second dose of the BNT162b2 vaccine. Results are shown for serum neutralization of USA-WA1/2020 and B.1.351-spike virus. Samples that have measurably different PRNT50 values against USA-WA1/2020 and mutant viruses are indicated by solid lines. Each PRNT50 data point is the geometric mean. From NEJM, Liu et al., Neutralizing Activity of BNT162b2-Elicited Serum — Preliminary Report. Copyright © (2021) Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
- Hodcroft et al. Emergence in late 2020 of multiple lineages of SARS-CoV-2 spike protein variants affecting amino acid position 677.external icon medRxiv (Preprint, February 21, 2021). Genomic surveillance programs in New Mexico and Louisiana detected a new SARS-CoV-2 variant with a Q677P substitution in the spike protein that is becoming more prominent in the US; phylogenetic analysis showed independent evolution of 6 distinct lineages of Q667H in addition to Q677P, suggesting a fitness advantage.
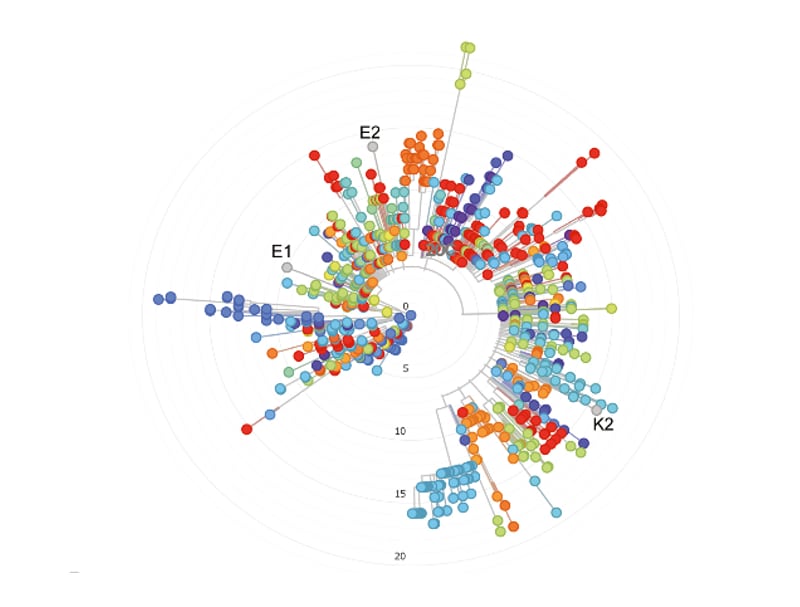
- Adrielle dos Santos et al. Recurrent COVID-19 including evidence of reinfection and enhanced severity in thirty Brazilian healthcare workers.external icon Journal of Infection (February 13, 2021). RT-PCR-confirmed COVID-19 recurrence in 33 people was associated with reduced antibody response during initial infection; in one patient (E), viral sequencing from the first and second episode revealed infection with different clades (lineages B.1 and B.1.80) which confirmed re-infection.
Figure.
Note. Adapted from Adrielle dos Santos et al. Phylogenetic analysis of viral genomes recovered from individuals with recurrent COVID-19. This phylogenetic tree has strains derived from Brazilian individuals. Patients E and K rendered full-length SARS-CoV-2 sequences. E1 and E2 represent samples of the patient E at first and second event of COVID-19, respectively. K2 represents the sample of patient K during the second episode of COVID-19. Licensed under CC BY-NC-ND 4.0.
