COVID-19 Science Update released: Jaunary 8, 2021 Edition 71

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
National trends in the US public’s likelihood of getting a COVID-19 vaccine— April 1 to December 8, 2020external icon. Szilagyi et al. JAMA (December 29, 2020).
Key findings:
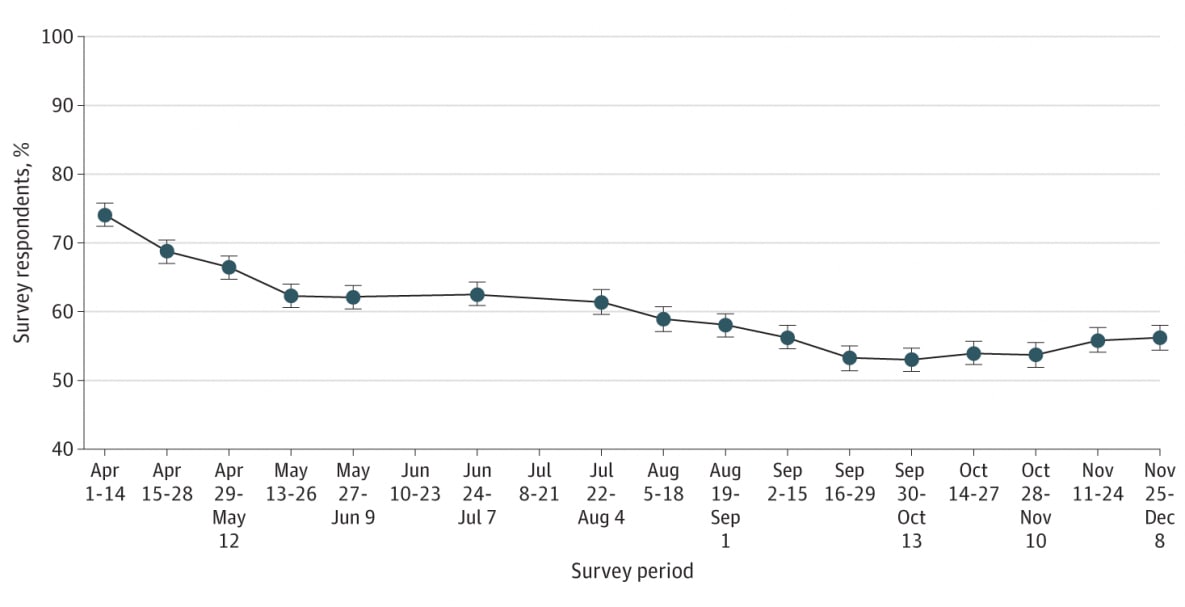
- From April to December 2020, the percentage of persons who stated they were somewhat or very likely to get vaccinated declined from 74% to 56% in the US (Figure).
- Significant declines were observed for women and men, all age groups, racial/ethnic groups and educational subgroups.
Methods: A cohort of 8,167 US adults enrolled in a probability-based internet panel surveyexternal icon responded between April and December 2020 about their likelihood of receiving a COVID-19 vaccine. Limitations: Small sample sizes for minority populations.
Implications: These findings suggest that the likelihood of COVID-19 vaccine acceptance has been declining since the beginning of the pandemic and highlight the need for educational campaigns to raise the public’s willingness to consider COVID-19 vaccination.
Figure:
Note: From Szilagyi et al. Percentage of US adults reporting likelihood of getting a COVID-19 vaccine. Percentages and 95% CIs are plotted. Reproduced with permission from JAMA. National trends in the US public’s likelihood of getting a COVID-19 Vaccine—April 1 to December 8, 2020. doi:10.1001/jama.2020.26419. Copyright©2020 American Medical Association. All rights reserved.
PEER-REVIEWED
Comparison of the characteristics, morbidity, and mortality of COVID-19 and seasonal influenza: A nationwide, population-based retrospective cohort studyexternal icon. Piroth et al. Lancet Respiratory Medicine (December 17, 2020).
Key findings:
- Compared with patients hospitalized with influenza, patients hospitalized with COVID-19 were older, more likely to be male, and have comorbidities.
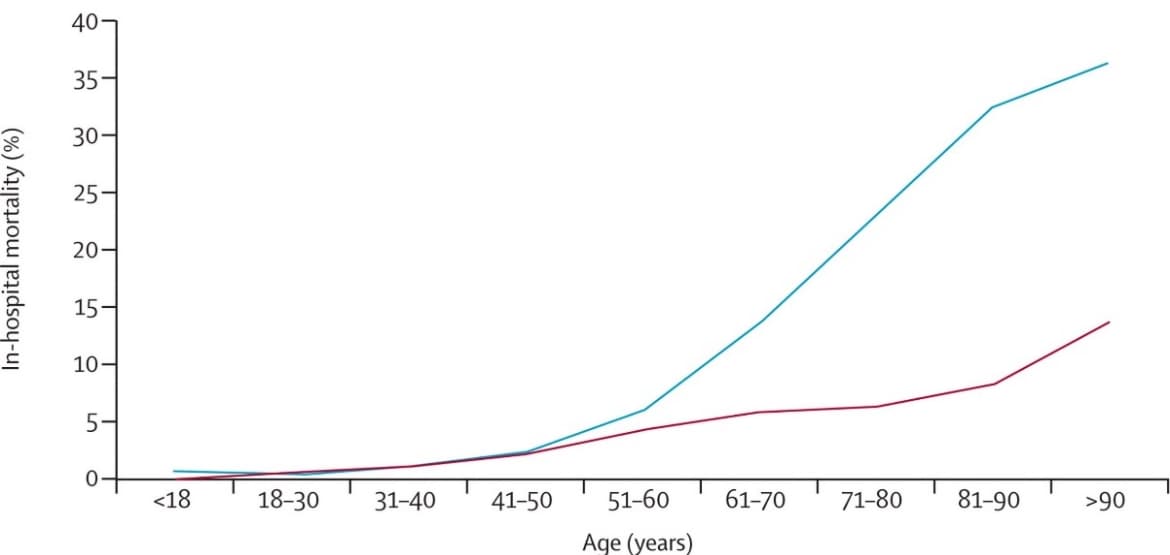
- In-hospital mortality was 2.9 (95% CI 2.8-3.0) times higher in patients with COVID-19 than in patients with influenza (Figure).
