 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Biological and Chemical Terrorism:Strategic Plan for Preparedness and ResponseRecommendations of the CDC Strategic Planning WorkgroupThe following CDC staff members prepared this report:Ali S. Khan, M.D. Michael J. Sage, M.P.H. in collaboration with the CDC Strategic Planning Workgroup Samuel L. Groseclose, D.V.M., M.P.H. Edwin Kent Gray David A. Ashford, D.V.M., M.P.H., D.Sc. Scott D. Deitchman, M.D., M.P.H. Paul K. Halverson, Dr.P.H., M.H.S.A. Joseph Hughart, M.P.H. Patricia Quinlisk, M.D. Biological and Chemical Terrorism:Strategic Plan for Preparedness and ResponseRecommendations of the CDC Strategic Planning Workgroup". . . and he that will not apply new remedies must expect new evils; for time is the greatest innovator. . . ." --The Essays by Sir Francis Bacon, 1601 Summary The U.S. national civilian vulnerability to the deliberate use of biological and chemical agents has been highlighted by recognition of substantial biological weapons development programs and arsenals in foreign countries, attempts to acquire or possess biological agents by militants, and high-profile terrorist attacks. Evaluation of this vulnerability has focused on the role public health will have detecting and managing the probable covert biological terrorist incident with the realization that the U.S. local, state, and federal infrastructure is already strained as a result of other important public health problems. In partnership with representatives for local and state health departments, other federal agencies, and medical and public health professional associations, CDC has developed a strategic plan to address the deliberate dissemination of biological or chemical agents. The plan contains recommendations to reduce U.S. vulnerability to biological and chemical terrorism --- preparedness planning, detection and surveillance, laboratory analysis, emergency response, and communication systems. Training and research are integral components for achieving these recommendations. Success of the plan hinges on strengthening the relationships between medical and public health professionals and on building new partner-ships with emergency management, the military, and law enforcement professionals. INTRODUCTIONAn act of biological or chemical terrorism might range from dissemination of aerosolized anthrax spores to food product contamination, and predicting when and how such an attack might occur is not possible. However, the possibility of biological or chemical terrorism should not be ignored, especially in light of events during the past 10 years (e.g., the sarin gas attack in the Tokyo subway [1] and the discovery of military bioweapons programs in Iraq and the former Soviet Union [2]). Preparing the nation to address this threat is a formidable challenge, but the consequences of being unprepared could be devastating. The public health infrastructure must be prepared to prevent illness and injury that would result from biological and chemical terrorism, especially a covert terrorist attack. As with emerging infectious diseases, early detection and control of biological or chemical attacks depends on a strong and flexible public health system at the local, state, and federal levels. In addition, primary health-care providers throughout the United States must be vigilant because they will probably be the first to observe and report unusual illnesses or injuries. This report is a summary of the recommendations made by CDC's Strategic Planning Workgroup in Preparedness and Response to Biological and Chemical Terrorism: A Strategic Plan (CDC, unpublished report, 2000), which outlines steps for strengthening public health and health-care capacity to protect the United States against these dangers. This strategic plan marks the first time that CDC has joined with law enforcement, intelligence, and defense agencies in addition to traditional CDC partners to address a national security threat. As a reflection of the need for broad-based public health involvement in terrorism preparedness and planning, staff from CDC's centers, institute, and offices participated in developing the strategic plan, including the
