 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. National Estimates of Nonfatal Injuries Treated in Hospital Emergency Departments --- United States, 2000On July 1, 2000, the Consumer Product Safety Commission's (CPSC) National Electronic Injury Surveillance System (NEISS) was expanded to collect data on all types and external causes of nonfatal injuries and poisonings treated in U.S. hospital emergency departments (EDs). This augmented system, called NEISS All Injury Program (NEISS-AIP), is a collaborative effort between CDC's National Center for Injury Prevention and Control and CPSC. This report presents annualized national estimates using NEISS-AIP data obtained during July 1--September 30, 2000, which indicate that approximately 31,000,000 persons were treated for nonfatal injuries in EDs in 2000. Although most of the injuries were unintentional, an estimated 1,973,000 were violence-related. Data from NEISS-AIP can be used for monitoring temporal trends in nonfatal injuries by mechanism and intent of injury. NEISS-AIP data were collected from 66 of the 100 NEISS hospitals, which were selected as a stratified probability sample of all hospitals in the United States and its territories with a minimum of six beds and a 24-hour ED (1,2). The 66 NEISS-AIP hospitals are a nationally representative sample of U.S. hospital EDs. NEISS-AIP hospitals provide data on approximately 600,000 injury- and consumer product-related ED cases each year. Data from these cases are weighted by the inverse of the probability of selection to provide national estimates (1). Annualized estimates were based on weighted data for 126,547 nonfatal injury-related ED visits during July 1--September 30, 2000. Each sample was weighted by four and then these adjusted weights were added to provide annualized estimates for the overall population and population subgroups (i.e., age, sex, and race/ethnicity*). SUDAAN was used to account for the complex sample design (1). Nonfatal injuries and poisonings were defined as bodily harm resulting from acute exposure to an external force or substance (i.e., mechanical, thermal, electrical, chemical, or radiant) and near drowning, including unintentional and violence-related causes. Cases were excluded if 1) the principal diagnosis was an illness, pain only, psychological harm (e.g., anxiety and depression) only, contact dermatitis associated with exposure to consumer products (e.g., body lotions, detergents, and diapers) and plants (e.g., poison ivy), or unknown; or 2) the ED visit was for adverse effects of therapeutic drugs or of surgical and medical care (3). All injuries were classified for intent of injury (i.e., unintentional, assault, self harm, and legal intervention) and mechanism of injury (i.e., fall, struck by/against, motor-vehicle-occupant--related incident, cut/pierce, and fire/burn) (4). Unintentional included unintended injuries and injuries in which no indication of intent to harm was documented in the ED record. Assault included suspected and confirmed injuries from interpersonal violent events (e.g., injuries to victims, innocent bystanders, police, and perpetrators). Self harm included suspected and confirmed intentionally self-inflicted injuries. Legal intervention included injuries inflicted by police or other legal authorities (e.g., security guards) while acting in the line of duty. The mechanism of injury represents