- In-hospital mortality was 10 times higher for COVID-19 than for influenza among patients ages 11–17 years.
- Patients hospitalized with COVID-19 were more likely than patients hospitalized with influenza to develop acute respiratory failure or pulmonary embolism, and more likely to require admission to intensive care and invasive mechanical ventilation.
Methods: Nationwide retrospective cohort study of 89,530 patients hospitalized for COVID-19 from March 1 to April 30, 2020 compared with 45,819 patients hospitalized for influenza between December 1, 2018, and February 28, 2019 in France. Limitations: Variable influenza testing practices and more patients were likely to have been tested for COVID-19 in 2020 than for influenza during 2018–19; no ethnicity data; findings in children were based on small numbers.
Implications: Poorer outcomes might reflect greater respiratory pathogenicity associated with SARS-CoV-2 infection than with influenza infection. Preventive measures such as vaccination are critical to preserve hospital capacity and limit infections and deaths.
Figure:
Note: Adapted from Piroth et al. Mortality of patients hospitalized for COVID-19 vs seasonal influenza, by age at admission. Reprinted from The Lancet Respiratory Medicine, Piroth et al., Comparison of the characteristics, morbidity, and mortality of COVID-19 and seasonal influenza: a nationwide, population-based retrospective cohort study, Copyright (2020), with permission from Elsevier.
Where has all the influenza gone? The impact of COVID-19 on the circulation of influenza and other respiratory viruses, Australia, March to September 2020external icon. Sullivan et al. Eurosurveillance (November 26, 2020).
Key findings:
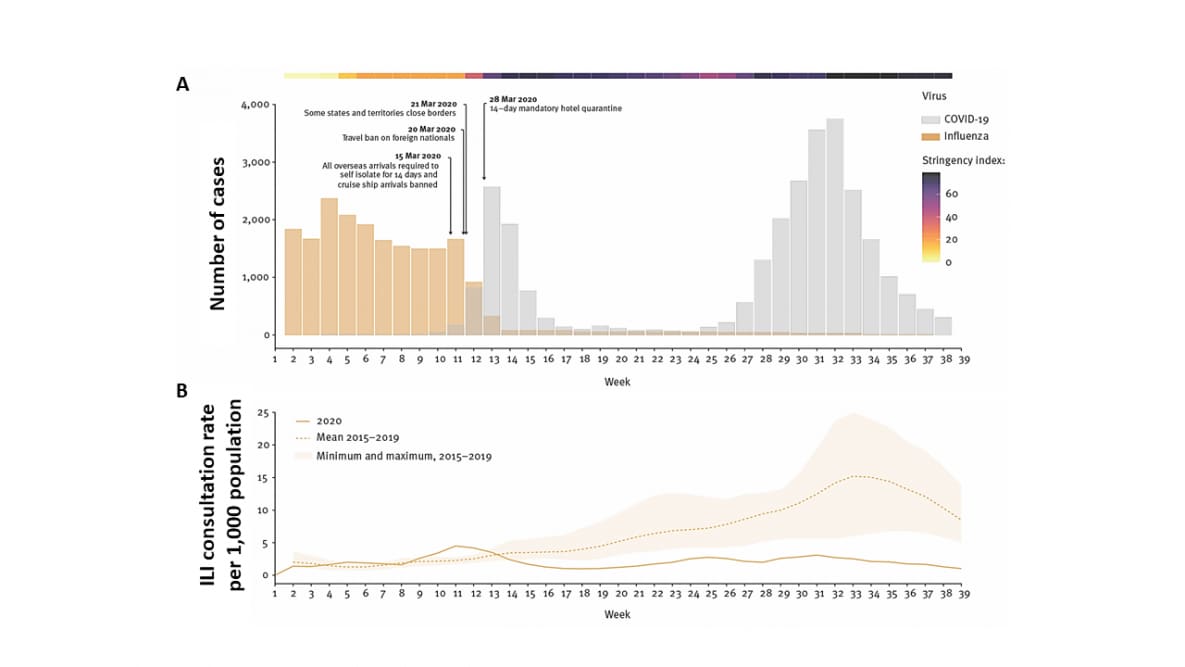
- Influenza cases in Australia dropped sharply between mid-March (week 11) and mid-April (week 14) 2020, when COVID-19 travel and work restrictions were introduced; after restrictions were relaxed cases did not increase during the usual influenza season (Figure A).
