 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Progress Toward Sustainable Measles Mortality Reduction --- South-East Asia Region, 1999--2002Substantial progress has been made toward meeting the 2003 World Health Assembly goal to reduce measles deaths 50% by the end of 2005, compared with deaths in 1999. Although measles remains the leading cause of vaccine-preventable deaths among children, the World Health Organization (WHO) estimates that, during 1999--2002, global measles mortality decreased 29%, including a 19% decline among South-East Asia Region (SEAR) member countries (1). In June 2003, the SEAR Regional Technical Advisory Group on Immunization endorsed a Regional Strategic Plan for Measles Mortality Reduction (2003--2005) (2). This report summarizes progress in measles control in SEAR during 1999--2002 and outlines plans for future activities in the region, which include strengthening measles surveillance, improving access to routine vaccination, and providing a second opportunity for measles immunization. Measles SurveillanceAll countries in the region include measles as a reportable disease in their routine communicable disease surveillance systems. Before 2001, Sri Lanka and Thailand collected case-based data nationwide. Health authorities in other countries relied on passive surveillance of clinically confirmed cases and maintained aggregated data at the national level. Beginning in 2001, the WHO-supported surveillance medical officers (SMOs) in Bangladesh, Indonesia, Myanmar, and Nepal have added measles to their original focus on acute flaccid paralysis (AFP) surveillance. In these countries, SMOs conduct outbreak investigations and routinely collect case-based data, including information on age, outcome, and vaccination status. In 2002, WHO established a regional network of national measles laboratories with standardized testing procedures for IgM antibody to measles in all SEAR member countries. Five to 10 samples are tested during each outbreak to confirm the diagnosis of measles. Reported IncidenceDuring 1989--1999, the number of measles cases decreased steadily, from approximately 440,000 reported cases to 45,000. However, the number of cases gradually increased to 88,000 in 2002, primarily because of increases in India, Indonesia, and Thailand (Table 1) and nationwide outbreaks in several other countries of the region. During September 1999--May 2000, a total of 15,337 measles cases and 23 deaths were reported in Sri Lanka. Of 6,352 cases with information available, 3,481 (54.8%) were in persons aged >15 years. A similar outbreak occurred in Maldives in 2002, in which 444 (54.2%) of 819 reported cases were in persons aged >15 years. In contrast, both routine and outbreak reporting from other countries have documented a broad age distribution, with the majority of cases in persons aged <10 years (Table 2). Mortality reported from both routine surveillance and outbreak investigations remains low. Nevertheless, on the basis of vaccination coverage and available case-fatality data, WHO estimated 243,000 measles deaths in the region in 1999 and 196,000 deaths in 2002 (1). Routine VaccinationAll countries in SEAR include a dose of measles-containing vaccine (MCV1) in their routine immunization schedule at age 9 months. Sri Lanka adds a second dose as measles-rubella vaccine at age 3 years. Thailand provides a dose of measles-mumps-rubella vaccine at age 9--12 months and at age 6 years. Administrative reporting indicated that the SEAR average measles vaccination coverage for MCV1 remained >85% during the 1990s (3). WHO/United Nations Children's Fund (UNICEF) estimates (Table 1), which rely on expert review of national reports and surveys, indicate the regional average in recent years is substantially lower than previous administrative reporting indicated. On the basis of WHO/UNICEF estimates, regional coverage for MCV1 has increased, from 58% in 1999 to 70% in 2002, primarily because of increases in India. Supplemental Immunization Activities (SIAs)Nationwide supplemental measles vaccination campaigns were conducted in the Democratic People's Republic of Korea (DPRK) in 1999, targeting children aged 9--23 months, and in Bhutan during 2000, targeting children aged 9 months--15 years. Myanmar began conducting a national campaign for children aged 9--59 months in three annual phases beginning in 2002. Subnational supplemental mass measles campaigns conducted include border areas in Bangladesh (1999 and 2001), urban areas in India (2000 and 2001), and underserved areas and school-aged children in Indonesia (2000 and 2002). Indonesia and Bhutan combined measles with polio campaigns. Coverage in SIAs ranged from 69% in India to >100% of the target in Bangladesh (Table 3). Reported by: Regional Office for South-East