 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Update: Syringe Exchange Programs --- United States, 1998Syringe exchange programs (SEPs) provide sterile syringes* in exchange for used syringes to reduce the transmission of human immunodeficiency virus (HIV) and other bloodborne infections associated with the reuse of potentially blood-contaminated syringes among injection drug users (IDUs) (1). This report summarizes a survey of 1998 SEP activities in the United States and compares them with 1994--1997 SEP activity surveys (1--3). SEPs are an increasingly common HIV prevention approach that offer a range of public health services in addition to syringe exchange. In October 1999, staff from Beth Israel Medical Center and the North American Syringe Exchange Network (NASEN) mailed surveys to 131 SEP directors (compared with 68 in 1994--1995, 101 in 1996, and 113 in 1997) (2--4), and followed up with telephone interviews about syringes distributed/returned, services provided, and budgets and funding during 1998. The methods of this survey were the same as previous surveys of SEP activities (2--4). Among the 131 SEPs contacted, 110 (84%) completed the survey. Some SEPs participated in the survey on the condition that their program data be reported only in aggregate. SEPs operated in 81 cities† and 31 states, the District of Columbia, and Puerto Rico§. The largest number of SEPs were in four states: 21 in California, 14 in New York, 12 in Washington, and nine in New Mexico. SEPs were classified by the number of syringes exchanged during 1998 (Table 1); 107 reported exchanging 19,397,527 syringes. The 12 largest programs exchanged 62% of all syringes¶. Referral to substance abuse treatment was provided by 104 (95%) of the 110 SEPs, 109 (99%) provided alcohol pads, 99 (90%) provided bleach, 108 (98%) provided male condoms, 80 (73%) provided female condoms, 104 (95%) provided referrals to substance abuse treatment, 70 (64%) provided on-site voluntary counseling and testing for HIV, 26 (24%) for hepatitis C, and 23 (21%) for hepatitis B. In addition, 21 (19%) provided on-site medical care, 18 (16%) provided hepatitis B vaccine, 17 (15%) provided tuberculosis screening, and 14 (13%) provided sexually transmitted disease screening. A median of 2.5 on-site services were provided by small, 3.0 by medium, 2.0 by large, and 7.0 by very large programs. During 1998, SEPs operated at 534 sites averaging five sites per program (median: nine; range: 1--31). Sites included 202 health van stops, 59 shooting galleries, 56 sidewalk tables, 51 cars, 43 storefronts/indoor sites, 30 SEP workers on foot, 23 health clinics, and 70 other sites. Delivery of syringes and other risk-reduction supplies to residences or meeting spots was reported by 55 (50%) SEPs, and 94 (85%) allowed participants to exchange syringes for persons other than themselves (secondary exchange). The 110 SEPs operated a mean of 20 hours per week per program (median: 22 hours; range: 1--140 hours). Sixteen SEPs had syringe shortages that caused four to close temporarily for 16 months (range: 2--8 months). The combined operating budget of 105 SEPs was $8,567,662 (range: 0--$771,053; mean: $80,493; median: $38,000). A total of 51 SEPs in 15 states** and Puerto Rico received public funding of $5,992,032. From 1994--1995 to 1998††, the number of SEPs participating in the activities survey increased from 60 to 110 (83%), the number of cities with SEPs increased from 46 to 81 (76%), and the number of syringes exchanged increased from 8.0 million to 19.4 million (143%) (Table 2). Nine SEPs received no funds; however, they exchanged >185,000 syringes and provided other services using donated supplies and volunteers. Reported by: MP Singh, MPH, CA McKnight, MPH, D Paone, EdD, S Titus, MPH, DC Des Jarlais, PhD, Edmond de Rothschild Foundation Chemical Dependency Institute, Beth Israel Medical Center; M Krim, PhD, American Foundation for AIDS Research, New York, New York. D Purchase, J Rustad, A Solberg, North American Syringe Exchange Network, Tacoma, Washington. Editorial Note:The findings of the 1998 survey indicated growth in the number of cities with SEPs and in the number of SEPs that provide prevention services for IDUs. Many SEPs, particularly the largest programs, serve as community-based HIV prevention and health promotion