Prevention, Mitigation, and Intervention Strategies
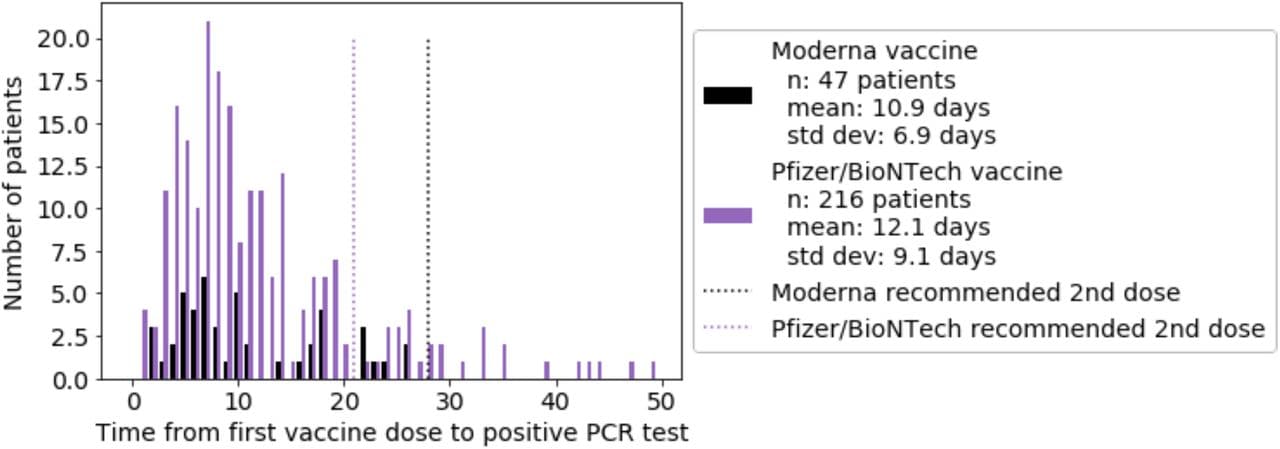
- Pawlowski et al. FDA-authorized COVID-19 vaccines are effective per real-world evidence synthesized across a multi-state health system.external icon medRxiv (Preprint, February 18, 2021). Published in Medexternal icon (June 29, 2021). Retrospective analysis of data from 62,138 persons who were vaccinated with BNT162b2 or mRNA-1273 between December 1, 2020 and February 8, 2021, found that real-world vaccine efficacy was 88.7% (95% CI: 68.4-97.1) after the second dose; 98% of all 263 SARS-CoV-2-positive vaccinated persons tested positive for SARS-CoV-2 before their second dose.
Figure.
Note. Adapted from Pawlowski et al. Distribution of the time from first vaccine dose to first positive PCR test, for the patients with at least one positive PCR test following vaccination by vaccine: mRNA-1273 (Moderna vaccine) and BNT162b2 (Pfizer/BioNTech vaccine). Dotted lines indicate the recommended time for the second vaccine dose for mRNA-1273 (28 days) and BNT162b2 (21 days). Used by permission of authors.
- Wu et al. Serum neutralizing activity elicited by mRNA-1273 vaccine — preliminary report.external icon NEJM (February 17, 2021). Sera obtained from persons who received the mRNA-1273 (Moderna) vaccine showed a reduction in titers of neutralizing antibodies by a factor of 6.4 against the full panel of mutations in B.1.351 compared with D614G.
Figure.
Note: Adapted from Wu et al. Serum samples obtained from participants who received the mRNA-1273 vaccine in a phase 1 trial were collected on day 36 (7 days after the participants received the second dose of the vaccine). The dots indicate the results from serum samples of the individual participants, the diamonds the same samples tested against the B.1.351 variant, and the horizontal dashed line the lower limit of quantification. The reciprocal neutralizing titers on the pseudovirus neutralization assay at a 50% inhibitory dilution (ID50) are shown. From NEJM, Wu et al., Serum neutralizing activity elicited by mRNA-1273 vaccine — preliminary report. Copyright © (2021) Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
Protection in Healthcare and Non-Healthcare Work Settings
- Courtney et al. Hydrating the respiratory tract: an alternative explanation why masks lower severity of COVID-19.external icon Biophysical Journal (February 11, 2021). Facemasks strongly increase the effective humidity of inhaled air which benefits the immune system by hydrating the respiratory epithelium and promoting muco-ciliary clearance of pathogens from the lungs, both before and after infection has occurred, and thus, mitigate disease severity.
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.