COVID-19 Science Update released: February 5, 2021 Edition 75

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
Antigen-based testing but not real-time polymerase chain reaction correlates with severe acute respiratory syndrome coronavirus 2 viral culture.external icon Pekosz et al. Clinical Infectious Diseases (January 20, 2021).
Key findings:
- The BD Veritor antigen test had a higher positive predictive value (PPV) (90.0%, 95% CI 76.3%-97.6%) than the Quidel Lyra RT-PCR SARS-CoV-2 test (73.7%, 95% CI 60.8%-85.3%) relative to positive viral culture.
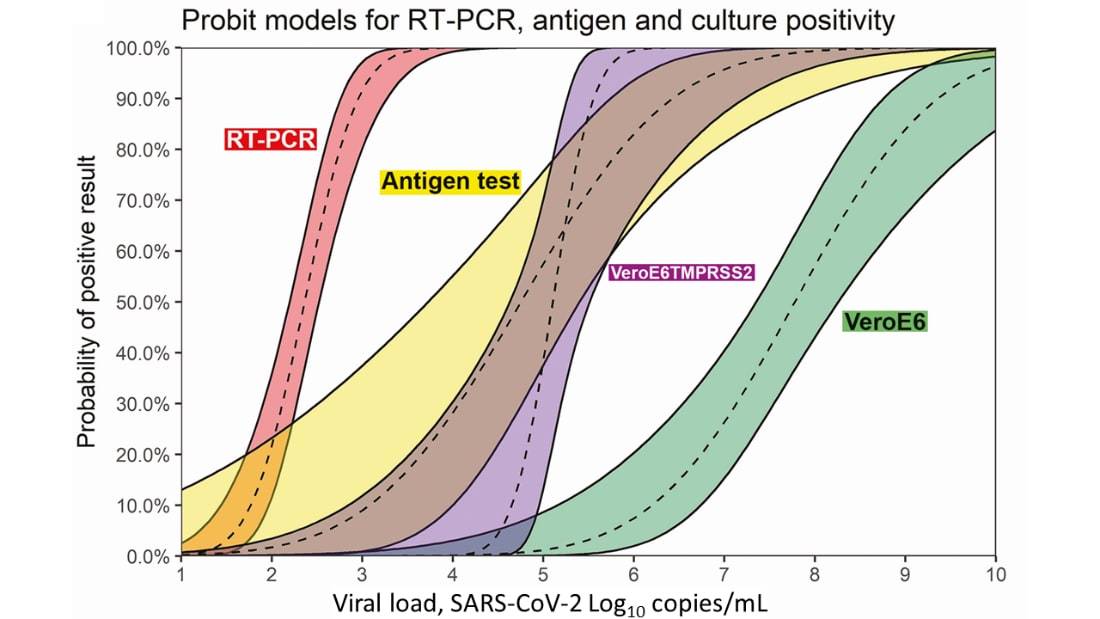
- Viral culture using VeroE6TMPRSS2 cells, which are susceptible to infection by influenza and coronaviruses, correlated better with antigen tests compared with VeroE6 cells (Figure).
Methods: RT-PCR and antigen tests were compared with SARS-CoV-2 viral cultures from 38 adult patients sampled within 7 days of symptom onset across 21 US localities in June 2020. Probability of positivity and viral loads were fit with probit models for each testing method. Limitations: Correlations may be valid only for samples taken within 7 days from symptom onset; small sample of symptomatic adults.
Implications: Point-of-care antigen tests might minimize the spread of SARS-CoV-2 by identifying infectious adults in areas of high community transmission.
Figure.
Note: Adapted from Pekosz et al. Modelled probability distributions of each SARS-CoV-2 test type, RT-PCR, antigen, and viral cultures (VeroE6TMPRSS2 and VeroE6), across log-transformed viral load. As viral load increases, the probability of any test producing a positive result increases. Licensed under CC BY-NC-ND 4.0.
PREPRINT (NOT PEER-REVIEWED)
Predictive power of SARS-CoV-2 wastewater surveillance for diverse populations across a large geographical range.external icon Melvin et al. medRxiv (January 25, 2021). Published in Scientific Reports as A novel wastewater-based epidemiology indexing method predicts SARS-CoV-2 disease prevalence across treatment facilities in metropolitan and regional populationsexternal icon (November 1, 2021).