centers for IDUs, including IDUs at high risk for bloodborne infections (5). SEPs also provide additional services (e.g., influenza and pneumococcal vaccinations) (6). Hepatitis B vaccination at a SEP was an important part of the public health response to a hepatitis B outbreak among IDUs in Pierce County, Washington (7). State and local governments funded approximately two thirds of the total SEPs budget for 1998. The findings in this report are subject to at least three limitations. First, the extent of SEP activity probably is underestimated because some of the known SEPs did not participate in this survey and others may exist that are not known to NASEN. Second, the information collected was self-reported and may be biased. Third, because 36 (33%) SEPs requested that their survey data be kept confidential, some data are included only as aggregate state-level information. IDU access to sterile syringes can be augmented by methods other than SEPs (8). During 2000, New Hampshire, New York, and Rhode Island adopted new syringe laws that partially or completely removed the requirement for a prescription to purchase syringes and legal penalties for syringe possession. Physician prescription of sterile syringes to IDUs is another possible mechanism (9). Assuming availability of sterile syringes for IDUs who continue to inject is only one component of a comprehensive approach to HIV prevention for IDUs. Other HIV prevention components include substance abuse treatment, community outreach, tailored HIV counseling and testing, prevention of sexual transmission, services in correctional settings, primary drug prevention, and services for HIV-infected IDUs (10). References
* "Syringe" refers to both syringes and needles. † Cities with multiple SEPs: Detroit, Michigan; Indianapolis, Indiana; Los Angeles, California; Minneapolis, Minnesota; New York, New York; Portland, Oregon; San Francisco, California; Seattle and Tacoma, Washington, and five others that asked that their program-specific information be kept confidential. § States with SEPs: California (21); New York (14); Washington (12); New Mexico (nine); Connecticut (six); Massachusetts (five); Michigan, Oregon, Pennsylvania, Wisconsin (three each); Colorado, Illinois, Indiana, Minnesota, Montana, Ohio, Puerto Rico, Texas, (two each); and Alaska, Arizona, District of Columbia, Georgia, Hawaii, Kansas, Louisiana, Maryland, North Carolina, New Hampshire, New Jersey, Oklahoma, Rhode Island, Tennessee, and Utah (one each). ¶ States with the largest SEPs: California (four); Washington (three); New York (two); and Illinois, Maryland, and Pennsylvania (one each). The largest SEPs were San Francisco AIDS Foundation, California (2.1 million syringes exchanged); Chicago Recovery Alliance, Illinois (1.5 million); Point Defiance AIDS Project, Tacoma, Washington (1.1 million); Seattle-King County Department of Public Health Needle Exchange Program, Seattle, Washington (1.0 million); Lower East Side Needle Exchange Program, New York, New York (0.9 million); Alameda County SEP, Oakland, California (0.8 million); Street Outreach Services, Seattle, Washington (0.7 million); Baltimore Department of Public Health, Maryland (0.7 million); and Clean Needles Now, Los Angeles, California (0.6 million). Three large SEPs that exchanged 2.8 million syringes during 1998 asked that their program-specific information be kept confidential. ** SEPs received public funding in the following: 1) states: Arizona, California, Colorado, Connecticut, Hawaii, Illinois, Massachusetts, Maryland, New Mexico, New York, Oregon, Pennsylvania, Puerto Rico, Rhode Island, Washington, and Wisconsin; 2) counties: Clark, King, Pierce, Skagit, and Snohomish, Washington; Pima, Arizona; Boulder, Colorado; Cook, Illinois; and Multnomah, Oregon; and 3) cities: Berkeley, Los Angeles, and San Francisco, California; Chicago, Illinois; Baltimore, Maryland; Portland, Oregon; Seattle, Washington, and Milwaukee, Wisconsin. †† From 1998 to March 2001, the number of SEPs known to NASEN increased from 131 to 168 (D. Purchase, NASEN, personal communication, 2001). Table 1 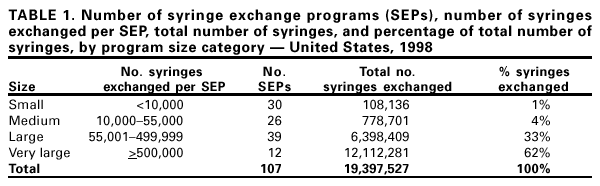 Return to top. Table 2 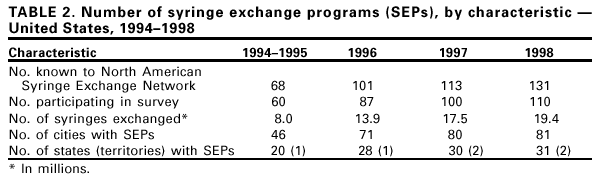 Return to top. Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 5/17/2001 |
|||||||||
This page last reviewed 5/17/2001
|