- There were 36 influenza-attributable deaths reported nationally in Australia from January to September 2020 compared with 812 deaths from January to September 2019.
- Influenza-like illness (ILI) surveillance consultation rates (Figure B) and influenza hospitalizations were lower in 2020 compared with 2015-2019.
Methods: Description of Australia’s national influenza case reporting in 2020, ILI surveillance in primary care from 2015-2020, and national sentinel influenza hospitalization data from 2015-2020, compared with COVID-19 notifications and measures implemented from March to September 2020. Limitations: Ecological evaluation; difficult to distinguish the relative contributions of different COVID-19 restrictions and the flu vaccination.
Implications: Influenza activity was at an all-time low in Australia in 2020. Restrictions implemented for COVID-19 may have substantially reduced transmission of influenza and potentially other respiratory pathogens.
Figure:
Note: Adapted from Sullivan et al. Surveillance data on (A) influenza and COVID-19 notifications (from the National Notifiable Diseases Surveillance Systemexternal icon) and measures implemented (Oxford Stringency Index indicates the severity of government restrictions); (B) influenza-like illness (ILI) consultation rates by week (3-week moving average), from the Australian Sentinel Practices Research Network. Licensed under CC BY 4.0.
Coronavirus disease 2019 in veterans receiving care at veterans health administration facilitiesexternal icon. Luo et al. Annals of Epidemiology (December 15, 2020).
Key findings:
- Among 14,259 COVID-19 cases in veterans, the relative mortality rate of Black veterans was 2.83 (95% CI 2.56-3.14) times higher than White veterans; however, the case-fatality rate (CFR) of Black veterans was 0.75 (95% CI 0.68-0.82) times that of White veterans.
- Among veterans who died from COVID-19 (n = 1703), large proportions were aged ≥ 65 years (90%), had cardiovascular disease (87%) and diabetes (57%).
Methods: Cross-sectional analysis of aggregated data from veterans’ electronic health records studied SARS-CoV-2 infections at Veterans Affairs (VA) facilities from March 4 to June 23, 2020. Unadjusted infection, mortality, and CFRs were determined by age, gender, race, and comorbidities. Limitations: was restricted to veterans treated at VA facilities; did not adjust for potential confounders.
Implications: This preliminary analysis shows differences in mortality by age and race from COVID-19 among veterans, however further analyses adjusting for potential confounders are needed.
Symptomatic SARS-CoV-2 reinfection of a health care worker in a Belgian nosocomial outbreak despite primary neutralizing antibody response.external icon Selhorst et al. Clinical Infectious Diseases (December 14, 2020).
Key findings:
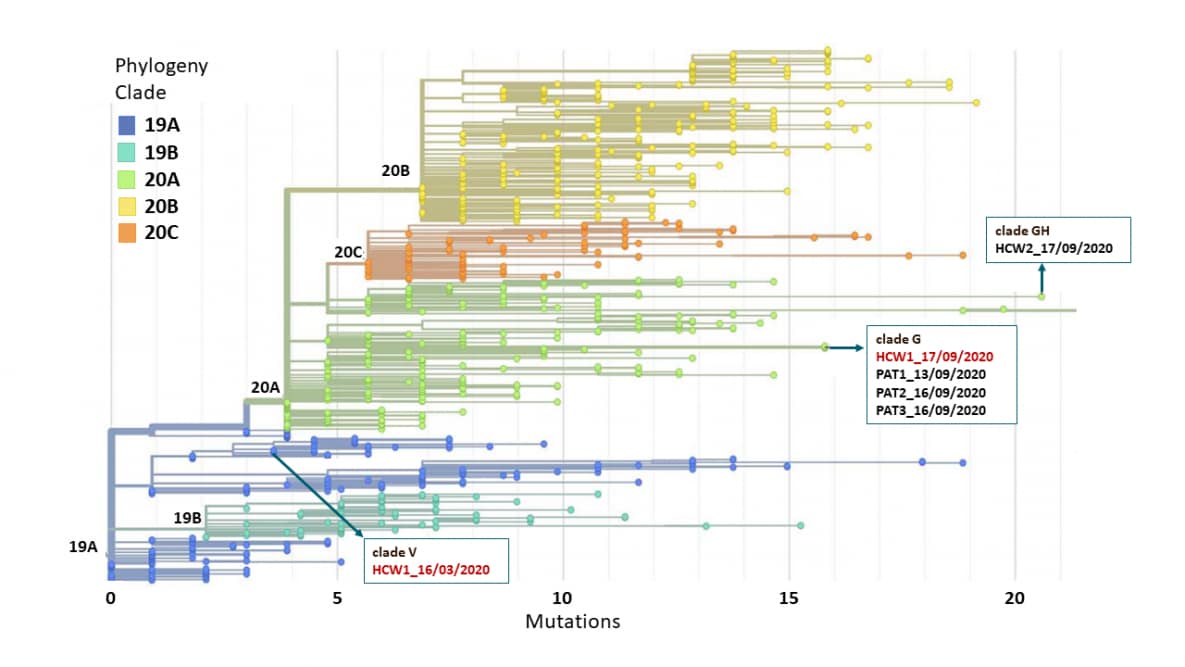
- SARS-CoV-2 reinfection with a virus belonging to a different SARS-CoV-2 clade (G clade) than the virus causing the first COVID-19 infection (V clade) was confirmed in a 39-year-old healthcare worker (HCW) 185 days after a symptomatic primary infection despite evidence of an effective humoral response (Figure).