Key findings:
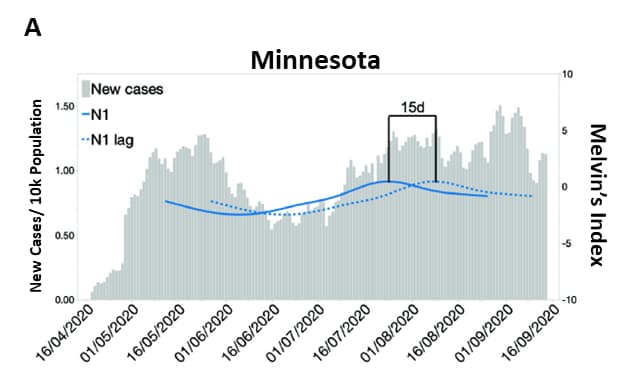
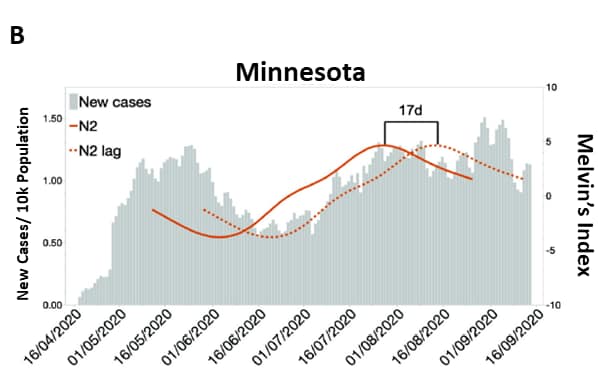
- In Minnesota, wastewater SARS-CoV-2 RNA levels, using RT-PCR to amplify 2 nucleocapsid gene targets (N1 and N2), predicted new clinical cases with a lag of 15 days for N1 (r = 0.73, p <0.001) and 17 days for N2 (r = 0.77, p <0.001) (Figure).
Methods: Compared Minnesota Department of Health COVID-19 case data with indexed SARS-CoV-2 RNA levels in municipal wastewater from 19 Minnesota cities in summer 2020. Developed a novel index (Melvin’s Index) of wastewater SARS-CoV-2 viral load, standardized based on a plant virus that is abundant in human feces, to control for factors such as treatment facility capacity, flow rate, and population size. Successively lagged Melvin’s Index values in 1-day increments to find the lag time (between observing an increase in SARS-CoV-2 RNA in wastewater and the appearance of confirmed new COVID-19 positive tests) that maximized correlation (r) between Melvin’s Index and new confirmed cases. Limitations: Variations in clinical SARS-CoV-2 testing might affect correlation with population wastewater viral load.
Implications: Wastewater surveillance for SARS-CoV-2 might allow early detection of local outbreaks, especially where access to healthcare services is limited. A studyexternal icon in Barcelona found SARS-CoV-2 was detected in sewage collected 41 days before the first COVID-19 case.
Figure.
Note: Adapted from Melvin et al. Correlation and lag analysis of wastewater SARS-CoV-2 levels with new COVID-19 clinical cases in Minnesota. A) Indexed N1 levels in real time and transposed (dotted line) to show lag (15 days) to clinical case reports B) N2 levels in real time and transposed (dotted line) to show lag (17 days) to clinical case reports. Licensed under CC BY-ND 4.0.
PEER-REVIEWED
Resurgence of COVID-19 in Manaus, Brazil, despite high seroprevalence.external icon Sabino et al. Lancet (January 27, 2021).