The Agency for Toxic Substances and Disease Registry (ATSDR) is also participating with CDC in this effort and will provide expertise in the area of industrial chemical terrorism. In this report, the term CDC includes ATSDR when activities related to chemical terrorism are discussed. In addition, colleagues from local, state, and federal agencies; emergency medical services (EMS); professional societies; universities and medical centers; and private industry provided suggestions and constructive criticism. Combating biological and chemical terrorism will require capitalizing on advances in technology, information systems, and medical sciences. Preparedness will also require a re-examination of core public health activities (e.g., disease surveillance) in light of these advances. Preparedness efforts by public health agencies and primary health-care providers to detect and respond to biological and chemical terrorism will have the added benefit of strengthening the U.S. capacity for identifying and controlling injuries and emerging infectious diseases. U.S. VULNERABILITY TO BIOLOGICAL AND CHEMICAL TERRORISMTerrorist incidents in the United States and elsewhere involving bacterial pathogens (3), nerve gas (1), and a lethal plant toxin (i.e., ricin) (4), have demonstrated that the United States is vulnerable to biological and chemical threats as well as explosives. Recipes for preparing "homemade" agents are readily available (5), and reports of arsenals of military bioweapons (2) raise the possibility that terrorists might have access to highly dangerous agents, which have been engineered for mass dissemination as small-particle aerosols. Such agents as the variola virus, the causative agent of smallpox, are highly contagious and often fatal. Responding to large-scale outbreaks caused by these agents will require the rapid mobilization of public health workers, emergency responders, and private health-care providers. Large-scale outbreaks will also require rapid procurement and distribution of large quantities of drugs and vaccines, which must be available quickly. OVERT VERSUS COVERT TERRORIST ATTACKSIn the past, most planning for emergency response to terrorism has been concerned with overt attacks (e.g., bombings). Chemical terrorism acts are likely to be overt because the effects of chemical agents absorbed through inhalation or by absorption through the skin or mucous membranes are usually immediate and obvious. Such attacks elicit immediate response from police, fire, and EMS personnel. In contrast, attacks with biological agents are more likely to be covert. They present different challenges and require an additional dimension of emergency planning that involves the public health infrastructure (Box 1). Covert dissemination of a biological agent in a public place will not have an immediate impact because of the delay between exposure and onset of illness (i.e., the incubation period). Consequently, the first casualties of a covert attack probably will be identified by physicians or other primary health-care providers. For example, in the event of a covert release of the contagious variola virus, patients will appear in doctors' offices, clinics, and emergency rooms during the first or second week, complaining of fever, back pain, headache, nausea, and other symptoms of what initially might appear to be an ordinary viral infection. As the disease progresses, these persons will develop the papular rash characteristic of early-stage smallpox, a rash that physicians might not recognize immediately. By the time the rash becomes pustular and patients begin to die, the terrorists would be far away and the disease disseminated through the population by person-to-person contact. Only a short window of opportunity will exist between the time the first cases are identified and a second wave of the population becomes ill. During that brief period, public health officials will need to determine that an attack has occurred, identify the organism, and prevent more casualties through prevention strategies (e.g., mass vaccination or prophylactic treatment). As person-to-person contact continues, successive waves of transmission could carry infection to other worldwide localities. These issues might also be relevant for other person-to-person transmissible etiologic agents (e.g., plague or certain viral hemorrhagic fevers). Certain chemical agents can also be delivered covertly through contaminated food or water. In 1999, the vulnerability of the food supply was illustrated in Belgium, when chickens were