- Reinfection was characterized by mild symptoms, rapid rise in serum IgG and neutralizing antibodies, high viral loads, and replicating virus in nasopharyngeal (NP)swabs.
Methods: SARS-CoV-2 whole genome sequencing was performed from NP swabs from 5 cases (3 patients and 2 HCWs) including samples from one re-infected immunocompetent person’s symptomatic primary infection to distinguish reinfection from persistent infection and determine whether transmission clusters could be detected during a Belgian nosocomial outbreak in September 2020. Humoral immune responses and viral infectiousness were quantified. Limitations: Unable to compare humoral and neutralizing antibody levels at similar time points during primary infection and reinfection.
Implications: Despite an effective humoral immune response, reinfection can occur after a relatively short period and transmission during reinfection appears possible.
Figure:
Note: Adapted from Selhorst et al. SARS-CoV-2 clade assignment of genomes recovered from 3 patients (PAT1, PAT2, PAT3) and 2 health care workers (HCW1, HCW2). Colors represent the different clades. The genomes and their clades are marked by arrows. Permission request in process.
PEER-REVIEWED
Analyses of risk, racial disparity, and outcomes among US patients with cancer and COVID-19 infection.external icon Wang et al. JAMA Oncology (December 10, 2020).
Key findings:
- Patients with a recent diagnosis of cancer were at significantly increased risk for COVID-19 infection and adverse outcomes.
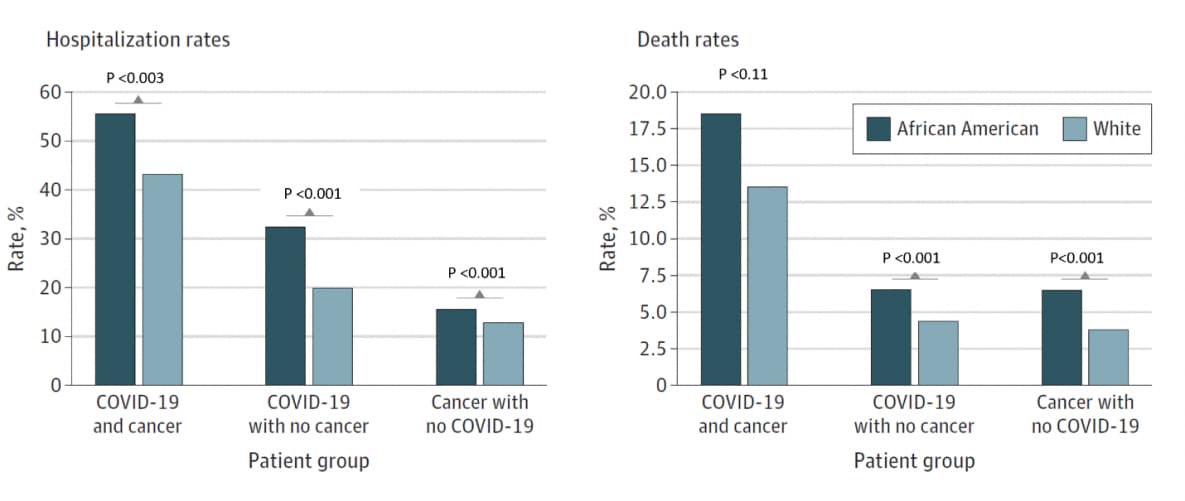
- Hospitalization and death rates for patients with a recent cancer diagnosis and COVID-19 were higher than for patients with COVID-19 but no recent cancer diagnosis and that for patients with recent cancer diagnosis but no COVID-19.
- African American patients with recently diagnosed cancers and/or COVID-19 had higher hospitalization and death rates than did White patients (Figure).
- Breast cancer showed the largest racial disparity (aOR 5.44, 95% CI 4.69-6.31).
Methods: A retrospective case-control analysis using electronic health records of 73.4 million adult patients from 360 hospitals across the US in August 2020. COVID-19 infection and 13 common cancer types and adverse outcomes were assessed by demographic factors. Limitations: Limited covariates assessed, underreporting of COVID-19 cases.
Implications: Cancer and COVID-19 had synergistic effects on adverse patient outcome. This study identified high risk groups such as African American patients with cancer who are more vulnerable to COVID-19.
Figure:
Note: Adapted from Wang et al. Hospitalization and death rates among African American and White patients stratified by recent diagnosis of cancer and COVID-19, COVID-19 without a recent diagnosis of cancer, and a recent diagnosis of cancer but no COVID-19. Reproduced with permission from JAMA Oncology. Analyses of risk, racial disparity, and outcomes among US patients with cancer and COVID-19 infection. doi:10.1001/jamaoncol.2020.6178. Copyright© (2020) American Medical Association. All rights reserved.
COVID-19 neutralizing antibodies predict disease severity and survival.external icon Garcia-Beltran et al. Cell (December 15, 2020).