Key findings:
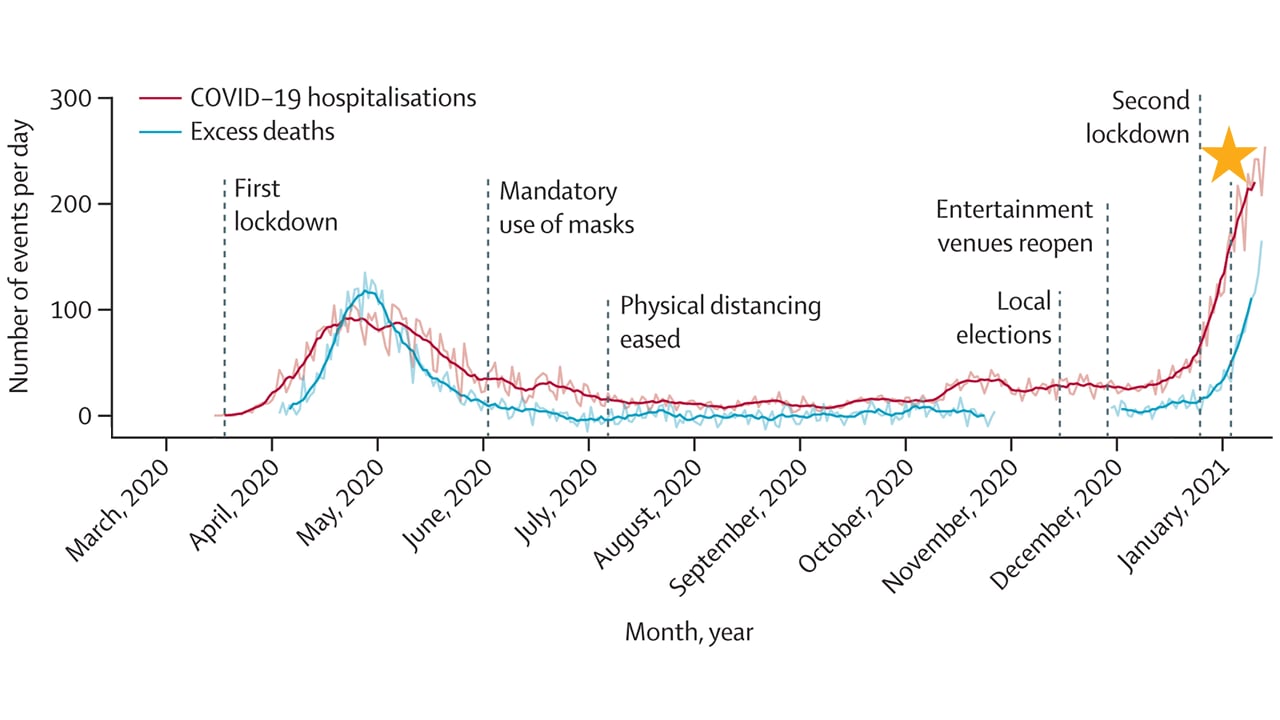
- Manaus, Brazil experienced a sharp rise in COVID-19 hospitalizations in January 2021 despite extensive transmission earlier in the pandemic and rates that had been stable and low for 7 months during relaxed COVID-19 mitigation (Figure).
- There are 4 possible explanations for the surge.
- Greater mixing of susceptible and infected persons in December 2020.
- Waning immunity in the population.
- Circulating variants, specifically B.1.1.7 (501Y.V1) and P.1 with the E484K mutation, evading immunity.
- New variants being more transmissible.
Methods: COVID-19 hospitalizations, excess deaths, and real-time effective reproductive numbers were assessed from the literature and qualitatively compared monthly from March 2020 to January 2021 in Manaus, Brazil. Limitations: Associations were not directly estimated.
Implications: New variants of SARS-CoV-2 might demonstrate changes in transmissibility and/or virulence and could lead to a resurgence of COVID-19 despite high reported seroprevalence. In Rio Grande do Sul, another state in Brazil, da Silva Francisco et al.external icon found wide circulation of the B.1.1.28 variant, with the E484K mutation, co-infection of variants, and new emerging variants. These findings stress the importance of tracking circulating viruses and of reaffirming COVID-19 mitigation measures.
Figure.
Note: Adapted from Sabino et al. Smoothed COVID-19 hospitalizations and excess deaths since March 2020 in Manaus, Brazil. Key mitigation events are marked with dotted lines. The gold star indicates the first detection of P.1 variant. Reprinted from The Lancet, Vol. 397 number 10273, Sabino et al, Resurgence of COVID-19 in Manaus, Brazil, despite high seroprevalence., Pages 452– 455, Copyright (2021), with permission from Elsevier.