the precipitating mechanism that initiated the chain of events leading to the injury, which is similar to the underlying cause for injury-related death. Mechanisms of injury were classified by trained coders into recommended major external cause-of-injury groupings (3,5) using definitions consistent with International Classification of Diseases, Ninth Revision, Clinical Modifications (ICD-9-CM) external cause coding guidelines (6). Because of limited resources, ICD-9-CM external cause-of-injury codes were not assigned. During 2000, persons with nonfatal injuries were treated in EDs at an estimated rate of 11,188 per 100,000 population. The nonfatal injury rate was approximately 40% higher for males than for females (Table 1). Males aged 15--19 years had the highest nonfatal injury rate (20,528 per 100,000 population) (Table 1). Of the estimated 31,000,000 nonfatal injuries, 93.6% were unintentional and the remaining 6.4% were violence-related, including assaults (5.5%), intentional self harm (0.7%), and legal interventions (0.2%) (Table 2). Falls were the leading cause of unintentional nonfatal injuries, accounting for an estimated 7,021,000 (24.4%) of unintentional injury-related ED visits. An estimated 3,299,000 persons were injured as an occupant in a motor vehicle (Table 2), of which 95.2% were traffic-related. Injuries to motor-vehicle occupants were the leading cause of unintentional nonfatal injury-related ED visits for females aged 15--24 years. The non-fatal injury rate for pedal cyclists was 2.9 times higher for males than for females (Table 2). An estimated 389,000 persons were treated in EDs for dog bites (Table 2). Of an estimated 1,973,000 violence-related nonfatal injuries, 66% were physical assaults that included being hit with an object or by another person (Table 2). Sexual assault was the fourth leading cause of violence-related, nonfatal injury-related ED visits; the nonfatal rate of sexual assault for females was 4.8 times higher than that for males (Table 2). Approximately 150,000 persons were treated in EDs for poisoning-related suicide attempts and the rate of intentionally self-inflicted, nonfatal poisonings for females was 1.6 times that for males (Table 2). Reported by: Office of Statistics and Programming, National Center for Injury Prevention and Control, CDC. Editorial Note:The findings in this report indicate that, in 2000, approximately 10% of U.S. residents were treated for nonfatal injuries in EDs. On the basis of NEISS-AIP and National Vital Statistics System data (7), for every injury-related death in the United States, approximately 200 persons were treated for nonfatal injuries in EDs. Most (93.6%) of these injuries were unintentional; however, approximately 2 million persons were treated for violence-related injuries. NEISS-AIP will provide a national data source for further characterizing these injuries by unintentional and violence- related causes and helping to identify those at risk. NEISS-AIP will provide additional data on the characteristics and circumstances of injuries that are treated in EDs. In addition to age, race/ethnicity, sex, intent of injury, and mechanism of injury, data are being collected on principal diagnosis, primary body part affected, locale where the injury occurred, work-relatedness, consumer products involved, and disposition at ED discharge. For transport-related injuries, data are