Key findings:
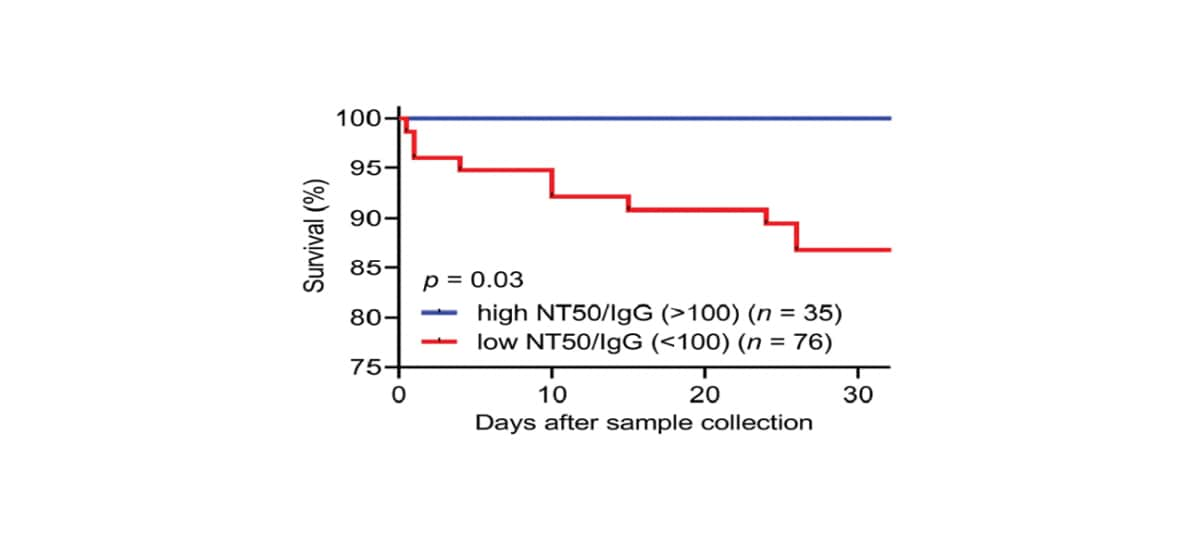
- High neutralizing potency of anti-receptor binding domain (anti-RBD) antibodies was protective against death (100% 30-day survival, n = 35) compared with low neutralizing potency (87% 30-day survival, n = 76) (Figure).
- IgG, IgM, and IgA antibodies together neutralize SARS-CoV-2, but only IgG was detected throughout the 3-month follow-up period.
- Sera were cross-neutralizing between SARS-CoV-2 wild-type and D614G mutated viruses.
Methods: Cohort study describing the humoral immune response (anti-RBD and IgG, IgM, and IgA antibodies) and clinical outcomes of 113 RT-PCR-confirmed SARS-CoV-2 infected persons with ≤3 months of follow-up from date of symptom onset and compared to 1,257 pre-pandemic serum samples in the US. A SARS-CoV-2 pseudovirus neutralization assay quantified the neutralization potency of humoral responses. Limitations: Inferences between COVID-19 treatments and disease severity are limited by multiple treatments being used.
Implications: The relationship between neutralizing humoral immunity and disease progression is important and merits further study to develop new therapeutics.
Figure
Note: Adapted from Garcia-Beltran et al. Survival probability (vertical axis) over 30 days (horizontal axis) for patients with high or low neutralizing potency, indexed by neutralizing titer at 50% / IgG titer (NT50/IgG). Reprinted from Cell, Garcia-Beltran et al., COVID-19 neutralizing antibodies predict disease severity and survival, Copyright (2020), with permission from Elsevier.
The first wave of the COVID-19 pandemic in Spain: Characterisation of cases and risk factors for severe outcomes, as at 27 April 2020.external icon Larrauri et al. Eurosurveillance (December 17, 2020).
Key findings:
- During the first pandemic wave in Spain, 45.4% of COVID-19 cases were hospitalized, 4.6% were admitted to an ICU and 11.9% died.
- Among those who died, 94.8% had at least one underlying disease; chronic renal disease had the highest odds of death (OR 1.47, 95% CI 1.29-1.68).
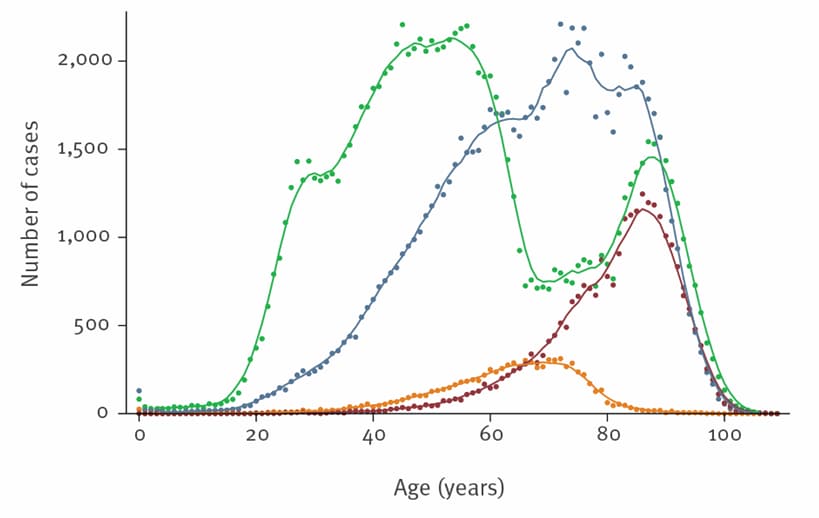
- Non-hospitalized cases had a bimodal age distribution, with the first peak observed among cases 50–60 years of age and the second peak among cases 90 years of age (Figure).