PREPRINTS (NOT PEER-REVIEWED)
SARS-CoV-2 seropositivity and subsequent infection risk in healthy young adults: a prospective cohort study.external iconLetizia et al. medRxiv (January 29, 2021). Published in The Lancet Respiratory Medicineexternal icon (July 1, 2021).
Key findings:
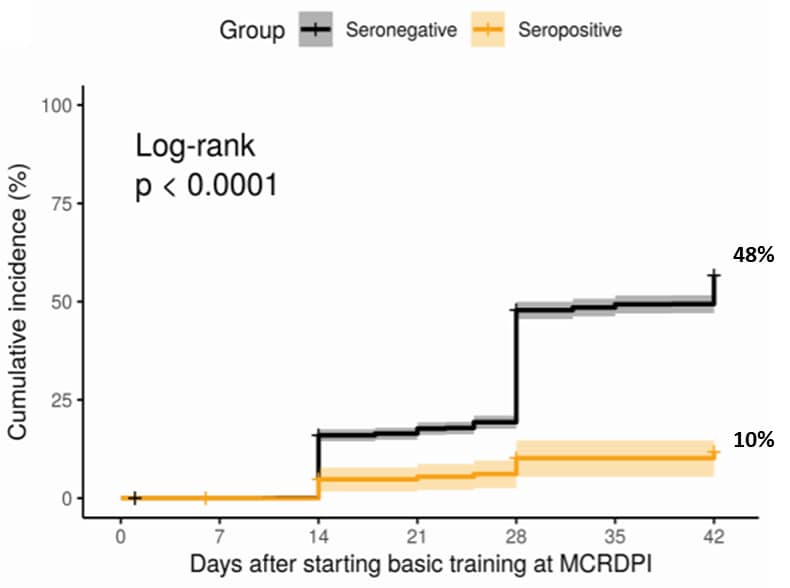
- Although seropositivity conferred an 82% reduced incidence rate, 1% of 189 seropositive participants had ≥1 positive RT-PCR test for SARS-CoV-2 (compared with 48.0% of 2,247 seronegative participants) (Figure).
- Among those infected, seropositive participants had only a modest, approximately 10-fold decrease in nares virus load compared with seronegative participants.
- Among seropositive participants
- New infection was associated with significantly lower baseline full-length spike protein IgG titers.
- Baseline neutralizing titers were detected in 83.3% of the first 54 participants who never became PCR positive compared with 31.6% of the 19 infected participants.
Methods: Prospective 6-week observational study of 3,249 predominantly male, 18–20-year-old Marine recruits, who underwent baseline 2-week supervised quarantine and SARS-CoV-2 RT-PCR and IgG antibody testing. Serial RT-PCR testing was conducted and questionnaires on development of symptoms were completed during and after quarantine. Limitations: Overall high attack rate might not be generalizable to other populations and settings; unknown when seropositive participants were initially infected.
Implications: Although persons with SARS-CoV-2 antibodies are largely protected, subsequent infection is possible for some persons due to lack of sterilizing immunity. Some re-infected individuals could have a similar capacity to transmit virus as those infected for the first time.
Figure.
Note: Adapted from Letizia et al. SARS-CoV-2 PCR positive incidence curves during the six-week follow-up period among baseline seropositive and seronegative groups. Licensed under CC BY 4.0.
Kinetics and correlates of the neutralizing antibody response to SARS-CoV-2.external iconVanshylla et al. bioRxiv (January 26, 2021).Published in Cell Host & Microbe as Kinetics and correlates of the neutralizing antibody response to SARS-CoV-2 infection in humansexternal icon (May 3, 2021).
Key findings:
- 82% of individuals developed serum, and 79% IgG, neutralizing antibodies (NAb) to SARS-CoV-2.