Asia, New Delhi, India. Dept of Immunization and Vaccine Development, World Health Organization, Geneva, Switzerland. Editorial Note:Before 1999, the majority of countries in SEAR used routine administrative reports to estimate official measles vaccination coverage rates (3). In 1999, countries began to use survey data as the source of official estimates. By 2002, both national official estimates and WHO/UNICEF estimates relied on survey results as a primary data source, resulting in greater agreement between national and WHO/UNICEF estimates. However, obtaining timely, reliable data on both coverage and incidence remains difficult. Despite encouraging trends in routine measles coverage for the region, as reflected in the WHO/UNICEF estimates, reported cases of measles actually increased during 1999--2002, and measles remains a substantial cause of morbidity and mortality among children in SEAR. The majority of this increase occurred in India and Indonesia, probably because of improved reporting and multiple outbreaks. Although coverage improved in these countries, the number of susceptible children in these highly populous areas remains the primary cause of sustained high morbidity. The increase in cases in Thailand and recent outbreaks among older children and adolescents in Sri Lanka and Maldives indicate that measles also is a substantial health risk even in countries with relatively high vaccination coverage levels. Similar to other regions (4), in SEAR countries where reported measles vaccine coverage is >80%, the majority of affected children are aged >10 years. Conversely, in countries with coverage <80% (e.g., Bangladesh, Indonesia, and Myanmar), the majority of cases occur in children aged <10 years. Although polio eradication remains a priority for SEAR, countries in the region have increased the priority of measles control. Integrating measles surveillance with AFP surveillance and establishing a measles laboratory network to confirm outbreaks increases the reliability of surveillance data. These data have been essential in determining appropriate control strategies, particularly in setting target age groups for catch-up campaigns. Case-fatality studies planned for 2004 in Nepal and Bangladesh will further help to characterize the mortality burden of measles in the region. SEAR countries have adopted a plan to reduce measles mortality 50% by 2005 (relative to 1999) in polio-free countries. Other objectives are to 1) achieve monthly reporting of the number of measles cases and deaths by 2004, 2) investigate 80% of outbreaks by 2005 to better direct vaccination strategies, 3) achieve and maintain 80% coverage with routine measles vaccination in >80% of districts in all countries by 2005, and 4) provide a second opportunity for MCV1 vaccination to all eligible children in the region by 2005 (5). In 2002 and 2003, Myanmar, Timor-Leste, and Indonesia began SIAs as a stopgap measure while improvements in routine vaccination services are made. In 2004, Indonesia plans to phase in a dose for school-aged children, and other countries will need to consider adding a second measles dose to their Expanded Program on Immunization (EPI) schedule once their routine coverage improves. Nepal also plans a phased national measles campaign starting in 2004. Large-scale campaigns in populous countries (e.g., Bangladesh, India, and Indonesia) present substantial resource and logistical challenges. These countries should evaluate their administrative areas separately and adapt specific strategies appropriately. Other countries, including Bhutan, DPRK, Maldives, Sri Lanka, and Thailand, have achieved low measles mortality levels, but experience periodic measles outbreaks. Sri Lanka and Thailand already provide a second MCV1 dose, and Bhutan and Maldives have indicated their intention to do so by 2005. These countries, which have already achieved the standards set for mortality reduction but have not yet officially adopted a national measles elimination policy, could strengthen their immunization strategies and surveillance standards by adopting recommendations of the recent global meeting on measles control (6). The ultimate goal for every member country is to achieve sustainable measles mortality reduction. Achieving this goal requires addressing issues related to access to measles immunization and mobilization of internal and external resources. Therefore, countries should prepare comprehensive national action plans for measles control that are linked to their national EPI plans. References
Table 1 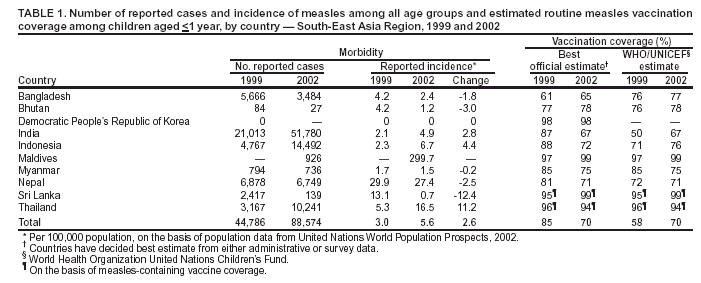 Return to top. Table 2 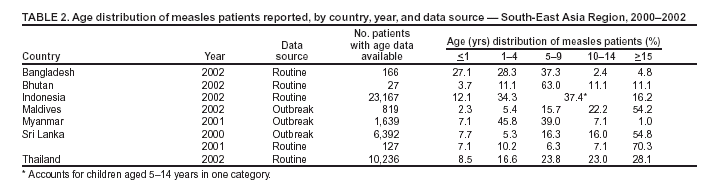 Return to top. Table 3  Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 7/1/2004 |
|||||||||
This page last reviewed 7/1/2004
|