- Compared with cases aged <40 years, cases aged ≥80 years had the highest odds of death (OR 28.4, 95% CI 19.85-40.78).
Methods: National surveillance data were used to describe 218,652 RT-PCR confirmed COVID-19 cases from January 31 to April 27, 2020 in Spain. Clinical severity of cases was classified, and multivariable regression identified independent risk factors for disease severity of hospitalized cases. Limitations: Inability to confirm mild or asymptomatic cases; incomplete data for certain variables leading to an under- or over-estimate of associations.
Implications: This study highlights the early impact of COVID-19 pandemic on older adults particularly those with comorbidities such as chronic renal disease. Surveillance provides information to health and government authorities to inform control measures, particularly in vulnerable populations.
Figure:
Note: Adapted from Larrauri et al. Distribution of COVID-19 cases by age and severity, Spain, January – April 2020. Severity Categories: Green– No hospitalization; Blue– Hospitalization; Orange– ICU admission; Red– death. Licensed under CC BY 4.0.
PEER-REVIEWED
Comparison of knowledge and information-seeking behavior after general COVID-19 public health messages and messages tailored for Black and Latinx communities: A randomized controlled trial.external icon Aslan et al. Annals of Internal Medicine (December 21, 2020).
Key findings:
- Persons who received COVID-19 messaging videos had lower knowledge errors (average incident rate [aIR] 0.065, 95% CI 0.062-0.068) than persons who did not receive public health messaging videos (aIR 0.085, 95% CI 0.076-0.095).
- Other ways of tailoring messaging did not change effectiveness.
- Black physician presenters slightly increased information-seeking among Black participants.
Methods: A randomized controlled trial of knowledge gaps and information-seeking about COVID-19 public health messaging among 14,144 Black and Hispanic/Latino respondents was conducted in May 2020. Intervention videos presented information on COVID-19 symptoms tailored by presenter’s racial/ethnic concordance with viewers and several other message characteristics. Limitations: selection bias of participants using online survey; behavior change resulting from interventions was not directly measurable.
Implications: Public health messaging can reduce knowledge gaps about COVID-19 and as mentioned by Cooper et alexternal icon., racial representation in that messaging may improve information-seeking among Black or other communities of color.
Detection, burden, and impact: Viral Genomics
- Wang et al. Genetic screens identify host factors for SARS-CoV-2 and common cold coronaviruses.pdf iconexternal icon Cell (January 7, 2021). Genome-wide CRISPR screens of three coronaviruses, including SARS CoV-2, showed that several shared host pathways might serve as effective drug targets for multiple coronaviruses.
- Yellapu et al. Evolutionary analysis of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) reveals genomic divergence with implications for universal vaccine efficacyexternal icon. Vaccines (October 8, 2020). Genomic divergence was observed among genomes with large numbers of nucleotide variations, suggesting that these variations should be considered in the development of a COVID-19 vaccine and that continued genomic divergence could hinder a universal vaccine.
Transmission
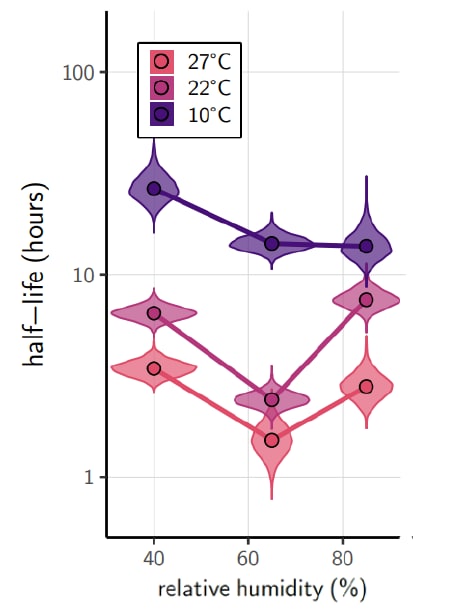
- Morris et al. Mechanistic theory predicts the effects of temperature and humidity on inactivation of SARS-CoV-2 and other enveloped virusesexternal icon. bioRxiv (December 18, 2020). Study looking at the half-life of SARS-CoV-2, showing longer survival in cold temperatures and shorter survival at higher humidity (Figure).
Note. Adapted from Morris et al. Schematic of effects of temperature and relative humidity on duration of SARS-CoV-2 viability. Used by permission of authors.
Natural History of SARS-CoV-2 Infection: Spectrum and Clinical Course
- Neupane et al. Gastrointestinal symptoms among patients admitted with COVID-19 and its relation to outcome: A multi-center retrospective analysis.external icon American Journal of Gastroenterology (October, 2020). Among COVID-19 patients admitted or evaluated in an ED, GI symptoms were common but were not associated with unfavorable COVID-19 outcomes or pre-existing GI conditions. The presence of GI symptoms alone was rare.
- Bowles et al. Surviving COVID-19 after hospital discharge: Symptom, functional, and adverse outcomes of home health recipients.external icon Annals of Internal Medicine (November 24, 2020). Among patients with COVID-19 who were admitted to home health care, comorbid conditions associated with rehospitalization or death included heart failure, diabetes, chronic pain and cognitive impairment.
