
Monthy Case Studies - 1999
Case #12 - May, 1999
An adult male patient went to a hospital in Virginia with symptoms suggestive of a complicated course of pneumonia, for which he was treated with antibiotics. He had traveled to Kenya four months earlier and to Beijing, China six days earlier. The blood smear showed the organisms seen in Figures A through D. Note: The infected erythrocyte in Figure B is not enlarged, compared to noninfected erythrocytes. What is your diagnosis? Based on what criteria?
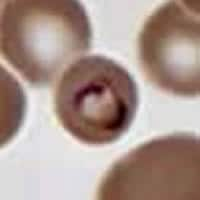
Figure A

Figure B
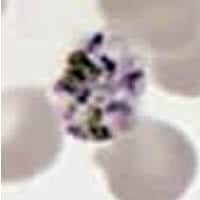
Figure C
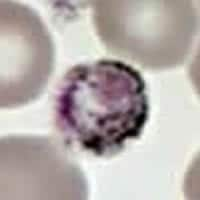
Figure D
Answer to Case #12
This was a case of malaria caused by Plasmodium malariae. Figures A, B, C, and D represented, respectively: a sturdy ring/trophozoite; a band-form trophozoite (typical for P. malariae); a schizont that is rosette-shaped, with a low number of merozoites (7 to 10, also typical for P. malariae); and a rounded gametocyte. Other diagnostic features present for P. malariae: the infected erythrocytes were not enlarged, they did not have Schüffner's dots, and the pigment was rather coarse and dark brown. The travel history was compatible with the acquisition of P. malariae in Kenya (there is no malaria transmission in Beijing, China). The relatively long period, four months, between probable infection and visit to the hospital might have been due to the fact that P. malariae tends to cause relatively mild symptoms.
In biological terms, P. malariae is the human Plasmodium species that has best adapted to its host, causing only relatively mild symptoms and enjoying a parasitic relationship with its host for a long time, possibly the lifetime of the human host. In contrast, P. falciparum would appear to be the least well adapted species, causing severe symptoms which can kill the human host—with dire consequences to the parasites, unless they can produce gametocytes and get an airlift in a passing mosquito!
More on: Malaria
Images presented in the monthly case studies are from specimens submitted for diagnosis or archiving. On rare occasions, clinical histories given may be partly fictitious.
 ShareCompartir
ShareCompartir