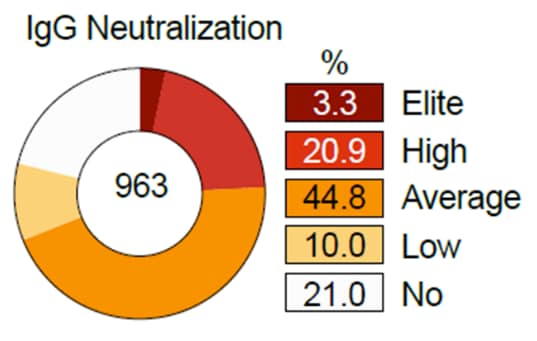
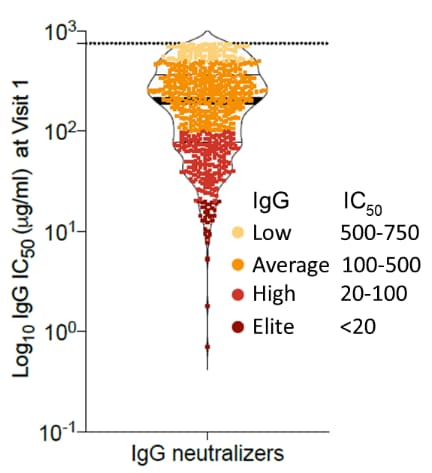
- Neutralizing activity was highly variable, ranging from 3% who were initially ‘elite’ neutralizers, with a 50% Inhibitory Concentration [IC50] of <20 µg/ml of IgG, to 21% who had no neutralizing activity (Figure).
- Higher anti-spike IgG levels, older age, time since disease onset, and fever during acute infection were predictors of SARS-CoV-2 neutralizing activity in mild courses of COVID-19.
- NAb had an initial half-life of 7 weeks in serum and 31 weeks in IgG titer samples.
Methods: NAb responses to SARS-CoV-2 were examined in 963 persons recently recovered from (mostly) mild COVID-19, during up to 4 follow-up visits between April 6 and December 17, 2020. Statistical modeling was used to infer antibody decay rates and to build a prediction model to evaluate how clinical features correlate with NAb titers. Limitations: Loss to follow up may bias results.
Implications: Although NAb can persist for up to 10 months after infection, persons who recover from mild COVID-19 illness have a broad spectrum of neutralizing activity which might affect protective immunity at a population level.
Figure.
Note: Adapted from Vanshylla et al. (A) Donut chart depicts the initial fraction of persons who developed NAb at study visit 1. (B) Violin plot depicts IgG IC50 values for the persons who developed neutralizing antibodies (n=760), categorized by IgG IC50: low (IC50 >500-750 µg/ml), average (IC50 >100-500 µg/ml), high (IC50 20-100 µg/ml), and elite (IC50 <20 µg/ml). Dotted line represents the limit of detection of the assay. Used by permission of authors.
PREPRINT (NOT PEER-REVIEWED)
Strategies to minimize SARS-CoV-2 transmission in classroom settings: combined impacts of ventilation and mask effective filtration efficiency.external icon Rothamer et al. medRxiv. (January 4, 2021).
Key findings:
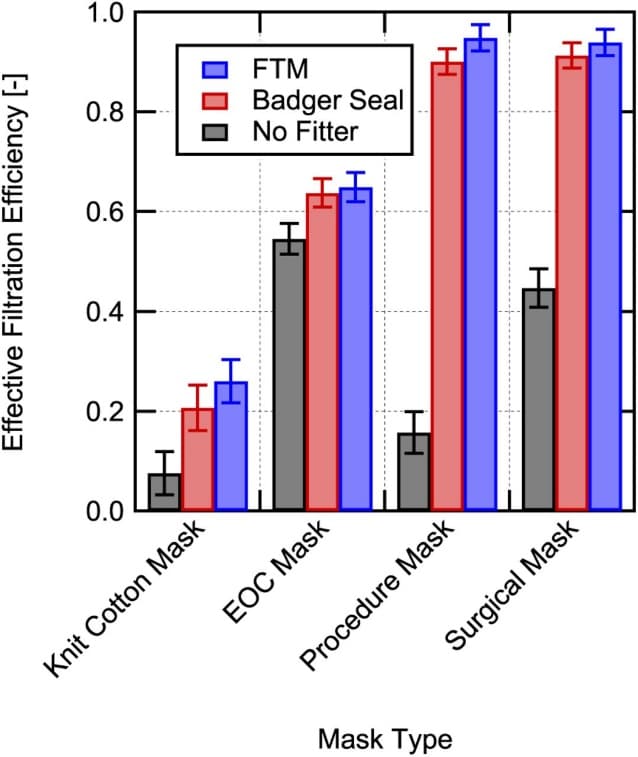
- Filtration efficiencies of four masks tested ranged from 7.5% to 54.5%.