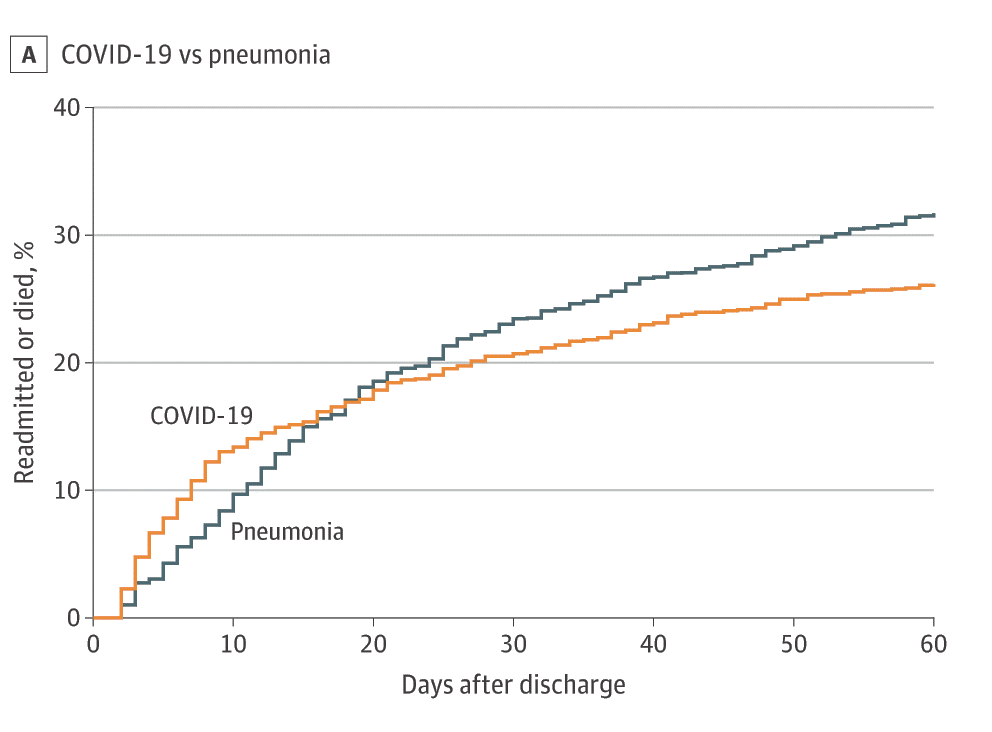
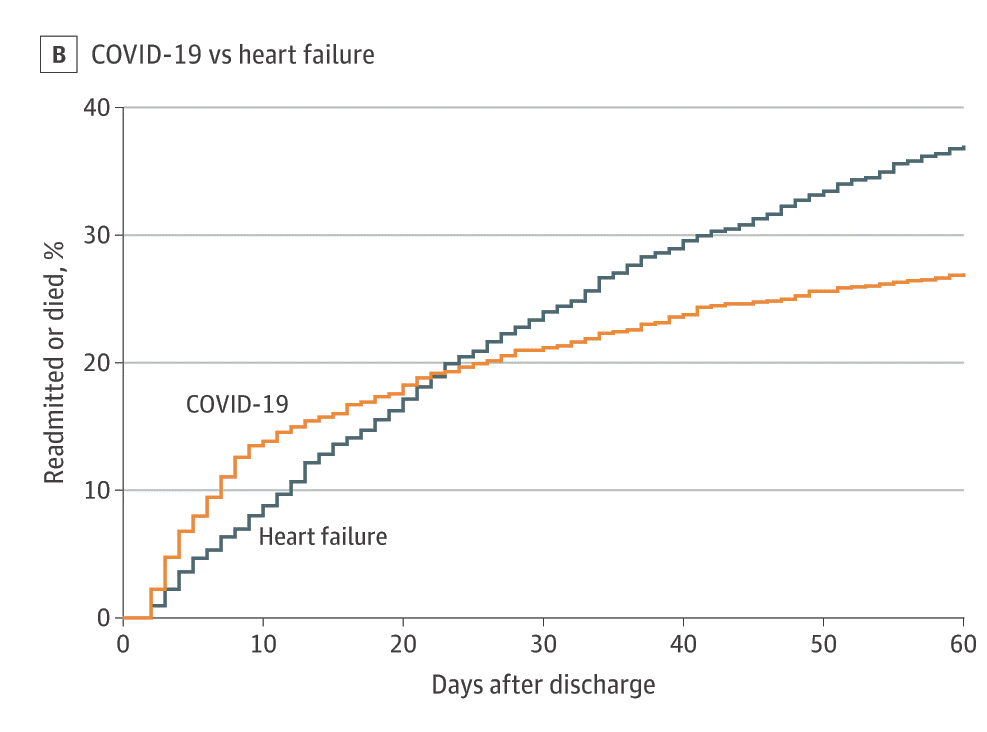
- Donnelly et al. Readmission and death after initial hospital discharge among patients with COVID-19 in a large multihospital system.external icon JAMA (December 14, 2020). Among hospitalized COVID-19 patients in the VA system, 27% were readmitted or died within 60 days of discharge. While rates were higher among COVID-19 survivors compared with cohorts of survivors of pneumonia and heart failure at 10 days post-discharge, they became comparatively lower over time (Figure).
Note: Adapted from Donelly et al. Kaplan-Meier curves comparing 60-day outcomes [A] among patients with COVID-19 (n = 1,366) and pneumonia (n = 1799) and [B] among patients with COVID-19 (n = 1,430) and with heart failure (n = 3,505).