being collected on traffic-relatedness and on motor-vehicle occupant status (e.g., driver, passenger, boarding, and alighting) at the time of the injury. For assaults, data are being collected on the relationship of the perpetrator to the injured person (e.g., spouse/partner, parent, other relative, friend, and stranger) and the context (e.g., altercation, robbery, sexual assault, drug-related, and gang-related). In addition, on the basis of information in the ED record, a brief narrative is being recorded that provides further details about the circumstances of the incident. Annualized national estimates of NEISS-AIP data for July 1--September 30, 2000, are comparable to estimates based on other surveys. Data for 1998 from the National Hospital Ambulatory Medical Care Survey (NHAMCS), which collects data on all types of ED visits and focuses primarily on health-care utilization, identified an average annual estimate of 37,111,000 injury-related ED visits (8). NHAMCS used an injury definition similar to that of NEISS AIP. However, the NHAMCS estimate includes both initial ED visits and revisits for the same injury; the NEISS-AIP estimate includes only initial ED visits. Data from a 3-month NEISS All Injury Pilot Study conducted during May 1--July 31, 1997, of a nationally representative sample of 21 NEISS hospitals identified an annualized estimate of 29,060,000 injuries (9). The distributions of injuries by intent and mechanism of injury were similar among all three data sources. For example, the percentage of injury-related ED visits that were violence-related was 5.2% for NHAMCS, 5.6% for the NEISS All Injury Pilot Study, and 6.4% for NEISS-AIP. The percentage of violence-related cases for NEISS-AIP might be expected to be highest because data were obtained for ED visits during July--September when assault rates are higher than during other months of the year (10). The findings in this report are subject to at least three limitations. First, this system provides only national estimates and does not allow for estimates by region, state, or local jurisdiction. Second, data are based solely on information provided in the ED record and are not linked to criminal justice, police reports, or other data sources to supplement or verify the cause and intent of injury. Finally, because the estimates were derived from 3 months of data, they do not account for cause-specific seasonal differences in the number of injuries (10). Hospital audits conducted by CPSC indicate that NEISS hospital coders identify approximately 90% of all reportable product-related cases (A. McDonald, CPSC, personal communication, 2001). NEISS also has the capacity to conduct special studies to collect more details about specific types and causes of injury, and in-depth follow-up interviews for case studies of injury circumstances and consumer product involvement. References
* On the ED record, often only one entry is available for race or ethnicity. The classification scheme for this report assumed that most white Hispanics probably were recorded on the ED record as Hispanics and most black Hispanics probably were recorded as black. Table 1 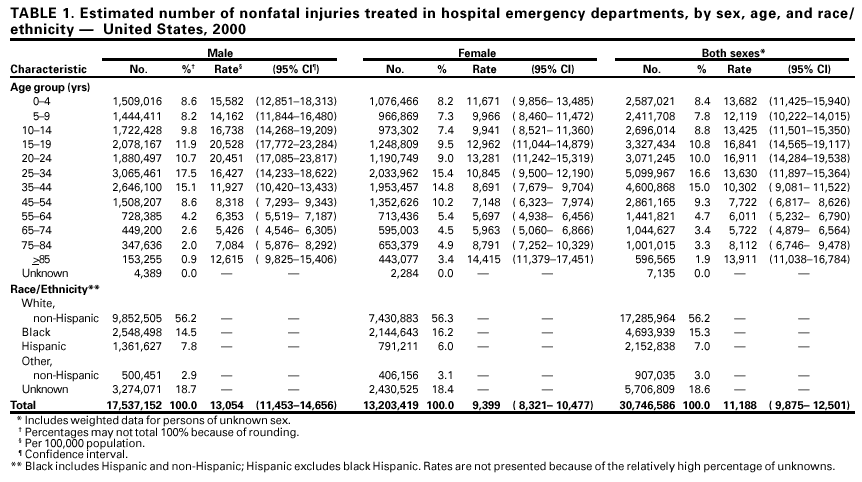 Return to top. Table 2 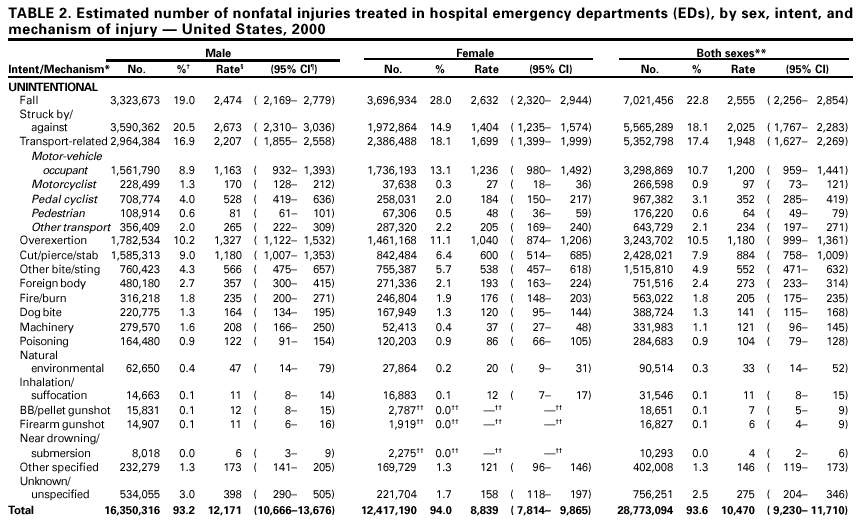 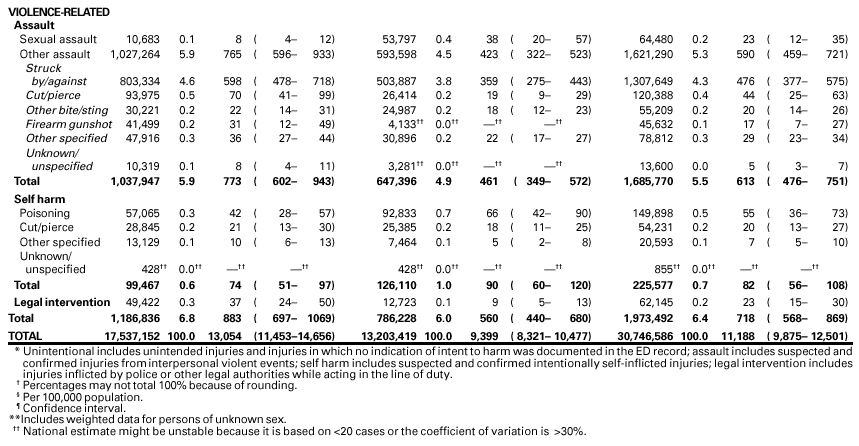 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 5/3/2001 |
|||||||||
This page last reviewed 5/3/2001
|