- The addition of mask fitters, devices to improve the seal of a mask, increased filtration efficiency from 20.6% to 91.3% (Figure).
- Ventilation alone did not substantially reduce infection risk.
Methods: A simulation study to evaluate ventilation and mask filtration efficiency of non-medical grade masks, with and without mask fitters, on aerosol transmission in a classroom setting using CPR manikins fitted with aerosol-releasing tubing. Two mask fitters were tested, Badger Seal and Fit the Mask (FTM), using 4 masks: 1) a commercial 4-ply knit cotton mask, 2) a 3-ply polypropylene mask, 3) a 3-ply disposable procedure mask, and 4) a surgical mask. Limitations: Potential overestimation of mask efficacy because manikins were fitted to minimize leakage; simulation might not represent real-world settings.
Implications: All non-medical grade masks are prone to leakage; however, the use of mask fitters can significantly reduce aerosol transmission of SARS-CoV-2 in a classroom setting. Gandhi et alexternal icon. hypothesized that the use of multi-layered, well-fitting masks could achieve >90% efficiency at reducing aerosol transmission.
Figure.
Note: Adapted from Rothamer et al. Overall effective filtration efficiency for inhalation for 4 masks by fitter status (with no mask fitter, with the Badger Seal mask fitter, with the Fit the Mask (FTM) mask brace). Licensed under CC BY-ND 4.0.
PEER-REVIEWED
Model-informed COVID-19 vaccine prioritization strategies by age and serostatus.external icon Bubar et al. Science (January 21, 2021).
Key findings:
- Prioritizing adults ≥60 years old shows the greatest reduction in mortality and years of life lost (YLL) after accounting for country-specific age structure, age-contact structure, infection fatality rates, seroprevalence, and age-varying efficacy of vaccine.
- Prioritizing adults aged 20–49 years old minimizes cumulative incidence but is only superior at minimizing deaths when R0 = 1.15 and vaccine efficacy is ≥80% or vaccine rollout is ≤0.2%, or when vaccine efficacy is lower in older adults (≥60 years old) compared to individuals <60 years.
- Prioritizing seronegative individuals provides the greatest benefit where seroprevalence is high.
Methods: A mathematical model quantified the impact of five age-stratified COVID-19 vaccine prioritization strategies on cumulative incidence, mortality and YLL. Limitations: Model assumptions limit generalizability; disease severity is considered by age only.
Implications: Pairing vaccination with serological testing of individuals may be a useful strategy for prioritization of limited vaccine supplies and to reach vulnerable populations.
PREPRINTS (NOT PEER-REVIEWED)
mRNA-1273 vaccine induces neutralizing antibodies against spike mutants from global SARS-CoV-2 variantsexternal icon. Wu et al. bioRxiv (January 25, 2021). Published in NEJM as Serum neutralizing activity elicited by mRNA-1273 vaccineexternal icon (April 15, 2021).
Key findings:
- Moderna mRNA-1273 vaccine was able to neutralize all known strains of SARS-CoV-2.
- Full neutralization was still achieved despite diminished neutralizing responses against the B.1.351 (South Africa) variant, with the E484K mutation, because neutralizing titers remained relatively high (1:290).
- No significant differences in neutralizing antibody titers against B.1.1.7 (UK), 20E, 20A.EU2, DG614-N439K, or mink cluster 5, variants were detected.
Methods: Neutralization assays using pseudovirus expressing SARS-CoV-2 spike protein mutations found in major current variants were used to determine the neutralizing capacity of sera from 8 human subjects and 12 non-human primates vaccinated with the Moderna mRNA-1273 vaccine. Neutralization was compared to the neutralization observed against D614G, the dominant strain of 2020. Limitations: Small sample size; P.1 variant was not included.
Implications: Moderna mRNA-1273 vaccine appears to be effective against both the UK and South African SARS CoV-2 variants. However, further studies are warranted to substantiate these findings.
The effectiveness of the first dose of BNT162b2 vaccine in reducing SARS-CoV-2 infection 13-24 days after immunization: real-world evidenceexternal icon. Chodick et al. medRxiv (January 29, 2021). Published in JAMA Network Open as Assessment of effectiveness of 1 dose of BNT162b2 vaccine for SARS-CoV-2 infection 13 to 24 days after immunizationexternal icon (June 7, 2021).