unintentionally exposed to dioxin-contaminated fat used to make animal feed (6). Because the contamination was not discovered for months, the dioxin, a cancer-causing chemical that does not cause immediate symptoms in humans, was probably present in chicken meat and eggs sold in Europe during early 1999. This incident underscores the need for prompt diagnoses of unusual or suspicious health problems in animals as well as humans, a lesson that was also demonstrated by the recent outbreak of mosquitoborne West Nile virus in birds and humans in New York City in 1999. The dioxin episode also demonstrates how a covert act of foodborne biological or chemical terrorism could affect commerce and human or animal health. FOCUSING PREPAREDNESS ACTIVITIESEarly detection of and response to biological or chemical terrorism are crucial. Without special preparation at the local and state levels, a large-scale attack with variola virus, aerosolized anthrax spores, a nerve gas, or a foodborne biological or chemical agent could overwhelm the local and perhaps national public health infrastructure. Large numbers of patients, including both infected persons and the "worried well," would seek medical attention, with a corresponding need for medical supplies, diagnostic tests, and hospital beds. Emergency responders, health-care workers, and public health officials could be at special risk, and everyday life would be disrupted as a result of widespread fear of contagion. Preparedness for terrorist-caused outbreaks and injuries is an essential component of the U.S. public health surveillance and response system, which is designed to protect the population against any unusual public health event (e.g., influenza pandemics, contaminated municipal water supplies, or intentional dissemination of Yersinia pestis, the causative agent of plague [7]). The epidemiologic skills, surveillance methods, diagnostic techniques, and physical resources required to detect and investigate unusual or unknown diseases, as well as syndromes or injuries caused by chemical accidents, are similar to those needed to identify and respond to an attack with a biological or chemical agent. However, public health agencies must prepare also for the special features a terrorist attack probably would have (e.g., mass casualties or the use of rare agents) (Boxes 2-5). Terrorists might use combinations of these agents, attack in more than one location simultaneously, use new agents, or use organisms that are not on the critical list (e.g., common, drug-resistant, or genetically engineered pathogens). Lists of critical biological and chemical agents will need to be modified as new information becomes available. In addition, each state and locality will need to adapt the lists to local conditions and preparedness needs by using the criteria provided in CDC's strategic plan. Potential biological and chemical agents are numerous, and the public health infrastructure must be equipped to quickly resolve crises that would arise from a biological or chemical attack. However, to best protect the public, the preparedness efforts must be focused on agents that might have the greatest impact on U.S. health and security, especially agents that are highly contagious or that can be engineered for widespread dissemination via small-particle aerosols. Preparing the nation to address these dangers is a major challenge to U.S. public health systems and health-care providers. Early detection requires increased biological and chemical terrorism awareness among front-line health-care providers because they are in the best position to report suspicious illnesses and injuries. Also, early detection will require improved communication systems between those providers and public health officials. In addition, state and local health-care agencies must have enhanced capacity to investigate unusual events and unexplained illnesses, and diagnostic laboratories must be equipped to identify biological and chemical agents that rarely are seen in the United States. Fundamental to these efforts is comprehensive, integrated training designed to ensure core competency in public health preparedness and the highest levels of scientific expertise among local, state, and federal partners. KEY FOCUS AREASCDC's strategic plan is based on the following five focus areas, with each area integrating training and research:
Preparedness and PreventionDetection, diagnosis, and mitigation of illness and injury caused by biological and chemical terrorism is a complex process that involves numerous partners and activities. Meeting this challenge will require special emergency preparedness in all cities and states. CDC will provide public health guidelines, support, and technical assistance to local and state public health agencies as they develop coordinated preparedness plans and response protocols. CDC also will provide self-assessment tools for terrorism preparedness, including performance standards, attack simulations, and other exercises. In addition, CDC will encourage and support applied research to develop innovative tools and strategies to prevent or mitigate illness and injury caused by biological and chemical terrorism. Detection and SurveillanceEarly detection is essential for ensuring a prompt response to a biological or chemical attack, including the provision of prophylactic medicines, chemical antidotes, or vaccines. CDC will integrate surveillance for illness and injury resulting from biological and chemical terrorism into the U.S. disease surveillance systems, while developing new mechanisms for detecting, evaluating, and reporting suspicious events that might represent covert terrorist acts. As part of this effort, CDC and state and local health agencies will form partnerships with front-line medical personnel in hospital emergency departments, hospital care facilities, poison control centers, and other offices to enhance detection and reporting of unexplained injuries and illnesses as part of routine surveillance mechanisms for biological and chemical terrorism. Diagnosis and Characterization of Biological and Chemical AgentsCDC and its partners will create a multilevel laboratory response network for bioterrorism (LRNB). That network will link clinical labs to public health agencies in all states, districts, territories, and selected cities and counties and to state-of-the-art facilities that can analyze biological agents (Figure 1). As part of this effort, CDC will transfer diagnostic technology to state health laboratories and others who will perform initial testing. CDC will also create an in-house rapid-response and advanced technology (RRAT) laboratory. This laboratory will provide around-the-clock diagnostic confirmatory and reference support for terrorism response teams. This network will include the regional chemical laboratories for diagnosing human exposure to chemical agents and provide links with other departments (e.g., the U.S. Environmental Protection Agency, which is responsible for environmental sampling). ResponseA comprehensive public health response to a biological or chemical terrorist event involves epidemiologic investigation, medical treatment and prophylaxis for affected persons, and the initiation of disease prevention or environmental decontamination measures. CDC will assist state and local health agencies in developing resources and expertise for investigating unusual events and unexplained illnesses. In the event of a confirmed terrorist attack, CDC will coordinate with other federal agencies in accord with Presidential Decision Directive (PDD) 39. PDD 39 designates the Federal Bureau of Investigation as the lead agency for the crisis plan and charges the Federal Emergency Management Agency with ensuring that the federal response management is adequate to respond to the consequences of terrorism (8). If requested by a state health agency, CDC will deploy response teams to investigate unexplained or suspicious illnesses or unusual etiologic agents and provide on-site consultation regarding medical management and disease control. To ensure the availability, procurement, and delivery of medical supplies, devices, and equipment that might be needed to respond to terrorist-caused illness or injury, CDC will maintain a national pharmaceutical stockpile. Communication SystemsU.S. preparedness to mitigate the public health consequences of biological and chemical terrorism depends on the coordinated activities of well-trained health-care and public health personnel throughout the United States who have access to up-to-the minute emergency information. Effective communication with the public through the news media will also be essential to limit terrorists' ability to induce public panic and disrupt