Bringing Mammograms to Uninsured Women in Florida
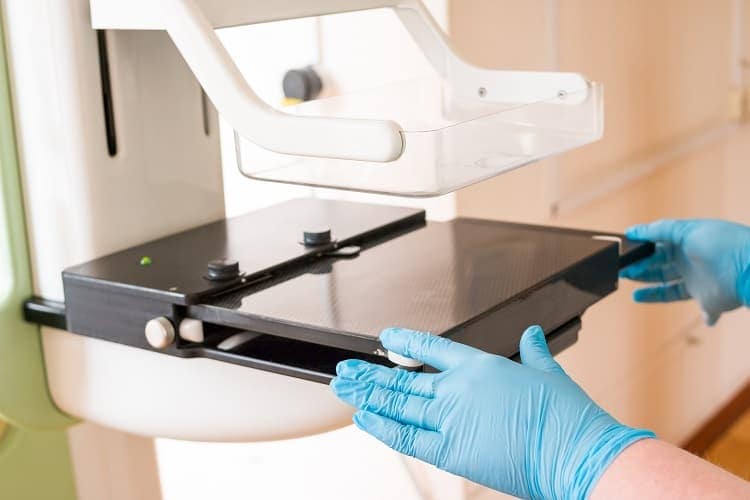
Mobile units, like the one shown here, can be used in vans to reach women in underserved areas. See how they are being used in Florida.
The Florida Breast and Cervical Cancer Early Detection Program increased the number of women without health insurance who received mammograms from 500 to more than 1,200 in one year.
How do you double the number of breast cancer screenings among women with the least access to health care? By looking at data.
In 2018, the Florida Breast and Cervical Cancer Early Detection Program (FBCCEDP) published a report that called attention to the high incidence rates of breast and cervical cancer among women without health insurance. The Florida Breast Cancer Early Detection and Treatment Referral Program Report [PDF-3.1MB] also brought attention to the low screening rates among women without health insurance who were older than age 50.
The data presented in this report were a call to action. With their current resources, how could the FBCCEDP reach more than 8% of the women aged 50 to 64 years who are eligible for the program?
Data Hold Answers
Using the data the staff collected in the report and geographic information system mapping, the staff located women with late-stage breast cancer diagnosis. Many were women without health insurance in rural areas, far from a screening facility. The FBCCEDP offered free mammograms at various locations, but few women used this resource.
The program focused on transportation and travel time as possible reasons for low screening rates. The FBCCEDP used their maps to decide where to send mobile mammography vans. The FBCCEDP built and strengthened partnerships between regional coordinators and van providers to improve screening rates and lower the number of late-stage breast cancer diagnoses.
Building Partnerships and Efficacy
“The importance of this program [FBCCEDP] is immeasurable…it has helped so many women who could not have afforded care otherwise.”
Odiane Medacier, ARNP
Using the information gathered, the FBCCEDP created a guidance manual to help regional coordinators create new partnerships and strengthen current ones with the mobile mammography van programs in the state. As a result, regional coordinators formed four new partnership agreements to provide mammograms in areas that did not have local testing sites. They brought the mammograms to women in need, rather than relying on them to make travel arrangements. This effort resulted in more women being screened (from 500 to more than 1,200) in one year.
What’s Next
The mobile mammography vans helped the FBCCEDP reach underserved women in rural communities, but there is still plenty of work to do. The program had some unexpected challenges. The vans could only provide screening mammograms, which look for possible signs of cancer. Women with symptoms need diagnostic mammograms that are more specific and require specialized care. Van reliability, complexity of event scheduling, and staff turnover also created complications for the program. Even with these challenges, the FBCCEDP intends to continue to provide free or low-cost screenings to improve access to mammography for uninsured women.