Key findings:
- The cumulative incidence of SARS-CoV-2 infection was 0.57% (n=2,484) during days 1-12 and 0.27% (n=614) during days 13-24 following the first dose of the BNT162b2 mRNA COVID-19 vaccine.
- There was a 51.4% reduction in the weighted average daily incidence of SARS-CoV-2 infection at days 13–24 after the first dose (21.8 per 100,000 population), compared to days 1–12 (43.41 per 100,000 population).
Methods: A retrospective cohort study of 503,875 individuals aged ≥16 years old in Israel estimated the effectiveness of the first dose of the BNT162b2 vaccine administered from December 19, 2020 to January 15, 2021. Daily and cumulative infection rates during days 13-14 were compared to days 1-12 after the first dose using generalized linear models. Limitations: Unreported vaccinations might bias results.
Implications: Based upon temporal incidence, the BNT162b2 vaccine (Pfizer-BioNTech) is approximately 51% effective at reducing the risk of SARS-CoV-2 infection at 13 to 24 days following the first dose.
Detection, Burden, and Impact
- Lowe et al. Association of smoking and cumulative pack-year exposure with COVID-19 outcomes in the Cleveland Clinic COVID-19 registry.external icon JAMA Internal Medicine. (January 25, 2021). Of 7,102 adults with COVID-19 in the Cleveland Clinic COVID-19 registry between March 8 and August 25, 2020, 341 persons who smoked >30 pack-years had higher odds of hospitalization and death, although the odds were attenuated with inclusion of comorbidities; these data demonstrate an apparent dose-dependent relationship between smoking and adverse COVID-19 outcomes.
- Ehrenberg et al. Launching a saliva-based SARS-CoV-2 surveillance testing program on a university campus.external icon medRxiv (Preprint, January 26, 2021). Published in PloS Oneexternal icon (May 26, 2021). Describes a successful university-based surveillance system using saliva-based testing for SARS-CoV-2 among 3,653 persons to identify asymptomatic and pre-symptomatic cases and prevent outbreaks.
Natural History of SARS-CoV-2 Infection
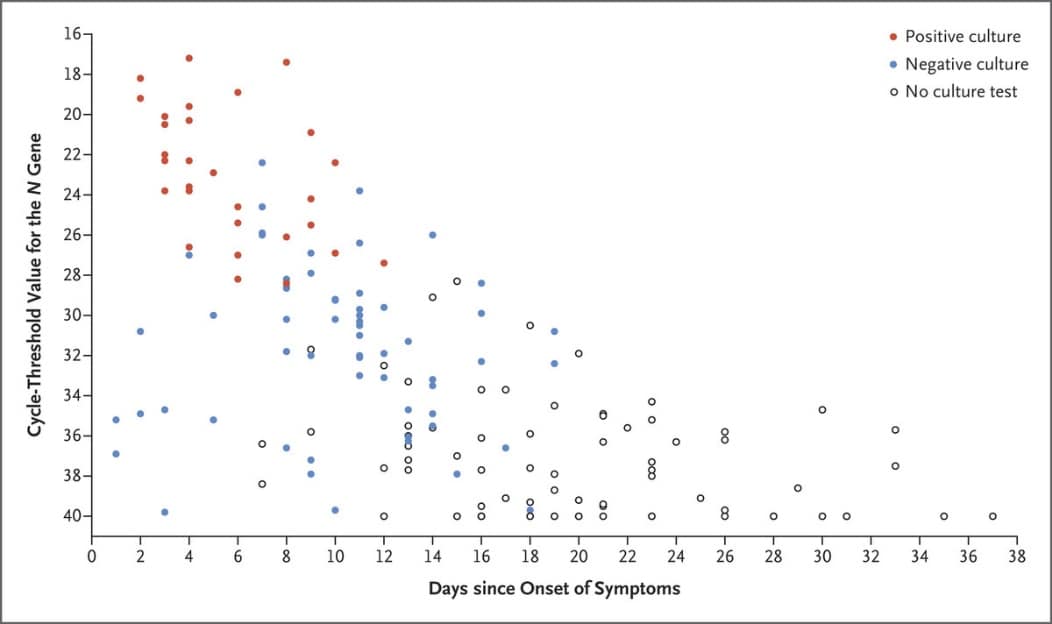
- Kim et al. Duration of culturable SARS-CoV-2 in hospitalized patients with COVID-19.external icon NEJM (January 27, 2021). Based on all 2-day RT-PCRs and viral cultures among 21 hospitalized patients with COVID-19, the median duration of shedding of viable virus was approximately 7 days (95% CI 5-10).