daily life. During the next 5 years, CDC will work with state and local health agencies to develop a) a state-of-the-art communication system that will support disease surveillance; b) rapid notification and information exchange regarding disease outbreaks that are possibly related to bioterrorism; c) dissemination of diagnostic results and emergency health information; and d) coordination of emergency response activities. Through this network and similar mechanisms, CDC will provide terrorism-related training to epidemiologists and laboratorians, emergency responders, emergency department personnel and other front-line health-care providers, and health and safety personnel. PARTNERSHIPS AND IMPLEMENTATIONImplementation of the objectives outlined in CDC's strategic plan will be coordinated through CDC's Bioterrorism Preparedness and Response Program. Program personnel are charged with a) helping build local and state preparedness, b) developing U.S. expertise regarding potential threat agents, and c) coordinating response activities during actual bioterrorist events. Program staff have established priorities for 20002002 regarding the focus areas (Box 6). Implementation will require collaboration with state and local public health agencies, as well as with other persons and groups, including
RECOMMENDATIONSImplementing CDC's strategic preparedness and response plan by 2004 will ensure the following outcomes:
CONCLUSIONRecent threats and use of biological and chemical agents against civilians have exposed U.S. vulnerability and highlighted the need to enhance our capacity to detect and control terrorist acts. The U.S. must be protected from an extensive range of critical biological and chemical agents, including some that have been developed and stockpiled for military use. Even without threat of war, investment in national defense ensures preparedness and acts as a deterrent against hostile acts. Similarly, investment in the public health system provides the best civil defense against bioterrorism. Tools developed in response to terrorist threats serve a dual purpose. They help detect rare or unusual disease outbreaks and respond to health emergencies, including naturally occurring outbreaks or industrial injuries that might resemble terrorist events in their unpredictability and ability to cause mass casualties (e.g., a pandemic influenza outbreak or a large-scale chemical spill). Terrorism-preparedness activities described in CDC's plan, including the development of a public health communication infrastructure, a multilevel network of diagnostic laboratories, and an integrated disease surveillance system, will improve our ability to investigate rapidly and control public health threats that emerge in the twenty first century. References
Figure 1 1 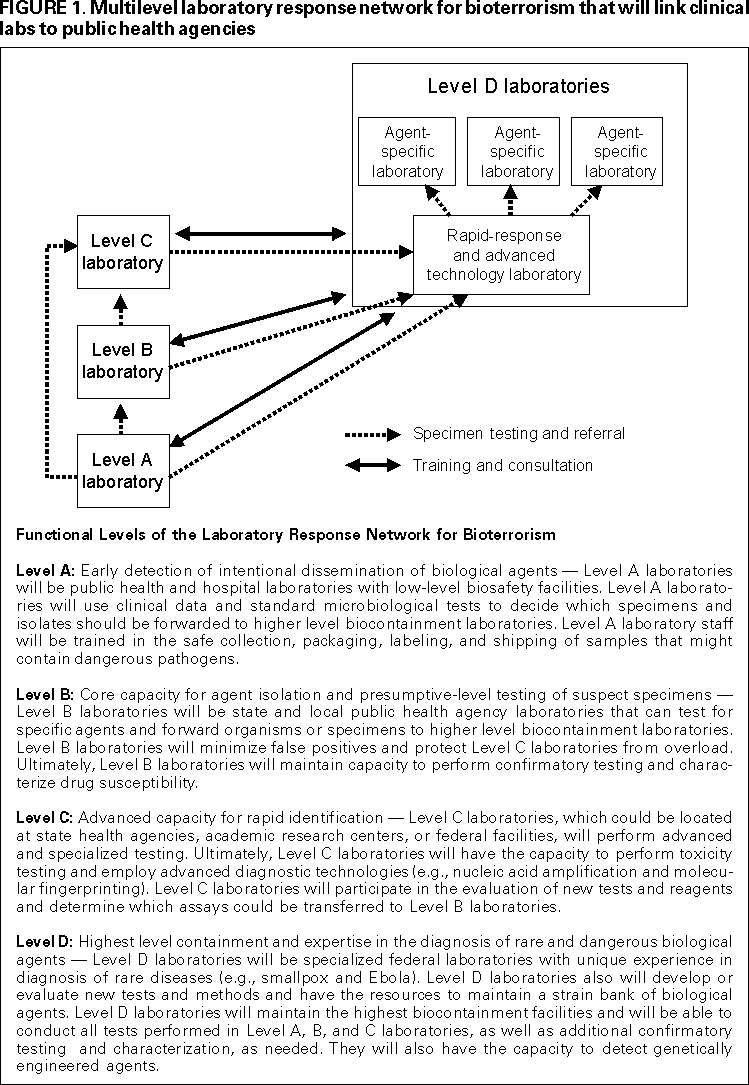 Return to top. Box 1 BOX 1. Local public health agency preparedness
Box 2 BOX 2. Preparing public health agencies for biological attacksSteps in Preparing for Biological Attacks
Box 3 BOX 3. Critical biological agentsCategory AThe U.S. public health system and primary health-care providers must be prepared to address varied biological agents, including pathogens that are rarely seen in the United States. High-priority agents include organisms that pose a risk to national security because they
Category A agents include
Category B Second highest priority agents include those that
These pathogens include but are not limited to
Category C Third highest priority agents include emerging pathogens that could be engineered for mass dissemination in the future because of
* CDC. Preventing emerging infectious diseases: a strategy for the 21st century.
Atlanta, Georgia: U.S. Department of Health and Human Services, 1998.
BOX 4. Preparing public health agencies for chemical attacksSteps in Preparing for Chemical Attacks
Return to top. Box 5 BOX 5. Chemical agentsChemical agents that might be used by terrorists range from warfare agents to toxic chemicals commonly used in industry. Criteria for determining priority chemical agents include
BOX 6. Implementation Priorities Regarding Focus Areas for 2000-2002Preparedness and Prevention
Detection and Surveillance
Diagnosis and Characterization of Biological and Chemical Agents
Response
All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 4/14/2000 |
|||||||||
This page last reviewed 5/2/01
|