AMD: Mapping Environmental Threats
Sometimes the very places where people live, work, and play can expose them to dangerous pathogens. Infectious, sometimes rare, bacteria and fungi can lurk in soil, in water, or even inside our homes, healthcare facilities, or recreational centers. Symptoms of illnesses from environmental pathogens tend to mimic cold and flu symptoms, making them less frequently identifiable. With AMD technologies, CDC scientists are finding ways to trace and pinpoint sources of environmental pathogen threats, both in people and in the places where we can be exposed. This work is helping locate and stop outbreaks much faster than ever before.
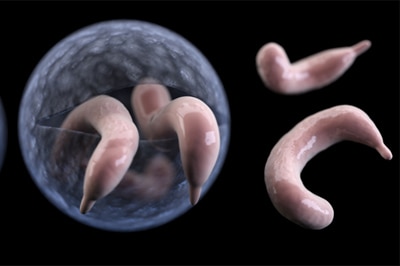
CDC upgraded the Cryptonet tracking system with AMD methods to better distinguish subtypes of waterborne Cryptosporidium parasites that make people sick.
A dangerous parasite lurks in water and it can show up in drinking water, rivers and streams, swimming pools, farms, and even in food. Cryptosporidium, or “Crypto” for short, is a microscopic parasite that causes cryptosporidiosis, a diarrheal disease that can last for weeks in people and animals. Crypto has a protective outer shell that protects it from environmental conditions and chemical disinfectants, like chlorine, commonly used to treat water and surfaces in homes, childcare settings, and healthcare facilities. CDC and state health departments collect and share Crypto DNA fingerprint data across the country through CryptoNet. Before CryptoNet was launched, scientists found it difficult to distinguish between the many Crypto species using traditional sequencing methods. In 2016, CDC developed newer, faster AMD methods, allowing investigators to look more closely at Crypto DNA, rapidly distinguish between the species and their subtypes, and better track how people are getting sick. These new data provide a clearer picture of how Cryptosporidium is spreading and what new subtypes are coming into the United States.
Legionnaires’ disease continues to cause outbreaks in the United States and is a leading cause of potable waterborne outbreaks.
Legionnaires’ disease is a serious type of bacterial pneumonia (lung infection) caused by inhaling small droplets of water that contain Legionella. Legionnaires’ disease continues to cause outbreaks in the United States and is a leading cause of potable waterborne outbreaks. To stop outbreaks, public health officials must identify the environmental source, such as cooling towers or indoor plumbing, and ensure adequate disinfection. Before CDC began applying AMD methods to Legionella, we did not have a reliable, rapid, or consistent laboratory test to analyze it. And detecting the bacterium in environmental samples was especially difficult. But with AMD technologies, we are now able to genetically compare Legionella bacterial strains from infected people to those collected in environmental samples and help identify the source of an outbreak. Through AMD methods, we are finding and stopping Legionnaires’ disease outbreaks faster than ever before.

The fungus Coccidioides lives in dry, dusty soil in certain areas of the United States.
Coccidioidomycosis, a serious fungal infection also called Valley fever, affects thousands of people every year when they inhale the microscopic fungus Coccidioides. The fungus is found in dry, dusty soil and other parts of the environment. In the past, scientists believed that this fungus lived only in the southwestern United States and parts of Latin America. That changed when public health officials identified three people in the south-central region of Washington State with Valley fever. CDC scientists used AMD methods on the Washington fungal strains and found they represent a distinct genetic group, different from the fungal strains seen in southwestern areas like California or Arizona. CDC scientists continue to use AMD technologies on patient and soil samples to understand how widespread Coccidioides is and to map geographic areas that could pose a risk for future infections.