Figure.
Adapted from Kim et al. Timing of presence or absence of viable SARS-CoV-2 on viral culture and Ct values for 165 serial samples. Viral loads were determined with the Ct value for the N gene of SARS-CoV-2. Each circle represents a sample obtained on the specified day. Viral culture was either positive or negative. DOI: 10.1056/NEJMc2027040. Copyright © (2021) Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
- Al-Samkari et al. Thrombosis, bleeding, and the observational effect of early therapeutic anticoagulation on survival in critically ill patients with COVID-19external icon. Annals of Internal Medicine (January 26, 2021). In a multi-center, observational cohort study of 3,239 critically ill patients admitted between March 4 and April 11, 2020, early therapeutic anticoagulation did not affect in-hospital survival.
- Starr et al. Prospective mapping of viral mutations that escape antibodies used to treat COVID-19.external icon Science (January 25, 2021). Mapping of viral mutations to SARS-CoV-2 receptor binding domain showed that a single amino acid mutation (E406W) escapes the two monoclonal antibody REGN-CoV2 cocktail.
- Rappazzo et al. Broad and potent activity against SARS-like viruses by an engineered human monoclonal antibody.external icon Science (January 25, 2021). An engineered human monoclonal antibody demonstrated neutralization potency similar to neutralizing antibodies currently in clinical use providing significant protection against COVID-19 in mouse models.
- Nemani et al. Association of psychiatric disorders with mortality among patients with COVID-19.external icon JAMA (January 27, 2021). In a retrospective cohort study of 7,348 patients with confirmed COVID-19 at 4 acute care hospitals in New York City from March 3 to May 31, 2020, persons with schizophrenia had significantly increased odds of 45-day mortality.
- Alam et al. An interactive COVID-19 virus mutation tracker (CovMT) with a particular focus on critical mutations in the receptor binding domain (RBD) region of the spike protein.external icon medRxiv (Preprint, January 25, 2021). Published in The Lancet Infectious Diseases as CovMT: An interactive SARS-CoV-2 mutation tracker, with a focus on critical variantsexternal icon (February 8, 2021). As new SARS-CoV-2 variants emerge with increased transmissibility and potential immune escape, it is important to monitor sequencing efforts and evolution of mutations. These authors developed a global mutation trackerexternal icon that is updated daily and includes clinical data.
Protection in Healthcare and Non-Healthcare Work Settings
- Moghadas et al. Evaluation of COVID-19 vaccination strategies with a delayed second dose.external icon medRxiv (Preprint, January 29, 2021).Published in PloS Biologyexternal icon (April 21, 2021). Based on an assumed 80% efficacy after the first dose, modelling showed that delaying the second dose of the Moderna vaccine by 9-12 weeks could reduce infections, hospitalizations, and deaths. However, for the Pfizer-BioNTech COVID-19 vaccine, with an assumed 52% efficacy after the first dose, there was no clear advantage to delaying the second dose due to waning immunity.
Prevention, Mitigation, and Intervention Strategies
- Crane et al. Change in reported adherence to nonpharmaceutical interventions during the COVID-19 pandemic, April-November 2020.external icon JAMA (January 22, 2021). National survey responses from 7,705 participants between April 1 and November 24, 2020, showed a decrease in adherence to nonpharmacological interventions indicating “pandemic fatigue; however, there was in increase in self-reported mask-wearing which may reflect improved public health messaging.
Social, Behavioral, and Communication Science
- Ayers et al. Suicide-related internet searches during the early stages of the COVID-19 pandemic in the US.external icon JAMA Network Open (January 21, 2021). Google searches related to suicide between January 1 and July 5, 2020, showed a decline after a national emergency was declared in March 2020. This decline was likely due to increased social support, called the “pulling together” phenomenon, often associated with catastrophes.
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.