AMD: Battling HIV and STDs
Sexually transmitted diseases (STDs) have long been a formidable challenge for public health. CDC estimates that approximately 20 million new STD infections occur in the United States each year, and that more than 110 million total (new and existing) people are infected at any given time. These infections also are an economic drain on the U.S. healthcare system. Data suggest the direct cost of treating STDs in the United States is nearly $16 billion annually. Even more concerning, some STDs are becoming increasingly resistant to antimicrobials used to treat them. AMD technology has the potential to greatly advance our understanding of STDs, improve surveillance for antimicrobial resistance markers in pathogen DNA, inform vaccine development, and potentially change the diagnosis and treatment paradigm into customized treatment for individual patients.
See also Developing faster tests for HIV
In a report from 2015, CDC estimates that 1.1 million people in the United States were living with HIV. Of those people, about 15%, or 1 in 7, did not know they were infected. Though we have made great strides in preventing and treating HIV, it remains a persistent problem in the United States and globally. Early detection is key in preventing spread of the virus, and CDC scientists are using AMD methods to improve diagnostic tests to catch infections weeks earlier than previous testing methods. In addition, CDC scientists used AMD bioinformatics capabilities to develop new computer software tools to identify transmission networks for HIV and other diseases.
With AMD technologies, we are able to combine traditional shoe-leather epidemiology work with genomic data to identify transmission clusters.
To stop STD or HIV outbreaks, public health agencies conduct surveillance to find out the most likely clusters of people involved. This helps target interventions where they will make the most impact. With AMD technologies, we are able to combine traditional shoe-leather epidemiology work with genomic data to identify transmission clusters. CDC investigators used AMD bioinformatics capabilities to develop new computer software tools to identify transmission networks for HIV. These easy-to-use tools merge large amounts of epidemiologic, genomic sequence, and clinical data to provide a visual representation of transmission networks, making it easy to pinpoint clusters of recent transmission. As CDC applies these tools to analyze transmission networks more broadly, we are seeing benefits at the state and local levels. For example, CDC used an early version of these tools to assist in a 2015 investigation of an HIV-1 outbreak in rural Indiana. Investigators are now applying these new AMD tools to analyze other large CDC datasets to identify and characterize transmission networks for other infections, such as TB, hepatitis, and gonorrhea. Additional work is underway to develop secure web-based and portable versions of these tools to share with state and local partners.
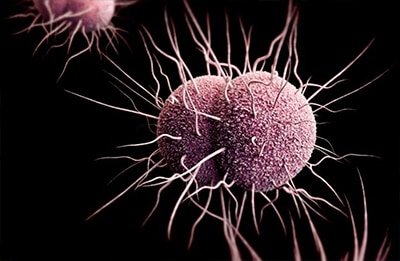
Gonorrhea is increasingly resistant to the drugs prescribed to treat it, and few antibiotic options remain. Research can help unlock the potential to develop new drugs to treat gonorrhea and better tests to find out if a patient has a resistant infection.
Before antibiotics, gonorrhea could lead to lifelong, severe illnesses, including blindness in newborns, infertility in women, and scarring of the urinary tract of men. With effective antibiotics, people are cured of gonorrhea with a single dose. But over the past few decades, public health agencies have seen a growing number of drug-resistant gonorrhea strains. To fight this urgent public health threat, CDC is using the latest advances in genome sequencing techniques to unlock the DNA of the bacterium that causes gonorrhea and identify the genes that cause antibiotic resistance. This innovative research will help scientists find better ways to prevent gonorrhea and keep untreatable gonorrhea from becoming a reality.
Hepatitis C is a contagious liver disease that can cause lifelong illness. People are infected with the hepatitis C virus (HCV) primarily through contact with the blood of an infected person, such as by sharing needles or other equipment to inject drugs. Genomic data acquired through AMD methods combined with epidemiologic information help researchers identify HCV transmission clusters and greatly improve capacity for rapid and effective response. Global Health Outbreak and Surveillance Technology (GHOST) is a web-based system that automatically performs a comprehensive analysis of genomic and epidemiologic data at the click of a button. Once a user inputs unique genomic data from an HCV sample, GHOST identifies transmission links between other virus samples and automatically creates a simple graph that shows plainly which cases are linked by transmission. GHOST sequencing technology also reduces the cost of molecular testing, making it more affordable to many more laboratories. In addition, CDC is expanding this modern molecular surveillance tool for other infectious diseases to help establish a platform for effective collaboration and communication across the public health system.

CDC researchers will work with a state health department to see why meningococcal urethritis has been on the rise.
In 2015, public health researchers found multiple cases of urethritis caused by Neisseria meningitidis, the bacteria that cause meningococcal disease. Urethritis, a swelling and irritation of the urethra (the tube that carries urine from the bladder), is typically associated with sexually transmitted diseases, like gonorrhea. Researchers are investigating how common meningococcal urethritis is, and are employing AMD methods to investigate what causes it and how it spreads. Importantly, researchers are also studying bloodstream infections and meningitis caused by N. meningitidis to determine if any belong to the group of N. meningitidis causing urethritis. This work is helping guide practices to control this disease and prevent it from spreading further.