Reproduced with permission from JAMA. Readmission and death after initial hospital discharge among patients with COVID-19 in a large multihospital system. doi:10.1001/jama.2020.21465. Copyright© (2020) American Medical Association. All rights reserved.
Prevention, Mitigation, and Intervention Strategies: Contact Tracing
- Brown et al. Training and incorporating students in SARS-CoV-2 case investigations and contact tracing.external icon Public Health Reports (December 10, 2020). Describes key components of a program to increase capacity of local and state health departments by including university students as case investigators for the COVID-19 response.
Prevention, Mitigation, and Intervention Strategies: Acceptability of COVID-19 Vaccines
- Largent et al. US public attitudes toward COVID-19 vaccine mandates.external icon JAMA (December 18, 2020). 61.4% of respondents indicated likelihood to accept vaccination, whereas mandated vaccination for children, adults, or employees were acceptable to fewer than 50% of respondents. Voluntary and mandated vaccination acceptance was associated with political affiliation and racial identity.
Social and Mental Health Impacts of the Pandemic
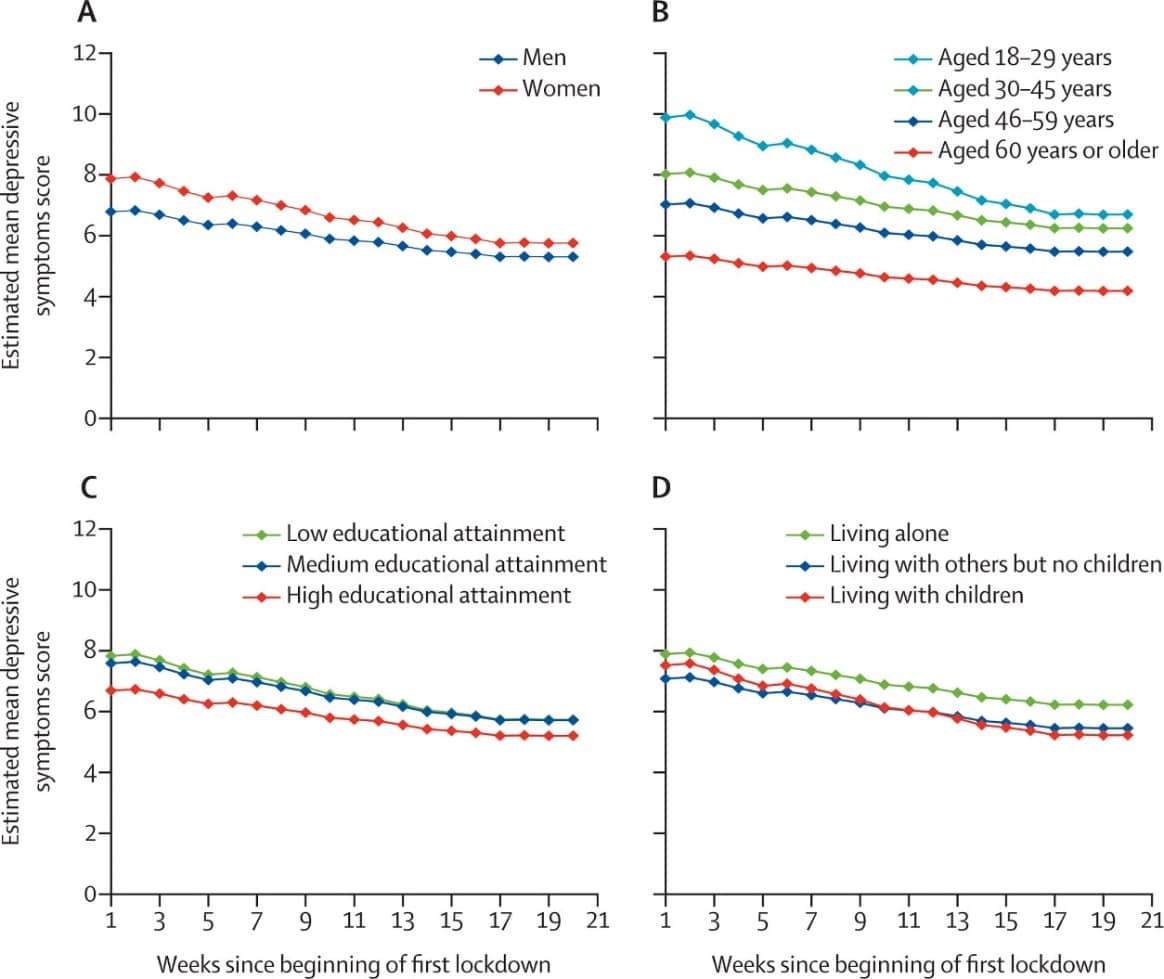
- Fancourt et al. Trajectories of anxiety and depressive symptoms during enforced isolation due to COVID-19 in England: a longitudinal observational study.external icon Lancet Psychiatry (December 09, 2020). Rates of depressive and anxiety symptoms were highest at the beginning of pandemic lockdown and steadily decreased over a 20-week period. Symptoms were highest among women, persons who had lower income or education levels, or who lived alone with children during the early lockdown period. Disparities declined over time but were still evident at 20 weeks (Figure).
Note: From Fancourt et al. Predicted growth trajectories of mean depressive symptom scores by individual characteristics. [A] gender; [B] age group; [C] educational attainment, and; [D] living with others Licensed under CC BY.
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.